Fig. 1
Anteroposterior radiograph demonstrating right hip dislocation, with superior displacement of the proximal femur, disruption of Shenton’s line, and the femoral head fragment of a Pipkin Type I injury remaining in the acetabulum (Figure from Kloen et al. [16])
Classification
Although several classification systems have been described for femoral head fractures, the system proposed by Pipkin in 1957 is the most commonly used [14] (Fig. 2). It describes femoral head fractures based on the location relative to the fovea capitis, as well as associated bony injuries to the hip articulation.
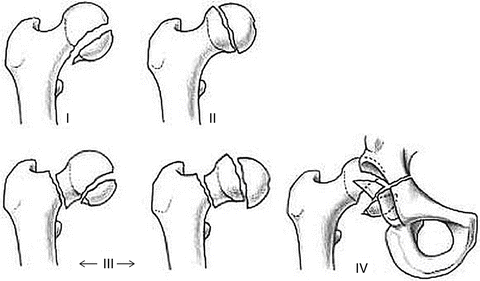

Fig. 2
The Pipkin classification: Type I (fracture of the head caudal to the fovea), Type II (fracture of the head cephalad to the fovea), Type III (Type I or II fracture with femoral neck fracture), Type IV (Type I or II fracture with acetabular fracture) (Figure from Kloen et al. [16])
Another system proposed by Brumback in 1987 is more comprehensive than the Pipkin classification and includes five types, including central and anterior hip dislocations, as well as A and B subtypes [15] (Fig. 3).
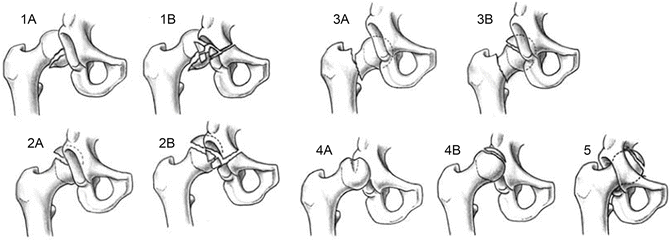

Fig. 3
The Brumback classification: Type I, posterior hip dislocation with femoral head fracture involving the inferomedial portion of the femoral head (IA, minimal or no fracture of the acetabular rim and stable hip joint after reduction; IB, significant acetabular rim fracture and hip joint instability); Type 2, posterior hip dislocation with femoral head fracture involving the superomedial, non-weight-bearing portion of the femoral head (IIA, minimal or no fracture of the acetabular rim and stable hip joint after reduction; IIB, significant acetabular rim fracture and hip joint instability); Type 3, dislocation of the hip with associated femoral neck fracture (IIIA, no associated femoral head fracture; IIIB, associated femoral head fracture); Type 4, anterior dislocation of the hip with fracture of the femoral head (IVA, indentation type; IVB, transchondral shear); Type 5, central fracture-dislocation of the hip with fracture of the femoral head (Figure from Kloen et al. [16])
The Arbeitsgemeinschaft für Osteosynthesefragen (AO) classification of femoral head fractures includes 31-C1 (split), 31-C2 (split/depression), and 31-C3 (associated femoral neck fractures) [16] (Fig. 4).
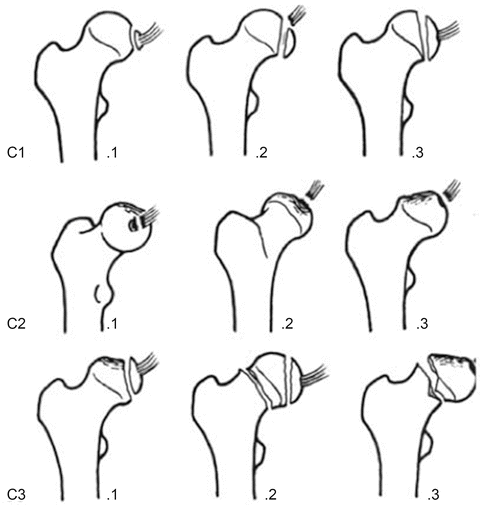

Fig. 4
The AO classification: 31-C1 (split), 31-C2 (split/depression), 31-C3 (associated femoral neck fractures) (Figure from Kloen et al. [16])
Management
Initial Management
A fracture-dislocation of the hip is considered to be an orthopedic emergency. Provided that there is no contraindication to closed reduction (e.g., femoral neck fracture, clear intra-articular blockage to reduction), immediate closed reduction should be attempted. A recent systematic review showed that 84 % of femoral head fracture-dislocations are reducible in the closed setting [9]. Lower rates of avascular necrosis have been reported when the hip is reduced within 6 h [17]. It has been recommended that multiple vigorous attempts at closed reduction be avoided due to risk of further trauma, including fracture to the femoral neck [9]. Further, a case series of irreducible superior femoral head fracture-dislocations has been presented in which the femoral head was found to be buttonholed through the capsulolabral junction with common findings of superior dislocation on x-ray and a clinical constellation of hip position in slight and fixed flexion and absent hip rotation, with leg length discrepancy [18]. The authors recommended that closed reduction should not be attempted in patients with this presentation, due to risk of iatrogenic femoral neck fracture. If closed reduction is unsuccessful or deemed to be too risky to be attempted, emergent open reduction should be performed.
Following closed reduction, repeat AP pelvis radiographs and a CT should be obtained to further evaluate the femoral head fracture pattern (location and size), presence of incarcerated intra-articular fragments, and joint congruence and better define any associated acetabular fractures to help guide further management.
Definitive Management
The overall goals of definitive management are to create a stable, concentric hip joint to maximize function and decrease the risk of future posttraumatic arthritis. Numerous methods have been proposed to this end, ranging from nonoperative management to surgical excision to open reduction and internal fixation to arthroplasty. Due to the rarity of these injuries, an optimized treatment algorithm has not been well defined, and small case series and personal experiences have guided the operative indications, surgical approach, and fixation strategies listed in this section.
Nonoperative Treatment
Historically, most femoral head fractures were treated with prolonged bed rest, immobilization, and traction [14]. For numerous reasons, this has largely been abandoned. However, it has been suggested that nonoperative indications still remain for small Pipkin I/II fractures, in which the femoral head is anatomically or near-anatomically (within 2 mm) reduced and the hip joint is stable and congruent, without interposed articular fragments. However, it has been shown in one study that only 1 in 12 femoral head fractures met those criteria for acceptable closed reduction [10], indicating a modern shift towards operative management of most femoral head fractures. In a small, randomized control trial comparing closed treatment to surgical excision of Pipkin I fractures, functional outcome scores of operatively treated patients were superior to those managed nonoperatively [19]. Hence, recent data suggests that even Pipkin Type I and II fractures may be better treated operatively; however, the exact criteria for acceptable fracture size, fracture location, joint stability, and joint concentricity are not well defined.
If nonoperative treatment is selected, the patient is restricted to partial weight bearing for approximately 3 months, and serial radiographs should be obtained frequently to ensure maintenance of fracture and joint reduction.
Operative Treatment
Most femoral head fractures are now managed operatively. Operative indications include all irreducible femoral head fracture-dislocations, Pipkin III injuries, Pipkin IV injuries (inherently unstable), and Pipkin I/II fractures with large, displaced fragments or any fracture-dislocation combination in which intra-articular fragments create a nonconcentric joint articulation. The goals of operative management are to create an anatomic reduction and stable articulation and to remove loose fragments. There has been significant debate as to the optimal approach (arthroscopic vs. open, various open approaches), treatment option (excision vs. ORIF vs. arthroplasty), and fixation strategy for these injuries.
Surgical Approach: Arthroscopy
A recent report suggested that incidence of hip arthroscopy performed for all indications has increased by over 600 % from 2006 to 2010 [20]. Consistent with this increase, recent studies have evaluated the utility of this technique in treating fractures of the femoral head and acetabulum [21–23], including removal of loose articular fragments and in arthroscopic-assisted open reduction and internal fixation of femoral head fragments.
Mullis et al. performed a diagnostic arthroscopy of 36 patients who sustained simple hip dislocations or fracture-dislocations that did not meet their indications for open surgical management [22]. They found loose bodies in 33 of 36 patients, including 7 of 9 patients who were not found to have fragments on standard postreduction x-ray and CT scans. They were able to successfully remove the loose bodies from the joint and concluded that arthroscopy is a good tool for removing loose fragments in hips that otherwise do not require open treatment. Further, Matsuda reported the successful arthroscopic treatment of a suprafoveal femoral head fracture, fixed with two Herbert screws [23].
Proposed advantages of the arthroscopic approach to femoral head fracture treatment include improved access for removal of loose bodies, less disruption to the capsuloligamentous structures, minimal blood loss, and faster recovery time [24]. Proposed disadvantages include technical difficulty, as well as other standard hip arthroscopy risks (traction neuropraxia, injury to lateral femoral cutaneous nerve, avascular necrosis, intraperitoneal fluid extravasation, retroperitoneal fluid extravasation) [24].
Surgical Approach: Open Techniques
Numerous open surgical approaches to the hip joint have been described for use in femoral head fractures, including medial (Ludloff), direct lateral (modified Hardinge), posterior (Kocher-Langenbeck), anterior (Smith-Peterson, modified Hueter), anterolateral (Watson-Jones), and, more recently, the trochanteric flip (digastric) osteotomy [13]. Each of these approaches has advantages and disadvantages, and ultimately, the approach should be decided based upon the location of the femoral head fracture, the treatment plan (excision vs. fixation), associated injuries (acetabular, femoral neck), and the direction of the dislocation.
The anterior approaches to femoral head fractures include the Smith-Peterson approach and modified Hueter approach. Historically, the anterior approaches were discouraged due to the belief that they would further compromise the femoral head blood supply, increasing the risk of avascular necrosis, by surgical ligation of the ascending branch of the lateral circumflex femoral artery. However, recent cadaveric studies have disproven this by demonstrating that the medial circumflex femoral artery is the dominant blood supply to the femoral head, with almost no contribution from the lateral circumflex femoral artery [7].
Advantages to anterior approaches include improved visualization of anterior-based femoral head fractures for reduction and fixation, decreased operative time, and lower rates of AVN when compared to posterior approaches [24–26]. Disadvantages include higher rates of heterotopic ossification (HO) compared to posterior approaches, decreased visualization of associated posterior wall fractures, and decreased access posteriorly, especially critical in the presence of irreducible incarcerated fracture-dislocations [24–26].
To address some of the downsides in visualization of the femoral head with the anterior approach, a modified Smith-Peterson approach has been described, in which anterior dislocation of the femoral head is possible for improved circumferential access of the femoral head [24]. The surgical technique is described in detail in the next chapter.
The posterior approach to femoral head fractures involves the standard Kocher-Langenbeck approach. This was historically favored for the treatment of femoral head fractures, as it was postulated that blood supply to the femoral head would be damaged after posterior hip dislocations and that further damage to the blood supply during an anterior surgical procedure was not advisable. As mentioned above, this has been disproven with recent understanding of the vascular anatomy of the femoral head [7]. The posterior approach, however, is advantageous for irreducible, incarcerated femoral head fracture-dislocations, in which posterior soft tissues, including the piriformis tendon and sciatic nerve, can block reduction of the femoral head. In addition, it is a favorable approach in femoral head injuries with associated acetabular fractures. A reported disadvantage of the standard posterior approach for femoral head fractures is an increased rate of AVN, recently reported in a meta-analysis to be 3.67 times higher compared to anterior approaches and 2.24 times higher compared to the trochanteric flip approach [9]. The main disadvantage to the posterior approach is that femoral head access is limited and reduction and fixation of anterior femoral head fractures are often difficult.
The trochanteric flip osteotomy, or digastric osteotomy, was originally described by Ganz and colleagues [27]. In this technique, a posterior approach to the hip joint is modified by the addition of a digastric trochanteric osteotomy to allow for anterior dislocation of the hip joint and preservation of the posterior blood supply (medial femoral circumflex artery). This approach, popularized for use in treatment of femoroacetabular impingement, has been applied for the treatment of femoral head fractures [28]. The surgical technique is described in detail in the next chapter.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








