Review of Studies on the Validity of Upper Cervical Chiropractic Care
Kirk Eriksen
Learning Objectives
After studying this chapter, the reader should develop a better understanding of the literature related to the following issues of upper cervical chiropractic care:
Inter- and Intraexaminer Reliability of the orthogonally-based upper cervical X-ray analysis
Issues related to the Validity of upper cervical radiographic assessment
Functional pelvic distortion and postural imbalance
Outcome assessments used by upper cervical chiropractors
Practice-based studies related to upper cervical chiropractic care
Studies and case reports related to the efficacy of upper cervical care for patients with a variety of conditions
Chiropractic philosophy
This chapter presents the scientific and clinical rationale for upper cervical chiropractic care, making a compelling and cogent argument for it as a chiropractic specialty. The procedures involved have been around for more than 70 years, but they have not been fully appreciated or properly evaluated by either the chiropractic or medical professions at large. This specific care is supported by more than 100 peer-reviewed, indexed references, with several hundred more literature citations indirectly supporting various premises of upper cervical chiropractic care.1 The Work, as it is referred to, has an impressive track record for safety as well. The quantification of the Subluxation and its assessment enables the spinal Adjustments to be reproduced from one doctor to the next. Indeed, the nature of this care allows it to be fine-tuned to satisfy the individual needs of patients and usually results in fewer visits to achieve clinical goals.
This chapter reviews the role of upper cervical chiropractic care in improving spinal alignment and how this affects the patient’s quality of life. The scientific and clinical data show that upper cervical specific procedures are not only safe and effective, they are helping to provide new insights into our understanding of Health and well-being. These issues may bring about a paradigm shift in our understanding of many Health problems.
Radiographic Assessment
X-ray analysis for the assessment of spinal misalignment is the real core of upper cervical procedures. The X-ray assessment provides a quantitative analysis as opposed to only qualitative information. This makes it possible to determine if the care is actually reducing the misalignment component of the Subluxation, or if it is just moving the structures around with no net correction. Thus, quantification of the misalignment provides a means of evaluating the effectiveness of the Adjustment. By using this information, the goal is to compute a correction vector that will help reduce all of the misalignment factors proportionately. In essence, the procedure enables the doctor to provide a tailor-made Adjustment.
Measurement Reliability
It should be noted that the upper cervical X-ray analysis involves angular measurements of the atlas in the frontal (Z), sagittal (X), and transverse (Y) planes. Angular measurements in degrees are used, as this analysis is less prone to radiographic magnification errors in comparison with Linear measurements. Inter- and Intraexaminer Reliability for reading orthogonally based upper cervical X-rays has revealed errors of only
<0.6° and <0.5° (1 standard deviation [SD]), respectively,2,3,4 with the exception of one study.5 The Sigler and Howe5 study demonstrated 41% to 71% Interexaminer errors; however, the protocol of the study suffered from design flaws that make the results of limited value.6,7 Studies have been published since this paper that have refuted the results. However, application of the study’s data from a clinical standpoint reveals intriguing information.7 Based on the study’s data, the following results were gleaned:
<0.6° and <0.5° (1 standard deviation [SD]), respectively,2,3,4 with the exception of one study.5 The Sigler and Howe5 study demonstrated 41% to 71% Interexaminer errors; however, the protocol of the study suffered from design flaws that make the results of limited value.6,7 Studies have been published since this paper that have refuted the results. However, application of the study’s data from a clinical standpoint reveals intriguing information.7 Based on the study’s data, the following results were gleaned:
92% of the comparisons were in agreement on the side of Atlas laterality
80% of the comparisons would have had no change in the Adjustment vector
16% would have a change of ¼ inch in the Height factor
2% would have a change of ½ inch in the Height factor
2% would have a change of ¾ inch in the Height factor
Of the 60 comparisons, only 3% should have been adjusted on the opposite side of the probable Atlas laterality
Another study1 involved three doctors from each of three upper cervical techniques (Orthospinology, atlas orthogonality, and National Upper Cervical Chiropractic Association [NUCCA]) to determine the Interexaminer Reliability of radiographic analysis. Five sets of X-rays were coded, labels masked, and mailed to the nine experienced practitioners of each technique. Each doctor constructed central skull (CS) and atlas plane (AP) lines on each of the nasium X-rays. The inclination of the CS and AP lines were measured in degrees from the vertical and horizontal planes, respectively. The acute angle between these two lines was measured and recorded as Atlas laterality. Dr. Ed Owens presented the results at the spring and fall 1995 Academy of Upper Cervical Chiropractic Organizations (AUCCO) joint meetings. The results showed that the mean error in Atlas laterality was 0.47° with an intraclass correlation coefficient (ICC) of 0.910. The mean error of the CS line inclination was 0.44° with a 0.933 ICC, and mean error of the AP line slope was 0.34° with a 0.847 ICC. The high ICC values (>0.8) indicate very good Reliability between readings. Results from this study found that no particular technique had more Reliability, nor did any method consistently over- or underestimate the measurements.
Grostic and Marshall8 tested the accuracy of the upper cervical X-ray analysis with the use of a model consisting of a dry skull with a movable atlas vertebra mounted underneath that could be set to a known degree of misalignment. The model was X-rayed, and the analysis of the film revealed very good agreement between actual and measured values. Owens9 reviewed chiropractic X-ray analysis techniques used to assess the cervical spine. He concluded that studies show inter- and Intraexaminer Reliability that is sufficient to measure lateral and rotational displacements of the atlas to within plus or minus 1°. A 1998 literature review determined that X-ray line drawing for the analysis of spinal displacement was found to have high Reliability with a majority of ICC in the range of 0.8 to 0.9.10 As a comparison, the Reliability for determining pathology on radiographs was found to be only fair to good by both medical doctors and chiropractors and by both chiropractic and medical radiologists. The majority of ICCs for these evaluations were found in the range of 0.4 to 0.75.10
Potential Sources of Error Affecting X-Ray Analysis Validity
Rochester and Owens11 have studied the issue of patient placement and the potential distortion errors that can take place in the measurement of upper cervical X-rays. Patient-to-film error can occur if head rotation is present when the film is taken. However, this study concluded that the distortion is insignificant in most all cases seen in clinical practice as long as Image rotation does not exceed 1.5° on the nasium film. Other potential errors include human measurement that can occur when the doctor draws lines on the X-rays and measures the deviations. This potential error has been greatly decreased with the development of Computer-aided digitization programs.12 The previous Reliability study by Rochester3 tested the DOC (digitizing radiographic analysis for the Orthospinology practitioner within chiropractic) program and revealed that it was as good as, if not superior to, manual analysis. The Orthospinology analysis has been programmed into the latest computer-assisted radiography technology available for doctors in the field (see Chapter 2). This technology should help to build on the accuracy of the radiographic analysis that has been previously demonstrated.
Studies have revealed that radiographic measurement of misalignments between the occiput and atlas is not significantly affected (from a clinical standpoint) when the head is placed, up to a certain degree, in off-centered positions.13,14,15 However, this does not indicate that X-ray placement is not important, as it can cause errors in other measurement parameters (i.e., Atlas plane line, Lower angle, axis spinous process). A study by Jackson et al.16 involved 38 subjects who had two sets of nasium and lateral cervical radiographs. The second set of X-rays was taken from one-half to 4 hours after the initial set. No chiropractic Adjustment was administered between radiographs,
although a simulated Adjustment was conducted. The data revealed Reliability measurements of ½° for the upper angle and 2/3° for the Lower angle. These numbers are similar to those found in Interexaminer Reliability studies related to the measurement system; thus, this study demonstrates the stability of upper cervical misalignments.
although a simulated Adjustment was conducted. The data revealed Reliability measurements of ½° for the upper angle and 2/3° for the Lower angle. These numbers are similar to those found in Interexaminer Reliability studies related to the measurement system; thus, this study demonstrates the stability of upper cervical misalignments.
Harrison17 reviewed the initial and follow-up radiographic data for six control groups from separate studies using Chiropractic Biophysics protocol. The data from these studies found that only two radiographic measurements out of 50 angles and distances showed a statistically significant difference between initial and follow-up evaluations of patients not receiving spinal Adjustments. It was concluded that posture is stable over time, X-ray positioning is repeatable, and the radiographic line drawing methods were reliable. One non–peer reviewed study has shown that barring trauma, an upper cervical misalignment pattern tends to be static.18 However, the magnitude of the misalignment tends to decrease over time when the patient becomes subluxated.19 Hart20 observed a similar finding, although the radiographic analysis involved lateral and anterior to posterior (AP) open-mouth views. The clinical and published evidence indicates that the upper cervical spine does not move around freely finding a new position each time the patient is X-rayed, and these misalignments measured on specific radiographs are somewhat static. The preliminary data suggests that the reduction of the misalignment postAdjustment is due to something other than patient X-ray placement if strict protocols are performed.
Post–X-Ray Assessment
Grostic and DeBoer21 published a study concerning pre- and post-X-rays of 523 cases from the files of John F. Grostic, D.C. They found a mean atlanto-occipital misalignment of 2.63° and 2.75°, respectively. The postfilm analyses were obtained after the first Grostic Adjustment and showed corresponding values of 1.40° and 1.43°, which is a statistically significant change. Spencer22 conducted a study to investigate to what extent bias might be responsible for the measured correction of atlanto-occipital misalignment using the Grostic X-ray analysis for Atlas laterality. Doctors were blinded as to whether the radiographs were either pre- or postAdjustment X-rays, and they made 45 analysis comparisons. The findings suggest bias to be minimally responsible for the corrections measured on postfilm (Fig. 21-1).
One large retrospective study23 (N = 458) found that the more the Subluxation was reduced, the better the patient outcome. This was determined by measuring patient rating of symptoms, as well as number of visits and necessary Adjustments. This study concluded that post–X-ray assessment was recommended to ascertain that at least a 50% correction was achieved after the initial Adjustment. However, the conclusion of the study could have been strengthened if post–X-rays had been taken at the end of the first month of care or at maximum improvement. As a result, a multisite study has been designed and is being submitted for institutional review board approval to address this issue.24 This study will evaluate patient outcomes and post–X-ray reductions that will be measured in a blinded fashion.
Rochester25 investigated the Validity of using Orthospinology procedures as an intervention in the management of spine-related pain by assessing the impact on patient outcome measures. Consecutive patient files from a private chiropractic practice over a 1-year period were reviewed for inclusion. Care was provided to 104 patients for an average of 2 weeks and six office visits. Radiographic procedures and the Supine leg check were used according to the Orthospinology procedure as mediating variables for when and how to make an Adjustment. Cervical paraspinal Palpation was also used, but this information was not included in the study. The Visual Analog Scale (VAS), the modified Neck Disability Index (NDI), and modified Oswestry Disability Index (ODI) questionnaires were used as outcome measurements.
Statistically significant improvements in neck pain VAS (66%), NDI (55%), back pain VAS (65%), and ODI (61%) after approximately 2 weeks of chiropractic care were observed. The data revealed that an average of 34% reduction of cervical alignment was necessary before a statistically and clinically significant improvement was detected for both NDI and neck pain VAS. This was compared with a conservative group representing the natural history of neck pain. Patients who “held” their Adjustments better demonstrated improved outcomes, verifying that the improvement of functional Leg length inequality (LLI) is a valid clinical goal. This study may shed some light on the concurrent and predictive Validity for the Supine leg check and Orthospinology radiographic procedures.
Chung-Ha Suh, Ph.D., a professor from the University of Colorado, has led several research projects in the past for the chiropractic profession. He was instrumental in obtaining the first federal grant for chiropractic research ($250,000) from the National Institutes of Health in the mid-1970s. He had a keen interest in upper cervical research and was a personal friend of Dr. John D. Grostic. Two of his main contributions have been the development of a computer kinematic model of the spine and the study of three-dimensional, distortion-free radiographic analysis. Unfortunately, because of lack of funding and other issues, the distortion-free radiographic analysis project was never completed. However, preliminary data showed conclusively
that structural change had taken place after upper cervical Adjustments.26,27
that structural change had taken place after upper cervical Adjustments.26,27
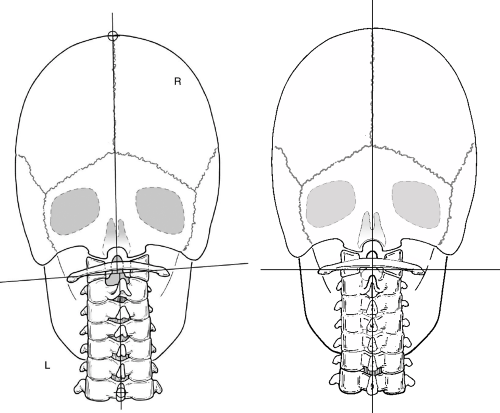 FIGURE 21-1 Subluxated cervical spine (L) and its correction to an Orthogonal alignment (R) as viewed on pre and post nasium X-rays. |
A single reported case revealed a patient’s upper cervical Subluxation being reduced significantly after a NUCCA upper cervical Adjustment.28 The patient was then sent to a practitioner who used diversified/Maitland Manipulation. When the patient returned to the NUCCA doctor, X-rays were once again taken, revealing that the misalignments had increased more than the original Subluxation. The patient was readjusted by the NUCCA doctor, and the Subluxation was reduced once again. Indeed, if improved cervical alignment is a clinical goal, then postradiographic assessment is necessary to determine the degree of correction or if an increase in misalignment factors has occurred.
A series of case studies has been published that reviewed significant errors in adjusting vectors that occurred in an upper cervical practice for various reasons.29 The upper cervical technique appeared to cause temporary iatrogenic symptomatic reactions in the unsuspecting patients, which included headache, dizziness, and pain in the neck, low back, leg, and foot. Once the errors were discovered and the Adjustment was modified, the symptoms were reversed. This phenomenon is an important finding as some believe that the specific upper cervical Adjustment is innocuous and ineffective because the patient feels very little force during the procedure. This type of Adjustment is too gentle to “injure” the patient, but osseous structures are realigned, and the central nervous system is affected in the process. The “seasoned” doctor understands that the most significant negative outcome lies in not correcting the Subluxation, which prevents the patient from experiencing optimum neurological integrity. As Knutson states:
Manipulations of the upper cervical spine are likely to cause only partial corrections in some percentage of patients. A partial correction could leave remnants of postural distortions that result in repetitive treatment, and/or could cause iatrogenic symptoms that are acute—headache, dizziness, etc.—and/or chronic—postural problems that later become symptomatic expressive.29
Various authors have criticized the use of radiography for biomechanical analysis of the spine.30,31,32 However, Harger et al.33 have revealed that 51% of chiropractors routinely take X-rays for biomechanical and postural assessment. It was also found that 63% of doctors of chiropractic used radiographic line drawing to
locate vertebral Subluxations. This type of patient evaluation is taught in most chiropractic colleges and by many mainstream chiropractic techniques. X-ray analysis for the purpose of characterizing vertebral Subluxations is within the standard of care of the chiropractic profession and is further supported by the International Chiropractors Association34 and Council on Chiropractic Practice35 clinical practice guidelines. A 2005 paper published in Clinical Chiropractic36 highlighted the importance of taking X-rays, from a safety standpoint, before administering care for patients with little to no cervical spine symptoms. The paper also makes a compelling and cogent case for the clinical and scientific rationale for taking cervical X-rays for the purpose of biomechanical assessment.
locate vertebral Subluxations. This type of patient evaluation is taught in most chiropractic colleges and by many mainstream chiropractic techniques. X-ray analysis for the purpose of characterizing vertebral Subluxations is within the standard of care of the chiropractic profession and is further supported by the International Chiropractors Association34 and Council on Chiropractic Practice35 clinical practice guidelines. A 2005 paper published in Clinical Chiropractic36 highlighted the importance of taking X-rays, from a safety standpoint, before administering care for patients with little to no cervical spine symptoms. The paper also makes a compelling and cogent case for the clinical and scientific rationale for taking cervical X-rays for the purpose of biomechanical assessment.
The two upper cervical vertebrae differ in shape and function from the remainder of the spine. The configuration of the atlantal and axial joints enables these structures to carry the head and determine its movement. These Articulations also provide protection for the intimate neurologic and vascular structures. The upper cervical spine is complex in both its motion and neurophysiological connections. The motion of the upper cervical spine is more complicated than the rest of the spine as it is capable of movement into the X, Y, and Z planes. It is vital that the doctor evaluate the patient’s cervical spine as thoroughly as possible. The chiropractor must provide care that has a high degree of probability for a successful outcome while reducing the possibility of iatrogenesis (see Chapter 10).
Palpation and other methods of determining upper cervical misalignments and asymmetry have not been shown to be reliable,37,38,39,40 nor has the static Palpation of the atlas transverse process.39 There is some evidence that nonradiographic methods of determining upper cervical misalignments have shown poor concordance compared with X-ray–determined misalignment.38,41 The radiographic procedure helps provide the information for the appropriate direction or vector to adjust the patient. These reasons, taken together, explain why upper cervical protocol calls for radiographic assessment of misalignment factors in an occipito-atlanto-axial Subluxation. Alternatives are so unreliable that they amount to guessing, which leads to borderline effectiveness at best and iatrogenesis at worst. Upper cervical radiographic assessment is necessary for a number of reasons that are in the best interest of the patient.
Postural Distortion
Upper cervical Subluxations manifest clinically in various forms of postural distortion, such as functional LLI, head and shoulder tilt, head translation, and unequal weight distribution (Fig. 21-2). The Supine leg check is an outcome assessment used by most all upper cervical doctors on a visit-by-visit basis. The physiological “short leg” is not necessarily anatomically short at all, but only appears so in non-weight-bearing leg checks. Functional pelvic distortion (FPD) is an accurate descriptor for what the doctor is actually measuring, which is muscle tone imbalance and resultant pelvic distortion, as opposed to LLI. Data have been published showing impressive ICC for inter- (>0.9) and Intraexaminer (>0.7) Reliability for the Supine leg check.42 The doctors were able to reliably measure the recumbent LLI to within ¼ inch in 80% of cases and within 1/8 inch in 60% of the trials. Moderate Reliability has been assessed for the prone leg check.43,44,45 Pilot studies on pre- and post-FPD assessment after an upper cervical Adjustment have been conducted46,47,48 with larger Validity studies planned for the future.49
Supine Leg Check
Knutson50 evaluated the Validity of the Supine leg check against a “bronze standard” of back pain in the general population. The study found 51% of people in a nonclinical population had a functional short leg in the supine position. A moderate association with recurrent back pain and a significantly increased pain intensity (VAS) related to the back (p<0.001) was found in these patients. The incidence of functional LLI in this population increased as the subjects reported more back pain for longer periods, with 85% of those with chronic back pain having FPD. Supine LLI was found to be valid ≥70% when correlated to recurrent back pain for sensitivity, specificity, and positive predictive value, and just <69% for negative predictive value (p<0.001). This study concluded that the Supine leg check had clinical Validity as a stand-alone test for recurring back pain. Another study examined a group of volunteers from the general population who were not currently under treatment for back pain.51 These subjects were found to have a significant relationship between the presence of the supine LLI and a decreased rating of general Health as determined by the SF-12 questionnaire.
Knutson and Owens52 studied volunteers who were placed in groups based on whether they displayed evidence of supine LLI or they appeared to be balanced. The Biering-Sorensen test determined that patients with supine LLI had a decreased amount of erector spinae muscle endurance compared with their balanced counterparts. The Biering-Sorensen test provides reliable measures of position-holding time (back muscle endurance) and has been shown to discriminate between subjects with and without nonspecific low-back pain (LBP).53 The quadratus lumborum (QL) endurance
tests showed that the QL muscle ipsilateral to the supine LLI had significantly decreased endurance times over the same-side QL fatigue times in the no-LLI group.
tests showed that the QL muscle ipsilateral to the supine LLI had significantly decreased endurance times over the same-side QL fatigue times in the no-LLI group.
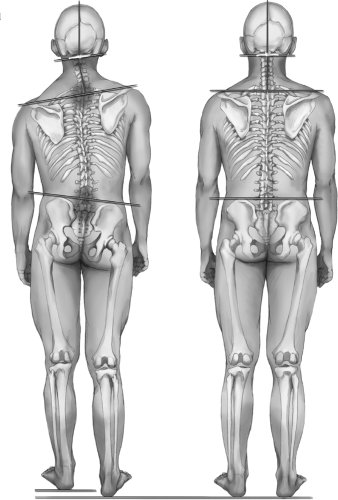 FIGURE 21-2 Upper cervical Subluxation and its correction, and its proposed impact on spinal and pelvic distortion. |
A blinded single case study demonstrated a statistically significant correlation between an objective thermographic evaluation and FPD evaluation when an upper cervical Adjustment was indicated.54 Knutson reported a case study involving occipitoatlantal intra-articular injections that moderated postural distortion.55 Another study also revealed postural changes occurring in subjects after undergoing upper cervical care.56 Two studies have shown statistically significant changes in right and left weight-bearing pre- and post-upper cervical Adjustment.57,58 The Seemann study57 involved 93 subjects who were found to have an average imbalance of 12.84 pounds before receiving care. After receiving one NUCCA upper cervical Adjustment, bilateral weight measurements showed an average imbalance of only 3.67 pounds. These studies imply, but do not prove, a causal link between postural distortion changes and upper cervical chiropractic care. The assessment of postural imbalances is an important outcome that has historically been used by upper cervical doctors. Chapter 9 reviews the stability of posture and the Reliability of its assessment. Structure dictates function, just as posture plays a significant role in the overall Health of the individual. Lennon et al. state:
Observations of the striking influence of postural mechanics on function and symptomatology have led to our Hypothesis that posture affects and moderates every physiologic function from breathing to hormonal production.59
Outcome Assessments
The purpose of outcome assessments can range from determining when an appropriate chiropractic Adjustment has been achieved to evaluating the patient’s response to care. Outcome assessments that have been studied in clinical and research settings with specific upper cervical chiropractic care include the following: Thermocouple scanning,60,61,62,63 surface electromyography (sEMG),46,47,64 static Palpation,65,66,67 somatosensory evoked potentials (SSEP),68,69,70,71,72,73 range of motion,74,75,76 and even bone densitometry.77
Collins and Pfleger70 conducted SSEP evaluations on a group of patients, which revealed neurological insult in 93% of the subjects. Eighty-five percent of the patients with documented deficits of the sensory nervous system pathways were shown to have significantly improved SSEP waveforms in both the brachial and lumbosacral plexuses after receiving Grostic upper cervical Adjustments. These changes in waveforms were consistent with improvement or elimination of various subjective symptoms. This technology assesses the nervous system directly compared with other typical outcome assessments (i.e., thermometry, sEMG, leg check). However, SSEP is typically cost prohibitive in its use for clinical practice.
Practice-Based Research
Practice-based research (PBR) is a type of cohort study that reflects the “real-life” care provided in private practice. The PBR attempts to answer the bottom-line question: “Is the care effective?” One investigation set out to assess changes in general Health status with the use of the SF-36 questionnaire and global well-being numerical scale after a course of upper cervical chiropractic care.78,79,80 The patients presented primarily with musculoskeletal symptoms; however, statistically significant improvement was seen for all SF-36 subscales at 4 weeks and at the point of maximum chiropractic improvement (MCI). The global well-being numerical scores demonstrated improvement as well. X-ray analysis found an average of 51% to 75% improvement in relative upper cervical alignment.
However, no control group was used in the design of this study, and fewer than one-third of the patients were tracked to MCI, so the conclusions drawn are somewhat limited. The majority of patients in this study had chronic symptoms lasting more than 8 weeks. The data indicated that there was no relationship between gains made on SF-36 general Health scores and the duration of symptom. Because acute as well as chronic Health symptoms showed similar outcomes under upper cervical care, the data suggested that the natural course of the condition is probably not responsible for the overall gains in Health seen in the study. Analysis of initial SF-36 scores showed a statistically significant difference in only the physical functioning scale between patients for whom completed data was available versus those with incomplete files. As a result, severity of the initial symptom did not seem to be related to compliance in the study.80
A pilot study used the SF-36 survey to assess patient outcome and correlation with the X-ray analysis between three upper cervical techniques (Grostic, Blair, and toggle).81 Atlas laterality was measured on the Nasium view (Grostic), protractoview (Blair), and the AP open-mouth view (toggle). Poor agreement was found between Grostic and Blair analysis (56%, Kappa = 0.08), and poor agreement was found between Grostic and toggle analysis of Atlas laterality (56%, Kappa = 0.10). The study also involved 20 subjects (10 Grostic and 10 Blair) undergoing 1 month of upper cervical care. It was found that patients under Grostic care had a significant improvement in physical functioning on the SF-36 subscale, whereas patients receiving Blair Adjustments had a significant improvement in role emotional and mental Health subscales. Dickholtz has conducted a PBR study on his own NUCCA practice with promising results.82
Studies on Patient Efficacy
Chiropractic care is not the treatment of disease or conditions, although whole-body effects have been noted since chiropractic’s inception in 1895. However, ill Health has multicausal contributions and not every occurrence will respond to spinal Adjustments. This section will present studies that appear to show, from a clinical standpoint, a relationship between the patient’s Health symptom and the correction/reduction of the upper cervical Subluxation. The studies will range from various musculoskeletal symptoms to conditions affecting almost every organ system of the human body. The case studies involve doctors reporting their own observations made while providing upper cervical care. It is acknowledged that this does not provide proof of a causal link between the spinal Adjustments and the patient results. It is incumbent upon the profession to continue to conduct more rigorous studies of the effects of chiropractic care. However, more than 110 years of clinical data and the growing amount of research evidence makes a compelling case for the role of chiropractic in the Health care arena.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








