80
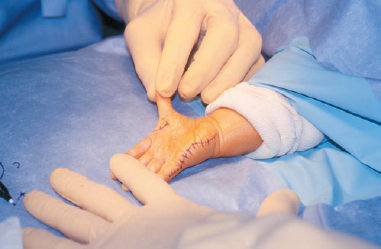
Reconstruction of a Type II Hypoplastic Thumb
Allan E. Peljovich and Peter M. Waters
History and Clinical Presentation
An 11-month-old boy was brought in by his parents for evaluation of his right thumb. At birth, he was noted to have a tethered cord, an imperforate anus, and a small thumb. He had previously undergone surgery on his spinal cord and has had the initial stages of surgery to reconstruct his anus and rectum. He has been referred for possible reconstructive surgery of his hand.
Physical Examination
There was mild radial deviation of the carpus of the right arm. The length of the thumb was to the level of the index proximal interphalangeal (PIP) joint. The thumb was adducted, and the patient had a narrowed thenar web space. He had intact flexor pollicis longus (FPL), extensor pollicis longus (EPL), and flexor pollicis brevis (FPB) motion and function. He had noticeable flattening of his thenar eminence, and did not oppose the thumb in play activity. He had complete ulnar collateral ligament instability at the metacarpophalangeal (MP) joint at both 0 and 30 degrees of MP flexion, and passively abducted his thumb through the unstable MP joint, and not through the web space. The carpometacarpal (CMC) joint was stable. He did use the thumb in play and grasp activity, and, in fact, pinched objects between his index and long fingers.
Diagnostic Studies
On radiographs, there appears to be mild ulnar positive variance (Fig. 80–1). The thumb ray is made of a metacarpal and two phalanges, albeit hypoplastic. The carpal ossification is normal for age, with the hamate and capitate ossified.
PEARLS
- Careful assessment of the patient and his or her hand is critical to a good outcome.
- When possible, surgery should be performed before the age of 18 months and ideally at 9 to 12 months of age.
PITFALLS
- Surgeon must be aware of the anatomic variability that can exist, and be flexible in his or her preoperative planning, and intraoperative decision making.
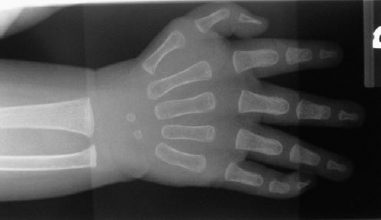
Figure 80–1 Anteroposterior (AP) radiograph of the patient’s hand. There is mild ulnar positive variance, which is suggestive of type I radial dysplasia. The ossified capitate and hamate are consistent with the child’s age; it is too early for ossification of the scaphoid or trapezium. The thumb ray is short.
Differential Diagnosis
Normal variant
Trigger thumb
Severe carpal tunnel syndrome
Any of the variants of hypoplastic thumb per the modified Blauth classification
Diagnosis
Hypoplastic Thumb (Type II) with Probable Type I Radial Dysplasia
Our case illustrates the principles involved in reconstructing most type II and IIIA hypoplastic thumbs. It is important to realize that the spectrum of deficiencies can range from simple shortening of the thumb ray to its complete absence. The choices for treatment include no treatment, surgical reconstruction, amputation, index pollicization, free tissue transfer, and any combination of the former. In 1981, Buck-Gramco expanded upon Blauth’s previous classification system that is helpful in understanding this spectrum and in choosing operative treatment. In 1995, Manske further divided type III hypoplastic thumbs into two variants based on the integrity of the CMC joint. Type IIIA thumbs have an intact and stable CMC joint, whereas type IIIB thumbs do not. The main difference for treatment is that some believe that the lack of a CMC joint precludes any successful attempt at reconstruction, and these thumbs therefore should be amputated. This classification system is illustrated in Table 80–1. Type I hypoplasia is often treated with observation only. Types II and IIIA hypoplastic thumbs are two common variants amenable to surgical reconstruction. Types IIIB and IV are usually treated by amputation and index pollicization. Type V is treated by index pollicization, provided there is a sufficient index finger present. Although our case illustration is that of a patient with type II hypoplasia, the principles involved in assessment and treatment apply to all hypoplastic thumbs.
When examining an infant or child, it is important to take account of the child’s health, as well as to examine the entire extremity. Associated syndromes include VATER (vertebral defects, imperforate anus, tracheoesophageal fistula, and radial and renal dysplasia), Holt-Oram, and Fanconi’s anemia. In 1996, James et al surveyed a large group of patients with hypoplastic thumbs. They found radial dysplasia in 59%, and associated syndromes in 43% of the patients.
| Type | Findings (Additive with Increasing Severity) |
| I | Thumb size diminished. Possible hypoplasia of median innervated thenar intrinsics. |
| II | Deficient/absent median innervated intrinsics. Adduction contracture/web space contracture. Ulnar collateral instability of metacarpophalangeal (MP) joint. |
| III | Deficient/absent ulnar innervated intrinsics. Ulnar and possible radial collateral instability of MP joint. Abnormalities/absence of thenar extrinsics. |
| IIIA | CMC is stable. |
| IIIB | CMC is unstable/proximal phalanx may be absent or deficient. |
| IV | Pouce flottant. No bony support to the present phalanges; only a neurovascular pedicle attaches thumb to hand. Thumb ray carpals deficient/absent. |
| V | Thumb aplasia. |
After a thorough examination is completed, surgical planning becomes more straightforward. The fundamental goal is to create a thumb that is mobile and opposable, and hence more useful. This requires a thumb that is stable, mobile, and strong, and with a wide-enough thenar web space and length to allow for grasp. The specific deficiencies that are present in any one patient determine the course of reconstruction. Our patient had a small thumb with an unstable ulnar collateral ligament, absent median innervated intrinsic muscles, and a narrow web space. Our reconstruction, therefore, served to address these deficiencies. Although the length of the thumb was not specifically addressed, we have often found that the web space widening/deepening results in a functionally longer thumb, thereby precluding the need to lengthen the thumb (see Fig. 80–5). One important consideration is the timing of surgery. Patients occasionally do not present until they are older, but typically present during infancy. We believe that when surgical intervention is appropriate, it is best done during infancy. The amount of cerebrocortical representation of the thumb in patients with hypoplasia is diminished, and we feel, as do others, that early intervention takes advantage of the plasticity of the infant’s central nervous system.
Surgical Management
Surgical Plan
- Restore stability to the MP joint of the thumb to provide a stable post for opposition/grasp through reconstruction of the deficient ulnar collateral ligament (UCL).
- Widen the thumb web space to improve grasping ability through the use of local flaps.
- Provide a thumb opposition force for function through a Huber [abductor digiti quinti manus (ADQM) to abductor pollicis brevis (APB)] transfer.
We initiate the procedure by dissecting the ADQM. Our landmarks for the incision are the pisiform proximally and the ulnar border of the little finger PIP joint distally. The incision curves ulnarly proximal to distal by the time it reaches the level of the MP joint of the little finger (Fig. 80–2). It is important to keep in mind that the proper digital nerve and vessel to the ulnar border of the little finger traverse the fascia of the hypothenar eminence. As such, it is important to penetrate the skin only, and then proceed with careful dissection to identify the muscle and the neurovascular bundle. The dissection of the ADQM, once identified, proceeds initially on the ulnar border to identify the entire ulnar aspect of the muscle from the level of the pisiform to its insertion at the level of the PIP joint. A fascial plane is evident ulnarly/dorsally separating the muscle belly from that of the opponens digiti minimi. A dorsal sensory nerve branch is evident and protected during this portion of the dissection in the distal half of the wound. The dissection then proceeds radially to outline the entire muscle. Careful dissection is required proximally for several reasons. First, the neurovascular pedicle to the ADQM exits Guyon’s canal at the radial border of the pisiform along with the remainder of the ulnar nerve and artery. The pisiform also serves as an origin of the ADQM. It is imperative to identify this pedicle at the exit point of Guyon’s canal, but not dissect it to avoid injury. Mobilization of the muscle does not require mobilization of the neurovascular pedicle. Second, the border between the ADQM and the flexor digiti minimi may not be easily distinguishable. In that circumstance, it is better to err on the side of taking a portion of the flexor as one secures control of the ADQM. Attention is then turned distally to the ADQM insertion. The insertion is not always clearly distinct. The lateral band on the ulnar side, which represents the insertion of the ADQM, is identified (Fig. 80–3). In our case, we did not identify a separate insertion into the proximal phalanx as has been described. The lateral band and tendon of the ADQM are then freed distally, gaining as much length as possible. The tendon is freed from its insertion subperiosteally, but not so aggressively as to release the UCL of the MP joint. One should now be able to mobilize the entire ADQM with the pisiform serving as the point of rotation. It is important to inspect the undersurface of the ADQM at the level of the pisiform to identify and protect the neurovascular bundle to the ADQM. Do not dissect the ADQM off the pisiform because this threatens the neurovascular pedicle. A grasping suture is then applied to the tendon edge.