Chapter 52 Unicompartmental Knee Arthroplasty in Anterior Cruciate Ligament–Deficient Knees
Management of unicompartmental osteoarthrosis of the knee continues to generate controversy. The 1970s and 1980s cast doubt on the benefit of a unicompartmental knee arthroplasty (UKA) as a surgical option for knee arthritis. However, more recent studies support the increased use of UKA based on lower morbidity, cost efficiency, longevity, and efficacy of unicompartmental arthroplasty.11,17 Symptomatic unicompartmental gonarthrosis in young and active patients with preexisting anterior cruciate ligament (ACL) deficiency has been a challenging problem that is being encountered on a more frequent basis with younger patients presenting for surgical intervention. The goal of surgical management remains the same—to offer the patient an intervention that will provide lasting symptom relief of both instability and osteoarthritic symptoms. With the advancements in implant designs and surgical techniques, various options exist for the treatment of unicompartmental knee gonarthrosis. Surgical options such as arthroscopic débridement, cartilage replacement techniques, with or without realignment osteotomy, and concomitant ACL reconstruction have their limitations, because ACL reconstruction addresses the instability but not the degenerative process. Realignment osteotomy with or without ACL reconstruction may improve the patient’s symptoms but does not completely relieve pain, and progression of contralateral compartment gonarthrosis remains an issue.14 In ACL-deficient knees, previous studies have demonstrated disappointing results when UKA alone, without ACL reconstruction, was performed to address unilateral gonarthrosis.7,9
Indications and Contraindications
Scott and colleagues13 have provided a framework for describing recommended indications and contraindications for unicompartmental knee arthroplasty. Their initial inclusion criteria include a diagnosis of unicompartmental gonarthrosis, age older than 60 years, low activity demand, weight less than 82 kg, minimal pain at rest, arc of motion more than 90 degrees, less than 5 degrees flexion contracture, and an angular deformity less than 15 degrees that is passively correctable to neutral. Initial contraindications to UKA were inflammatory arthritis, patient age younger than 60 years, high activity level, patellofemoral or pain in the contralateral compartment, and ACL-deficient knees.3,13 However, recent studies have reported good or excellent results in patients who underwent UKA despite not falling within the traditional indications. A retrospective series of patients with UKA aged 60 years or younger (range, 35 to 60 years) demonstrated an excellent survivorship of 92% at 11 years.15,16 Moreover, a series published by Tabor and associates20 has demonstrated comparable survival and clinical outcomes of UKA in obese patients with a body mass index (BMI) more than 30 at up to 20 years compared with nonobese patients. In general, there are reports of fixed-bearing UKA designs, such as the Miller-Galante (Zimmer, Warsaw, Ind) and Marmor UKAs (Smith & Nephew, Memphis, Tenn) reporting no higher failure rates in heavier patients.19 Therefore, increased weight and activity are not considered an absolute contraindication of fixed- or mobile-bearing UKAs. Failures in these types of patients may in part also be attributed to certain implant designs and/or surgical technique.1
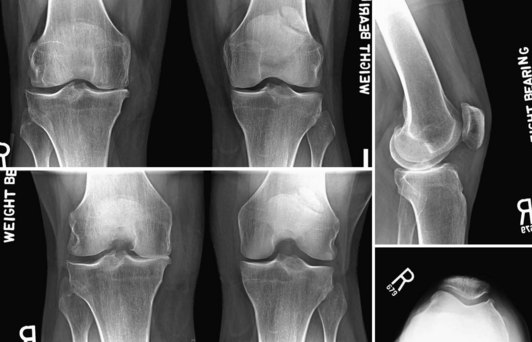
Preoperative weight-bearing anteroposterior (AP) standing, flexed posteroanterior (PA) or Rosenberg standing, and lateral standing radiographic views are necessary and helpful. A lateral standing x-ray is useful for identifying wear pattern and predicting whether the ACL is intact.12 Preoperative films clearly demonstrate a more posterior wear pattern on the lateral standing x-ray, suggesting ACL insufficiency (Fig. 52-1). Preservation of the lateral tibiofemoral and patellofemoral compartment may provide further support for considering a combined UKA and ACL reconstruction. Obtaining a preoperative magnetic resonance imaging (MRI) scan may also be useful in identifying other unforeseen soft tissue abnormalities and evaluating the integrity of the articular surface and meniscus in the contralateral compartment.
Unicompartmental Knee Arthroplasty in the Anterior Cruciate Ligament–Deficient Knee
The debate continues as to whether a functional ACL is necessary for successful implantation of a unicompartmental knee arthroplasty. Most adult reconstruction surgeons agree that an intact and functional ACL is necessary to have a successful outcome with a UKA.8 However, two large series with a minimum of a 9- to 10-year follow up demonstrated good to excellent results with UKA, even in ACL-deficient knees.4,5 A 10-year follow up of 60 Marmor UKAs included 10 knees with ACL deficiency at the time of surgery, none of which required revision arthroplasty surgery; 7 of 10 were asymptomatic, 2 knees demonstrated mild instability, and 1 knee required a revision ACL reconstruction. It remains unclear whether these patients were young and active or older and less active. Cartier and coworkers4 have suggested that these osteoarthritic ACL deficient knees were stable because there was no other soft tissue disruption and additional stability was provided by the formation of osteophytes. However, removal of these osteophytes during implantation of a UKA, especially meniscus-bearing designs, could accentuate instability and potentially lead to changes in wear pattern or even dislocation of the meniscal component. Hernigou and colleagues10 have also demonstrated that the degree of posterior slope is associated with the outcome of a UKA. In their series, 81 of 99 knees had an intact ACL at the time of unconstrained UKA implantation. Of the 18 knees in which the ACL was absent at the time of implantation, 11 still had the implant in situ at a mean follow-up of 17 years. In these 11 knees, the posterior slope was less than 5 degrees. Of the 7 ACL-deficient knees that required revision, mean slope was greater than 8 degrees and anterior tibial translation was greater than 10 mm, as observed on a single-stance lateral radiograph. Previous studies have also demonstrated that every 10-degree increase in posterior tibial slope is associated with a 6-mm increase in anterior tibial translation in monopodal stance.6
Furthermore, increased anterior tibial translation ultimately leads to an increased sliding motion or tibiofemoral subluxation that may result in accelerated wear and failure of the polyethylene (PE) component or dislocation in mobile-bearing designs. Fixed-bearing designs may have an advantage over mobile-bearing designs by eliminating the possibility of a meniscus-bearing dislocation; however; at this time; no data exist to support this. Argenson and associates2 used videofluoroscopy to evaluate the tibiofemoral contact areas in 20 subjects implanted with a UKA. Normal axial rotation was observed in 12 of 17 patients after medial UKA and 2 of 3 patients after lateral UKA. Abnormal axial rotation seen in the other subjects may have been caused by the inability of the ACL to pull the femur anteriorly in full extension. The authors suggested that the ACL plays a significant role in knee kinematics and may ultimately contribute to UKA longevity. Suggs and coworkers18 have performed an in vitro robotic study to determine the role of the ACL in the anterior-posterior stability of the knee after UKA. After UKA, the knee exhibited tibial translation and forces in the ACL similar to those of the native knee. The ACL-deficient knee after UKA, however, demonstrated significantly greater anterior tibial translation than both the native knee and the knee after UKA with an intact ACL. Their data suggest that medial UKA does not alter the anterior stability in the knee with an intact ACL, but that a functional ACL is necessary to ensure normal mechanics after UKA.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree