CHAPTER 78 Thoracic and Lumbar Spinal Injuries
Incidence
The thoracolumbar junction is the most common injury site for thoracic and lumbar trauma. Most patients are young males involved in high-energy accidents. More than half of fractures occur between T11 and L1, and another 30% occur between L2 and L5.1–3 More than 50% of injuries are sustained in motor vehicle accidents, and another 25% are sustained in a fall from greater than 6 feet. Complete neurologic injuries occur in about 20%, and incomplete neurologic injuries occur in about 15% of patients. Associated injuries including fractures, head trauma, pulmonary injuries, and intra-abdominal injuries occur more than 50% of the time. Noncontiguous spine injuries remote from the site of the primary injury occur in 5% of patients.1–3
Anatomic Considerations
Considerable anatomic differences exist throughout the thoracolumbar spine, contributing to the differences in spinal injury patterns in the thoracic spine, thoracolumbar junction (T11 to L2), and lower lumbar spine. The thoracic spine is kyphotic and has the greatest amount of intrinsic stability because of the rib cage, but it also has a relatively narrow canal that gives little reserve for neural element protection after spine trauma.4 Axial rotation is greater in the thoracic spine than the lumbar spine because of the coronal alignment of the facets. The lower lumbar spine is lordotic and has the greatest amount of flexion and extension capabilities due to the sagittal facet joint orientation.5,6 The human body’s center of gravity is anterior to the thoracic and thoracolumbar spine, which places compressive forces on the vertebral bodies and tensile forces on the posterior ligamentous structures in the upright position. The center of gravity is located more posteriorly in the lower lumbar spine, in part due to the greater degree of regional lordosis, and the posterior elements, in particular the osseous components, experience significant compressive rather than tensile forces in the upright position.7–10 The posterior osteoligamentous complex consists of the lamina, facets, facet joint capsules, and interspinous ligaments. These structures are commonly referred to as the posterior ligamentous complex, reflecting the key role of the ligaments in maintaining spinal stability when there is injury to the vertebral body and intervertebral discs. The lower lumbar spine is inherently stable and somewhat protected from injury due to its lordotic configuration, distribution of compressive forces across the vertebral bodies and posterior elements, and relatively large vertebral bodies. The thoracolumbar junction is the transition zone from the rigid, stable kyphotic thoracic spine to the mobile, lordotic, relatively stable lower lumbar spine and is therefore particularly susceptible to injury.
Mechanisms of Injury
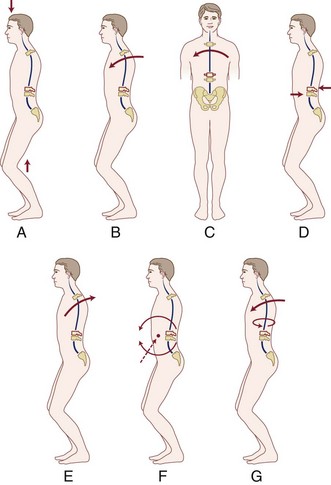
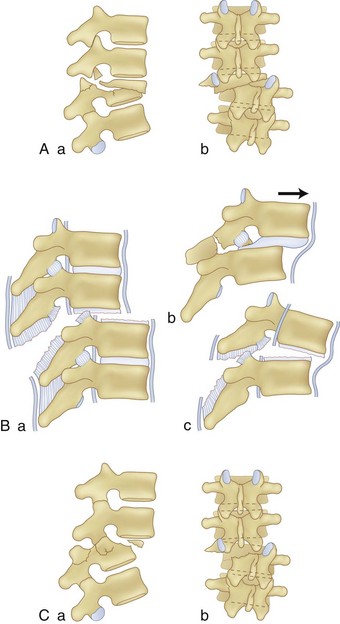
Thoracic and lumbar spinal injury patterns can usually be explained by the application of one or two force vectors. These forces cause relatively consistent injury types that serve as the basis for the main classification schemes, which are described later. The most common primary forces are axial compression, lateral compression, flexion, extension, distraction, shear, and rotation (Fig. 78–1A-E). The most common force combinations are flexion-rotation and flexion-distraction (Fig. 78–1F-G).
Initial Evaluation and Management
Associated injuries are common including chest and abdominal injuries, orthopedic injuries including pelvis and extremity fractures, head trauma, as well as contiguous and noncontiguous spine injuries.11,12 The potential for these injuries must be kept in mind and reassessed periodically, especially in the early stages and in obtunded or severely injured patients who cannot direct attention to their injuries. The initial assessment and subsequent surveys should be systematic and thorough from head to toe, knowing that even in the highest volume and most experienced trauma centers, injuries in the spine and elsewhere sometimes go undetected and can have significant functional consequences.3,13–15
The use of pharmacologic agents in spinal cord injury as part of the initial resuscitative protocol has been extensively studied and debated. The rationale is to minimize the harmful secondary cascade of events such as the inflammatory response and oxidative cell injury that occurs after mechanical injury to the spinal cord. The National Acute Spinal Cord Injury Studies (NASCIS II and III) examined methylprednisolone, naloxone, and tirilazad. If administered within 8 hours of injury, there may be improvement in long-term neurologic function with high-dose methylprednisolone. The study dose was a bolus of 30 mg/kg, followed by a 5.4 mg/kg/hour infusion for 23 hours if therapy is initiated within 3 hours of injury or 48 hours if initiated at 3 to 8 hours after injury. There are significant potential complications such as pneumonia, postoperative wound infection, gastrointestinal bleeding, and sepsis with the use of steroids.16–18 Steroids have not been shown to be effective in purely lower-motor neuron lesions. GM-1 ganglioside has been studied as well.19 The use of steroids has not been universally accepted and remains controversial but can be considered as a treatment option, as can GM-1 ganglioside.20 There is interest in systemic hypothermia after spinal cord injury, but clinical data are limited.21
Initial Neurologic Evaluation
Neurologic injury may have a profound effect on a patient’s ultimate function, and the presence or absence of a neurologic deficit often guides subsequent injury management including operative versus nonoperative treatment. A detailed neurologic examination is therefore critical and consists of testing of motor and sensory function and reflexes in a sequential and systematic manner. Findings should be carefully documented to enable accurate assessment of neurologic deterioration or recovery. Motor function is assessed in the main muscle groups in the upper and lower extremities, which can sometimes be difficult in an injured extremity, but every attempt should be made under these circumstances. Motor function should be graded on a 0 to 5 scale. A score of 5 is normal with full range of motion against gravity and resistance, 4 is full range of motion against gravity and slight resistance, 3 is full range of motion against gravity only, 2 is full range of motion only with gravity eliminated, 1 is palpable or visible contraction of a muscle without joint motion, and 0 is a muscle without any function. Rectal sphincter tone and volitional control should be tested as well. Sensory function should be assessed in a dermatomal distribution. This should include testing of the perineal region because sparing of the sacral dermatomes may provide an indicator for functional recovery in patients sustaining a spinal cord injury. Temperature, pain, and light touch are spinothalamic tract functions and can be assessed with a sterile needle and an alcohol swab. Vibration and position sense are posterior column functions and can be assessed with a tuning fork and limb or digit positioning. Reflexes include superficial abdominal (stroking of the abdominal skin causes the umbilicus to be drawn toward the stimulated area, above the umbilicus T7-T10, below the umbilicus T11-L1); cremasteric (in males, stroking of the inner thigh causes the scrotum to be drawn upwards, T12-L1); patellar tendon (quadriceps reflex or knee jerk, L3-L4); Achilles tendon (ankle jerk, S1); anal wink (anal sphincter contraction with stimulation of the perineal skin, S2-S4); and bulbocavernosus reflex (described later, S2-S4). Pathologic reflexes indicating an upper motor neuron lesion include clonus and an abnormal Babinski test. The Babinski test is normal when a stroke along the lateral plantar aspect of the foot results in down-going toes and is abnormal with up-going toes. The neurologic examination is covered in greater detail in Chapter 11.
Neurologic Injury Classification
The central cord syndrome usually involves an injury to the cervical spine in older patients and is characterized by upper extremity weakness with relative sparing of the lower extremities and sacral nerves. Although this injury pattern usually applies to cervical spine injuries because of the upper extremity involvement, Bohlman described a central cord injury pattern in thoracic spine trauma with a greater degree of muscle weakness in the trunk and proximal muscle groups with relative sparing of the distal muscle groups and preserved bowel and bladder function.22 Although the central cord syndrome is the most common of the incomplete patterns when considering all spinal cord injuries, it is rare when cervical injuries are excluded and thoracic injuries alone are considered. The anterior cord syndrome is the most common incomplete pattern in thoracic spine injury, characterized by loss of all motor and most sensory function below the level of the lesion, with sparing of the vibratory and position sense via the posterior columns.22 This has a poor prognosis for recovery and is a debilitating injury pattern. The posterior cord syndrome is rare and involves loss of vibratory and position sense. Patients cannot rely on tactile lower extremity feedback for spatial orientation and must use visual cues when ambulatory. They have preserved bowel and bladder function. The Brown-Séquard syndrome is usually a result of cord hemisection by penetrating trauma and is characterized by ipsilateral loss of motor function and contralateral loss of pain, temperature, and light touch sensation. Patients typically have preserved bowel and bladder function, are ambulatory but may require assistive devices, and have the best prognosis for recovery of the incomplete spinal cord injury syndromes.
The conus medullaris marks the anatomic transition from the upper motor neurons of the spinal cord to the lower motor neurons of the cauda equina and is usually found at the T12-L1 levels. The conus medullaris injury pattern is characterized by flaccid paralysis, loss of reflexes, and sensory loss of the lower extremities with bowel, bladder, and sexual dysfunction. Injury to the cauda equina below the conus medullaris is a purely lower motor neuron injury and presents with the same types of findings as with conus medullaris injury, except that there is a higher incidence of asymmetric involvement and can occur at any level below the conus medullaris. These injuries may be complete or incomplete.23,24
Radiologic Evaluation
Anteroposterior (AP) and lateral conventional radiographs of the thoracic and lumbar spine are the most basic imaging modalities available. A swimmer’s view of the upper thoracic spine may be necessary to visualize the vertebral bodies through the shoulder region. The lateral radiograph is used to examine the height, width, and alignment of the vertebral bodies, pedicles, spinal canal, neural foramina, facets, and spinous processes. The cortical margins of the vertebral bodies should be smooth and contiguous and, when viewed in conjunction with adjacent vertebral bodies, should form a gently arcing line both at the anterior margin (anterior vertebral body line) and posterior margin (posterior vertebral body line). The AP radiograph allows assessment of coronal alignment, interpedicular distance, and alignment of the spinous processes and best visualizes the ribs and transverse processes. Anterior wedging of the vertebral body with a break in the anterior cortical margin signifies a compression fracture. Loss of posterior vertebral body height, a break in the posterior vertebral body cortical margin, spinal canal narrowing, and widening of the interpedicular distance signifies a burst fracture.25 The posterior vertebral body angle can also be used to distinguish subtle burst fractures from compression fractures.26 Facet widening; spinous process splaying or malalignment; fracture lines in the pedicle, lamina, facets, and spinous processes; and vertebral body translation signifies injury to the posterior elements including possible ligamentous injury and are radiographic markers of potential instability.27 Conventional radiography of the thoracolumbar spine has technical, logistical, and diagnostic limitations and therefore CT has become a key modality in evaluating thoracolumbar trauma.
Many trauma centers now use screening spiral CT of the chest, abdomen, and pelvis as part of the standard trauma evaluation. These images include collateral thoracic and lumbar spine information, and as a result, some centers are adopting CT protocols as the initial screening radiologic modality for spine trauma.28–30 Studies have shown that CT scans have a higher sensitivity than conventional radiographs in the detection of thoracic and lumbar spine fractures, although this applies mainly to stable rather than unstable fractures.31–33 CT is better than conventional radiography at discerning compression fractures from burst fractures, and misdiagnosis may occur in up to 25% of injuries when relying on conventional radiography alone.34–36 Screening CT scans may decrease the incidence of missed, delayed, or incorrect diagnoses of thoracic and lumbar trauma, especially in obtunded and multiply injured patients, but the clinical significance of this has not been determined and it is not standard in all trauma centers to obtain screening CT scans. The typical protocol for a trauma-screening CT scan consists of sequential 5-mm axial images with or without reconstructions, whereas a dedicated spine CT protocol consists of 2- to 3-mm axial images with sagittal and coronal reconstructions. It may be necessary to obtain a dedicated spine protocol CT scan if it seems that some important detail may not have been imaged during the screening examination. If the thoracic or lumbar spine injury is initially diagnosed on conventional radiographs alone and a high-energy mechanism is known or suspected, a dedicated spine protocol CT scan should be considered. The main limitation of CT is the limited ability to visualize the soft tissues, for which a MRI scan may be useful.
MRI allows for high-resolution imaging of soft tissues and is particularly important in the evaluation of spinal cord injury because the neural elements can be visualized. This helps in delineating edema, hemorrhage, hematoma, compression, and transection of the neural elements. MRI findings may contribute to the understanding of injury severity including the potential for spinal instability and the need for surgical intervention, and they may be useful for predicting the potential for neurologic recovery.37 Hemorrhage within the spinal cord and edema extending over multiple cord levels are correlated with poor prognosis for neurologic recovery.38–40 The posterior ligamentous structures can be reliably evaluated with MRI.41–44 Unless contraindicated, MRI should be considered in all cases with neurologic injury and in cases where further evaluation of the posterior ligamentous complex is necessary in deciding between operative versus nonoperative treatment. The main limitations for MRI are logistics, cost, and the inferior visualization of the bony elements, so MRI is usually complementary to CT rather than a substitute.
Concept of Spinal Stability and Its Role in Fracture Classification Systems
Spinal mechanical stability refers to the structural integrity of the spinal column and in its simplest form is the ability to resist physiologic loads without progressive deformity or damage to the neural elements.45 Spinal neurologic stability refers to the presence or absence of a neurologic deficit. The concept of mechanical stability serves as the basis for the main recognized fracture classifications and, more recently, attempts have been made to incorporate neurologic stability into the classification schema. Classification systems are potentially useful for communication, research, determining prognosis, and guiding treatment. With respect to thoracic and lumbar spine injuries, certain fracture patterns and associated injury mechanisms have been recognized and terminology has evolved to form a core group of specific injuries with relatively consistent nomenclature, even though there is not a universally accepted classification system. The majority of fractures can be grouped into these main well-recognized categories, but some injuries are of a mixed pattern and are not readily classifiable. The underlying theme of modern classification systems is to determine whether or not an injury is mechanically stable, and the lack of universal acceptance of one classification system reflects the great difficulty in assessing stability in some cases. As the injury severity increases, so does the degree of instability, but this occurs along a continuum and it is not always possible to determine the point where the transition from a stable injury to an unstable injury occurs. Despite intense work in this area, assessment of mechanical stability remains a judgment call at times, and this mainly explains the disparity in treatment approach for certain injuries (especially burst fractures) from one surgeon to the next.
Fracture Classification Systems
Classifications have evolved since their introduction in the mid-20th century. Descriptions of thoracic and lumbar injuries first appeared in print publications in the mid-1900s.46–48 Nicoll49 credited these early authors and classified injuries as anterior wedge fractures, lateral wedge fractures, fracture-dislocations, and isolated neural arch fractures in 1949. Holdsworth expanded on this classification and detailed the traumatic forces causing distinct fracture patterns, described as flexion, flexion and rotation, extension, and compression. He conceptualized the two-column theory of spinal stability, with the anterior column resisting compressive loads and the posterior ligamentous complex resisting tensile forces. Wedge compression and compression burst fractures were considered stable due to preservation of the posterior ligamentous complex integrity, whereas dislocations, extension fractures and dislocations, and rotational fracture-dislocations were considered unstable.50 Kelly and Whitesides51 built on Holdsworth’s work and formally presented the two-column theory as a conceptualization of spinal stability as it relates to spine trauma. These classification systems did not incorporate the extent of neurologic injury, and other authors focused on this aspect of the injury.52,53
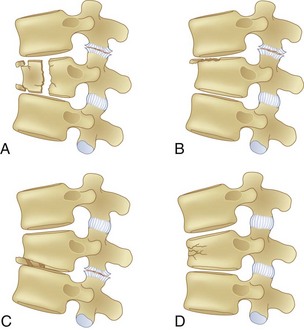
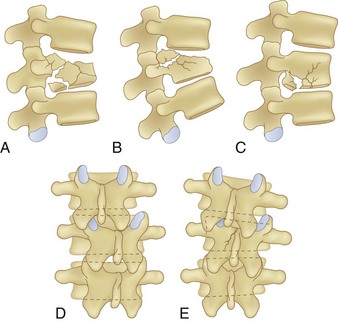
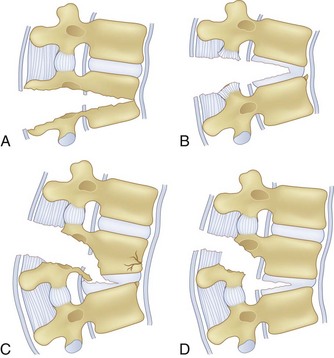
The application of CT to spine imaging marked a major change in the understanding of the various fracture patterns, and the modern classification systems evolved. Denis analyzed 412 thoracic and lumbar spine injuries with CT scans and classified major injuries as compression fractures, burst fractures, flexion-distraction injuries, and fracture-dislocations (Figs. 78-2 to 78-5). He proposed a three-column theory of spinal stability and delineated the concepts of mechanical instability and neurologic instability. In this scheme the anterior column is composed of the anterior longitudinal ligament (ALL), anterior annulus, and the anterior portion of the vertebral body. The middle column is composed of the posterior vertebral body, posterior annulus, and posterior longitudinal ligament. The posterior column is composed of the ligamentum flavum, neural arch, facet joints and facet capsules, and the posterior ligamentous complex. Mechanical instability begins to occur with failure of two of the three columns.54,55 The three-column theory was later validated with biomechanical cadaver studies.56 Injuries with a neurologic deficit were deemed by Denis to have neurologic instability. Neurologic instability was felt to be an important concept because injuries severe enough to cause neurologic injury are usually also mechanically unstable. Subsequent classification systems and current treatment algorithms are based on the perceived mechanical stability of the injured spine and the presence or absence of neurologic injury. Mechanical stability is a continuum, and great controversy exists in determining at what point a “stable” injury becomes “unstable.” This controversy is most evident with burst fractures.
McAfee described a classification based on analysis of the CT scan appearance of 100 fractures. Six basic injury patterns were proposed: wedge-compression, stable burst, unstable burst, Chance, flexion-distraction, and translational.57,58 Ferguson and Allen59,60 combined the three-column theory with the forces causing the injury and proposed a mechanistic classification. Fracture types included compressive flexion, distractive flexion, lateral flexion, translational, torsional flexion, vertical compression, distractive extension, and isolated transverse process fractures. The Arbeitsgemeinschaft für Osteosynthesefragen (AO) system was an attempt at comprehensively classifying spine injuries. Three main injury types were recognized: vertebral body compression, anterior and posterior element injury with distraction, and anterior and posterior element injury with rotation. Multiple subtypes exist within each group.61,62 Most recently, the Spine Trauma Study Group has integrated key concepts of these various classification systems to create a more simple and reproducible scheme. Neurologic status is included in the classification, with the goal of generating a more standardized thoracic and lumbar spine injury treatment approach. The Thoracolumbar Injury Classification and Severity Score (TLICS) is based on three categories: injury morphology, integrity of the posterior ligamentous complex, and neurologic status. Injuries are analyzed and point values assigned to subgroups within each category. More severe injuries receive higher injury scores, and therefore treatment theoretically may be guided by calculating the injury score.63–67
Description and Diagnosis of Specific Fracture Types
Sprains
Injuries to the spinal column involving the ligaments and musculotendinous units that do not cause facet joint subluxation, fracture, or listhesis are considered sprains and are stable.68 This tends to be a diagnosis of exclusion based on the history, physical examination, and imaging studies. With a reliable history, mild physical examination findings, and otherwise normal spine anatomy, plain radiographs may be sufficient to rule out spinal instability and diagnose a sprain. If there is a high-energy mechanism, unreliable history, significant physical examination findings such as obvious swelling or neurologic injury, or abnormal anatomy such as with ankylosing spondylitis or congenital anomaly, advanced imaging studies are warranted. CT and then MRI are often necessary under these circumstances to diagnose a sprain rather than a more significant injury.
Disc Herniations
Traumatic disc herniations caused by high-energy mechanisms are relatively rare as an isolated injury. Fractures are often associated with disc disruption, and the displaced disc material may contribute to neurologic injury, but the category of injury described here refers to an otherwise intact spinal column in association with a disc herniation that appears to be traumatic on the basis of the patient’s history, symptoms, and physical examination combined with correlating imaging studies. Disc herniations are commonly associated with minor trauma such as lifting an object, but the disk herniations considered here are due to high-energy trauma such as motor vehicle accidents that also caused or had the potential to cause other significant injuries. Diagnosis is made with MRI. There may be other imaging or clinical evidence of injury to the spinal column such as a soft tissue injury that would otherwise be called a sprain, but in order to be considered an isolated disc injury, there must not be any facet subluxation or traumatic listhesis. The classification scheme is anatomically descriptive and identical to that used in atraumatic disc herniations: bulging, protruded, extruded, or sequestered.69,70 It may be difficult to definitively establish a disc herniation as traumatic rather than preexisting because disc herniations are common in the asymptomatic population and it is a rare luxury to have available preinjury magnetic resonance images. From a clinical perspective it is not so important to establish a disc herniation as traumatic or preexisting because management of the disc herniation depends primarily on the presence or absence of neurologic symptoms (radicular pain), the physical examination findings (sensory and motor deficits), and the apparent temporal sequence in which these signs and symptoms developed. The spinal column itself is usually stable with isolated disc injuries.
Compression Fractures
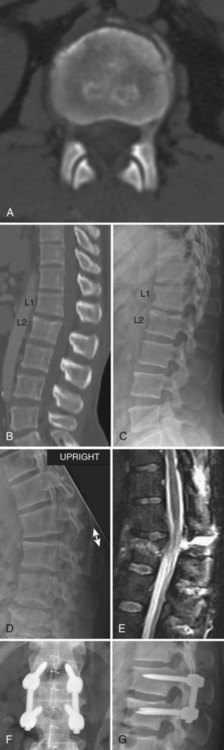
Compression fractures result from axial compression through the vertebral body, with failure through the anterior column. The fracture may involve the superior or inferior endplate alone, both endplates, or buckling of the anterior cortex with endplate preservation. The posterior column is usually not involved, but occasionally is. When this is the case, what appears to be a compression fracture may be a more significant flexion-distraction injury, described later as a “Chance” fracture (Fig. 78–6). The main distinguishing feature of the compression fracture is predominant failure of the anterior column in compression, whereas the flexion-distraction injury is characterized by predominant failure of the posterior column in tension.
Plain radiographs are usually diagnostic, but CT scans may be necessary to confirm the diagnosis because extension into the middle column may be subtle and burst fractures may be misdiagnosed as compression fractures 25% of the time on the basis of plain radiographs alone.36
Burst Fractures
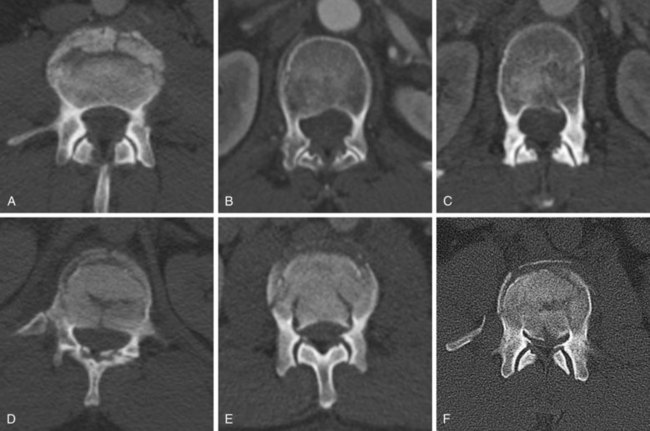
Burst fractures, like compression fractures, are caused by axial compression through the vertebral body. The fracture may involve the superior or inferior endplate alone, both endplates, or rarely with preservation of the endplates. Lateral compression forces may cause an injury variant that is asymmetrical in the coronal plane. The posterior column may or may not be involved, though more frequently it is involved when compared with compression fractures. In more severe injuries, the distinction between a burst fracture and a compression fracture is clear, with retropulsion of the fractured middle column fragments into the spinal canal being the hallmark of a burst fracture. But in less severe injuries, the distinction between compression and burst fractures is less clear and practically speaking may be in nomenclature alone, such as when the middle column fracture is minimally displaced and barely extends into the posterior cortex and there is minimal retropulsion of the middle column fragments (Fig. 78–7). The generally accepted differentiation between compression and burst fractures occurs at the middle column, which is spared in compression fractures and involved with burst fractures. Practically speaking, the transition from compression fracture to burst fracture represents a continuum of injury rather than distinct injury patterns because the same force vector is responsible.
Plain radiographs are often diagnostic, but CT scans are usually necessary to distinguish compression fractures from subtle burst fractures.36 For classification and descriptive purposes, if on CT scan the fracture extends into the posterior cortex of the vertebral body, regardless of the degree of displacement, it is referred to as a burst fracture.
Flexion-Distraction Injuries (Chance Fractures and Chance Variants)
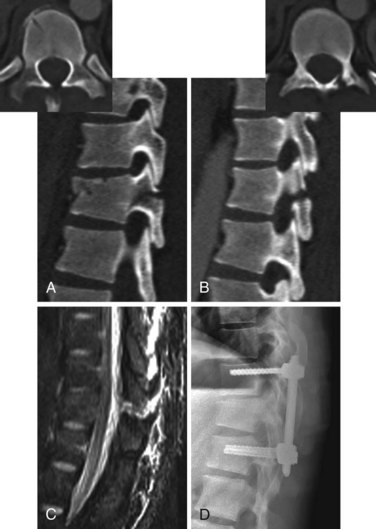
Flexion-distraction injuries are characterized by primary distractive forces on the spine, rather than crushing forces as seen with compression and burst fractures. These distractive forces cause tension failure of the posterior ligamentous complex and associated injuries to the anterior and middle column, either involving the disc or vertebral body. The axis of rotation is within or just in front of the anterior column, and at times the height of the anterior column can be relatively well maintained. The injury may be entirely osseous or entirely discoligamentous in nature or a combination of osseous and ligamentous (Fig. 78–8). Chance described the purely osseous lesion as a horizontal fracture extending through the spinous process, through the lamina and pedicles, and into the vertebral body.57 These injuries are commonly referred to as Chance fractures. Variants of this injury involve disc and ligamentous disruption with or without fracture. Anterior column disruption occurs through the disc space, not the vertebral body, and posterior column disruption is manifested as facet dislocation and ligamentous rupture, rather than fracture through the pedicle. These discoligamentous injuries are commonly referred to as Chance variants. If the axis of rotation is anterior to the spine, the vertebral body may be completely intact without fracture; if such an injury is severe, all the spine ligaments including the ALL may be disrupted, resulting in a severely unstable injury. If the axis of rotation is within the anterior column, there may be a vertebral body fracture with radiographic findings consistent with a compression or burst fracture, and if attention is not paid to the posterior elements and the distractive nature of the injury is not appreciated, underdiagnosis as a compression or burst fracture may occur.
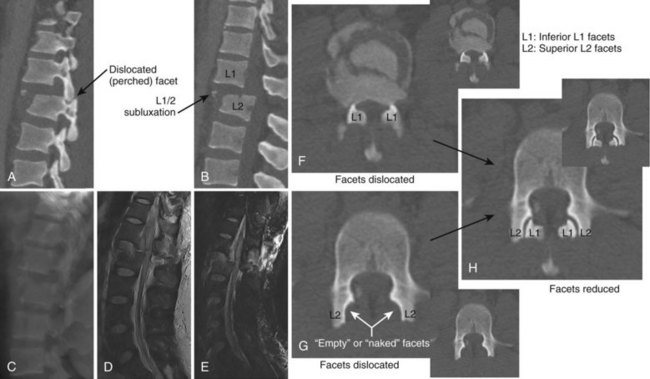
The diagnosis of a flexion-distraction injury may be made with plain radiographs, but CT is helpful in defining the precise anatomy of the osseous injury and identifies minimally displaced and nondisplaced injuries. Facet dislocations have a characteristic appearance on axial CT images, known as the “naked facet” or “empty facet” sign.71 This was first described in Chance variant injuries but is probably seen more commonly with fracture-dislocations.72 MRI is particularly good at detailing the extent of ligament and disc involvement with Chance fractures and Chance variants.
Fracture-Dislocations
Diagnosis can often be made on plain radiographs. The AP view may show lateral translation, whereas the lateral view may show anterior or posterior translation. CT scans will better quantify the bony injury and often demonstrate the “naked facet” or “empty facet” sign (Fig. 78–9).71,72 MRI should also be performed to assess the degree of disk and ligament injury and to visualize the neural elements.
< div class='tao-gold-member'>
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree