ROBERT A. CHRISTMAN, MARY OEHLER, CASIMIR F. STRUGIELSKI, AND DAVID E. WILLIAMSON
THE IMAGE RECEPTOR
For over 100 years, radiography has used some form of film/intensifying screen combination as an image receptor. X-rays, after passing through the patient, interact with the image receptor, and a latent image (an invisible change that represents the object that was radiographed) forms in the film. The radiographic film is processed with chemicals to produce a visible (manifest) image, which is then viewed on a light box, catalogued, and physically stored. The typical image receptor used in film–screen radiography consists of a radiographic film that is sandwiched between two intensifying screens, all protected in a container known as a cassette.
Intensifying Screen
About 99% of the exposure on radiographic film comes from the light emitted by the intensifying screen. X-rays are extremely inefficient in producing optical density (blackening) of the radiographic film. Because x-radiation is absorbed by tissue (and accumulated), any method to reduce dosage and yet provide a usable image is desirable. The intensifying screen is primarily responsible for making radiographic imaging a relatively safe medical diagnostic tool.
Intensifying screens are composed of light-emitting phosphors that fluoresce when exposed to x-rays. Because radiographic film is sensitive to light, fewer x-rays are needed to expose the film. This allows the exposure technique to be reduced, which reduces patient exposure to x-radiation. Intensifying screen selection traits include its speed and, more importantly, spectral qualities.
Two types of intensifying screens are available: calcium tungstate and rare earth. Calcium tungstate screens emit light in the blue/blue–violet portion of the visible light spectrum; rare-earth screens primarily emit green light, although a few emit blue light. Green-sensitive (orthochromatic) film must be used with green-emitting intensifying screens and blue-sensitive film with blue-emitting intensifying screens. Incorrect matching of the film and screen will result in a slower film/screen system speed, which means using a longer exposure technique. Rare-earth intensifying screens are faster than calcium tungstate film/screen systems and do not sacrifice resolution. They have, therefore, widely replaced calcium tungstate systems.
If they are cared for properly and not accidentally damaged, intensifying screens can last many years. They should be cleaned as recommended by the manufacturer. Screen cleaners often contain an antistatic solution. Do not spray the formula directly onto the screen; spray onto a cloth first. A drop of chemical could stain or damage the screen before it is wiped off. Exercise extreme care not to touch the screen except when cleaning. Scratches, for example, will permanently damage the screen.
Radiographic Film
In medical radiography, many products have been designed to offer a vast array of speed levels and contrasts appropriate for the body part being radiographed. Generally speaking, the film’s inherent speed depends on the silver halide crystal (grain) size, structure, and sensitivity; the choice of developer; and the time and temperature that the film is processed. It naturally follows that the larger the silver halide crystal, the faster the speed of the film and the less the exposure. Combinations of different-sized crystals are used to create the desired characteristic curve, a measurement that describes the relationship between radiographic exposure and optical density.
The layers of an x-ray film (Figure 2-1) and their functions are as follows:
• Overcoat: A protective layer that aids in scratch protection both before and after processing
• Emulsion: The light-sensitive layer, made up of silver halide suspension in a high-grade gelatin support
• Subcoat: A very thin coating that ensures adherence of the emulsion to the base support
• Base support: The material that forms the structural support onto which the other sensitive and protective layers are coated
• Backing: Another gelatin layer sometimes used to prevent curl, inhibit light piping, and improve image quality or to act as a filter to make the film insensitive to certain wavelengths
The two primary types of radiographic film are direct exposure film and screen film. Direct exposure film provides a sharp image of thin body parts having high subject contrast. However, long exposure time is necessary to create an image with appropriate optical density. Direct exposure film was primarily employed to assess the extremities but has been widely replaced with faster high-detail film/screen combinations.
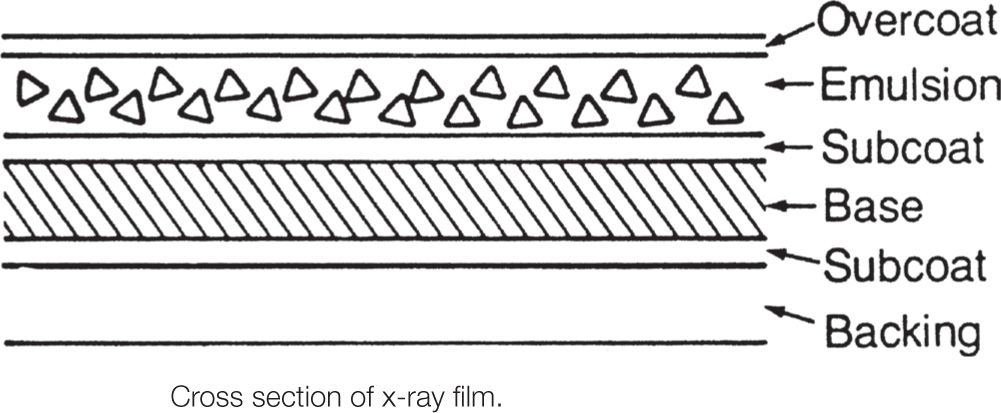
FIGURE 2-1. Cross section of x-ray film.
Many types of screen film are available from several manufacturers. This type of film is sensitive to light emitted from an intensifying screen as well as x-rays. Screen film is either single or double emulsion. Single-emulsion film is only coated on one side. It provides a sharper image when used with a single-emulsion, high-detail/fine-grain intensifying screen than does double-emulsion film used with two screens. Single-emulsion film is not used very often nowadays because of the availability of newer high-detail double-emulsion film/screen combinations that give optimum image sharpness.
Other film characteristics to consider include contrast, speed, and light absorption. After selecting a film type, it must be matched to an appropriate intensifying screen. The choices for film contrast are high, medium, and low. High-contrast film produces more blacks and whites on the radiograph. Medium-contrast film has more shades of gray than does high-contrast film. Low-contrast film demonstrates a long scale of grays, referred to as latitude. Latitude is inversely proportional to contrast. Medium-to-high–contrast film is typically used for extremity radiography.
The term film speed refers to the time it takes to respond to an exposure. Faster film speed correlates to less radiation exposure for the patient. However, faster films are not as sharp as slower films. Slower-speed, high-detail (high-resolution) films are primarily employed for extremity studies.
Each type of film has specific light absorption characteristics. There are blue-sensitive and green-sensitive (also known as orthochromatic) films. A blue-sensitive film must be used with an intensifying screen that emits blue light and a green-sensitive film with a screen that emits green light. Mismatched film/screen combinations require increased exposures, thereby increasing the patient dose.
Specific guidelines should be followed regarding storage and handling of radiographic film. A relative humidity of 40% to 60% and a constant 70°F temperature are ideal for storage. In a hot, humid environment, the film may stick together. Check the expiration date of each box of film; rotate the film accordingly, using older film first. Expired film should not be used; film quality may be impaired. Film should be stored on its side or end, not flat. Pressure marks (artifacts) may develop if the film is stored flat. Handle films with clean, dry hands. Be careful not to bend or crease the film during handling.
The radiographic image is greatly influenced by the type of film and intensifying screen used. Because there are many different types of films and screens, they must be properly matched to one another and to the study (in this case, extremity radiography). Inappropriately matched film/screen combinations can significantly impair the radiographic quality. The wrong film/screen combination can ultimately lead to misdiagnosis and increase radiation exposure to the patient if a study is repeated.

FIGURE 2-2. Rigid cassette (opened, revealing intensifying screens and rectangular cutouts for identification imprinting). (Courtesy of Providence Imaging Products, Inc., Providence, RI.)
Film–Screen Cassettes
Cassettes are lighttight film and screen holders. They swing open on a hinge mechanism. The screens are permanently affixed inside the cassette, one on each side (if two screens are used). The film is “sandwiched” between the two screens; it must be loaded in the darkroom (unless one is using a daylight loading system). Most cassettes are rigid devices (Figure 2-2); major film manufacturers may provide cassettes at little or no cost if you agree to use their film.
All cassettes have a backing material to absorb radiation that passes through the cassette. This prevents backscatter that could otherwise impair the image quality.
IMAGE QUALITY
The goal of producing a radiographic image is to provide the greatest amount of usable information to aid in diagnosis. In medical radiography, there is no tolerance for anything other than the closest to reality that one can achieve. Consistency and faithful recording of anatomical structures with optimum detail are primary goals. Anything less is unacceptable for the interests of both the doctor and the patient.
Quality can be described as a level of excellence. There are many adjectives used to clarify it. In medical imaging, one must think of matching the interpreter’s trained eye with the optimum image capturing characteristics of the film. When the image can be visualized to allow the most concise and informative interpretation, one can say that the highest level of radiographic quality has been attained. Many factors contribute to or detract from the end-product quality. This chapter discusses those factors that the radiographer/limited x-ray machine operator (LXMO) can control and measure, and offers general concepts for assessing radiographic quality.
When a film is labeled “high quality,” it usually has low fog, appropriate contrast to display small differences in density, and sufficient speed to overcome blurring caused by motion. This is all embodied in an emulsion that has grain structure fine enough not to impair the definition of the part being radiographed.
The radiologic examination is an important adjunct in determining the etiology (or etiologies) of a patient’s complaint. It is equally important that the finished radiograph be of the highest quality, providing as much information as technically possible.
Definitions
Radiographic quality refers to the exactness of representation of the anatomic structure on the radiograph within the useful density range. Quality is not easy to objectify and is influenced by radiographic noise and resolution.
Radiographic noise is the undesirable fluctuation in the optical density of the image. Radiographic noise has three components: film graininess (size/spacing of silver halide crystals—grains—in the film emulsion; the smaller the better), structure mottle (size/spacing of phosphors in a screen; again, the smaller the better), and quantum mottle (random interaction of x-rays with the image receptor; the greater the number of primary beam x-rays that strike the image receptor, the smoother the quantum mottle). Noise is primarily due to scatter radiation.
Resolution is the ability to separate and distinguish between two separate objects; this is also referred to as detail. There are two types of resolution: spatial and contrast. Spatial resolution is of great importance when imaging the foot and ankle; it is the ability to distinguish between two objects demonstrating high subject contrast, such as between bone and soft tissue. Contrast resolution best applies to imaging of the abdomen, where organs of similar contrast need to be distinguished.
The ability of an x-ray film to respond to an x-ray exposure is the measure of its sensitivity or speed. Fast-image receptors (≥400) have high noise and low resolution; slow-image receptors (50–300) have low noise and high resolution. Therefore, to obtain a high-quality foot or ankle radiograph, meaning one with low noise, high contrast, and high detail, one would use a slow-speed film/screen combination.
Factors that affect radiographic quality are related to the x-ray film (density, contrast/latitude, speed, processing time, and temperature), geometrical issues (distortion, magnification), and the subject (motion, and contrast relating to thickness, density, and atomic number). Just as no two patients are alike, situations and technical factors that produce the image will vary. The fundamental concept is that the finished radiograph should exhibit sufficient radiographic density, acceptable contrast, optimal detail, and minimal distortion.
Radiographic Density
The radiographic density, also referred to as optical density (OD), is defined as the amount of blackening in a radiograph. Density and adequate differences in density, or contrast, are considered the most important properties of a radiograph. Proper densities and adequate contrast are required to give visibility to the structural detail of a subject.
