Fig. 1
Trunk lean

Fig. 2
Supine walkouts on ball
Greater Trochanteric Pain Syndrome
Greater trochanteric pain syndrome (GTPS) includes a number of disorders of the lateral hip, including trochanteric bursitis, tears of the gluteus medius and minimus muscles, iliotibial band syndrome, and external coxa saltans (snapping hip) [21]. Patients typically present with pain and tenderness in the region of the greater trochanter, buttocks, or lateral thigh. During clinical examination, passive range of motion often causes minimal pain, while active motions of the hip tend to be more painful. Muscle length assessments may show adaptive shortening especially of the hip abductor and hip flexor muscles. Weakness of the hip abductor muscles is common, and it is recommended to assess the patient’s strength in both open- and closed-chain positions. Caution should be used to not overload joint structures if testing in long lever side-lying positions. Single limb stance may reveal a hip drop (Trendelenburg sign) (Fig. 3) or excessive elevation of the contralateral pelvis (compensated Trendelenburg sign) [22]. During gait assessment, one may observe movement compensations in all planes of motion but most commonly in the frontal plane. Patients often excessively rotate through the pelvis and lumbar spine in order to compensate for limited extension of the hip, especially noted during the late to terminal stance phases of gait.
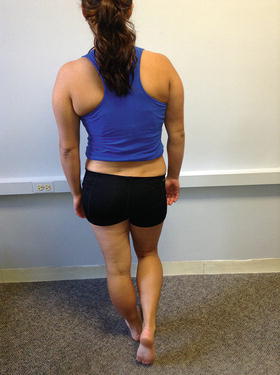

Fig. 3
Trendelenburg
Conservative management of GTPS starts with decreasing irritation of the lateral hip with manual therapy techniques, pain relieving modalities, and regaining normal range of motion. Manual techniques should include stretching into hip adduction, internal rotation and extension, cross friction mobilization to the gluteal tendons, and deep tissue techniques to the lateral hip musculature and tensor fasciae latae. Once acute irritation has been addressed and range of motion normalized, the clinician needs to assess the biomechanics of the trunk and lower extremity. Reduced neuromuscular control of the trunk commonly causes compensatory movements, throughout the lower extremity chain; therefore, core stabilization is very important for these patients. Exercise progressions to address these muscle imbalances include strengthening the hip muscles in the closed chain position using verbal, tactile, and/or demonstrative cues on pelvic, trunk, and lower extremity position to encourage appropriate activation patterns. Initial dynamic activities include gait retraining exercises and dynamic multiplane progressions. Other dynamic activities may include active pelvic depression and hip hiking standing on the involved side (Fig. 4). Appropriate hip strength progressions include supine bridging series, side plank series, and squats progressing from double to single leg focusing on control throughout the entire movement [23].


Fig. 4
Hip hiking
Internal and External Snapping Hip Syndromes
Internal snapping hip syndrome results from the iliopsoas tendon snapping over the iliopectineal eminence of the femoral head as the femur moves from a position of flexion to extension. External snapping hip syndrome results from the iliotibial band snapping over the prominence of the greater trochanter while actively moving the thigh into flexion and then into extension [23]. These syndromes are more prevalent in a younger population and typically occur between the ages of 15–40 years. Imbalance between the agonist and antagonist muscle groups of the hip and trunk often precedes this injury, and commonly patients demonstrate weakness or improper firing of the core musculature with functional movements.
Passive range of motion of these patients is commonly unremarkable. Mechanical symptoms are usually only reproduced with active movement, and external snapping can be reproduced in standing by moving the pelvis into hip adduction [23]. Initial treatment includes addressing muscular asymmetries of the deep abdominals, iliopsoas, and hip abductor muscles. It is critical if the patient demonstrates transverse abdominus weakness to retrain to maintain pelvic neutral with all movements of the pelvis over the femur. Initial core exercises consist of eccentric training of the hip flexors and abdominals by performing trunk leans with the feet on the floor while sitting on a stool or therapy ball. Progress the core exercises by adding short lever-arm lower extremity exercises such as bent knee flexion and small lower extremity movements while cueing the patient to maintain a neutral lumbar position by recruitment of the deep abdominals. Strengthening is progressed to involve more challenging abdominal tasks including plank progressions, prone walkouts on the therapy ball to tuck positions (Fig. 5), and abdominal exercises with the lower extremities lifted. For all strengthening exercises, it is required to cue the patient to maintain lumbar neutral with strong abdominal and gluteal control.


Fig. 5
Walkouts to ski tuck
Hamstring Injuries
Injuries to the hamstring muscle and tendons can occur traumatically from an eccentric muscle overload at the end range of hip flexion with the knee in a position of extension or chronically through overuse. It is important for clinicians to fully identify the mechanism of injury in order to structure treatment interventions to address the underlying contributing impairments.
An acute hamstring muscle or tendon injury often results in ecchymosis of the posterior thigh and leg. Severe swelling and ecchymosis may indicate a torn proximal hamstring tendon and should be evaluated with an MRI. The indications for proximal hamstring repair are rupture two or more tendons and/or greater than two centimeters of displacement from the ischial tuberosity. In general, orthopedic surgeons want to repair within 2 weeks to minimize risk to adhesions to nearby structures (i.e., sciatic nerve). Examination will reveal shortening of the hamstring musculature with pain and muscle guarding. Palpation will clarify the exact location of the tear. In severe cases, reduced hamstring strength when compared to the opposite side will be present.
Conservative management of acute hamstring injury includes addressing ecchymosis and edema through soft tissue massage, compression, and modalities such as electrical stimulation and pulsed ultrasound. Once the patient is out of the acute phase, 3–5 days post injury, gentle passive range of motion into hip flexion and extension may be initiated, followed by isometric strengthening in a closed-chain position. Caution should be taken in the acute phase to gently stretch the lower extremity to end range hip flexion while maintaining knee flexion to minimize tension through the proximal hamstring tendons.
Chronic proximal hamstring tendinopathy occurs as a result of repetitive microtrauma. Often these patients have a history of recurrent hamstring injury and underlying neuromuscular imbalance of the pelvis, trunk, or lower extremities. Patients will complain of a deep ache in the posterior hip and buttocks, which is commonly exacerbated with activity. Hip extension and knee flexion weakness and pain with palpation to the ischial tuberosity may be present. Passively moving the patient’s hip and knee into full flexion and then slowly extending the knee will also reproduce the patients pain in the posterior buttocks.
Conservative management of chronic proximal hamstring injury should focus on soft tissue mobilization to the hamstring insertion at the ischial tuberosity. Initial strengthening exercises include hip extension bridges on a stable surface progressing to an unstable surface such as a therapy ball. The use of a pilates reformer for isolated and dynamic movements such as double leg hamstring curls and single leg marching while maintaining a bridge position is also an effective strengthening progression (Figs. 6 and 7). Additional exercises include standing double and single leg dead lifts with the knees in multiple angles of flexion. These exercises promote activation of the hamstring muscle across both the hip and knee joints simultaneously. It is important to note that because the hamstring is a two joint muscle, maximal stress is exerted in full knee extension and hip flexion. Multiplane strengthening in this lengthened position should precede the progression to jumping, landing, agilities, and cutting drills. When starting these drills, cueing the patient to land and slowly flex into the squat position will retrain the involved hamstring muscle eccentrically and will encourage equal weight bearing through both extremities.
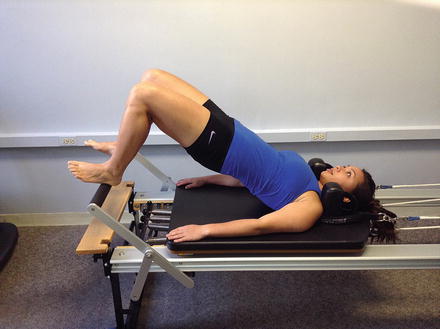


Fig. 6
Hamstring bridge on reformer

Fig. 7
Hamstring bridge with marching
Athletic Pubalgia and Osteitis Pubis
Pelvic pain syndromes as a source of injury around the hip have been found to affect 5–18 % of athletes involved in competitive sports [24]. Athletic pubalgia, or “sports hernia,” causes groin pain in the absence of an actual hernia. The etiology is an overuse injury related to repetitive rotation and commonly occurs during sports, such as hockey and tennis. Groin pain usually arises insidiously with an occasional patient report of feeling a tearing sensation in the groin. Underlying muscle imbalances in the trunk and pelvis lead to abnormal force transfers across the pelvis and lead to soft tissue tearing and injury. Initially, symptoms are reproduced only during high-level function, but as the severity progresses, pain may be reproduced during routine activities of daily living.
Osteitis pubis is defined as a separation of the pubic symphysis resulting from a series of repetitive twisting, cutting, and/or pivoting movements. Often this occurs in conjunction with frequent acceleration and deceleration that are necessitated in sports such as soccer, football, rugby, swimming, and hockey. During these repetitive movements, one can develop chronic insertional tendinosis of the adductor mass at the pubis. Weakness and poor neuromuscular control of the abdominals combined with adaptive shortening and/or hypertonicity of the adductor muscles may cause instability of the pubic symphysis [24]. These microtraumas can lead to symptom reproduction over the symphysis, medial groin, abdomen, and/or scrotum. Symptoms can be provoked with resisted adduction of the thigh, dynamic single leg activities, or dynamic abdominal activities such as a traditional sit-up [25].
Initial treatment of both athletic pubalgia and osteitis pubis should focus on minimizing aggravating positions until symptoms subside. Avoidance of lower extremity cutting, pivoting, and dynamic abdominal activities are important to allow proper healing of the pubic symphysis and tendinous insertions to the pelvis. Manual therapy can be utilized to correct any malalignment of the pelvis, decrease pain, improve muscle length, and to decrease abnormal muscle tone. Isometric strengthening can be initiated with emphasis on transverse abdominus, rectus femoris, gluteus medius, and hip adductor musculature when a patient tolerates. Once pain has decreased, progression into straight plane and subsequent multiplane strengthening should be initiated. These exercises should be performed within pain-free ranges of motion and intensity with cueing to maintain pelvic alignment. Higher-level core stabilization exercises such as planks, side planks, hip extension bridges, and trunk leans while sitting on a therapy ball are recommended as exercises which strengthen the abdominals without excessive activation of the hip flexors and adductor muscles. Often abdominal strengthening exercises in which the lower extremities are off of the ground cause more irritation to the healing pubic bones. This may be due to an increase in shearing across the pubic symphysis if imbalances are present between the agonist and antagonists muscle groups. At all times clinicians need to be assessing pubic bone and groin pain and modify the exercises if any activities or positions are painful. Once straight plane stability is established and the athlete is no longer having pain, higher-intensity training may be initiated. Sport-specific training of cutting, pivoting, kicking, skating, and jumping should always focus on maintaining proper form through the trunk and pelvis. The patient’s training program, even after discharge from therapy, should always include maintaining abdominal and core strength.
Adductor Muscle Strains
Muscle strains of the adductors can occur traumatically from an excessive eccentric activation of the muscle during a slip of the planted foot while the body moves in an opposite lateral direction. This can also occur when pivoting on a planted foot and forcefully rotating the pelvis. The patient will often feel an immediate pull or strain through the groin with pain that may radiate down to the knee. Overuse adductor injuries occur from repeated contraction of the adductor muscles to stabilize the pelvis when there is limited motion of the opposite hip or from muscle imbalances in the pelvis. Initial rehabilitation includes manual therapy to reduce pain and swelling. Gentle stretching and hip range of motion can be performed within pain-free ranges during the first few weeks of rehabilitation. Once swelling and gentle mobility are regained, closed-chain strengthening may be initiated. Double leg squats, hip extension bridge series, and balance retraining are all appropriate initial exercises. When sagittal plane motion is pain-free, the clinician can introduce lateral hip strengthening being sure to work the injured leg in both the open and closed chain. Initial lateral strengthening includes skater series exercises on a pilates reformer or slide board (Figs. 8 and 9), side stepping with a theraband at varied degrees of hip flexion, and progressing to lateral stepping over a step or balance board. Healing of injured muscles can take a number of weeks or months, and it is important to not push an athlete back into high-level activity prior to full healing. Use pain and strength as a guideline for the overall progression of return to full function.



Fig. 8
Skater series knees extended

Fig. 9
Skater series side lunge
Intra-articular Pathologies
The most common intra-articular hip injuries that can benefit from nonoperative rehabilitation include chondral defects, hip osteoarthritis, femoroacetabular impingements, and labral tears. When treating a patient with an underlying abnormal tissue or boney morphology, clinicians need to be cautious to not exacerbate symptoms due to the non-modifiable nature of these contributors to injury. To be successful with rehabilitation, it is crucial to understand which positions, movements, and functional daily activities will likely increase joint irritation and exacerbate the underlying pathology. The role of the physical therapist is to educate the patient on how to modify activity to accommodate the underlying pathoanatomy. Many patients with intra-articular hip conditions can lead an active healthy lifestyle with minimal pain if they are taught a few modifications to reduce stress across involved hip joint tissues. Teaching patients the importance of supportive and shock absorbing shoe wear for both exercise and work can immediately decrease joint pain especially in the osteoarthritic population. Additionally, it may be beneficial to instruct patients to select low impact exercises such as swimming, biking, and walking. Balance exercises and improving lower extremity proprioception are important to improve overall function. Encouraging hiking with walking poles or using an assistive device in the community can greatly benefit patients and decrease forces through the lower extremities. These lifestyle modifications in addition to reduction in body weight may decrease joint pain and minimize subsequent extra-articular irritation of the muscles surrounding the joints due to increased demands with daily function.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








