CHAPTER 54 Total Facet Replacement
Facet Anatomy and Function
The lumbar facet joints have been thoroughly studied. Much is known about their loading, biomechanical function, time-related anatomic changes, tropism and asymmetry, modes of articular wear, and soft tissue attachments.1–35
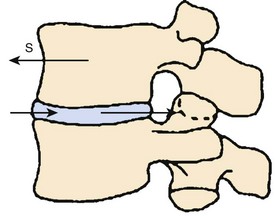
At its most narrow analysis, the facet joint is designed to function as a shear stop—an anterior shear stop (Fig. 54–1). Facet joints prevent anterior shear forces from destroying the disc, which is primarily designed to absorb compressive loads. The disc is so well designed for its purpose that it is essentially impossible to injure the anulus with purely compressive loads.26 Also, the facets control varying amounts of rotation and limit flexion of the lumbar spine,28–3136 but their most important function is to protect the disc from parallel force vectors.
Viewed in this simplified manner, it becomes clearer why degeneration of these lumbar apophyseal joints produces so much spinal pathology. The loss of even 1 mm of cartilage thickness within the facet joint allows a significant increase in anterior-posterior translational motion to occur. This increased motion causes repeated strain of the multifidus muscle and facet capsule ligaments, increases the shear load on the disc and the posterior and anterior longitudinal ligaments, and allows the neural foramen and lateral recess to collapse with flexion and extension of the spine. At the same time, cartilage wear stimulates spur formation in all directions around the facet joint, as cartilage wear typically does in all degenerative synovial joints. These osteophytes encroach further on the neural elements increasing central and lateral stenosis, and the osteophytes may act as a source of pain when they impinge on each other or the pars interarticularis. Degeneration can continue until facet subluxation occurs, producing further stenosis (Fig. 54–2).
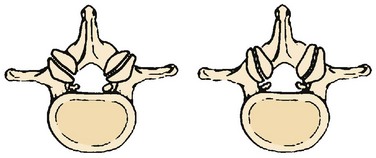
Concomitant with the five degenerative changes in the apophyseal joints—loss of articular cartilage, spur formation, loss of control of anterior shear forces, facet subluxation, and increased anterior-posterior translation—the facets also frequently undergo disadvantageous morphologic changes with aging. These changes undermine the ability of the spine to withstand shear forces. In infant spines, the facets are primarily coronally oriented.25 In adult spines, the lumbar facets generally have a small anteromedial coronal component and a large posterior sagittal component (Fig. 54–3). As the spine ages, the facet becomes more and more sagittally aligned with a smaller and smaller coronal component (Fig. 54–4). The coronal part of the facet joint controls shear forces.28 In a presentation at the International Spinal Arthroplasty Society Meeting in Montpelier, France in 2002, DuPont, using finite element analysis, verified how the shear forces across the disc increase as the facets are directed more and more sagittally.
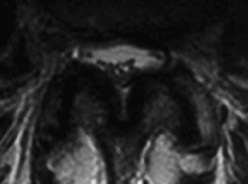
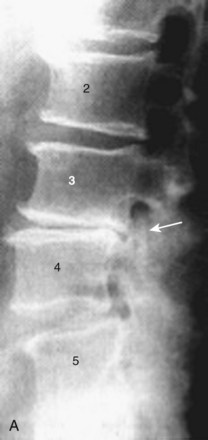
FIGURE 54–4 Sagittally aligned, asymmetric, and dislocated facet joints at L4-5 in a 56-year-old patient.
There is at least one additional force working on the lumbar facet joint. Depending on the position of the spine, the facets absorb 0% (in full flexion) to 33% (in full extension) of the compressive (axial) load at a given level.23,37 An incompetent, degenerative facet joint can no longer absorb its share of the compressive loads, which can narrow the neural foramen further in an up-down direction, especially with the spine in extension.
Radiologic Diagnosis and Issues
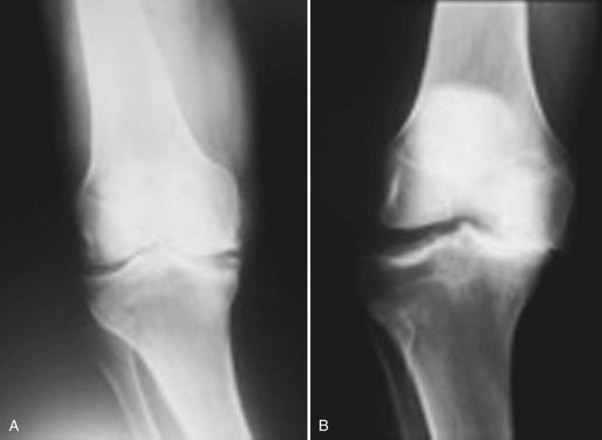
Although excellent radiologic tools have been developed, including computed tomography (CT), CT myelogram, and magnetic resonance imaging (MRI), they may not be used to their fullest advantage. There is no spinal equivalent to the 30-degree weight-bearing anteroposterior view of the knee (Fig. 54–5) to detect cartilage wear or joint laxity. Similar positional views of other joints of the extremities, such as weight-bearing anteroposterior and lateral views of the feet and the 30-degree angle view of the shoulder, have been developed to aid in diagnosing arthritis and instability but not as well with advanced imaging for the spine.
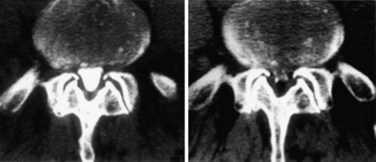
A vest with pantaloons has been developed that can individually manipulate vertebral bodies to obtain much more information on a segmental level, but this is under development, and weight-bearing extension views of the lumbar spine probably will not be ready for initial usage before 2012. Other investigators have developed CT scan techniques to show positional lateral recess stenosis (Fig. 54–6).
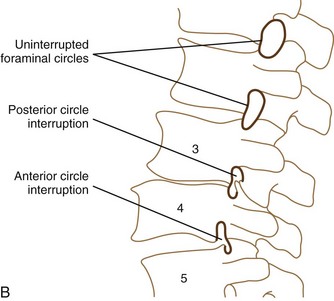
In the same vein, the inferior arc of the pedicle should follow the posterior aspect of the superior and inferior vertebral bodies associated in its foraminal opening, along with the inferior articular process and the arc of the superior articular process. If this circle is unbroken (i.e., the line is smooth) (Fig. 54–7), the foraminal space, at least in a static film, is probably adequate from a bony standpoint. If the proximal end of the superior articular facet or the superior spurs of the inferior articular surface intrude into the hemicircle formed by the pedicle and the inferior facet, the broken foraminal line would indicate facet joint degeneration and possibly suggest instability. This line can be assessed on flexion and extension films and is a more subtle sign than measuring the number of millimeters of spondylolisthesis. An additional sign within the foramen to aid in diagnosis could be the intrusion sign of the superior endplate into the intervertebral foramen. Figure 54–7 illustrates both abnormalities, the former at L3-4 and the latter at L4-5.
Current Treatment of Posterior Lumbar Degeneration
All of these operations have their successes and their failures with quite a bit of variability as reported in the literature. Wide decompressive laminectomy has been shown to have 57% to 85% good results at 4 years.38–41 Postoperative problems and complications include segmental instability, recurrent spinal stenosis, continued back pain, infection, neural injury, and dural tears.35,42
Decompression and arthrodesis are the mainstays of treatment for degenerative facets. Numerous fusion techniques and associated implantable instrumentation are available, and the operation has improved to the point where a successful radiographic fusion is the rule. As Vaccaro and Ball42 have written, “Though the majority of studies have shown that the radiographic fusion success rate is improved with the addition of internal fixation, the benefits in the majority of degenerative spinal disorders are unclear in terms of patient function.” Some of the complications from combined decompression and fusion include 3% to 6% infection rate,43 continued pain, juxtasegmental instability or fracture (Fig. 54–8), failed fusion, and failed hardware.
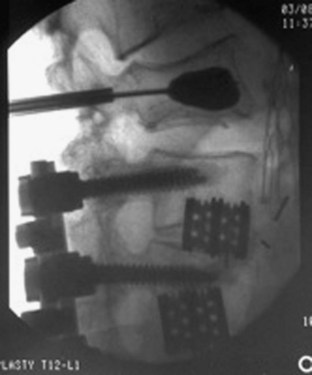
FIGURE 54–8 Vertebral body fracture with kyphoplasty repair of fracture occurring above spinal fusion.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree