Implant Removal in Revision Hip Arthroplasty
Daniel H. Williams, Donald S. Garbuz, Clive P. Duncan and Bassam A. Masri
Key Points
Introduction
The key aims of revision total hip arthroplasty are (1) to extract failing components, ensuring minimal damage to host bone and soft tissue, (2) to implant new components to provide long-term stable fixation, and (3) to manage bone loss by augmenting deficient bone stock. Preserving the maximum possible intact host bone during implant removal provides an optimum platform on which to build a successful reconstruction. The ease of implant removal depends on the implant design and the method of fixation employed at the primary procedure, how well the primary procedure was performed, the host response to the implant, and the cause of implant failure. Thus the removal of cemented components presents challenges unique to the removal of components fixed without cement. Loose implants may be “tapped” out, whereas solidly fixed components can be technically challenging to remove. This chapter will discuss the principles and techniques applied to different etiologic settings for the removal of failing acetabular and femoral components. Emphasis will be placed on preoperative planning and the surgical approach in the revision setting; discussion will focus on the management of difficult scenarios, such as the distally fixed broken stem.
Indications/Contraindications
Once the decision has been made to proceed with revision surgery, general principles dictate that failed or failing implants should be removed and replaced. Certain indications for implant removal are clearer than others. Broken components clearly need to be removed, but the indications for changing implants in cases of instability can be more subtle.
Despite recent improvements in bearing surface material properties, aseptic loosening usually secondary to osteolysis (attributed to the macrophage response to accumulated wear debris) remains one of the main causes of failed hip arthroplasty. Removal of loose implants is clearly indicated, but the paired primary component may be left in situ if solid fixation, component compatibility, and adequate soft tissue balancing can be ensured in combination with the new revision implant. Changing a loose acetabular component may require the replacement of a modular femoral head to achieve these goals. A monoblock stem that is not compatible with the new socket or that provides inadequate soft tissue tension may have to be removed despite being well fixed. Removal might also be necessary during an intended isolated single-component revision when the component to be left in situ is inadvertently damaged (e.g., trunnion damage, scratching of the head on a monoblock stem).
If detected early enough, osteolytic defects around solidly fixed implants with satisfactory position and an intact locking mechanism can be managed without component removal. Bearing surface exchange, with or without bone grafting of the osteolytic defect, may allow satisfactory treatment (see Chapter 88). Cementing a new liner into a well-fixed acetabular shell is a good option in suitable patients1 if the available liner is not compatible with the in situ socket. This technique can also be considered when a liner of increased constraint, obliquity, or posterior wall height is required for the treatment of instability. This technique necessitates the sole removal of the liner without removing a well-fixed acetabular component—typically an easy task that does not require any specialized techniques.
Cement-in-cement revision of the femur is appropriate when the cause of revision is not on the femoral side and the cement-bone interface remains pristine. Bonding of the new cement to the old mantle is good and allows implantation of a smaller cemented stem. Specific cemented revision stems have recently come to market for this purpose, and the technique has good reported medium-term results.2–5 The technique is suitable when treating the failed acetabular component where the stem requires removal only to grant access to the acetabulum. Substantial correction of femoral version may not be possible with this technique, although minor correction is possible as long as the cement mantle is not fractured in the process.
Traumatic periprosthetic fractures usually affect the femur. The femoral component may be retained in the treatment of Vancouver classification type A and C fractures, which do not violate the bony interface with the stem or the cement mantle. Type B1 fractures are identified by the presence of a well-fixed stem, which can be retained. Type B2 fractures (with a loose component) and B3 fractures (with inadequate bone) require stem and any cement mantle to be removed before reconstruction is begun.6
Two or more episodes of recurrent dislocation indicate the need to proceed to revision in medically fit patients. Well-fixed components may be retained:
If these conditions are not met, one or, less commonly, both components may have to be removed.
Recommended treatment of chronic periprosthetic infection requires removal of all foreign implant material, followed usually by a two-stage reconstruction.7,8
Other causes of revision specific to the use of alternative bearing surfaces include “squeaking” or rarely fracture of a ceramic-on-ceramic bearing couple, which generally requires implant removal. Management of raised serum metal ions in association with a metal-on-metal bearing couple is controversial.9 In the symptomatic patient, with or without the presence of so-called pseudotumor, removal of components becomes necessary to allow revision to an alternative bearing surface. The same treatment may be recommended in the asymptomatic patient with an overly abducted or anteverted acetabular component. Failure of hip resurfacing secondary to femoral neck fracture clearly requires the removal of at least the femoral component, if not both components, to convert to a non–metal-on-metal bearing surface.
Preoperative Planning
Preoperative planning for implant removal in hip revision surgery cannot be divorced from preoperative planning for hip reconstruction (see Chapter 86). Planning for implant removal focuses on selection of the appropriate approach to the hip, including the requirement for an extensile exposure or osteotomy, and choice of the appropriate instruments required to remove failed components. Planning must therefore consider decisions made at the primary procedure regarding the choice of implant design and the method of fixation employed, how the primary procedure was approached and how well it was performed, the host response to the primary implant, and the cause of implant failure.
Thus relevant documentation and background information from the primary procedure, including implant labels showing the manufacturer, brand, size, and catalogue number of the components, need to be available. The function of the liner locking mechanism of an uncemented component should be understood and specialized tools for removal of the liner made available. The correct screwdriver for screw removal and other specialized tools for implant removal should also be available. On the femoral side, if a cemented stem was precoated with methacrylate, removal may be significantly more challenging, and femoral osteotomy may be required. The distal extent of any porous coating and the point at which any metaphyseal taper meets the cylindrical distal part of the stem should also be known ahead of time.
Up-to-date and previous serial plain radiographs of the hip (if available) should include an anteroposterior (AP) pelvis, a centered AP of the hip and femur, and a lateral radiograph of the involved hip of sufficient length. Forty-five–degree Judet views allow assessment of the integrity of the anterior and posterior columns and the extent of any osteolytic lesions.10 Vascular contrast studies may be indicated if there is concern that the iliac vessels may be damaged during removal of the acetabular component. If the vessels lie between the implant and the bone, a retroperitoneal approach to the socket would be favored. An adequate picture of the distal extent and distribution of any femoral cement mantle guides the direction of osteotomes, chisels, and other cement removal instruments at the time of revision surgery. A good quality lateral is particularly useful in this regard. Computed tomography (CT) or magnetic resonance imaging (MRI) can demonstrate cement that does not contain radiopaque barium, and a CT scan can provide a more accurate picture of bone loss.11 The criteria for loosening of cemented12,13 and uncemented14 components have been published elsewhere and are beyond the scope of this chapter.
Preparation for an extensile exposure, osteotomy,15–17 or cortical window18–22 should be done preoperatively and all suitable instruments made available. The templated length of an extended trochanteric osteotomy (ETO)15–17 measured on the AP radiograph should ensure that any broken stem, femoral stem porous coating, or retained cement can be readily accessed. Preoperative planning for implant removal cannot be separated from planning for femoral reconstruction, and the templated femoral stem length should bypass the distal extent of any osteotomy by a suitable distance, usually said to be approximately two diaphyseal diameters.
Occasionally, a specific extractor may be required for a particular stem or for part of a stem (in the case of modular stems or a modular centralizer attached distally to an uncemented stem). If unfamiliar with a particular stem design, the surgeon should contact the manufacturer to obtain any specific extraction instructions and to make sure that any required instruments are made available at the time of surgery.
Description of Techniques
With a clear understanding of the indications, and after a preoperative plan has been formulated, the surgical approach, acetabular implant removal, and femoral implant removal can be considered.
Surgical Approach
The objectives while approaching the hip during a revision procedure are to adequately expose the hip, preserve bone, preserve soft tissue, and preserve blood supply. The approach should provide sufficient exposure of the components to be removed, any associated bone defects, and any neurovascular structures that require visualization. This allows preservation of the maximum possible intact host bone during implant removal. Planned extensile incisions of sufficient length or osteotomies that can be adequately repaired are preferable to an unplanned iatrogenic cortical breach or periprosthetic fracture.23 Utilization of previously healed incisions without compromising surgical exposure minimizes additional scar tissue. Finally, avoiding unnecessary devascularization of bone is of paramount importance, particularly in cases of sepsis, where dead bone can act as a nidus for ongoing infection.
The choice of approach depends on the implant design and its method of fixation, how the primary procedure was approached, the degree of bone loss, and the indication for revision. Good circumferential exposure is required to assess whether cemented or uncemented acetabular components require removal. A more extensile exposure to the outer table of the ilium is required if a reconstruction cage or a metal augment is to be removed (or inserted), or if a superolateral or posterior column defect requires assessment (or reconstruction). If removal of a well-fixed femoral cement mantle is indicated, an ETO15–17 or a cortical window18–22 will significantly improve visualization, particularly of a long column of distal cement. An ETO also is often deemed necessary for removal of a cemented stem that has been precoated with methacrylate. The rigid implant-mantle bond is strong and makes removal of the stem from above impossible. Osteointegrated uncemented stems present a similar problem, and familiarity with design specifications remains important. Knowledge of the extent and location of porous coating, the modularity of the prosthesis, the presence of a collar, and the level at which the metaphyseal flare joins the more tubular distal part of the stem will ensure the correct choice of approach. Varus remodeling of the proximal femur (Fig. 87-1), which is more common when the femoral component is loose, may add considerable difficulty to removal of a straight stem from the intact femur and may indicate the need for an osteotomy. A broken stem, cemented or not, also presents a unique problem that also often requires an ETO15–17 or a cortical window.18–22
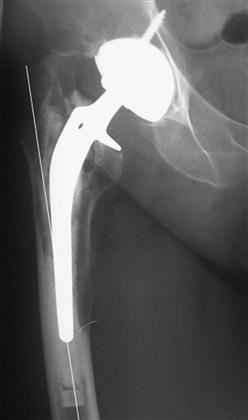
Figure 87-1 Anteroposterior (AP) radiograph showing varus remodeling in response to a stem that has failed with severe osteolysis.
The incision, superficial and deep dissection used to approach the primary, and any previous revision operation should be taken into account. As much of the previous incision as possible should be used at revision to avoid unnecessary railroad-track incisions and attendant risks of wound-edge necrosis. Skin laxity may allow utilization of an incision that is not optimally positioned so long as the correct fascial incision can be made. Deep dissection through a previous exposure is often best employed. A nonunited greater trochanter may provide an obvious route to the hip joint, and a poorly healed transgluteal approach may be reused. Some controversy continues as to whether a gluteal tear should be incorporated into a transgluteal approach24 and repaired during closure of the revision, or whether a posterior approach25,26 should be employed and the gluteal tear ignored. The preferred compromise is reuse of the old gluteal tear, if it affords adequate exposure, and subsequent transosseous repair at the end of the procedure. Otherwise, use of a posterior approach is preferred.25,26 In cases of chronic sepsis, an infected sinus tract, often along the route of the primary approach, is ideally completely excised.
Each of these factors contributing to the choice of approach needs to be balanced with the primary goal of preserving bone during implant removal. The revision arthroplasty surgeon therefore needs to be comfortable not only with the standard anterolateral (see Chapter 18),24,27-32 posterior (see Chapter 19),25,26 and transtrochanteric (see Chapter 20)33,34 approaches to the hip but also with the more extensile approaches, osteotomies, and other specialized exposures (see Chapter 21)15-22,35-37 required to gain adequate access to the acetabular and femoral components.
The Acetabulum
Good circumferential exposure is required to remove a cemented or an uncemented acetabular component while ensuring optimal preservation of intact host bone.
Removal of the Cemented Acetabular Component
The aim is to loosen the solidly fixed cemented acetabular cup from the underlying polymethylmethacrylate (PMMA) cement by one of five methods:
• The all-polyethylene component can be thinned with sequential acetabular reamers.38 The rigidity of the polyethylene diminishes as it becomes thinner, and it is lifted out of the cement mantle when sufficiently flexible.
• A pneumatic impact wrench is used to deliver a repetitive torsional shear load to the implant-cement-bone interface. In eight components tested with this technique, however, one technical failure and one pelvic fracture occurred.39 This technique is therefore not favored.
• A high-speed burr can be used to section the all-polyethylene cup and remove it piecemeal.
Cement-splitting osteotomes are used to remove the cement in a piecemeal fashion. Cement plugs in large and small holes used to achieve a macro-lock at the primary procedure can be carefully curetted out or burred away. Large intrapelvic extensions of cement require removal only in cases of infection, cases of dysuria secondary to bladder irritation by the cement, and cases of dyspareunia in female patients. In most cases, intrapelvic cement may be left undisturbed because it is outside the surgical field, and its presence will not affect the final reconstruction. If removal is planned, preoperative assessment with intrapelvic contrast studies is required and a retroperitoneal approach employed with the assistance of a general surgery colleague.40–44 Thus with adequate preoperative planning and operative exposure, the acetabular implant and the cement may be removed safely, under direct vision, with optimal preservation of intact host bone.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








