Rehabilitation after fracture
Other issues to consider during rehabilitation
INTRODUCTION
Older adults are the fastest growing segment of the United States and global population, and so the prevalence of geriatric fracture and the associated healthcare and societal costs can be expected to increase in commensurate fashion.1,2 As older adults in general have a more limited functional reserve, a fracture in this patient population can have significant adverse consequences, including loss of independence, institutionalization and even an increased risk of death. Hip fracture is the archetype of this phenomenon; in the year following hip fracture up to 50% of older adults may be institutionalized, while reported mortality rates range from 12% to 35%.3,4 Other fragility fractures associated with increased morbidity and mortality include spine, proximal humerus and distal forearm fractures.4 However, even a relatively minor fracture of an older adult’s dominant hand may have a marked impact on an older individual’s functional independence if they are, for instance, living alone with no family or social support. Rehabilitation is the process of restoring function, and the primary goal of a rehabilitation program in an older adult who has sustained a fracture is to optimize their functional recovery to at least, if not above, their pre-fracture level. For those living in the community, this goal would include returning to their previous living setting.
The purpose of this chapter is to present the key principles and components of a post-fracture rehabilitation program for geriatric patients. This includes a review of the main components of a rehabilitation assessment in an older adult patient, the key elements of a rehabilitation program including the healthcare practitioners involved in the rehabilitation process, the continuum of rehabilitation care post-fracture, including the rehabilitation facilities where post-fracture rehabilitation can occur, and other considerations during rehabilitation. It is beyond the scope of this chapter to discuss the rehabilitation program for all types of fractures, however the key principles and components of a post-fracture rehabilitation program are reviewed. A rehabilitation program should be tailored to each individual patient. It should also be recognized that a formal structured rehabilitation program is not necessary for all geriatric fracture patients merely because of their age. However, as older individuals tend to be at greater risk for functional compromise, even a minor fracture may offer an opportunity for a thorough geriatric assessment and initiation of preventive measures (e.g. osteoporosis evaluation and falls prevention).
REHABILITATION ASSESSMENT
While it has only relatively recently been reported that geriatric and orthopaedic co-management of hip fractures results in better outcomes with reduced healthcare costs, it is certainly reasonable to institute this type of management paradigm for other geriatric fracture patients.5,6 However, as there are not enough geriatricians to manage all such patients, other physicians, including primary care specialists, will need to become familiar with these management programs. Fortunately, the standard rehabilitation assessment regimen typically encompasses many of the same elements as a comprehensive geriatric assessment.7,8
While this comprehensive assessment is perhaps more critical for individuals sustaining a major fracture (e.g. hip fracture), the key components of the rehabilitation assessment described below should be considered in all geriatric fracture patients, regardless of the particular type of fracture.
Pre-morbid function, cognition and family/social support
Compromised pre-fracture function and cognitive impairment have been identified as negatively impacting recovery from hip fracture and other geriatric fractures.4,8,9 Similarly, having better social support, such as family or friends available to provide physical assistance, is associated with more positive outcomes in hip fracture patients. Consequently, it is important to determine an older individual’s baseline physical function, cognitive status and available family/social support.
Physical function is assessed by inquiring as to an individual’s ability to perform both basic and instrumental activities of daily living (ADL) before their fracture. Basic ADL include eating, grooming, bathing, toileting, transferring and walking, while instrumental ADL include more advanced activities such as shopping, driving/community transportation and managing personal finances. Basic ADL function may be assessed with either the Katz Index or the Barthel Index, while the Lawton instrument is often used to rate instrumental ADL function.10,11 and 12 Assessment of ADL function should include ascertaining the amount of assistance, if any, required for each activity. This would include determining whether gait assistive devices (e.g. cane or walker) had been necessary, as post-fracture ambulatory function might be adversely impacted. For instance, in a patient who before the fracture utilized a walker for ambulation, a upper extremity fracture necessitating temporary non-weight bearing will require that an alternative means of mobilization will need to be identified (e.g. motorized scooter). As functional assessment is a standard part of physical or occupational therapy evaluation, this information may be obtained from or confirmed by these therapy specialists. Finally, the functional evaluation should also include inquiry as to the patient’s status regarding driving (e.g. previous driver, plan to return to driving), as well as avocational (or vocational) activities. The ability to return to these activities can be particularly satisfying for many individuals; driving in particular affords freedom and thus many patients are eager to return to this activity.
Implicit in a functional evaluation is ascertainment of the individual’s physical residence as it is vital to understand what obstacles may need to be overcome for them to return their prior living setting. This is particularly critical for individuals living in the community. For instance, for a patient living in a multi-level residence and unable to negotiate stairs after a fracture, it must be determined how the patient will access all essential living space (i.e. kitchen, bathroom and bedroom) for their basic ADL activities. All options should be considered, and may include, for instance, temporary home modification (e.g. bedside commode in the bedroom), assistance from family/friends (e.g. to mobilize the patient or provide meals) or temporary residence in a more accessible setting (e.g. a sibling’s one-level home). Also, while it may be assumed that the patient will be returning to their previous living setting, this should be confirmed with the patient and their family (or other social support system). For instance, it may have been recognized that the patient’s ability to remain living independently was rather tenuous and institutional settings (e.g. assisted living) had recently been considered.
Current and pre-fracture cognitive status are obtained as part of the rehabilitation assessment to determine if there is any baseline dysfunction, or any significant change since the fracture. Mild cognitive impairment may not have been overtly identified pre-fracture and may only become apparent on investigating the patient’s cognitive status with family and/or friends. Delirium is quite common in older hospitalized patients and has significant adverse consequences. The symptoms of delirium (e.g. memory impairment and disorganized thinking) may persist for weeks and may adversely impact on an individual’s ability to participate in rehabilitation activities. Thus, this syndrome should be proactively identified and managed.13
Current function and functional limitations secondary to fracture
In order to determine what functional elements require improvement, one must determine the post-fracture patient’s current level of function, as well as any temporary functional restrictions and long-term prognosis. If temporary weight bearing or joint range of motion restrictions are in place, the timing for progression and/or discontinuation of the restrictions should be determined. The expected timing of follow-up evaluation with the orthopaedic surgeon should be clarified as well.
In a typical hospital setting, the current functional status of a patient is most commonly ascertained via a physical or occupational therapy consultation. Frequently, this is initiated immediately after surgery by the orthopaedic surgeon as the benefits of early mobilization are well recognized. The orthopaedic surgeon will include any relevant weight bearing restrictions; however, if there is any confusion the orthopaedist should be contacted directly for clarification. A recent review indicates that compliance with weight bearing restrictions is generally poor, but early weight bearing may be well tolerated and result in an earlier return to function for lower extremity periarticular fractures.14
If appropriate, wound care management plans including timing of suture/staple removal should be obtained from the orthopaedist. In concert with wound management, a pressure ulcer prevention program should also be considered, particularly for patients with limited mobility. As some orthopaedic surgeons have preferred post-operative care methodologies, additional patient management issues including the pain management regimen and venous thromboembolism (VTE) prophylaxis may be clarified with the orthopaedic service as well. Alternatively, if a geriatrician is co-managing or providing primary medical management, then this information can be obtained from him/her.
Medical comorbidities and medication review
This includes a review of current active medical problems and medications. For virtually all older fracture patients this affords an opportunity to make sure an osteoporosis evaluation is initiated as well as treatment if warranted (see Chapter 10).
As noted, it has been recognized that management of older adults sustaining a fracture is better when geriatricians co-manage these patients with an orthopaedist. Co-management of these older fracture patients has been reported to result in improved outcomes and reduced cost.15 In the situation in which a hospitalized patient is transitioning to a post-acute care rehabilitation facility, continued primary medical management by the same geriatrician (or geriatric team) would be optimal. However, if the primary medical team will not be continuing to manage a patient, it is critical that the accepting rehabilitation service obtain a complete and accurate discharge summary including pertinent medical conditions managed during the acute care hospitalization, complications, current active medical conditions, past relevant medical conditions and a current list of medications including any planned modification (e.g. date/timing of VTE prophylaxis discontinuation). For facilities with a linked electronic medical record, review of this information may be more convenient, although the primary team may need to be contacted directly if there are any questions regarding the management plan.
REHABILITATION PROGRAM
As with any other fracture patient, post-fracture rehabilitation and recovery in an older adult should begin promptly after the fracture has been stabilized regardless of whether surgical repair was necessary. The post-fracture rehabilitation process is particularly important for older adults due to their greater risk for adverse consequences. However, it is also critical to recognize physiological age as opposed to chronological age. It should be readily apparent that, almost irrespective of the type of fracture, the functional reserve and prognosis, for example, of a 90-year-old community dwelling, functionally independent individual who is regularly engaged in vigorous exercise is most certainly greater than that of a frail 65-year-old with multiple medical comorbidities requiring assistance for bathing even before their injury. The development of an individualized rehabilitation program, including the requisite therapy resources, requires identifying each individual’s functional deficit as obtained from their rehabilitation assessment, the likelihood of full functional recovery, and an assessment of their living setting (e.g. home or apartment) and available social supports (e.g. family).
Each individual patient’s functional deficit and resultant rehabilitation needs will depend in large part upon the extent and severity of their injury and their functional reserve. Fractures may range from relatively minor single bone injuries (e.g. metacarpal or phalanx fracture) to fractures associated with substantial morbidity and mortality (e.g. hip fracture) and multiple fractures associated with a major traumatic event (e.g. motor vehicle collision). Rehabilitation may be an informal process for minor fractures in a patient with substantial functional reserve and multiple family members available to provide assistance. Alternatively, individuals sustaining multiple or severe fractures related to a major traumatic event will often require ongoing direct medical care and a multidisciplinary rehabilitation program after discharge from the acute hospital setting (e.g. transfer to inpatient rehabilitation) with eventual transition to a community setting with continuation of therapy and medical management.
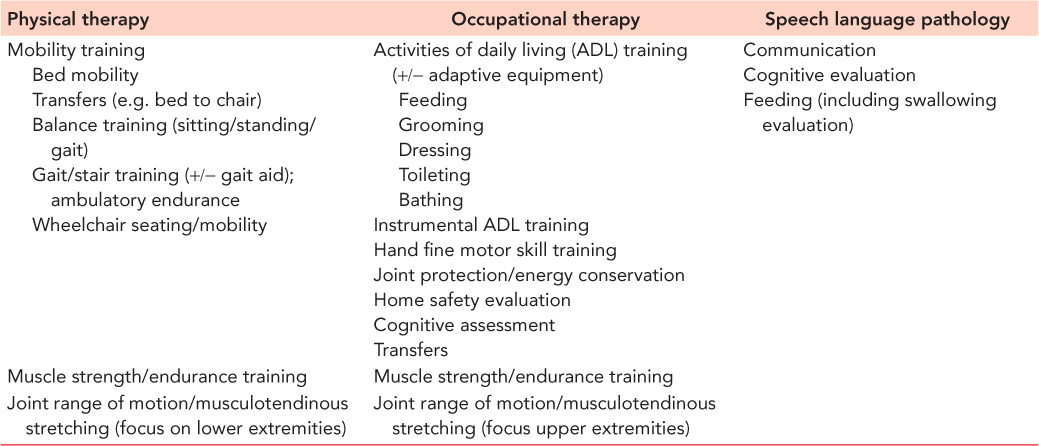
Determining the rehabilitation needs of a fracture patient requires a thorough functional history to ascertain the individual’s pre-morbid function and an evaluation of their current functional capability. From this assessment, one can identify the patient’s functional deficits and the rehabilitation provider(s) most well suited to address these deficits. Table 8.1 delineates the functional scope of physical, occupational and speech therapists. Physical therapists primarily focus on lower extremity function, including mobility and ambulation, while occupational therapists address basic ADL functional training; therapists with dedicated expertise in recovery of hand function are often occupational therapists, although some physical therapists may have expertise in this area as well.
For the patient in the acute hospital setting with an apparent functional deficit, it is recommended to obtain a therapist consultation to determine an individual’s current functional ability, to provide training and/or equipment to improve their function and to assess their tolerance for therapy in case transfer to a post-acute rehabilitation facility is a consideration. Typically, physical therapy is initially consulted, as ambulation is the functional activity of greatest concern to patients and clinicians. However, for a patient with an upper extremity fracture and an evident basic ADL deficit, an occupational therapy evaluation may be more appropriate. In the acute hospital setting, therapists with orthopaedic expertise are typically readily available and therapist evaluations may be components of standard post-fracture order sets. For patients for whom discharge to a post-acute care rehabilitation facility is being considered, a physical medicine and rehabilitation (PM&R) physician (i.e. physiatrist) may be consulted to assist in identifying the optimal facility for a particular patient. As a PM&R physician consultation service may not always be available, alternative options may include recommendations from the patient’s physical and/or occupational therapists, or from a nurse evaluating patients on behalf of a rehabilitation facility. In many outpatient orthopaedic practices, physical and occupational therapists are co-located on site and referral is also frequently part of a standardized care plan.
Table 8.1 Functional scope of physical, occupational and speech therapists
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








