Chapter 107 Cemented Total Knee Arthroplasty
The Gold Standard
Evolution of Cementless Fixation
Cementless fixation was developed as a response to early failures of total hip arthroplasty (THA) in young patients. Cemented total hips did poorly in this subset of patients. Dorr et al reported a 67% revision rate in patients undergoing cemented total hips who were younger than 45 years of age.9 Ranawat et al reported a 30% radiographic loosening rate in patients who had cemented total hips between ages 40 and 60.28 Sullivan et al looked at 90 patients with an 18-year follow-up, all of whom were younger than 50 years old, and found that 50% of the acetabular components loosened, while 8% of the stems loosened.36 In an effort to improve the long-term results of hip replacement, cementless fixation was offered as a potential solution. The transition from cemented total hip arthroplasty to cementless total hip arthroplasty in young patients has been truly successful. Tapered or extensively coated cementless femoral hip implants have demonstrated outstanding clinical results at long-term follow-up. In addition, the success and durability of modern cementless femoral components in young patients are well documented.35 At this point in time, many authors would suggest that total hip fixation is a solved problem.
Rationale for the Use of Cementless Total Knee Arthroplasty
Reduced operative time is probably the most seductive reason for a surgeon to use this technology. By eliminating the 15 to 20 minutes per case needed for polymerization of the cement, the surgeon can complete the procedure in a timely manner. In the age of diminishing reimbursement, this certainly is enticing. In addition, elimination of cement from the surgical procedure removes a possible source of third body wear. Retained cement has been shown to be a leading factor in the damage of retrieved polyethylene inserts and has the potential to be a source of increased polyethylene wear and osteolysis.7,22,27,37
Another potential advantage of cementless knee fixation is ease of revision. In the absence of cement interdigitation, component removal is simplified. The interface between the host bone and the prosthesis is divided, and there is no need to remove embedded cement fragments. Additionally, when porous implants have failed to show ingrowth, removal is easily accomplished with disruption of the fibrous membrane. The resultant bone is usually a sclerotic bed that can be prepared for revision implants with only a few millimeters of bone resection. However, data have shown that the results of revision of a failed cementless implant to a cemented construct are similar to those of a failed cemented knee revised with cement.13
The main advantage of cementless fixation in young patients is the potential for improved longevity. With improved success of TKA, indications are being expanded to younger patients. Concern remains regarding the durability and longevity of a cemented TKA in the young, more physically demanding patient population. In addition, recent demographic data suggest that by 2011, nearly 50% of all TKAs will be performed in patients younger than age 65.26 These factors are the driving force behind the evolution to cementless total knee fixation.
Once a cementless implant becomes osseously integrated, it is extremely rare for it to subsequently loosen. This outcome certainly is attractive for our younger patients. In contrast, concern has arisen that the bone-cement interface has the potential for late deterioration, especially in young, active patients. Although this failure mechanism is possible, it occurs infrequently. It must be recognized that a cemented knee replacement is loaded primarily in compression—a force well tolerated at the bone-cement interface. This is distinctly different from hip replacement in which the forces on the cement-bone interface are a combination of tension, compression, and shear. Although such forces can lead to early failure in young, active hip patients, little evidence in the literature substantiates that deterioration of this interface is a significant problem in young, cemented knee replacement patients.6,8,12,30,32
Results of Cemented Total Knee Arthroplasty
To justify this change to a cementless design, we first must analyze the currently available data on cemented TKA to determine whether in fact change is necessary. Second, we must determine whether cementless designs eliminate concerns associated with cemented TKA. An evidence-based approach to the current literature offers the best opportunity to do so. To date, true long-term prospective studies comparing the results of cemented versus cementless TKA are scarce and fail to show the advantages of a cementless design.1
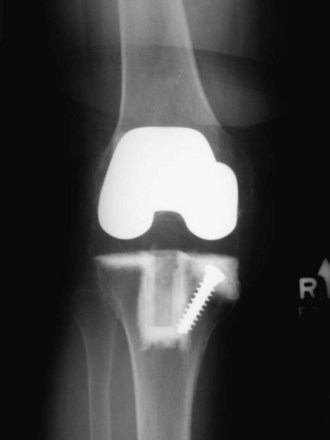
The long-term results of cemented TKA in all age groups are outstanding (Fig. 107-1). Without stratifying for age, multiple published articles cite a greater than 90% success rate. Scuderi et al, looking at 1200 posterior stabilized knees, had 98% good or excellent results.33 Ranawat et al, reporting on a 14-year survivorship of cemented total knee replacement, described a 95% success rate.29 Font-Rodriguez et al, upon evaluating more than 2000 posterior stabilized metal-backed knees at 14 years’ follow-up, noted a success rate of 98%.16
Cemented Total Knee Arthroplasty in Young Patients
Initial reports of mid- to long-term results of cemented condylar knee design in young patients have been encouraging. Ranawat reported a 94% ten-year survivorship in patients younger than 55 years of age using cemented fixation.30 Gill reported 98% good or excellent results at 10 years in his cemented total knee patients younger than 55 years,19 Diduch et al, in evaluating 118 patients younger than 55 had 94% good or excellent results at 8 years using cemented fixation.8
More recent reports have echoed these results, indicating the continued durability of a cemented condylar knee design in a young, high-demand patient population. Ritter and colleagues reported on 207 cemented cruciate-retaining TKA patients younger than age 55.32 The survival rate at 12 years was 94.8%. Duffy and coworkers reported a 96% survivorship at 10 years using a Press-Fit condylar prosthesis (Depuy, Warsaw, Ind) on patients younger than 55 years.12 No revisions for aseptic loosening were required.
Comparative Literature: Cement versus Cementless
Numerous studies reported in the literature directly compared cemented fixation versus cementless fixation in TKA.11,17 Rand and associates looked at more than 11,000 TKAs and performed a survivorship analysis at 10 years. When cemented fixation was used, 92% of total knees were successful, compared with only 61% successful without cement (P < .001).31 Barrack and colleagues examined 82 cementless rotating platform knees and compared them with 76 cemented rotating platform mobile-bearing knees.2 Eight percent of cementless knees were revised, and no cemented knees were revised. The cementless knees had significantly lower Knee Society scores. Gioe et al evaluated 5760 knees treated with various implants and methods of fixation and found that cementless total knees had the lowest survival rate of all implants reviewed.20 Berger and coworkers, in evaluating 131 cementless total knees at a mean follow-up of 11 years, found that 8% of the tibial components never achieved ingrowth.3 The authors of this article and designers of this implant commented that they have abandoned cementless fixation in TKA. Duffy and colleagues and Gioe and coworkers reported the results in a community-based registry on TKA in patients younger than 55 years.21 Patients were implanted with 1047 joints of three predominant designs by 48 surgeons in four hospitals associated with a community joint registry. The mean age for this cohort was 49.8 years, and 62.8% (657/1047) of the patients were female. A total of 73 revisions were performed—5.6% (37/653) in women and 9.2% (36/394) in men. Cemented TKAs performed best, with a cumulative revision rate of 15.5%, compared with 34.1% in cementless designs. Eighty-five percent of cemented TKA implants survived at 14 years in the population younger than 55 years, and cementless designs were an independent risk factor for revision.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree