Age
Common conditions
0–5
Transient synovitis
Septic arthritis
Osteomyelitis
Discitis
DDH
Toddler’s fracture
Non-accidental injury
5–10
Transient synovitis
Septic arthritis
Osteomyelitis
Discitis
Perthes’ disease
10–15
SCFE
Septic arthritis
Osteomyelitis
Spondylolysis
Spondylolisthesis
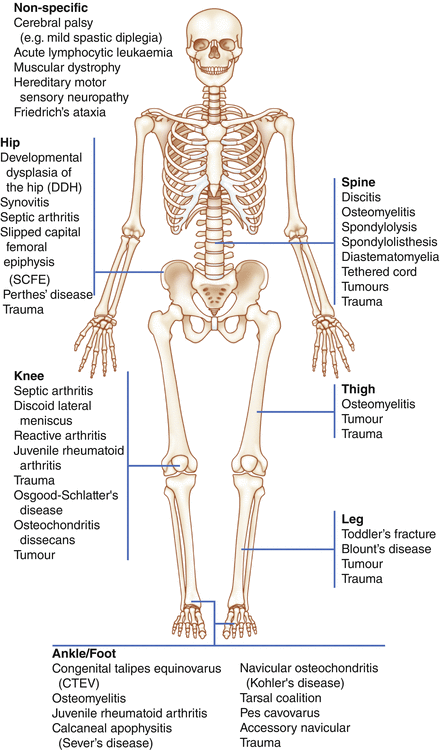
Figure 2.1
Causes of limping based on site of pathology
History
It is important to obtain a complete and precise history, using open questions where possible. The history may well be vague, especially in the case of the younger child. Parents will often find it difficult to describe the exact nature of the limp or provide an accurate timeline of symptoms. It is important not to lead the parents towards a presumptive diagnosis or be overconfident in one’s approach as this can lead to greater diagnostic error.
A complete history must include the duration and nature of the limp, the association of the limp with any pain, any episode of trauma which may have been originally dismissed as trivial, recent illness and/or co-current ‘red flags’ i.e. fever, rigors, malaise, pain poorly responsive to analgesics, night pain (which manifests as night awakening), loss of weight and night sweats. The clinician must be vigilant regarding any recently recorded pyrexia, as swinging pyrexia may be at its trough during the clinical encounter.
Precision regarding the nature of the onset of the limp, whether it is getting better or worse, treatment to date, including use of analgesics (whether simple, strong or NSAIDs), will aid to clarify the severity of the problem and also make the clinician aware that the clinical picture that is being observed may have been affected by that treatment e.g. a controlled pyrexia or a greater range of motion.
Examination
The examination of child can be extremely challenging, especially in a child who is yet to talk. Gaining the confidence of the child and parents is vital.
Standard physiological indices of temperature and pulse should always be recorded, and the standard “look, feel and move” approach can then be followed. Although the history and observing the child alone may lead to a diagnosis, it is still prudent to examine the child in a complete fashion. The un-affected limb should be examined first so that a comparison can be made and the confidence of the child gained further.
Look
General unobtrusive observation of the child walking and displaying the limp should be the first step. This will require the child to be undressed appropriately.
Gait
Remembering normal gait milestones is important. Children begin to walk independently from 12 to 14 months. This is preceded by crawling or “bum shuffling”, the latter of which may delay independent walking. ‘Stiff running’ may be observed from 16 months. Walking down steps (non-reciprocal) may be observed from 20 to 24 months, and walking up stairs using alternate feet from around 3 years. A mature gait is not usually reached until the age of 7, prior to which a toddler’s gait is observed. This consists of a wider base, often a toe to heel foot pattern and a much higher cadence. It may be that a limp cannot be readily appreciated in a slowly ambulating child and may only present itself when he or she walks much quicker or runs.
A systematic approach to the child’s gait should be adopted i.e. general cadence, stance and swing phases of each lower limb and then looking up from foot to trunk and back down.
The most common abnormal gait is an antalgic gait with the stance phase being shortened on the painful limb and a reciprocal longer stance phase on the unaffected side. In cases of back or “spinal” pain, a very slow and wary gait may be observed.
A Trendelenburg gait is observed when the abductors have limited function due to weakness, mechanical disadvantage, pain inhibition or a combination of all three. The pelvis is seen to tilt away from the affected side with a compensatory movement of the trunk towards the affected side. When no pain is present, the length of the stance phase is normal; often a Trendelenburg gait will only be seen when the child has walked for a longer period of time.
With proximal muscle weakness, the child will walk with an increased lumbar lordosis and will display Gower’s sign (climbing up their body using their hands) on getting up to walk. A spastic gait is most readily recognised when toe walking or scissoring is displayed; however many more subtle signs can be displayed dependent on the muscle groups affected. Again a longer period of observation and asking the child to walk faster may be the only way of revealing the abnormality. A short limb may be recognised from compensatory toe walking on the shortened limb and/or continued flexion of the longer limb at the hip and/or knee.
If the limp cannot be identified, then asking the child to hop with or without assistance may identify the affected limb. With children younger than 3 who usually cannot hop, lifting them up and down from a standing position will often lead to them not placing the affected limb down when landing.
The spine should be inspected for abnormal curvature, swelling, erythema and paraspinal spasm both in the standing and sitting positions. If the child is asked to pick something up from the floor and they have a painful back, they may do so by flexing at the hips and knees keeping their spine stiff and protected.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








