Intracapsular proximal femoral fractures
INTRODUCTION
Based on the current literature and estimates, the absolute number of hip fractures is expected to increase dramatically over the coming decades. By the year 2050, it is estimated that the total number of hip fractures world wide will exceed 6 million annually.1 For the individual patient a hip fracture may cause short- and long-term pain, impaired function and reduced quality of life. Up to 50% of the patients will not regain their pre-injury mobility, independent living may no longer be possible, and the mortality is high.
Intracapsular femoral neck fractures represent 60% of all hip fractures.2 These fractures have been one of the most extensively investigated and well-documented topics in the orthopaedic literature. However, we still do not know the best treatment for each patient and there are no generally accepted guidelines on how to manage these injuries. In recent years the treatment has shifted towards the increased use of arthroplasty and a reduction in fixation. Which patients, if any, should still have their fractures fixed? And if this is still a valid option, have we found the ideal implant and method of fixation? Treating a displaced femoral neck fracture in an elderly patient with an arthroplasty is no longer controversial. But how do we define ‘an elderly patient’? Furthermore, what type of arthroplasty should be used, and should this be a cemented or uncemented procedure? Many options are available, but there are no clear answers to these questions.
EPIDEMIOLOGY
Hip fracture incidence varies considerably both between and within countries and continents. In Europe, there is a higher hip fracture incidence in northern Scandinavian countries compared to Mediterranean countries in the south. A similar difference is found between North and South America and between countries in Asia. In Oslo, the capital of Norway, the highest hip fracture incidence ever published was found in 1988/89 (124/100,000 annually for patients aged ≥50 years).3 These numbers also represent a 50% increased hip fracture risk in Oslo compared to rural areas in the same country. The importance of increasing age, female gender, comorbidities, smoking, low body mass index (BMI) and previous osteoporotic fractures for hip fracture risk is well known. Further, the importance of sunlight and vitamin D and calcium for bone health is well established, as are the positive effects of physical activity. Genetic and ethnic differences also play an important role in the individual risk of sustaining a hip fracture.
In Norway, the average hip fracture patient is 80 years old and 72% of patients are female.2 In parts of the world where life expectancy is much lower, geriatric fractures are, for obvious reasons, less of an issue. However, life expectancy is expected to increase considerably in developing countries and the elderly population in Asia and Western countries will multiply over the coming decades. These demographic changes, despite being indicators of improved health status and better living conditions, will also bring major challenges. Providing adequate healthcare services for future generations and a rapidly growing number of elderly patients will be demanding. However, several recent studies from Western countries have actually found a decline in hip fracture incidence, for women in particular.4,5 and 6 Whether this reflects better health in general, a reduction in osteoporotic fractures secondary to medication, or other reasons, is not clear.
CLASSIFICATION
Femoral neck fractures have traditionally been classified as intracapsular or extracapsular fractures. Several classification systems have been designed to grade intracapsular fractures, based on anatomical location (subcapital or transcervical), displacement of the fracture (Garden and AO/OTA) or the angle of the fracture (Pauwels). Many authors suggest that the most reliable classification of intracapsular femoral neck fractures, both clinically and in scientific papers, is simply to divide the fractures into displaced and non-displaced.
Garden classification
The Garden classification was first described in 1961 and still is the most commonly used classification system for intracapsular fractures.7 The fractures are divided into four groups based on the type and degree of displacement on the anteroposterior (AP) radiograph (Figure 34.1). A Garden I fracture is an incomplete fracture with an intact medial calcar and valgus impaction. A Garden II fracture is a complete but undisplaced fracture. A Garden III fracture is a complete fracture with incomplete displacement, where the trabecular lines in the proximal fragment are in varus relative to those in the distal fragment and in the acetabulum. A Garden IV fracture is a complete fracture with complete displacement.
A major drawback with the Garden classification is that it has been found to have poor reliability.8,9 and 10 Several authors have advocated a simplification of the classification into non-displaced (Garden I and II) and displaced (Garden III and IV) fractures, which increases the reliability.9,10 and 11 Studies have found this simplification sufficient for clinical use, with no benefit conferred when subdividing the undisplaced and displaced fractures further.12,13 Accordingly, the simplified Garden classification is clinically relevant and is extensively used in treatment guidelines and scientific papers.
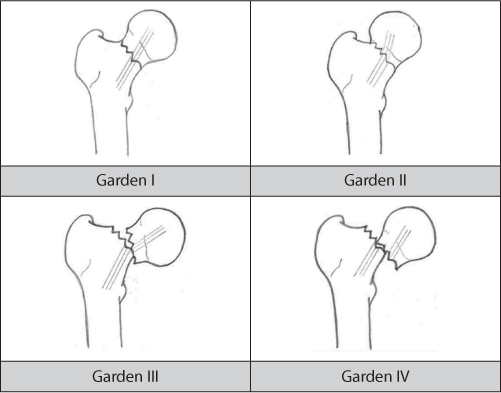
Figure 34.1 Garden classification.
Pauwels classification
The Pauwels classification was described in 1935.14 This classification uses the inclination angle between the fracture line and the horizontal line on the AP radiograph to identify three subtypes of femoral neck fractures (Figure 34.2). Pauwels type I fractures have an angle of less than 30 degrees, in type II fractures the angle is 30–50 degrees and in type III the angle is larger than 50 degrees. The shearing stress over the fracture increases with increasing fracture angle at the expense of compression forces. Pauwels consequently suggested that the greater the angle of the fracture, the greater the probability of nonunion and failure following internal fixation. However, this association has not been supported in the literature.15 There are several problems related to the use of Pauwels classification. First, to measure the fracture angle is difficult because the femur may be rotated. Second, the interpretation of the classification system in the literature has frequently been wrong.16 Finally, the reliability of Pauwels classification has been reported as fair.17
AO classification
The AO (Arbeitsgemeninschaft für Osteosynthesefragen) has developed a comprehensive classification system for femoral neck fractures according to their severity and complexity in subtypes 31 B1 to 31 B3.18 Type B1 comprises subcapital fractures with impaction or slight displacement, the transcervical fractures are defined as subtype B2 and the displaced subcapital fractures are defined as subtype B3. The AO classification has, however, not been used frequently either clinically or for research purposes, probably due to its complexity.
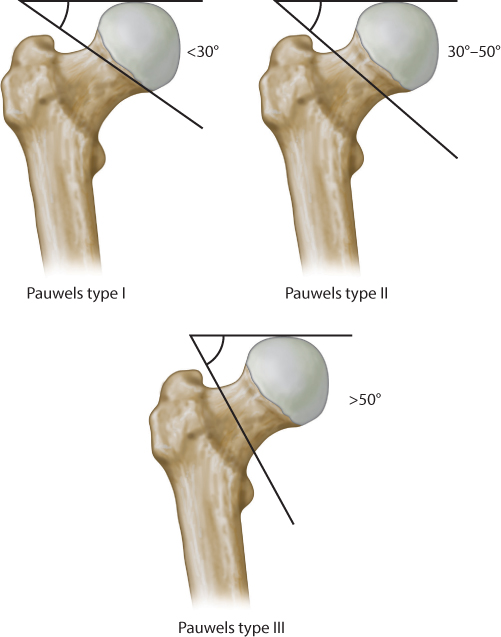
Figure 34.2 Pauwels classification.
CLINICAL ASSESSMENT
The clinical assessment of these patients can be difficult due to cognitive impairment and occult causes for the fall that may have precipitated the fracture. The patient should be assessed with a complete history and physical examination. A collateral history from family members or carers can be invaluable. The history should clearly determine both the mechanism of injury, as well as for any medical causes that have led to the presentation, e.g. arrhythmia or stroke. Be sure to establish if the patient has had a prolonged lie prior to presentation, as this can lead to a raised CK level and renal failure.
The medical and drug history should identify all pre-existing comorbidities and medications, including anticoagulants that may need to be adjusted perioperatively. An understanding of the patient’s baseline cognitive and functional status is essential.
The classic presenting features of a neck of femur fracture are hip pain, inability to weight bear and a shortened and externally rotated leg. The neurovascular status of the limb should be assessed, as well as the presence of any associated injuries. Please also see the perioperative care section below.
Imaging
Imaging should include an AP X-ray of the pelvis and a lateral view of the affected hip. Advanced imaging such as a bone scan, CT or MRI may be required when the diagnosis is in doubt or when a pathological fracture is suspected.
TREATMENT
The treatment of intracapsular femoral neck fractures should be individualized. Generally, and well supported in the literature, displaced femoral neck fractures in the elderly should be treated with an arthroplasty, and no longer with closed reduction and internal fixation.19,20,21,22,23,24,25,26,27,28,29,30 and 31 This will reduce pain, improve function and substantially lower the number of surgical complications and subsequent need for reoperations. This trend, which shifted over the past few decades from internal fixation to arthroplasty, is also reflected in data from the Norwegian Hip Fracture Register (NHFR) (Figure 34.3). It is, however, less clear which type of arthroplasty is best, and whether arthroplasties should be cemented or not. Furthermore, it remains controversial which fractures and patients may still be treated with an internal fixation. Finally, several implants for internal fixation are optional, and there is no clear consensus as to which implant should be preferred. The decision-making should be evidence based on the patient’s physiological age, functional status and a detailed analysis of the fracture pattern.
Non-operative treatment
In general, all intracapsular fractures of the proximal femur in the elderly should be treated surgically. Fractures left untreated will either have an increased risk of secondary displacement or, if primarily displaced, will cause unacceptable pain, and appropriate nursing or mobilization of the patient will be impossible. The mortality for these patients is high.
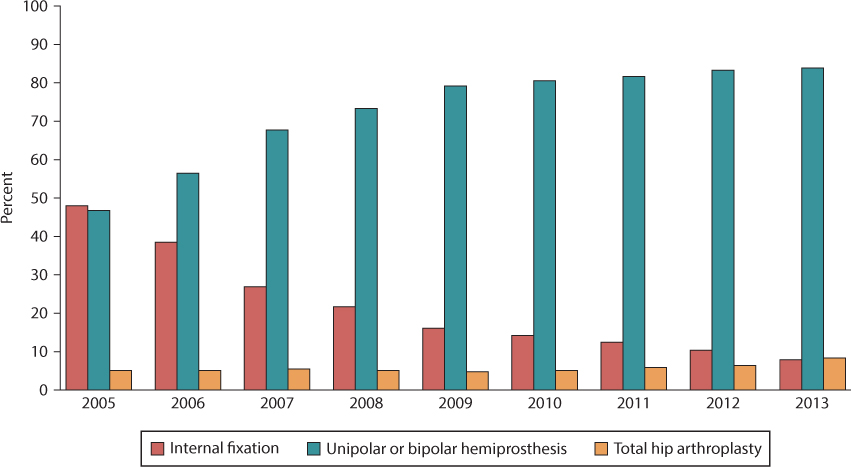
Figure 34.3 Time trends in the treatment of displaced femoral neck fractures. (Data from The Norwegian Hip Fracture Register, Annual Report 2014.)
Conservative treatment of valgus impacted or undisplaced femoral neck fractures (Garden I and II) in younger patients may have a good prognosis and acceptable rates of secondary displacement, but much higher complication rates must be expected in the elderly.32,33 In their study of 115 patients with undisplaced femoral neck fractures, Shuqiang et al. found a strong correlation between secondary displacement and age, whereas fracture instability was independent of gender, American Society of Anesthesiologists (ASA) grade and Pauwels angle.33 For patients in their seventh and eighth decade, a 48% secondary dislocation rate was found. Raaymakers found a similar correlation with age in a study of undisplaced fractures in 311 patients.32 For healthy patients <70 years of age, a 7% secondary dislocation rate was found, while 41% of the patients older than 70 years had a secondary fracture dislocation. Additionally, fracture instability was also found to be negatively influenced by comorbidities, and for patients older than 70 years of age with more than one concomitant disease the failure rate increased to 83%.
There are, however, exceptions where non-operative treatment might be considered even in the elderly. When patients are so unwell that they are not expected to survive surgery, non-operative management might be justified. Non-operative treatment should include early mobilization, and only a short bed rest if required for pain relief. Non-weight-bearing would be preferable, but if this is not possible, weight bearing as tolerated should be accepted. If pain does not subside over time, if ambulation is not possible and certainly if fracture displacement is apparent, surgical treatment should be recommended. Treating acute hip fractures conservatively with bed rest for several weeks or months should no longer be an alternative. In our practice, non-operative treatment for any kind of femoral neck fracture is very unusual, and we do not recommend it.
Internal fixation
For young patients with displaced intracapsular femoral neck fractures the goal is to preserve the native femoral head, and closed reduction and internal fixation of the fracture are generally recommended. In the elderly, however, recent literature would suggest that displaced femoral neck fractures should be treated with an arthroplasty.19,20,21,22,23,24,25,26,27,28,29,30 and 31 Compared to internal fixation, an immediate hip replacement for elderly patients will predictably reduce pain, speed up recovery, improve function and substantially lower the surgical complication rate and subsequent need for reoperations.
UNDISPLACED FRACTURES
Some 15–20% of all hip fractures are valgus impacted or undisplaced intracapsular femoral neck fractures (Garden I and II). Regardless of age and functional status of the patient, internal fixation is usually considered a good treatment option for these fractures. Percutaneous or mini-invasive surgical techniques using cannulated screws, or alternatively a sliding hip screw (SHS), are the most commonly used methods.34 Parker et al. compared 346 patients treated with cannulated screws for undisplaced intracapsular fracture to a matched group of patients treated with a hemiarthroplasty for displaced intracapsular fractures.35 They reported an increased risk of reoperation after treatment with cannulated screws compared to hemiarthroplasty, but internal fixation resulted in less perioperative complications, better functional outcome and a lower 1-year mortality. They concluded that internal fixation should be the treatment of choice for all undisplaced femoral neck fractures, even for elderly patients. Sikand et al. came to the same conclusion in their study. They found a higher mortality rate after hemiarthroplasties but more reoperations in the internal fixation group.36
Nevertheless, despite this apparent consensus on treatment, and a relatively good prognosis, mechanical failure, avascular necrosis, nonunion and hardware related pain may cause reoperation rates of 11–27% after internal fixation of undisplaced fractures.35,37,38,39,40 and 41 In addition, the studies defining current treatment standards for undisplaced hip fractures were mostly based on old and uncemented prostheses with well-documented inferior results. Today, these prostheses should probably no longer be used. The results in favour of internal fixation in such studies should therefore be interpreted with caution.
A recent observational study from the NHFR found that patients with undisplaced fractures treated with cannulated screws had a poorer clinical outcome and a significantly higher reoperation rate after 1 year compared to a similar group of patients treated with contemporary hemiarthroplasties for displaced femoral neck fractures.39 These data suggest that there might be a potential for improving results after undisplaced femoral neck fractures by using hemiarthroplasty. Another study from the NHFR could not find any significant difference in 1-year mortality comparing internal fixation (IF) and hemiarthroplasty (HA) in displaced fractures.25
Hui et al. suggested hemiarthroplasty as the preferred treatment for undisplaced fractures in patients older than 80 years.42 They found a 31% reoperation rate for undisplaced fractures in patients older than 80 years treated with an SHS, whereas patients younger than 80 years had a significantly better prognosis (7% reoperation rate). Similarly, patients greater than 80 years with displaced fractures treated with a hemiarthroplasty had a 7% reoperation rate. In their study, mortality was not different between treatment groups.
To our knowledge no randomized clinical trial comparing IF and HA for undisplaced fractures has been published. The evidence in the current literature is inconsistent and limited, and the role of primary arthroplasty in the treatment of undisplaced femoral neck fractures in the elderly remains unclear. More studies, preferably large randomized trials, are required before the extended use of arthroplasty in elderly patients with undisplaced femoral neck fractures might be established as a common treatment. These studies should also take into account the health economic aspects of treatment.
DISPLACED FRACTURES
In general, closed reduction and internal fixation is no longer recommended for displaced femoral neck fractures in the elderly. These fractures are best treated with an arthroplasty and will be discussed later in this chapter.
However, some healthy elderly people remain very active, and their activity level, bone stock and biological age may be comparable to people much younger. Having an arthroplasty might be incompatible with their lifestyle and expectations of remaining highly active. In an effort to preserve a high functional level, even at the expense of an increased risk of mechanical failure, nonunion and avascular necrosis, closed reduction and internal fixation might be justified for these particular patients. Unless a perfect reduction of the fracture is obtained, a primary arthroplasty should be the treatment of choice for these patients.
IMPLANTS
The type of implant for internal fixation of femoral neck fractures is still a matter of discussion. It has not yet been proven whether cannulated screws or an SHS, with or without an antirotation screw, is the better implant.43,44 Previous studies have not been sufficiently powered to give a definitive answer, and even meta-analyses have so far been unable to detect any major difference in outcome between these two implants. A summary of the results from 30 randomized trials comparing different implants in more than 6000 patients with femoral neck fractures concluded that the existing evidence does not clearly support one type of cannulated screw or pin over another.44 Even though cannulated screws may result in a shorter operative time and less blood loss, and fractures treated with an SHS may have less avascular necrosis, long-term clinical outcomes and complication rates are comparable. Most of the relevant literature on these implant issues is not up-to-date. The question of whether there are clinically relevant differences between cannulated screws and a SHS device is currently being addressed in a large randomized multicenter and multinational clinical trial.45
Several new implants have been invented in recent years with the aim of improving results after internal fixation of femoral neck fractures, including various angular stable implants, as well as hydroxyapatite coated or augmented implants. So far, it remains to be proven in larger series whether these new implants will outperform traditional methods. Results after internal fixation of femoral neck fractures seem to be more dependent on fracture type, patient characteristics, quality of reduction and implant position than on the implant itself. In lateral or basocervical femoral neck fractures, where the calcar support for the cannulated screw is no longer intact, alternative methods such as the SHS are preferred.
PROGNOSIS AND SURGICAL TECHNIQUE
Increasing age, high ASA grade, cognitive impairment and pre-fracture domicile are established predictors of a poorer outcome, including nonunion and mechanical failure after internal fixation of femoral neck fractures. Unfortunately, these factors cannot be influenced. However, the quality of the reduction and the implant position are also important predictors, and these factors can be optimized.
Fracture reduction
Nonunion and mechanical failures correlate with fracture type and the quality of fracture reduction. Garden stated in his classic paper from 1961 that poor reduction is almost synonymous with nonunion, and that a good reduction greatly improves the outcome.7 Yang et al. found a threefold increased risk of mechanical failure after internal fixation of displaced intracapsular hip fractures compared to undisplaced fractures. Fractures inadequately reduced had an 18 times higher rate of failure compared to those anatomically reduced.46 Although the results regarding poor outcome are heterogeneous, all studies agree on the importance of a perfect reduction on mechanical failure and reoperation rates in intracapsular hip fractures. Accordingly, anatomical reduction should always be the goal, but a minor valgus position of the femoral head might be accepted. A varus reduction should be avoided as this is a more unstable configuration with shearing instead of compressive forces across the fracture.
Undisplaced fractures may have a posterior tilt of the femoral head in the lateral view. Palm et al. have described a method to measure the posterior tilt of the femoral head in the lateral plane and found a 1-year reoperation rate of 56% for fractures with more than 20 degrees of posterior tilt, as compared to 14% for those with a posterior tilt of less than 20 degrees.40 Comparable results have also been found in other studies,38,47 but Lapidus et al., in a review of 382 undisplaced femoral neck fractures, did not find any prognostic value of the posterior tilt measurement.48 For younger patients we suggest trying to reduce any major dorsal angulation by careful distraction and internal rotation of the leg, but certainly not at the cost of displacing the fracture. Without any reduction, achieving a desirable position for the cannulated screws and thereby sufficient fracture stability may be difficult. Whenever a fracture cannot be satisfactorily reduced, a prosthesis should be the treatment of choice. In elderly patients, fractures with posterior tilt greater than 20 degrees should probably be treated as displaced fractures.
Implant position
The position of the implant is important. Regardless of the number of cannulated screws used, the key position of the first screw is low and central in the femoral head and neck. This screw should have direct calcar support and the threads should be anchored in the subchondral bone (Figure 34.4). This gives the cannulated screw the best three-point fixation and support for the fracture reduction. The second screw is placed parallel to, and as far away as possible from the first screw (in the AP view). Still, this screw should be anchored in the posterior part of the femoral head and neck for the best purchase in the bone. To provide three-point support, the second screw should rest on the (posterior) cortex. If three screws are used, two of the screws should be placed in the positions described above. The third screw should be placed anterior in the femoral head and neck fragment, thus creating an inverted triangle together with the two other screws (Figure 34.5). For the fracture to settle, and enabling compression without rotation, it is crucial that the screws are parallel. If, for instability reasons, more screws are felt to be required, an arthroplasty should be performed.
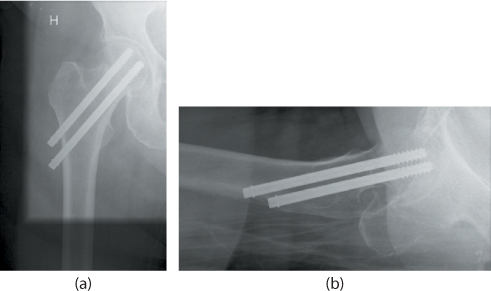
Figure 34.4 Internal fixation with two cannulated screws. (a) Anteroposterior (AP) and (b) lateral views of the right hip.
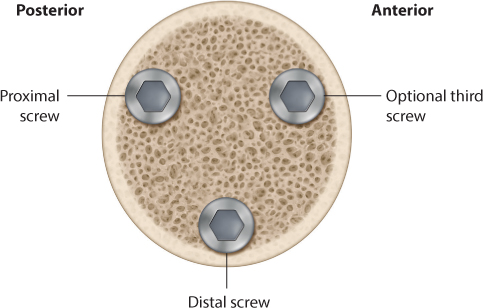
Figure 34.5 Configuration of cannulated screws.
Whereas three screws seem to be the most common fixation in most countries, two parallel screws are most frequently used in Scandinavia. The number or type of screws does not seem to have any major influence on outcome. Less attention has been paid to the position of the femoral head and neck screw in an SHS device in femoral neck fractures. A centre–centre position in the AP and lateral plane, as described for intertrochanteric fractures,49 is probably the best for intracapsular femoral neck fractures. Alternatively, the position might be slightly more caudal, at least when an extra antirotation screw is added. This would be the case for basocervical fractures, fractures with a vertical fracture line, or fractures with comminution causing inherent instability.
Arthroplasty
HEMIARTHROPLASTY
The main indication for hemiarthroplasty is a displaced femoral neck fracture. Historically, prostheses with well-documented inferior clinical results, such as uncemented Austin-Moore and Thompson prostheses, have been used as treatment for hip fractures. Contemporary prostheses have been more commonly used over the last decade.50,51 When performing a hemiarthroplasty, femoral stems that have performed well in total hip replacement should be preferred whenever possible.
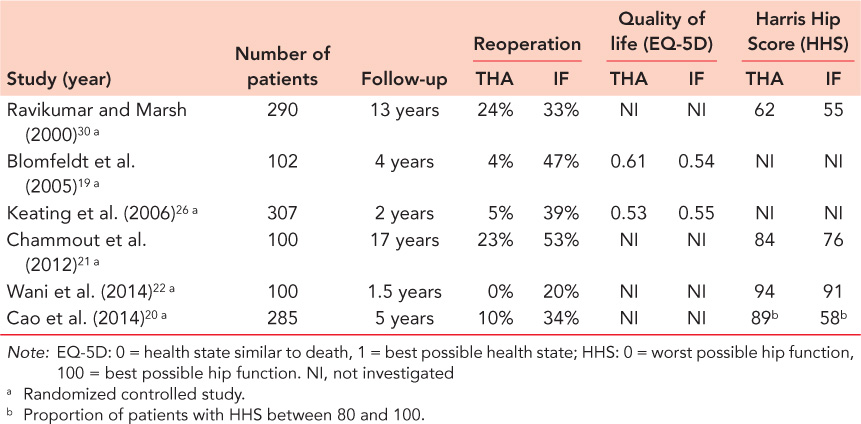
Treatment with hemiarthroplasty has been compared to internal fixation in several studies (Table 34.1). Treatment with hemiarthroplasties reduces the number of complications and reoperations compared to internal fixation.23,24,25,26,27,28,29,30 and 31 The functional results with contemporary hemiarthroplasties have also been found to be superior to internal fixation.23,24 and 25,31
Studies comparing old, uncemented Austin-Moore hemiprostheses and internal fixation have not reported such differences, indicating that these prostheses are inferior and should no longer be used.27,28,30,52 From an economic point of view, hemiarthroplasties are preferable to internal fixation. The initial lower cost associated with internal fixation compared to hemiarthroplasties is outweighed by subsequent costs related to more reoperations and readmissions after internal fixation later on.55,56 Based on the current literature, modern hemiarthroplasties appear to outperform internal fixation for displaced femoral neck fractures in elderly patients.
A hemiprosthesis can be either uni- or bipolar (Figure 34.6). Several studies have compared the results of bipolar and unipolar prosthesis. The results are summarized in Table 34.2. Unipolar and bipolar hemiarthroplasties seem to have equivalent short-term clinical results. The main concern with unipolar prostheses is the risk of acetabular erosion causing pain and impaired hip function, with some suggesting their use should be limited to very elderly patients with low demands and a relatively short life expectancy. The severity of erosion correlates with age, the level of physical activity and the duration of follow-up.64,65 Increasing erosion over time may cause acetabular protrusion that has been found to be present in up to 16% of unipolar prostheses 10 years postoperatively.66
Bipolar prostheses have been found to reduce the risk of acetabular wear due to the dual-bearing system.59,60 One disadvantage of bipolar hemiarthroplasties is that polyethylene wear may increase the risk of loosening of the prosthesis or interprosthetic dislocation.67 Two large register based studies have found increased risk of revisions after bipolar hemiarthroplasties, in particular due to infection and periprosthetic fracture in the oldest patients.61,68 There is no evidence in the current literature in favor of bipolar hemiprostheses regarding clinical outcome in the year following surgery. However, most studies comparing unipolar and bipolar prostheses have a short follow-up.57,58,59 and 60,62,63,69,70,71,72 and 73 Some studies, with longer follow-up, have found better quality of life in patients with a bipolar prosthesis.59,63,72
Table 34.1 Overview of studies comparing clinical results after hemiarthroplasty (HA) and internal fixation (IF)
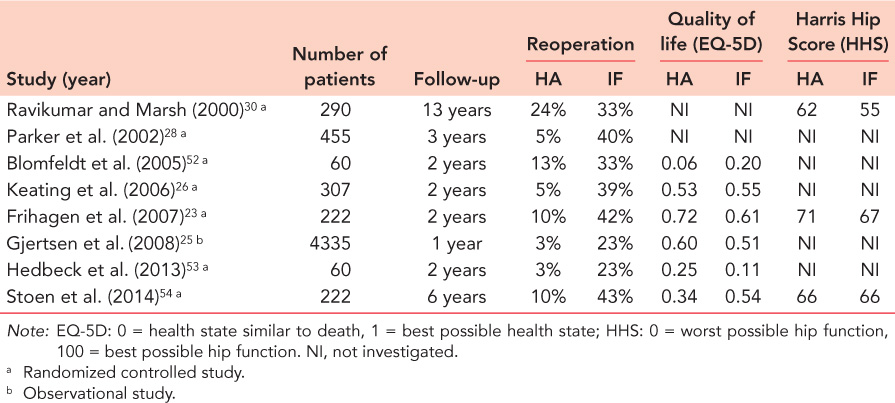
Table 34.2 Overview of studies comparing clinical results of bipolar versus unipolar hemiarthroplasties
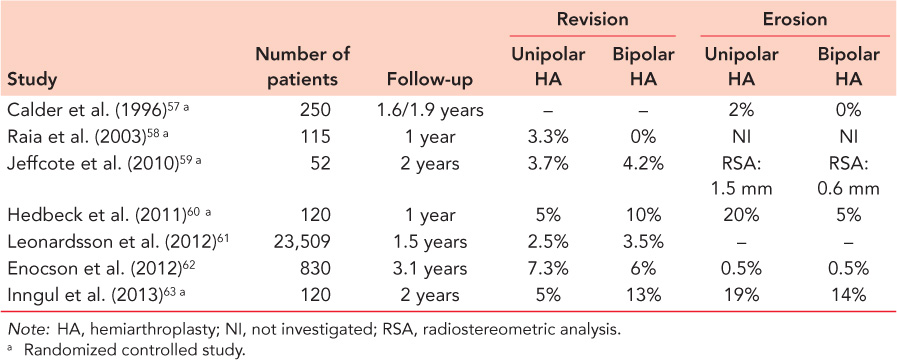
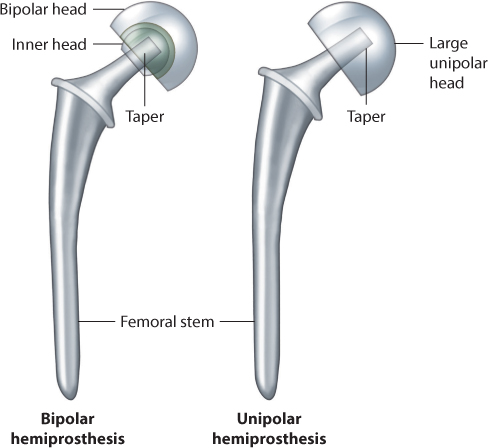
Figure 34.6 Unipolar and bipolar hemiprostheses.
For active elderly patients, with a longer life expectancy, a bipolar hemiarthroplasty may reduce the risk of erosion and improve function over time and could be used even if it is more costly. A unipolar prosthesis is certainly appropriate for the oldest and less active patients.
TOTAL HIP ARTHROPLASTY
Total hip arthroplasty (THA) is a well-documented treatment for displaced femoral neck fractures in healthy and independently mobile patients with no cognitive impairment.19,26,30,65,74,75,76,77 and 78 For patients with systemic disease affecting the hip joint, such as rheumatoid arthritis, a THA should be considered as primary treatment for a femoral neck fracture. Compared to both internal fixation and hemiarthroplasties, THAs in cognitively fit patients demonstrate superior patient reported outcomes, including less pain, improved quality of life, and better hip function and walking ability.19,26,75,76,77,78,79 and 80 The results of studies comparing THAs with internal fixation are summarized in Table 34.3. Fewer reoperations are reported after THA compared to internal fixation.
Table 34.4 summarizes the results of studies comparing the results of hemiarthroplasties and THAs. According to three meta-analyses, the total risk of reoperation is doubled following hemiarthroplasty versus THA.81,83 A THA provides good and predictable long-term outcome but at the cost of an increased risk of early dislocation compared to a hemiarthroplasty.81,83,84 Dislocation is twice as common following THAs when compared to hemiarthroplasties.81,82 and 83 Age, cognitive impairment and a posterior approach are factors associated with a higher dislocation rate.85,86,87 and 88 To minimize the risk of dislocation the use of larger heads is recommended.85 The use of dual mobility cups may further reduce the risk of dislocation and should be taken into account for patients at particularly high risk of dislocation.89,90 and 91
Compared to a hemiarthroplasty, a THA clearly represents greater surgical trauma for patients with a longer operation time and increased blood loss. Even so, no differences in the number of general complications or in mortality have been found.81,82 and 83 Finally, THA is more expensive than a hemiarthroplasty. However, taking into account the improved long-term implant survival, superior functional outcome and a superior independence for patients who have received a THA, the costs appear to be justified.
Based on the recent literature, a total hip replacement for displaced femoral neck fractures in elderly, cognitively fit patients is a safe procedure with acceptable complication rates and good long-term outcome. A THA should be the first choice in healthy patients with good pre-functional status and limited comorbidities.
Table 34.3 Overview of studies comparing clinical results after total hip arthroplasty (THA) and internal fixation (IF)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








