Preoperative Planning and Templating for Revision Hip Arthroplasty
Jay Patel and Kevin Bozic
Key Points
Introduction
Revision total hip arthroplasty (THA) is a complex procedure associated with inferior patient outcomes, higher rates of complications, and greater hospital resource utilization compared with primary THA.1–4 Furthermore, the number of revision THA procedures is expected to increase in proportion to the substantial increase in primary THA procedures.5 Much effort has historically been placed on improving implant design, materials, and surgical techniques to improve outcomes of revision surgery. Although these efforts have generated many benefits, preoperative planning is an imperative, but often overlooked, step in anticipating the added challenges of revision surgery and minimizing complications. The process of preoperative planning for revision THA surgery is not algorithmic but includes three consistent steps.
First, the surgeon must diagnose the specific mode and cause of failure. Patient complaints can often be vague, and a thorough history, physical examination, and diagnostic evaluation are required to determine why revision surgery is indicated. Second, the surgeon must identify the goals of surgery. This entails identifying the technical goals of surgery, such as improving abductor tension or improving alignment of the acetabulum, and determining the patient-oriented goals of surgery, such as reducing hip pain or preventing hip dislocation. The patient must actively contribute to the goals of surgery and be made aware of the risks of surgery. Third, the surgeon must create a surgical plan that involves templating, anticipating alternative surgical methods, and ensuring that all necessary implants, instruments, and bone grafts are readily available on the day of surgery. The entire preoperative planning process is critical to the success of the surgery.
Preoperative Diagnosis
The preoperative planning process begins during the patient’s first office visit. The surgeon should listen carefully to the patient’s complaint and begin to establish the surgeon-patient relationship. The history and physical examination should be thorough and should include significant detail about the hip, as well as general medical conditions. Hospital records, previous radiographs, and all previous operative reports, with implant labels, should be brought to the visit.
Patients often present with reports of pain or instability of the hip (Fig. 86-1). The pain should be defined in terms of its quality, severity, onset, progression, and location, as well as alleviating and exacerbating factors. The type of pain can be suggestive of a diagnosis. Aseptic loosening commonly presents with pain, which is worse with activity and is improved with rest. Pain in the groin or the gluteal region can be suggestive of a loose acetabular component, whereas pain in the thigh is suggestive of problems of the femoral component.6,7 Groin pain occasionally can be due to hernias, lymphadenopathy, psoas abscess, or various gynecologic or genitourinary causes.6–8 Start-up pain or pain with walking a few steps is also a hallmark of a loose femoral component.6,7 If the patient had a pain-free interval after surgery, existing pain may be due to late infection, aseptic loosening, stress fracture, or osteolysis.6,7,9 Persistent pain after surgery without a pain-free interval is suggestive of early infection, failure to obtain initial implant stability, periprosthetic fracture, or misdiagnosis of the original problem.6,7,9 Constant pain, pain at rest, or night pain may be due to infection or malignancy.9 Pain associated with a decreased range of motion (ROM) is a sign of infection, heterotopic ossification, subsidence, or acetabular protrusio. Acute pain is associated with hip dislocation and periprosthetic fracture. Patients with lumbar spine disease may be more active after hip arthroplasty, causing exacerbation of their neurogenic claudication.10
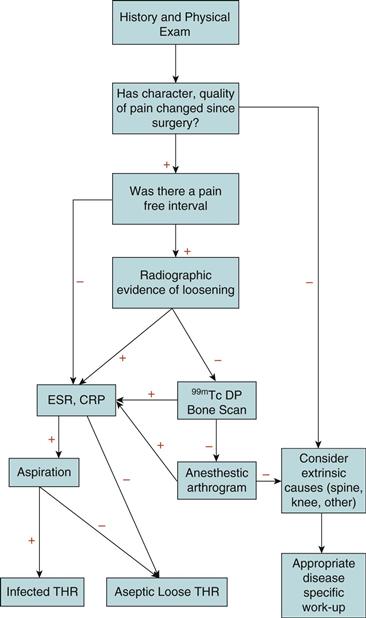
Figure 86-1 Algorithm to evaluate painful total hip arthroplasty (THA).
Thigh pain, although sometimes associated with a loose femoral component, is more commonly associated with well-fixed porous ingrowth or press-fit femoral components. Persistent thigh pain with no radiographic evidence of loosening has been described in 12% to 41% of patients with cementless implants,11,12 although with modern implants and techniques, it is probably less common now. Some patients with persistent thigh pain have also been found to have well-fixed femoral components at the time of surgery.13,14 Femoral component revision can be indicated for continued thigh pain despite well-fixed components. Tip of stem pain may be caused by modulus mismatch between a stiff cementless femoral stem and the less stiff surrounding bone.9
Hip instability is another common chief complaint. For these patients, a history of dislocation, including the number of dislocations, the timing of dislocation relative to the date of surgery, the position of the leg at the time of dislocation, the surgical approach used for the index procedure, and the method of reduction of the hip should be elicited. For patients who have symptoms of instability without dislocation, identifying the position of the leg when instability arises is important. Preoperative live fluoroscopy may be obtained to demonstrate the positions of impingement and instability. Causes of instability include inadequate soft tissue tension, component malposition, and bony impingement.
Intrinsic hip pain after hip arthroplasty must be distinguished from pain from extrinsic causes (Box 86-1). Intrinsic causes of pain include mechanical loosening, sepsis, stress fracture, implant failure, modulus mismatch, and subluxation or impingement.9 Extrinsic causes of pain include lumbar spine disease, neurogenic or vascular claudication, trochanteric pain syndrome related to bursitis, abductor avulsion, tendinitis or abductor deficiency, peripheral nerve dysfunction, abductor or iliopsoas tendinitis, femoral or inguinal hernia, and malignancy.9 A snapping hip may be confused with hip subluxation. Nonunion of the greater trochanter or painful hardware at the trochanter, from cerclage wires or a trochanter fixation plate, produces pain over the trochanter. Spinal stenosis can create radicular pain in the hip, thigh, and gluteal region. Vascular claudication from aortoiliac artery stenosis or in the gluteal branches can cause pain that is worse with activity, better with rest, and also present in the calf if distal run-off is poor. Although vascular claudication is typically due to atherosclerotic disease, it may also be caused by vascular injury during the primary surgery or by malpositioned acetabular screws.
Periprosthetic joint infection should be considered in all patients with a painful THA (see Fig. 86-1). Important elements of the history should include whether the patient is experiencing fevers, chills, or drainage from the wound. Patients who have a history of infection, postoperative hematoma, prolonged wound drainage, previous revision surgery, night pain, or pain with rest have a higher probability of developing infection. A history of other systemic infections, diabetes, nutritional deficiency, or immunocompromised status must also be elicited. Procedures that may cause transient bacteremia such as dental work, colonoscopy, or cystoscopy put the patient at risk for bacteria seeding the hip.
Identifying the patient’s functional status, both before the index arthroplasty procedure and at the current time, is important when determining the goals of surgery. The surgeon should document whether the patient is household or community ambulatory, what distances the patient can walk without taking a rest, whether walking aids such as canes or walkers are used, whether the patient has caretaker assistance, and what activities of daily living the patient is able to perform. Because younger, more active patients are now undergoing primary hip arthroplasty procedures, the surgeon should also understand what types of sports and fitness activities the patient wishes to be able to do. Quantitative functional outcome measures, including the Harris hip score, can be helpful in assessing a patient’s functional status both before and after THA.
A comprehensive medical evaluation is necessary to ensure that the patient’s overall health is optimized before surgery is begun. Poor dentition can increase the risk of infection; therefore patients should undergo dental cleaning or obtain dentures well in advance of the date of surgery. Poor nutrition is also a risk factor for infection; the nutritional status of patients can be assessed at the preoperative planning stage by measuring serum albumin, prealbumin, and total protein in high-risk patients.15–18 Patients with low prealbumin are at risk of poor wound healing and may need nutritional supplementation before the time of surgery. Peripheral vascular disease can increase the chance of infection, venous stasis ulcers, and deep venous thrombosis (DVT). If the patient has had a previous recent DVT, a lower extremity ultrasound is indicated to confirm resolution. In some cases, as in periprosthetic fracture or dislocation, surgery must be done immediately. In those cases, if a DVT is present, surgery should be delayed, or an inferior vena cava filter should be placed to prevent symptomatic pulmonary embolus. Similarly, if the patient is at risk of stasis because of poor ambulatory status from severe disability, recurrent dislocation, or periprosthetic fracture, a preoperative ultrasound may be considered to rule out DVT. Revascularization procedures for arterial insufficiency should be done in advance of revision hip arthroplasty procedures when in the opinion of a vascular surgeon the circulation is too poor to allow proper wound healing. This is a rare occurrence.
Urologic disorders such as benign prostate hyperplasia, urinary retention, and urinary tract infection should be addressed by a urologist. Urinary tract infections are common in the revision hip arthroplasty population and may put the hip at risk of being seeded as well. Hematologic disorders are also important to know about and are rarely identified. Difficulty with clotting or prolonged wound drainage during previous hip surgery may put the patient at risk for hematoma formation and wound infection. Preoperative hemoglobin levels should be measured to assess for anemia. The use of erythropoietin preoperatively to raise hemoglobin levels and reduce the amount of postoperative blood transfused may be considered.19 Patients with body mass index greater than 35 are at increased risk of dislocation and would benefit from weight reduction,20 although this is often futile. Cardiac and pulmonary comorbidities should be optimized before surgery to reduce anesthetic and surgical risks. Patients with a history of coronary bypass surgery, coronary stents, or congestive heart failure may need a preoperative pharmacologic stress test or cardiac catheterization if indicated. Diabetic patients should have their blood sugar control improved before undergoing surgery. Poor glycemic control has been shown to be associated with increased risk of stroke, urinary tract infection, ileus, postoperative hemorrhage, blood transfusion, wound infection, and death.21
Physical Examination
The physical examination of a patient with a painful THA should involve a comprehensive evaluation of both lower extremities and the spine, along with a full motor, sensory, and neurovascular examination.
Patients with a failed THA can have a number of gait patterns. Trendelenburg gait is a sign of hip abductor dysfunction and is more common after the direct lateral approach.9 Causes of hip abductor dysfunction can include poor strength, poor abductor tension, superior gluteal nerve injury, trochanteric nonunion, and a failed repair. In addition to causing a limp, poor abductor strength can put the patient at risk of dislocation. If a trochanteric fracture or a nonunion occurs, this may be repaired at the time of surgery, although such repairs are not very predictable when done late. If abductor function is absent, a constrained liner may have to be available at the time of surgery. An extensor lurch occurs when the back hyperextends during the stance phase to compensate for a weak gluteus maximus. Drop foot gait, a sign of peroneal nerve injury, is manifested by the patient using high degrees of hip and knee flexion to clear the foot during the swing phase. During antalgic gait, the patient may use short steps to minimize motion at the hip. Finally, during short leg gait, a sign of limb length discrepancy, the pelvis will be noted to tilt downward, and the shoulder will be tilted upward on the short leg side.
Examination of previous incisions can guide both diagnosis and treatment planning. Existing scars and previous operative reports should be reviewed to determine which surgical approach has been used in the past. Previous wounds should be inspected for signs of infection, including warmth, erythema, fluctuance, wound drainage, and sinus tracts. In rare cases of chronic wounds with exposed prosthesis, bone, or hardware, muscle flap coverage by a plastic surgeon may be required. Local wound care is possible for small superficial wounds.22 The surgical approach for revision surgery is guided by both the anatomic exposure that is required and the familiarity of the surgeon with particular approaches. Skin bridges between old and new incisions, or in cases where two incisions are required at the time of revision surgery, should be maximized to preserve skin blood supply. Commonly, extensile approaches are required to safely remove existing prostheses, treat bone deficiency, and implant revision components. The posterior approach is frequently used because it can be easily extended both proximally and distally.
Limb length discrepancy is common after failed primary hip arthroplasty and should be corrected as much as possible at the time of revision surgery. In many cases, however, full correction is not feasible, and patients should be counseled accordingly. Multiple methods may be used to measure limb length discrepancy. True limb length discrepancy is the distance from the anterior superior iliac spine to the medial malleolus with no pelvic tilt. The apparent limb length discrepancy is the distance from the umbilicus to the medial malleolus. Preferably true and apparent leg lengths should be measured with graduated blocks because patients with lumbar spine disease and fixed pelvic obliquity or both may present with notable differences between their true and apparent limb length discrepancies.9 When significant deformity, scoliosis, flexion contractures, or obesity is present, a scanogram radiographic series or a computed tomography scan may be necessary. Progressive limb shortening after the primary procedures is suggestive of mechanical failure of fixation.9
Range of motion should be carefully measured to determine which positions re-created the patient’s pain and/or instability symptoms. Pain with active ROM or extremes of motion can be indicative of loosening, whereas pain with passive ROM is suggestive of sepsis. Pain with a positive straight-leg raise suggests sciatic nerve irritation. Apprehension in certain positions is indicative of instability or impingement. Patients with instability may have a palpable or audible click during ROM. Pain with resisted hip flexion and passive extension is associated with iliopsoas tendinitis.9 Limited ROM may occur secondary to ankylosis of the hip or acetabular protrusio. The Thomas test, a test for hip flexion deformity, is positive when flexion of the unaffected hip causes the affected leg to lift off the examination table and lumbar lordosis is maintained.
A detailed neurovascular examination, including motor, sensory, and peripheral vascular examinations, should be performed to assess for neurogenic or vascular causes of pain and dysfunction. Patients with spinal stenosis are at risk for peripheral nerve injury from the “double crush” phenomenon as a result of retraction or excessive limb lengthening.6
Radiographic Evaluation
Preoperative planning for revision hip arthroplasty requires evaluation of serial plain radiographs. Multiple radiographic views can be used to obtain information about bone stock, migration, and osteolysis. Care must be taken to ensure that proper radiographic technique is used, including orientation, penetration, and rotation.
The anteroposterior (AP) pelvis view provides information about limb lengths by comparing the distance from the lesser trochanter to the interischial line. Although Kohler’s line, or the ilioischial line, is used to assess for medial position of the cup, the acetabular teardrop has been found to be a more reliable landmark for detection of medial and superior migration.23 The AP hip view is best obtained with 15 degrees of internal rotation of the lower limbs to best approximate the femoral neck shaft angle. Patients with contractures can be positioned semiprone to allow a perpendicular view of the femoral neck.6 Adequate lateral film of the hip should include the entire prosthesis, cement column, and bow of the femur.6 The shoot-through lateral technique, obtained with a 45-degree angled beam with the affected hip extended and the contralateral side flexed, is used to assess acetabular version. For patients with hip flexion contracture, a Lowenstein lateral, or a “table down lateral,” can be obtained with the affected hip and knee flexed and the patient positioned in a lateral decubitus. The advantage of a Lowenstein lateral is that it demonstrates the femoral bow. In particular, if a femoral prosthesis longer than 15 cm is anticipated, it is helpful to evaluate the femoral bow preoperatively. A full-length AP and lateral view of the femur is indicated in cases of periprosthetic fracture, anticipated osteotomy, and ipsilateral hardware or total knee arthroplasty with stemmed implants. Judet views assist in evaluating bone stock and the integrity of the anterior and posterior columns.
Identifying which components may have to be removed is an important part of the radiographic evaluation. In an epidemiologic study of revision total hip arthroplasty, 41.1% of operations involved all component revision, 13.2% involved femoral component revision, 12.7% involved acetabular components, and 12.6% involved femoral head and liner exchange.3 Loosening of a cemented femoral component can be classified radiographically.24 Possible loosening is present when a radiolucent line spans 50% to 100% of the bone-cement interface. Probable loosening is characterized by a continuous or 2-mm-wide line at the bone-cement interface. Definite loosening is present when the following are noted: stem migration, a new continuous radiolucent line at the prosthesis-cement interface, prosthesis fracture, or cement fracture. Porous ingrowth stems can have signs of osseointegration, which include endosteal spot welds and radiodense lines around the coated part of the stem, calcar atrophy, a stable distal stem, and absence of a pedestal.11 Failed osseointegration, on the other hand, is demonstrated by reactive lines around the porous stem and by the lack of endosteal spot welds, as well as implant migration distally or into varus.11 In cemented acetabular cups, loosening can be estimated by the number of 2-mm demarcation zones identified on radiographs.25 Migration of the cup and cement mantle together is defined as socket break-in, and migration of the cup relative to the cement is defined as socket break-out.6 Findings have been mixed regarding the use of radiographs to determine whether porous ingrowth acetabular components are well fixed.26,27 Migration, screw breakage, and component fracture, however, are definite signs of failure of cementless cups. Continuous radiolucent lines and evidence of bead shedding suggest probable loosening.
The degree and location of bone loss must be determined during the planning stage. Kitamura and associates demonstrated that the AP radiograph has 67% sensitivity and 72% specificity for detecting acetabular osteolysis.28 Sensitivity improved to 90% when the osteolysis lesion volume was greater than 10 cm3. Thomas and colleagues demonstrated the value of Judet oblique radiographs in identifying osteolysis lesions. In a retrospective review of patients undergoing revision hip arthroplasty, the mean osteolytic area on AP radiograph was 384 mm2, whereas the area on obturator oblique and iliac oblique radiographs was 790 mm2 and 512 mm2, respectively. Claus and coworkers reported that although multiple radiographic views allow for better approximation of osteolysis size and location, radiographs still have limitations. In their study, the sensitivity of detecting an osteolysis lesion on a single radiograph was 41.5%, but sensitivity increased to only 73.6% when four views were obtained. Saleh and associates have described a classification system based on standardized plain radiographs that is reliable for predicting bone loss at the time of revision surgery.29
Computed tomography (CT) imaging has been found to better demonstrate osteolytic lesions than plain radiographs30 (Fig. 86-2). Kitamura and associates demonstrated how CT imaging can be used to differentiate osteolysis from preexisting bone defects by the identification of communication pathways. Lesions without communication pathways were smaller and not associated with cortical erosions, whereas lesions with pathways were larger with erosions. In their study, cortical erosions were a hallmark of osteolysis lesions.31 To avoid radiation exposure, some have used new magnetic resonance imaging (MRI) protocols to assess for acetabular osteolysis. Weiland and colleagues reported that MRI has a sensitivity of 95% for osteolysis detection.32 Walde and coworkers found that the sensitivity of detecting osteolytic lesions was 51% for radiographs, 74% for CT, and 95% for MRI. Although MRI was found to have higher sensitivity than CT, CT was found to be more accurate in detecting lesion volume.33
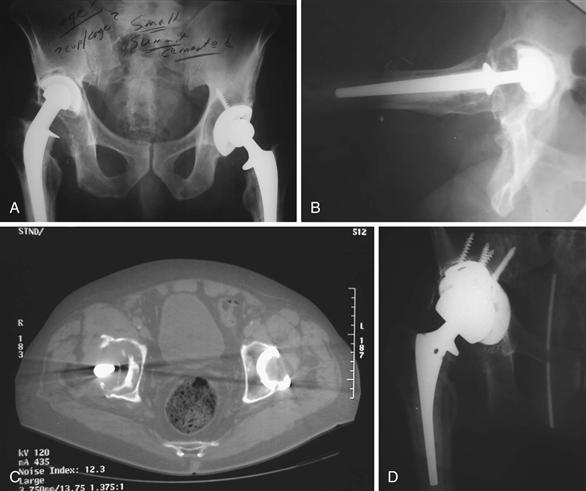
Figure 86-2 Imaging of acetabular osteolysis. A and B, Anteroposterior (AP) and lateral views demonstrating acetabular osteolysis with superior migration of the acetabular component. C, Computed tomography (CT) scan better demonstrating location and volume of acetabular bone loss. D, Revision of acetabular component with tantalum cup with augment. (Courtesy Robert Gorab, MD.)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








