Figure 4.1
(a) Clinic photograph of a pseudarthrosis of a clavicle. Notice the prominent lump on the right hand side. (b) Radiograph of the same patient. Notice the prominent sternal half of the clavicle (Reproduced from Benson et al. Children’s Orthopaedics and Fractures, 2009, Springer)
The main differential diagnosis is a clavicle fracture. This generally presents with pain, a history of a birth disorder and callus on the radiograph.
Surgical options are rarely indicated. Cosmetic issues from the lump are the primary indication for intervention.
Sprengel Deformity
Also known as “congenital elevation of the scapula”, this is the most common congenital malformation of the shoulder girdle and has a male to female ratio of 3:1. It is associated with malposition and dysplasia of the scapula. The condition is generally sporadic and most commonly affects the left side, although it may also be bilateral. Associated malformations are often present with this condition. These include scoliosis and upper extremity anomalies. Approximately one third of patients with Klippel-Feil disease will have a Sprengel deformity (Fig. 4.2).
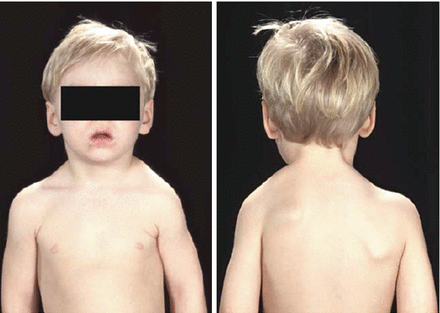

Figure 4.2
A child with Sprengel’s deformity of the shoulder (Reproduced from Benson et al. Children’s Orthopaedics and Fractures, 2009, Springer)
Clinically they present with shoulder asymmetry. The affected scapula is elevated and adducted and the inferior pole rotated medially. Scapulothoracic movements may be severely limited. Indications for surgical treatment are when there are significant cosmetic concerns and significant loss of shoulder abduction in children under 6 years of age. During surgery, the dorsal scapular nerve, spinal accessory nerve and the suprascapular nerve are all at risk.
Elbow
To aid with diagnosis and management, knowledge of the secondary ossification centres around the elbow is paramount as the elbow often presents diagnostic problems. The most commonly used mnemonic for the sequence of ossification is CRITOL.
C
Capitellum – 3 years.
R
Radial head – 5 years.
I
Internal (medial) epicondyle – 7 years.
T
Trochlea – 9 years.
O
Olecranon – 11 years.
L
Lateral epicondyle – 13 years.
Congenital Radial Head Dislocation
This is the most common congenital anomaly of the elbow. The aetiology is unknown. The direction of dislocation is anterior in 45%, posterior in 45% and in 10%, there is a lateral dislocation. They are often bilateral and patients have minimal functional limitations. They may become painful in adolescence due to degenerative changes. 60% are related to other abnormalities or syndromes, e.g.:
Arthrogryposis.
Larsen syndrome.
Cornelia de Lange syndrome.
Nail-patella syndrome.
Clinically the patient has restricted forearm rotation and elbow extension. Radiological findings show that the radial head is dome shaped and there is mild bowing of the proximal ulna. Non-operative treatment is recommended, but if the patient remains symptomatic after skeletal maturity, radial head excision can be considered. Complications associated with earlier resection are postoperative radioulnar synostosis, cubitus valgus deformity, valgus instability and proximal radial migration.
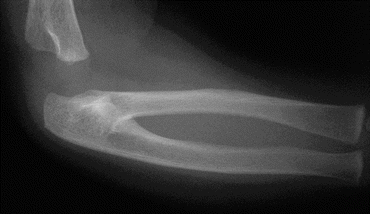

Figure 4.3
Radiograph of a proximal radioulnar synostosis, which results from the failure of completion of the distal-to-proximal separation of the forearm mesenchyme
Radioulnar Synostosis (Fig. 4.3)
This condition is usually bilateral and has an autosomal dominant inheritance. It results from failure of segmentation of the radius and ulna. Patients present with a fixed position of the forearm, ranging from neutral rotation to severe pronation. When the condition is mild there is little disability; however when there is severe pronation, it can have a significant impact on activities of daily living.
Attempts at resection of the synostosis to restore rotation have on the whole been unsatisfactory. Rotational osteotomy either distal to the synostosis or through the synostosis, fixing the forearm in a functional position have been advocated.
Panner’s Disease
This condition begins with necrosis of the capitellum and is followed by regeneration and reossification. The lesion is usually noted in the anterior central capitellum where it is in maximal contact with the head of the radius. Usually the capitellar epiphysis assumes a normal appearance. The mainstay of treatment is non-operative.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