Milliampere-second (mAs) is the primary controlling factor for radiographic density. It is a product of milliampere multiplied by the exposure time expressed in seconds (s).
mAs = mA × s
15 mA × 8/60 s = 120/60 = 2 mAs
30 mA × 4/60 s = 120/60 = 2 mAs
Both sets of exposure factors (mA and s) yield the same mAs value; therefore, both films should exhibit the same radiographic density, assuming that all other technical factors are unchanged. Also, it is important to remember that as mAs increases, both x-ray quantity and radiographic density increase proportionally, and vice versa. This is known as the law of reciprocity (Figure 2-3).
To cause a visible shift in radiographic density, a ±30%-mAs alteration is necessary to produce this effect. This is the minimum change required that will be perceived by the human eye. If adjustment in density is necessary, however, changes in mAs should be made by factors of 2 (either double or half). A film that displays insufficient density and that was originally exposed using 2 mAs, for example, should be repeated at 4 mAs.
A film of questionable radiographic density should be outside the acceptable limits to justify a repeat exposure, either very light or very dark (i.e., the anatomic structures under consideration cannot be adequately distinguished). The appropriate change would be to either double or half the mAs. However, when doing so, change either the mA or the exposure time, not both; changing both will increase the mAs value above the half or double value required.
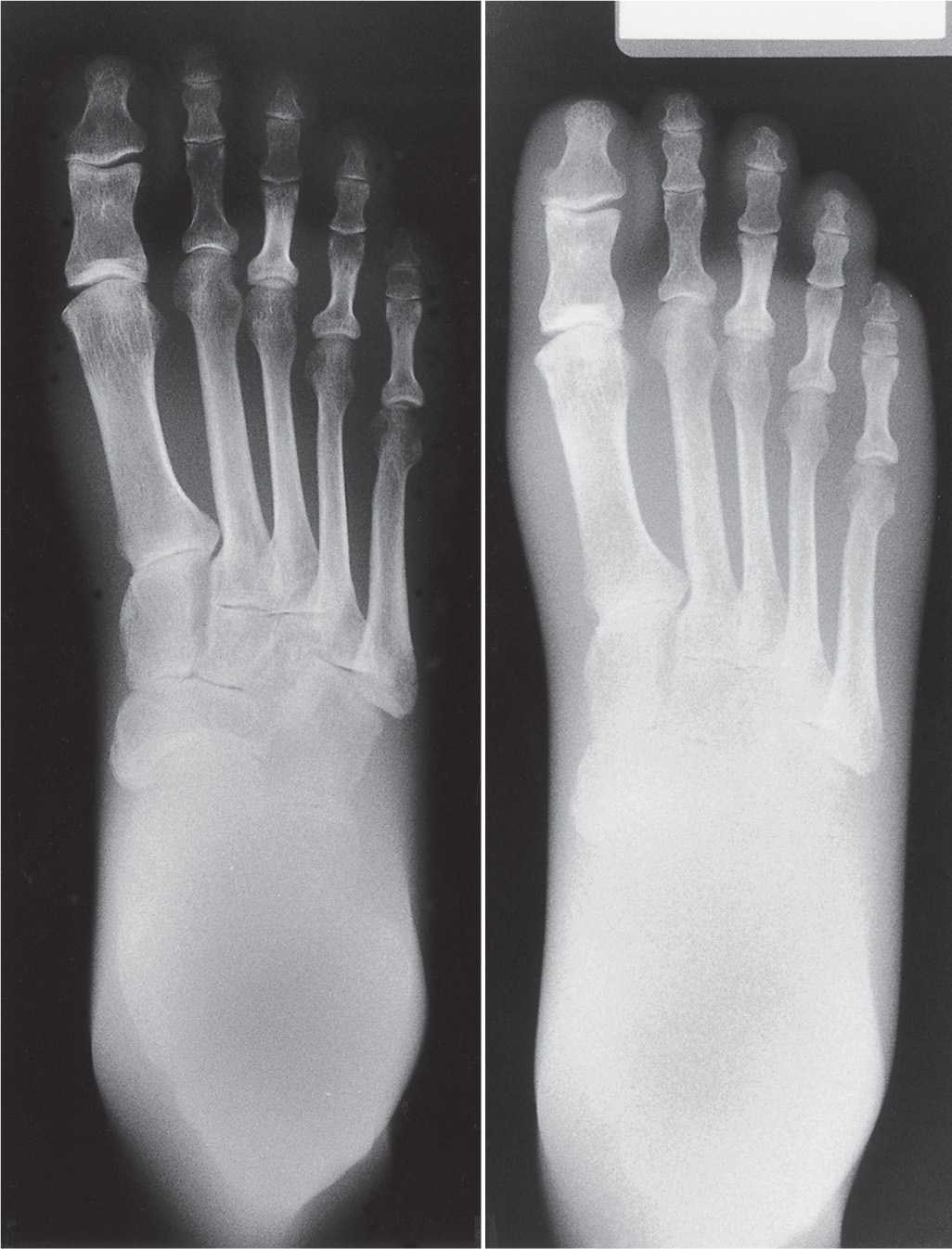
FIGURE 2-3. As time or mA changes (mAs), a corresponding change in density (law of reciprocity) occurs. Left image: 4 mAs exposure versus 2 mAs exposure (right image); all other exposure factors (kVp and SID) are unchanged.
Other factors influencing radiographic density are kilovoltage, distance, film/screen combination, and film processing.
Kilovoltage
Kilovoltage alters both the quality (energy) of the x-ray beam and the quantity of x-ray photons produced. A 15% increase in kVp will cause the same change in radiographic density as doubling the mAs, and a 15% decrease in kVp will result in a change in density similar to decreasing the mAs by half. This is referred to as the 15% rule. A 4% to 8% change in kVp is necessary in order to produce a visible difference in the radiograph. This will require a change in at least 3 to 7 kVp (the kVp range used with lower extremity–specific x-ray units is 50–70 kVp).
Distance
Changes in distance between the x-ray tube and the film, also referred to as the source-to-image distance (SID), will alter the number of photons striking the film (quantity of radiation). This can significantly alter the radiographic density. If the tube is too far away from the film, an insufficient number of x-ray photons strike the film, producing a light film (decreased radiographic density). And, if the tube is too close to the film, a greater number of x-ray photons, than are required, strike the film, producing a very dark film (increased radiographic density). This is known as the inverse square law and is expressed by the following formula:
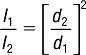
where I1 = original intensity, I2 = new intensity, d1 = original distance, and d2 = new distance.
For example: The original exposure intensity is 2 mAs at an SID of 28 in. What would the radiation intensity be at the film if the SID were increased to 36 in?
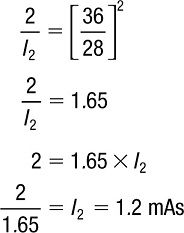
Therefore, by increasing the SID from 28 to 36 in, the x-ray intensity at the film has been reduced to 1.2 mAs, nearly half of the original 2 mAs, which results in a film with decreased radiographic density.
In order to determine the mAs needed at the 36-in SID to produce the same radiographic density as the original film (2 mAs and 28-in SID), use the following formula:
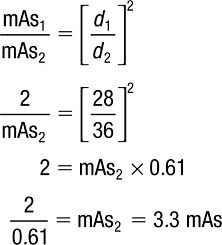
This type of scenario will arise when performing radiography with variable SID, such as with a portable/mobile x-ray unit.
Film/Screen Combinations
Years ago, the speed of film/screen systems was divided into three groups:
Slow (detail) | Double the average screen speed |
Average (medium, par) | Baseline |
Fast | Half the average screen speed |
The speed of the film/screen system can also be expressed in numeric terms, developed by the manufacturers, referred to as the relative speed (RS) value (Figure 2-4). This refers to the sensitivity or response that the intensifying screen phosphors have to x-ray photons. The higher the RS, the faster the film/screen system speed; therefore, less radiation is needed to produce an image. However, there is a compromise: higher film/screen system speed reduces image sharpness (detail).
Since older calcium tungstate screen phosphors have mostly been replaced by rare-earth phosphors in imaging technology, the compromise between detail and speed has diminished. A balance between speed (sensitivity to x-ray photons) and resolution (detail) has been accomplished.
Should it become necessary to use or change factors because you are employing different speed systems, the following formula can be used:
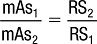
where mAs1 = old mAs, mAs2 = new mAs, RS1 = old relative speed, and RS2 = new relative speed.
For example: If there was a change from a slower 200 RS system, using 2 mAs, to a faster 400 RS system, what mAs would be necessary to produce a film with the same radiographic density as the original system (assuming all other technical factors remain unchanged)?
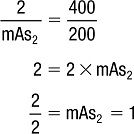
Therefore, doubling the speed of the film/screen system resulted in a reduction of mAs by half.
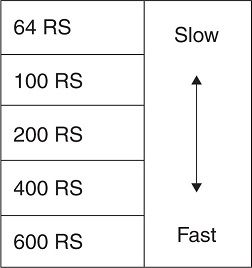
FIGURE 2-4. RS values of film/screen systems.

FIGURE 2-5. Single-screen system. Position of notches (arrow and arrowheads) aids in proper placement of emulsion against intensifying screen.
Film/screen systems generally have two intensifying screens, one on either side of the film, which has emulsion on both sides. A single screen may be employed to image the extremities. This system improves the sharpness of detail. However, when using a single-screen imaging cassette, the correct film type (single-sided emulsion) must be used. Care must be taken when loading the film into the cassette. The film emulsion, generally the dull side, must face the single screen. This can be accomplished by making sure that the notch of the film is placed in the correct position in the cassette to have the film emulsion side face the screen surface (Figure 2-5). If switching from a dual-screen system to a single-screen system, the mAs would need to be doubled to obtain the same radiographic density as with the double-screen system.
Compensation Filter
The foot thickness is not the same in the forefoot as in the rearfoot. As a result, in the anteroposterior/dorsoplantar foot view, the radiographic density varies considerably between the toes and the tarsus. If an exposure technique is selected to obtain an ideal film density for the toes, the tarsus will be underexposed (decreased radiographic density). In contrast, a technique chosen to image the tarsus will overexpose the toes, which may appear too dark (increased radiographic density). The unequal radiographic density between the forefoot and the rearfoot can be balanced by using device known as a compensation filter. This type of filtration can improve the visibility of bone and soft tissue and lower patient exposure.
The compensation filter system (Figure 2-6) is easily attached to most conventional collimators. The plate is wedge shaped and made of a radiolucent lead–plastic material; it does not alter image quality or contrast. Patient, film, and tube head positioning as well as light beam collimation are performed before attaching the filter. Attention must be paid to initial installment of the filter holder and placement of the filter; the thick portion of the wedge must be positioned at the toe end of the light field so that the thinner portion of the wedge approaches the midfoot. To be certain the filter is positioned over the forefoot properly, and light beam collimation should also be performed after attaching the filter. Use the same technical factors that would be used to image the tarsus only. The LXMO must remember to remove the filter before performing other positioning techniques.

FIGURE 2-6. Compensation filter system. (Courtesy of Nuclear Associates, Carle Place, NY.)
After using the compensation filter, the toes are more visible in the resultant film and the radiographic density is similar to the tarsus. Also, if the area of concern is limited to the digits, a collimated view of the toes alone is preferable; the adjustment of technical factors obviates the need for the compensation filter.
Effects of Film Processing
When proper temperature, replenishment rate, and sequence of film processing are maintained, processing should not be an influencing factor concerning radiographic density. However, the temperature of the developer solution is a crucial factor. Manufacturers have compiled recommended temperature and time charts for each specific type of film.
If the film is immersed in the developer shorter than the required length of time, it will exhibit decreased radiographic density; increased radiographic density results if the film is immersed longer than the required time. If, for some reason, the developer temperature increases, the time that the film is immersed in the developer solution should decrease; if not, increased radiographic density will result. Likewise, if solution temperature decreases, the film immersion time should increase. (Generally speaking, one should not deviate from the film manufacturer’s recommendations.)
Adequate replenishment rates must be maintained to have proper activity level of the processing chemicals. Improper replenishment, either too high or too low, will affect the radiographic density. To ensure proper activity of the processing solutions, new chemicals should be prepared every 1 to 2 months.
Automatic processors should be monitored regularly for correct temperature levels, replenishment rates, proper roller transport function, proper water circulation, and sufficient dryer blower function. Even if not required by state regulations, sensitometry and densitometry, also known as sensidensitometry, should be performed daily on your processor in the morning prior to performing any studies. Sensidensitometry confirms whether or not the processor is working properly, that is, that the chemicals are in the appropriate concentration and temperature to achieve a radiographic image of optimal quality.
Sensitometry and Densitometry
Sensitometry is the study of a film’s response to exposure and processing. The graphic basis of sensitometry—the H&D (Hurter and Driffield) curve—is an important tool for measuring the relationships between radiographic exposure and density. Radiographic density is the result of a deposit of metallic silver remaining on a film after exposure and processing. Densitometry measures the amount of blackening after shining a light through the film. The more the blackening, the more light is absorbed and the less is transmitted. Densities are read by a specialized light meter called a densitometer, and the results are measured in logarithms. Applied to sensitometry, density is defined as the common logarithm of the ratio of the amount of light striking one side of the film, compared to the amount of light coming out of the other side. When 10 units of light are shined at a film and only 1 unit comes out the other side, the film is said to have a density of 1; there is a 10:1 ratio. When the ratio is 100:1, the density is 2, and when the ratio is 1000:1, the density is 3, and so on.
To produce an H&D (characteristic) curve, the film is first exposed to a calibrated step wedge that has a series of equal-increment step changes. The film is processed, and each step of density is read and plotted on special graph paper. Figure 2-7 is a characteristic curve of an x-ray film exposed with intensifying screens and processed in x-ray chemistry. The portion of the curve designated as the “toe” demonstrates the response of the emulsion to relatively small amounts of radiant energy. With an increase in exposure, the density builds slowly until the “straight-line” portion of the film is achieved. Along this straight-line portion the density increases uniformly with the logarithm of the exposure until the shoulder of the curve is reached. In the shoulder region, additional exposure results in smaller increases in density to a point where additional exposure does not produce any greater density. In fact, if sufficient exposure is given, the density will actually decrease.
Sensitometrically, the term contrast refers to the slope or steepness of the characteristic curve of the film; contrast is a generic term. There are different contrasts depending on where they are “read” on the characteristic curve, as follows.
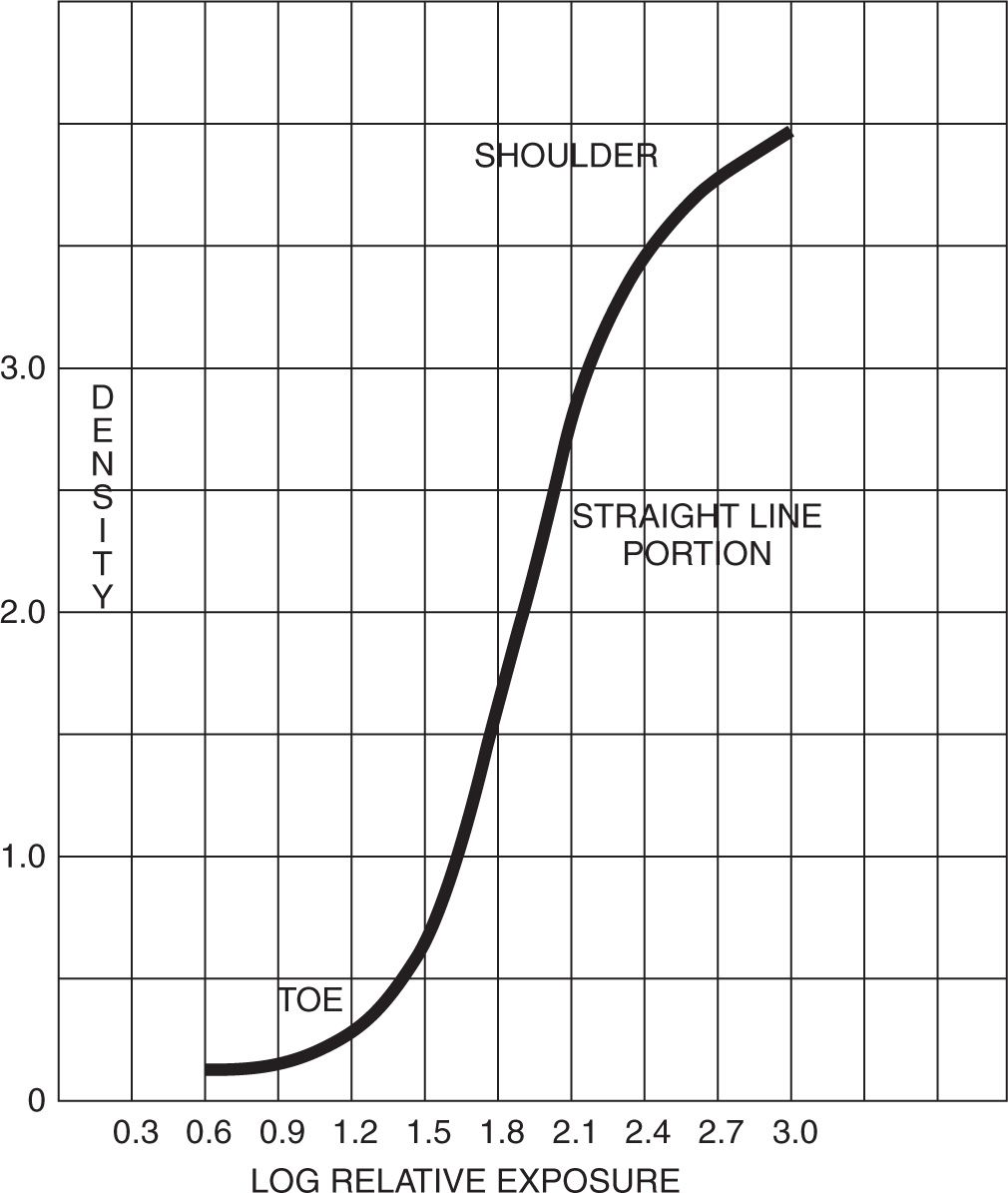
FIGURE 2-7. Characteristic curve of x-ray film.
Gradient is the contrast of the film at a given density. When a straight line is drawn tangent to the characteristic curve at a particular density, this line forms a slope that is the gradient (or contrast) at this density (Figure 2-8).
Average gradient is found most often in radiography because it is more useful to have a single number to indicate the effective contrast of a film. This number, known as the average gradient, is determined by drawing a straight line between two selected densities on the characteristic curve. The two densities used for this measurement are those most often at the thresholds of where the information in the radiograph falls—from 0.25 to 2.00 (Figure 2-9).
Another term used to describe density is gamma, the slope of the straight-line portion of the characteristic curve. This term is seldom used in radiography, because the curves of radiographic films have relatively short straight-line portions. Also, this portion of the curve may not coincide with the density range that is most useful in radiology. If gamma is a reference, it is best to determine exactly which of the “contrasts” is being referred to.
Exposure is defined as intensity multiplied by time. This can be expressed in either absolute exposure units (ergs per square centimeter of x-radiation) or relative units. Relative exposure is much more convenient and equally useful to us. In radiography, we refer to exposure in terms of milliampere-second (mAs). In general, when the mAs is doubled, the exposure is doubled, kVp remaining constant.
In plotting a characteristic curve, density is plotted against the log of relative exposure. If the kilovoltage remains constant, the ratios of the exposures reaching the film through two different regions of the subject are always the same, regardless of the values of the milliamperage, time, or SID. On a logarithmic scale, the same distance on the exposure scale, regardless of the absolute values, will always separate any two exposures whose ratio is constant. For example, two exposures, one of which is twice the other, will always be separated by 0.3 on the logarithmic scale (the logarithm of 2 is 0.3).
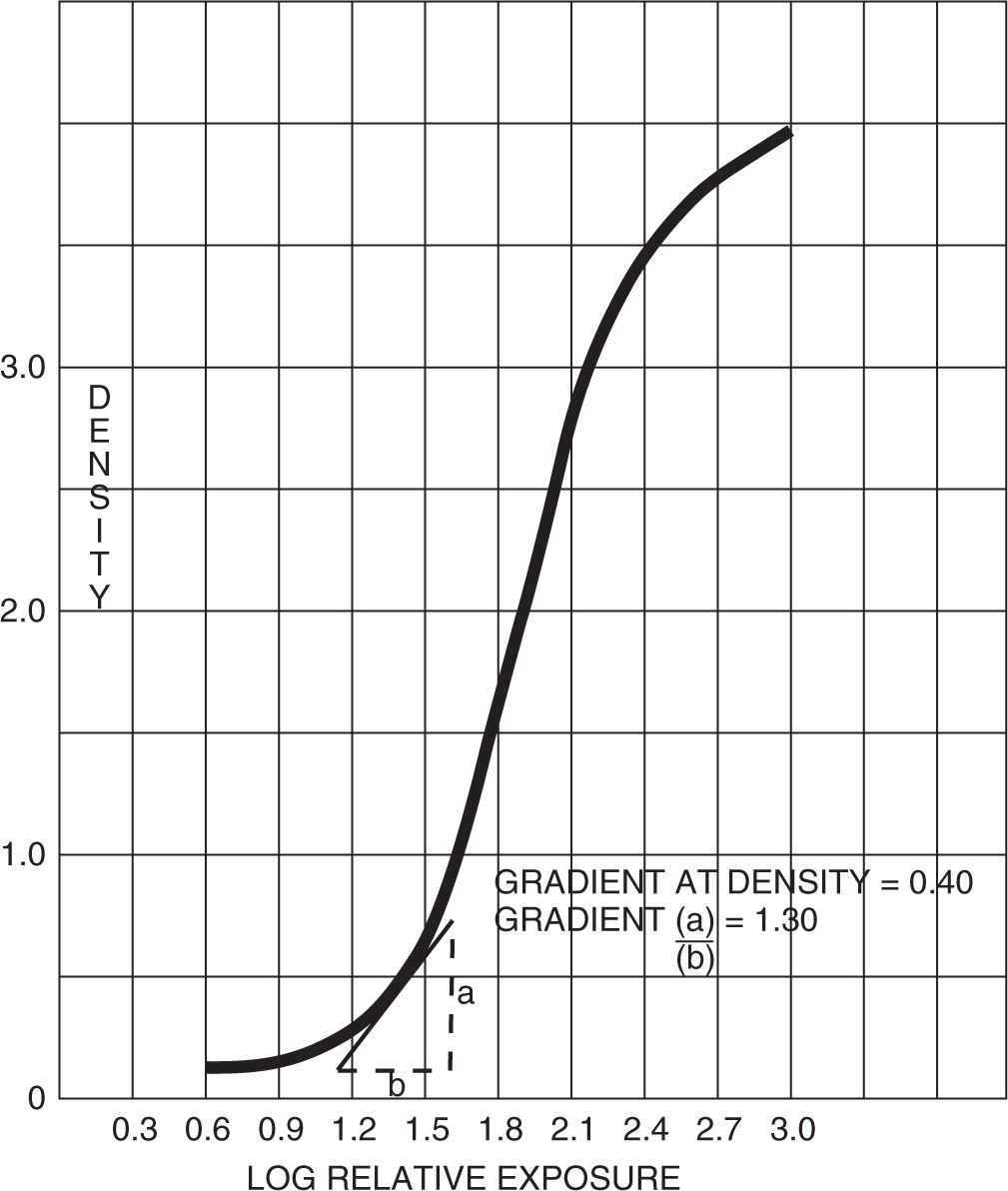
FIGURE 2-8. Calculation of gradient.
It has been determined that the contrast of a film is indicated by the shape of the characteristic curve. Speed is indicated by the location of the curve along the exposure axis. The faster a film is, the more it will lie toward the left of the graph. The faster it is, the less relative exposure it will take to reach the speed point density. The separation of two films plotted on the same graph may be measured at the speed point to determine the speed difference (Figure 2-10).
The convenience of using relative exposures also applies to speed. The speed of one film can be expressed on a relative basis to another when one is made the standard of comparison. The reference film can be assigned any arbitrary speed value, such as 100. If another film only requires half as much exposure to reach the same density as the reference film, then the faster film will have a RS of 200.
A density of 1 above base plus fog has been designated as the density for computing film speeds. This density was chosen because it represents the average of the useful density range (0.25–2.00). However, a density of 0.25 above base plus fog appears to be the approximate density most often viewed in the diagnostic region of a typical radiograph. For practical purposes, RSs are often calculated at this lower density.
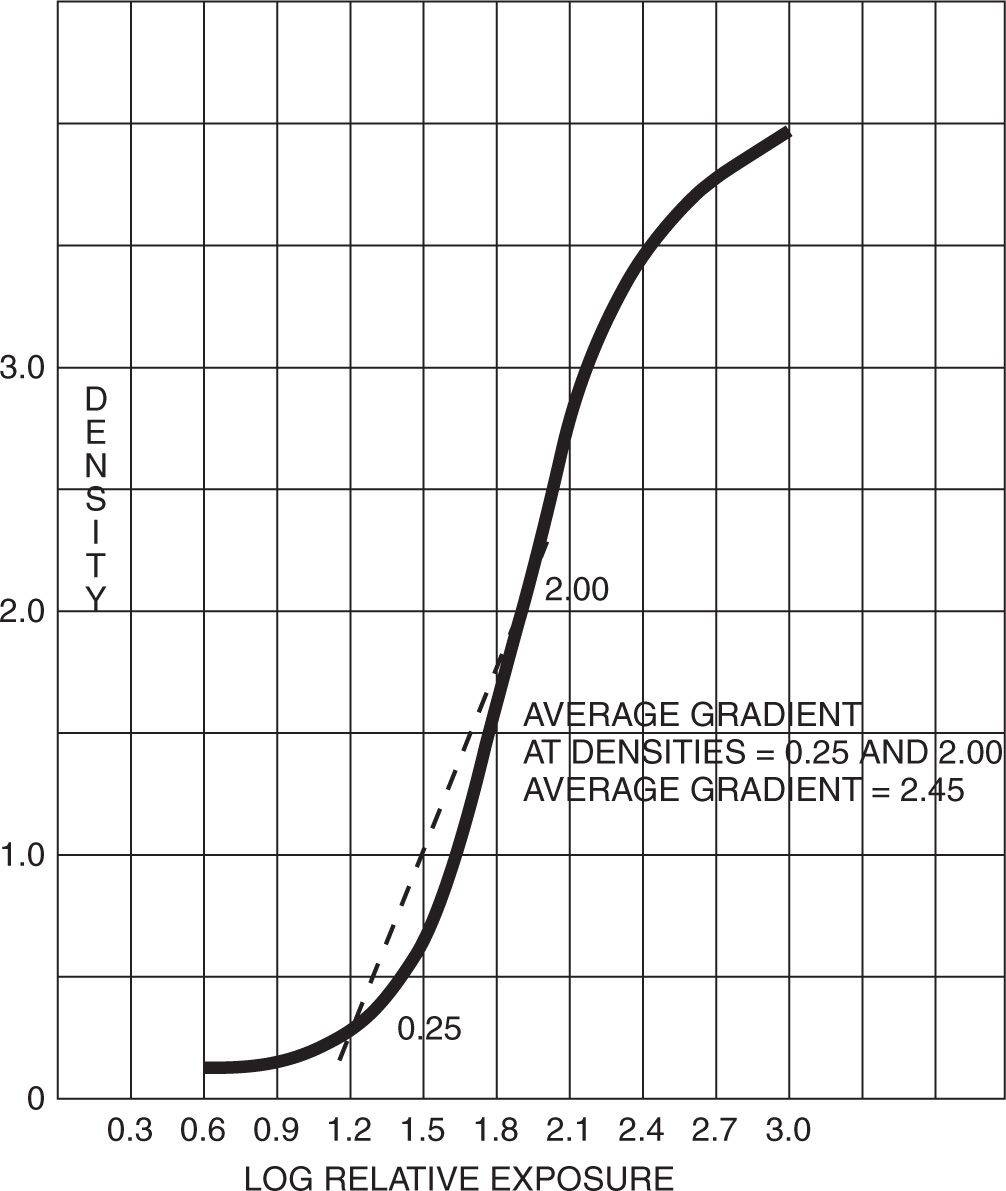
FIGURE 2-9. Determination of average gradient.
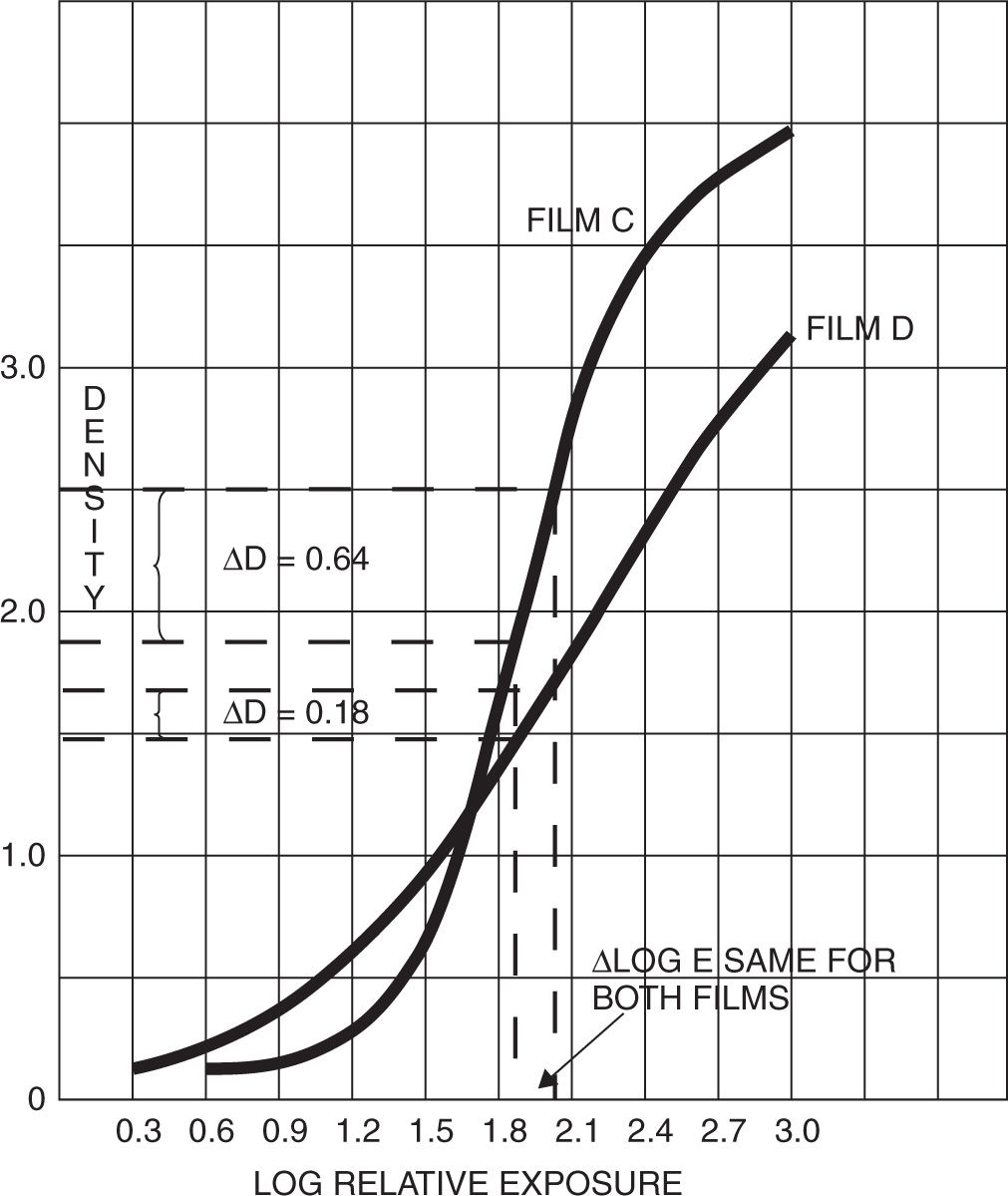
FIGURE 2-10. Differences of film contrast and speed result in changes of curve shape and position, respectively.
Contrast
Contrast is primarily responsible for allowing the visibility of detail. There are two types of contrast: radiographic and subject. Radiographic contrast is the variation or difference in densities that allows one to discern between two adjacent densities within the image. It is influenced by the type of intensifying screen, the film’s density and characteristic curve, and processing. Subject contrast is the result of attenuation differences as the x-rays pass through a body part; it is affected by tissue thickness, type, atomic number, and density.

FIGURE 2-11. Example of contrast scale. Aluminum step wedge: The left image was produced using 50 kVp. It demonstrates higher contrast (short gray scale, smaller number of steps). The right image was produced with 70 kVp and demonstrates lower contrast (long gray scale, larger number of steps).
The two scales of contrast, long and short, are differentiated in Box 2-1 and Figure 2-11. A short scale of contrast is most appropriate for radiography of the foot and ankle, which primarily concerns bone anatomy (trabeculations, cortex) and distinguishing the bone margins from adjacent soft tissue. Abdominal radiography would require a longer scale of contrast to visualize the different soft tissue structures that have more similar densities.
BOX 2-1 Characteristics of Short-Scale and Long-Scale Contrast
Short-Scale Contrast | Long-Scale Contrast |
High contrast | Low contrast |
Limited number of gray shades | Increased number of gray shades |
Increased contrast | Decreased contrast |
Lower level of kilovoltage | Higher level of kilovoltage |
Limited areas of visibility | Thicker areas more visible |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








