Chapter 23 Tuberculosis and Other Unusual Infections
Tuberculosis
Operative Treatment
Foot
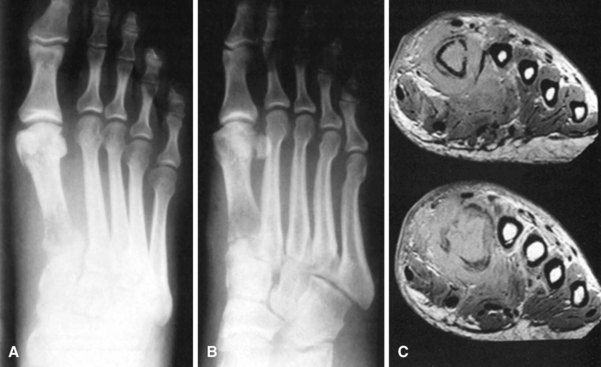
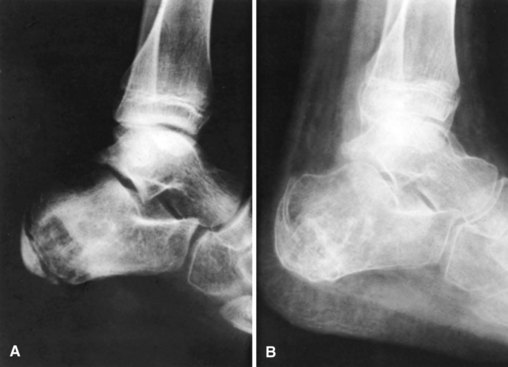
In tuberculosis of the foot (Fig. 23-1), many bones may become involved, and a delay in diagnosis increases the risk of joint involvement. Operative indications include juxtaarticular focus or joint destruction. Bones with cystic changes typically respond better than rheumatological-appearing joints. When present, isolated lesions usually involve the calcaneus or talus. When several bones are involved, especially in adults, amputation is the procedure of choice. Curettage is indicated for isolated lesions even when sinuses are present.
Curettage for Tuberculous Lesions in the Foot
 Make an incision directly over the lesion or directly through a sinus or abscess, if present.
Make an incision directly over the lesion or directly through a sinus or abscess, if present.
 Remove all necrotic and scarred tissue but not uninvolved osteopenic bone.
Remove all necrotic and scarred tissue but not uninvolved osteopenic bone.
 Pack the cavity with autogenous cancellous bone, and close the incision (Fig. 23-2).
Pack the cavity with autogenous cancellous bone, and close the incision (Fig. 23-2).
 In the presence of secondary infection, omit the bone grafts and close the incision loosely over drains.
In the presence of secondary infection, omit the bone grafts and close the incision loosely over drains.
When lesions involve the subtalar or midtarsal joints, a triple arthrodesis is indicated (see Chapter 34). When the subtalar and the ankle joints are affected, posterior arthrodesis (see Chapter 11) of these joints can be done.
Excision of Metatarsal
 In the presence of secondary infection, make a longitudinal incision over the affected bone extending from the distal row of the tarsus to the middle of the proximal phalanx.
In the presence of secondary infection, make a longitudinal incision over the affected bone extending from the distal row of the tarsus to the middle of the proximal phalanx.
 Expose the bone without injuring the extensor tendons.
Expose the bone without injuring the extensor tendons.
 Excise the bone with the periosteum intact, and close the wound loosely over drains.
Excise the bone with the periosteum intact, and close the wound loosely over drains.
Excision of Cuneiform Bones
 Make a 5-cm longitudinal incision laterally, and expose the joint between the cuboid and fifth metatarsal.
Make a 5-cm longitudinal incision laterally, and expose the joint between the cuboid and fifth metatarsal.
 Approach the first cuneiform and the base of the first metatarsal through a similar medial incision.
Approach the first cuneiform and the base of the first metatarsal through a similar medial incision.
 Expose the second and third cuneiforms by subperiosteal dissection.
Expose the second and third cuneiforms by subperiosteal dissection.
 Excise the anterior half of the cuboid and the three cuneiforms with an osteotome.
Excise the anterior half of the cuboid and the three cuneiforms with an osteotome.
 Resect the articular cartilage from the anterior surface of the navicular and the bases of all five metatarsals.
Resect the articular cartilage from the anterior surface of the navicular and the bases of all five metatarsals.
 Approximate the denuded surfaces of the metatarsals to those of the navicular and cuboid.
Approximate the denuded surfaces of the metatarsals to those of the navicular and cuboid.
Excision of Navicular
 Expose the midtarsus through an anterolateral approach.
Expose the midtarsus through an anterolateral approach.
 Make an additional medial incision to expose the navicular.
Make an additional medial incision to expose the navicular.
 Excise the navicular by sharp subperiosteal dissection. Avoid injuring the dorsalis pedis artery and the branches of the deep peroneal nerve on the dorsum of the foot.
Excise the navicular by sharp subperiosteal dissection. Avoid injuring the dorsalis pedis artery and the branches of the deep peroneal nerve on the dorsum of the foot.
 Expose the calcaneocuboid joint, and excise the articular cartilage and subchondral bone from the distal end of the calcaneus and the proximal one third of the cuboid.
Expose the calcaneocuboid joint, and excise the articular cartilage and subchondral bone from the distal end of the calcaneus and the proximal one third of the cuboid.
 Remove the articular cartilage from the head of the talus and from the proximal surfaces of the cuneiforms.
Remove the articular cartilage from the head of the talus and from the proximal surfaces of the cuneiforms.
 Approximate the raw surfaces of the denuded bones, obliterating the space. The position can be maintained by crossed, threaded wires.
Approximate the raw surfaces of the denuded bones, obliterating the space. The position can be maintained by crossed, threaded wires.
 After excision of the navicular, a midtarsal arthrodesis should be performed to stabilize the foot in satisfactory alignment.
After excision of the navicular, a midtarsal arthrodesis should be performed to stabilize the foot in satisfactory alignment.
Excision of Cuboid
 Approach the cuboid through an anterolateral approach, and excise it by sharp subperiosteal dissection.
Approach the cuboid through an anterolateral approach, and excise it by sharp subperiosteal dissection.
 Resect the articular surfaces and adjacent bone from the proximal aspect of the cuneiforms and the fifth metatarsal and from the distal surface of the calcaneus.
Resect the articular surfaces and adjacent bone from the proximal aspect of the cuneiforms and the fifth metatarsal and from the distal surface of the calcaneus.
 Excise the navicular, and remove the articular surface and superficial bone from the head of the talus.
Excise the navicular, and remove the articular surface and superficial bone from the head of the talus.
 Approximate the denuded surfaces of the bones, and maintain the position by crossed, threaded wires.
Approximate the denuded surfaces of the bones, and maintain the position by crossed, threaded wires.
Calcanectomy produces considerable disability, but the result may be preferable to amputation.
Excision of Calcaneus
 Begin a Kocher incision (see Technique 1-19) 10 cm proximal to the lateral malleolus, and follow the lateral border of the Achilles tendon to the superior surface of the calcaneus; continue it inferiorly to the lateral malleolus, and end it 2.5 cm distal to the calcaneocuboid joint.
Begin a Kocher incision (see Technique 1-19) 10 cm proximal to the lateral malleolus, and follow the lateral border of the Achilles tendon to the superior surface of the calcaneus; continue it inferiorly to the lateral malleolus, and end it 2.5 cm distal to the calcaneocuboid joint.
 Divide the calcaneofibular ligament, and displace the peroneal tendons superiorly and anteriorly.
Divide the calcaneofibular ligament, and displace the peroneal tendons superiorly and anteriorly.
 Incise the capsule of the calcaneocuboid joint, and divide the ligamentous attachments of the calcaneus in this area.
Incise the capsule of the calcaneocuboid joint, and divide the ligamentous attachments of the calcaneus in this area.
 Insert a periosteal elevator or lamina spreader into the subtalar joint, and divide the interosseous talocalcaneal ligaments.
Insert a periosteal elevator or lamina spreader into the subtalar joint, and divide the interosseous talocalcaneal ligaments.
 Dislocate the subtalar joint; use sharp subperiosteal dissection to free the soft tissues from the medial, anterior, and posterior surfaces; and divide the attachment of the Achilles tendon.
Dislocate the subtalar joint; use sharp subperiosteal dissection to free the soft tissues from the medial, anterior, and posterior surfaces; and divide the attachment of the Achilles tendon.
 Deliver the calcaneus from the wound. Avoid injuring the tibial nerve and vessels on the medial side of the bone.
Deliver the calcaneus from the wound. Avoid injuring the tibial nerve and vessels on the medial side of the bone.
 Suture the Achilles tendon to the inferior surface of the talus and to the short muscles of the foot.
Suture the Achilles tendon to the inferior surface of the talus and to the short muscles of the foot.
Excision of Talus
 Approach the talus through a Kocher (see Technique 1-19) or anterolateral (see Technique 1-22) approach.
Approach the talus through a Kocher (see Technique 1-19) or anterolateral (see Technique 1-22) approach.
 Divide the capsule of the talonavicular joint on its dorsolateral and inferior aspects.
Divide the capsule of the talonavicular joint on its dorsolateral and inferior aspects.
 Divide the components of the fibular collateral ligament of the ankle at their fibular attachments.
Divide the components of the fibular collateral ligament of the ankle at their fibular attachments.
 Dislocate the ankle, and displace the foot medially.
Dislocate the ankle, and displace the foot medially.
 Grasp the neck of the talus and apply slight traction; use sharp subperiosteal dissection to sever all soft tissues and ligamentous attachments on the posterior and inferior aspects from anteriorly to posteriorly, and remove the talus. If the bone is necrotic, it must be removed in pieces.
Grasp the neck of the talus and apply slight traction; use sharp subperiosteal dissection to sever all soft tissues and ligamentous attachments on the posterior and inferior aspects from anteriorly to posteriorly, and remove the talus. If the bone is necrotic, it must be removed in pieces.
 Use subperiosteal dissection to free the soft tissues on both malleoli and both sides of the anterior aspect of the calcaneus.
Use subperiosteal dissection to free the soft tissues on both malleoli and both sides of the anterior aspect of the calcaneus.
 Displace the foot posteriorly, placing the anterior aspect of the calcaneus between the malleoli. The articular surfaces of the calcaneus should approximate the articular surface of the tibia.
Displace the foot posteriorly, placing the anterior aspect of the calcaneus between the malleoli. The articular surfaces of the calcaneus should approximate the articular surface of the tibia.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree