Clavicle fractures
Epidemiology and fracture types
Associated injuries and comorbidities
Clinical evaluation of the elderly patient with a clavicle fracture
Clavicle fracture management options: special considerations in the elderly patient
INTRODUCTION
Non-operative management is the mainstay of treatment for most fractures of the clavicle in elderly patients. The decision to pursue surgery in the elderly patient is influenced by medical and social factors. Biological and technical factors related to fracture patterns unique to osteoporotic bone are also a consideration. The goals of orthopaedic surgery, which are typically to achieve a united fracture with good alignment, must be balanced with a thorough appreciation of the risks, needs and expectations of the elderly patient with a clavicle fracture.
EPIDEMIOLOGY AND FRACTURE TYPES
Fractures of the clavicle account for approximately 2.6–4% of all fractures, and 35–44% of all fractures involving the shoulder girdle, making it one of the most commonly fractured bones in the human body.1,2 and 3 In 1967, Allman published an anatomic classification system of clavicle fractures, dividing the clavicle into medial third, middle third and lateral third types.4 Several variations of this system have been proposed which account for more specific morphological patterns such as comminution and degree of displacement including the AO/OTA system,5 but none have taken into account the factors of patient age (paediatric vs elderly) or bone quality (i.e. osteoporosis).
Bone quality declines slowly after 30 years of age and osteoporosis most commonly develops after the age of 50.6,7 Osteoporotic bone is known to have a greater propensity to fracture, and elderly patients have a greater propensity to fall.8,9 Taken together, it would seem that clavicle fractures would be most likely to occur in elderly individuals. Surprisingly, this is not observed in practice, as clavicle fractures are most commonly observed young males.1,3,10 However, there is a second, smaller peak in elderly patients, and this peak has nearly equal male and female preponderance (Figure 19.1). In the young male population, the mechanism of injury is most commonly a sporting injury or motor vehicle crash, whereas simple falls are the most frequent mechanism in older patients.3,10,11
Between the ages of 18 and 30, medial third fractures account for 2% of all fractures, middle third 80% and lateral third 18%.3 Among patients aged 61 and over, 10% of clavicle fractures involve the medial third, 67% the middle third and 23% the lateral third.3 Therefore, while middle third fractures remain the most common subgroup, there is a higher proportion of both lateral and medial third clavicle fractures in the elderly compared to the younger population.10
For midshaft fractures, patients over 50 have a higher incidence of comminuted and displaced fractures than patients below 50.11 Since the fracture mechanism is more commonly low energy in older patients, the increased complexity of fracture morphology in elderly patients can likely be attributed to poor bone quality.
ASSOCIATED INJURIES AND COMORBIDITIES
Comorbidities and associated injuries frequently complicate both the management and outcome of trauma in the elderly. Clavicle fractures, particularly those associated with higher energy trauma, are commonly associated with other injuries.12 Elderly patients have less ability to tolerate these injuries, which is reflected by the finding in the orthopaedic literature that the elderly are 4–4.6 times more likely to die than younger patients as a result of a traumatic event of similar severity, and age older than 65 years is an independent predictor of death after trauma.13
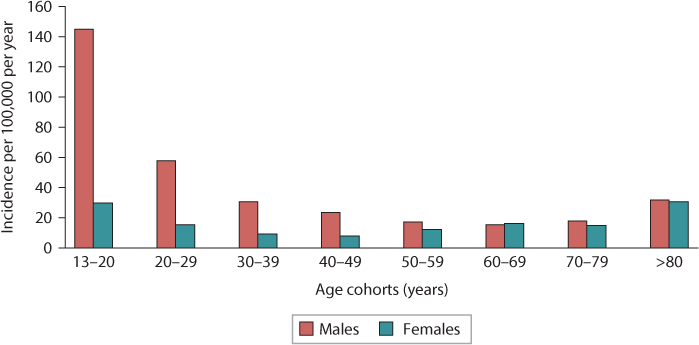
Figure 19.1 Epidemiology of clavicle fractures according to gender and age (From Robinson CM. J Bone Joint Surg Br. 1998;80:476–84. Reprinted with permission and copyright of the British Editorial Society of Bone and Joint Surgery.)
The presence of a clavicle fracture may be a particular sign of associated injuries and subsequent poor outcomes in higher energy geriatric trauma patients. Of all long bone fractures, the presence of a clavicle fracture is the strongest predictor of mortality in the geriatric trauma population, with a mortality rate of 23% in those patients (compared to a mortality rate of 13% in geriatric trauma patients without clavicle fractures).12 In contrast, young major trauma patients with clavicle fractures have a mortality rate of only 7%.
Interestingly, while associated injuries are found in greater prevalence in the population of elderly high-energy trauma patients,14,15 this may not be the case with high-energy clavicle fracture patients. In a recent study by Keller et al., geriatric patients with clavicular fractures had an average admission Injury Severity Score, Glasgow Coma Scale score, and Brain, Thorax, and Lower Extremity Abbreviated Injury Scores that were worse compared with the average scores of elderly or younger patients without clavicle fractures, but were similar to the average scores of younger patients with clavicle fractures.12 The authors concluded that the increased mortality rate in elderly clavicle fracture patients is due to the associated injuries being less well tolerated by the elderly, rather than the associated injuries being more severe in the elderly.
CLINICAL EVALUATION OF THE ELDERLY PATIENT WITH A CLAVICLE FRACTURE
History
The same principles apply to history taking for the elderly patient as for younger patients, and some may argue that the history is even more important in the elderly patient. The history is important both for determining the diagnosis and for deciding on treatment. One must bear in mind that due to the prevalence of osteoporosis, lower energy injuries may lead to significant fractures in the older patient, and therefore descriptions of a relatively benign fall should not diminish the surgeon’s suspicion for fracture. Similarly, geriatric patients are often better able to tolerate clavicle fractures and their sequelae and are frequently far less symptomatic (and in some cases asymptomatic) compared with younger patients1; therefore in elderly patients, the absence of pain should not lead the surgeon to rule out a fracture without carrying out a thorough work-up.
In addition, it should be remembered that a fall in an elderly person might have resulted from a cardiac or neurological event that may require further investigation and treatment, especially if surgical intervention is contemplated.
Despite the importance of history, unfortunately, history taking can be challenging if dementia or delirium is present. In these cases, witnesses or family members may be able to describe the injury in order to indicate to the physician the injured body part. As important as identifying the injured body part is determining the patient’s baseline functional level and daily physical demands, which are crucial in order to decide on the best treatment plan.
Physical examination
The physical examination of the clavicle is no different for elderly patients than it is for the rest of the population and includes observation of skin abnormalities (swelling, bruising, ecchymosis and deformity), palpation for pain, an upper extremity neurological examination and a thorough shoulder evaluation (within the patient’s limitations) in order to rule out concomitant injury to the shoulder girdle.
What is different is that greater attention should be paid to the general physical examination of the other body systems. This is important for two reasons. First, it can rule out injury to other body systems that, if missed, may lead to worse consequences than in the younger patient. Second, it may identify underlying comorbidities, which are more common in elderly patients and play a large role in determining the appropriate treatment. If surgery is being considered, an underlying comorbidity may be identified which may alter the risk–benefit ratio of surgical intervention and affect the decision to proceed.
Imaging
Anteroposterior (AP) radiographs of the clavicle are sufficient to diagnose clavicle fractures and should be performed in all elderly patients complaining of shoulder pain after trauma. A chest radiograph may also suffice, and in some cases provides additional information by including the contralateral clavicle for comparison, and will likely be needed as part of the preoperative evaluation if surgery is being considered. Surgical decision-making is aided by assessing displacement on the AP view; however, this can be misleading as the deformity may occur in the AP plane and thus the true displacement will be masked by bony overlap. Dedicated views such as the Zanca view (cephalic tilt of 15 degrees) can be particularly helpful in this regard and are also used for lateral clavicle fractures (as well as direct views of the acromioclavicular joint) in order to avoid overlap from the upper ribs.16 This is a standard part of our evaluation of these injuries.
As is the case with younger patients, advanced imaging of the clavicle such as CT scanning is rarely required, except in cases of medial clavicle fracture or dislocation, or to evaluate for associated fractures in the shoulder girdle. However, in elderly trauma patients who often receive a chest CT in the emergency department, the scan should be carefully scrutinized for a clavicle fracture, as these are a prognostic marker for increased mortality in the geriatric population.12
CLAVICLE FRACTURE MANAGEMENT OPTIONS: SPECIAL CONSIDERATIONS IN THE ELDERLY PATIENT
Non-operative management
Non-operative management remains the mainstay of treatment for all non-displaced or minimally displaced fractures of both the midshaft and distal clavicle in elderly patients. The decision of when to consider surgery is complex and discussed below, although even displaced fractures may be successfully managed non-surgically in the elderly. Several points should be considered that are unique to the elderly patient with a clavicle fracture being treated non-operatively.
A standard protocol for non-operative management of both midshaft and distal clavicle fractures is the use of a conventional sling for 4–8 weeks, with active self-assisted stretching exercises initiated when fracture healing is established.8,17 The sling must be worn with adequate padding, as elderly patients lose collagen and fat within the subcutaneous layer of the skin, making the skin vulnerable to frictional or pressure-related injury from the shoulder strap, which has been reported.18 In addition, the effect of the sling on the independent function of an elderly patient must be considered.
Operative indications
The role of surgery for displaced midshaft clavicle fractures is still debated. Numerous prospective and randomized studies demonstrate improved functional outcomes for certain subsets of patients treated with surgical management of displaced midshaft clavicle fractures, as well as a reduced incidence of non-union and malunion.16,19,20,21 and 22 As observed in a recent large-scale population study, the dissemination of this information led to an increase in the number of clavicle fractures treated operatively in the past decade.23 This study excluded patients over the age of 60, therefore it is not known if this trend has occurred in elderly patients as well.
Similarly, there is ongoing debate regarding the appropriate indications for operative treatment of distal clavicle fractures in patients of all ages. Non-operative management is the mainstay for non-displaced fractures, but displaced fractures have a high rate of non-union.24,25 Surgery reduces the risk of non-union for displaced fractures,26 but several studies have shown similar outcomes in patients treated with surgery or non-operatively (Figure 19.2).27,28 and 29
The issue of choosing surgery over non-operative treatment for clavicle fractures (both midshaft and distal) is considerably more complex in the elderly patient. Osteoporotic bone might be more prone to delayed and non-union.17,30 Elderly patients have more comorbidities and anaesthesia poses a greater risk. Older patients are also more prone to postoperative delirium and confusion. The soft tissues are thinner and more prone to dehiscence and wound complications, which in turn can lead to colonization or infection. The bone is weaker, and thus more prone to failure of fixation. Physical demands are usually much less, making the problem of non-union (or malunion) less of a functional deficit compared to a younger person who engages in manual work or sport. Finally, non-union of the clavicle seems to be more readily tolerated in elderly individuals compared to younger patients (Figure 19.3).
In 2004, a study by Robinson et al. followed a cohort of 101 patients who had sustained displaced distal clavicle fractures and were treated non-operatively.28 At 7–24 months after injury, 14 patients had severe persistent symptoms and underwent delayed surgical treatment. The remaining 87 patients never progressed to surgery, and the non-union rate in those patients was 21%. Surprisingly, there was no difference in the Constant or SF-36 scores between those who had delayed surgery, those who developed non-union with non-operative management and those who healed with non-operative management. These results suggest that an initial trial of non-operative management seems prudent in the large majority of displaced clavicle fractures, and that the indication for surgery should be unacceptable symptoms that can be addressed with surgery, and it might be wise to wait a year.
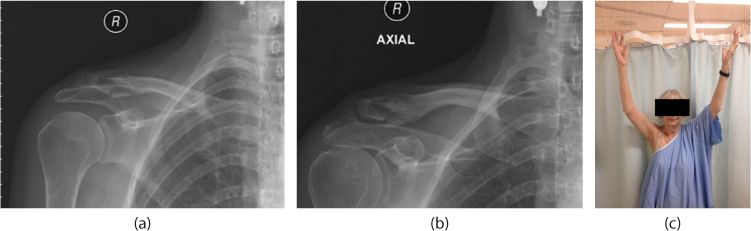
Figure 19.2 (a) A displaced distal clavicle fracture. The 75-year-old low demand patient was treated non-operatively with a sling for 4 weeks followed by progressive passive, then active range of motion exercises and return to full activity by 3 months. (b) The same fracture at 6 months after injury, demonstrating non-union. (c) Despite the non-union, the patient is asymptomatic with no pain and has an excellent range of motion.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








