CHAPTER 57 Minimally Invasive Posterior Lumbar Instrumentation
Overview
Over recent years minimally invasive surgical techniques have evolved to safely allow access to the spine with less collateral damage as compared with traditional open surgical approaches. The basic principles of spinal surgery remain unchanged. The most basic tenant of minimally invasive spine surgery is to perform the same surgery as has traditionally been done open but with less soft tissue destruction and equal or better outcomes. Minimally invasive surgical techniques have demonstrated less blood loss, shorter hospital stays, and lower infection rates as compared with open surgical techniques.1–5 However, operative times are longer and there may be a trend toward more technical complications.1,2 Also, there is a prolonged and slow learning curve associated with minimally invasive surgery.
Obesity
Approximately one third of American adults older than the age of 20 are considered obese.6 Complication rates as high as 36% to 50% have been reported for obese patients undergoing lumbar fusion.6 Although obesity certainly makes minimally invasive surgery more challenging, it can be done safely and effectively in this population. The authors’ personal experience has found that oftentimes pedicle screws can be placed more easily through a minimally invasive Wiltse-type approach as compared with midline approaches because there is much less muscle, fat, and soft tissue retraction necessary to obtain the correct screw trajectory. Also, the retractor can help to keep adipose tissue and the deep (often thick) musculature out of the surgical field.
Park and colleagues7 compared the perioperative complications in patients with a BMI greater than 25 kg/m2 with patients having a BMI less than 25 kg/m2 who underwent a minimally invasive lumbar spinal surgery. Minimally invasive decompressions in patients with a BMI greater than 25 kg/m2 had a 6.5% complication rate as compared with 11.8% in patients with a BMI less than 25 kg/m2. Minimally invasive fusion procedures had a 24% complication rate in patients with a BMI greater than 25 kg/m2 as compared with 25% in patients with a BMI less than 25 kg/m2. No infections were recorded in either group. No statistical differences were noted between groups. Similarly, Rosen and colleagues6 did not find a correlation between BMI and postoperative changes in ODI, VAS, and SF-36 scores using a linear regression model.
Minimally invasive fusions in obese patients also create less postoperative dead space, which may lead to lower infection rates. O’Toole and colleagues8 reviewed surgical site infections in MIS decompressions, discectomy, and fusion cases. One-thousand, three-hundred, and thirty-eight cases were included for the review. Three postoperative surgical site infections were identified. Two patients developed superficial cellulitis after minimally invasive fusions, and one patient developed discitis after a microendoscopic discectomy (MED). The reported surgical site infection rate for simple decompressive procedures was 0.1% and 0.74% for fusion with internal fixation. The overall infection rate for the entire cohort was 0.22%. The reported infection rate for minimally invasive fusion compares favorably with open fusion infection rates. Importantly, there were no cases of postoperative deep wound infection in O’Toole and colleagues’ cohort. The one patient with discitis developed symptoms 1 month after developing a lower extremity cellulitis. The disc space biopsy grew the same organism as the cellulitis. No patient in their series required reoperation for a deep wound infection. In contrast, Picada and colleagues9 reported a 3.2% deep wound infection after reviewing 817 patients who underwent an open lumbosacral fusion. Minimally invasive fusions can be performed safely and effectively in obese patients, but these cases may be more technically demanding as the working length through the tube increases.
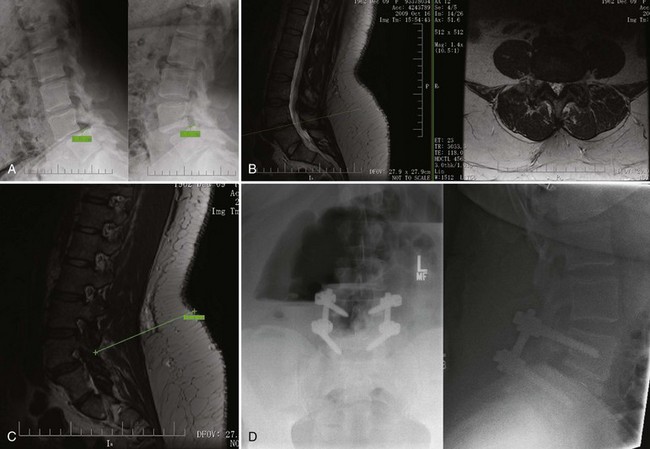
In obese patients the authors have found it helpful to measure the distance from the dorsal aspect of the facet at the level of the intended procedure on the preoperative magnetic resonance imaging (MRI) to help determine the length of retractor needed in heavier patients (Fig. 57–1). During a surgeon’s initial experience with minimally invasive fusions, patients with an expected retractor length greater than 80 mm are a relative contraindication, particularly early in the learning stages. However, with experience obese patients are a relative indication for minimally invasive fusion and instrumentation rather than a contraindication.
Technical Outcomes of Minimally Invasive Fusion Surgery
At the time of this publication there is still a relative paucity of published literature detailing the clinical results of minimally invasive fusion surgery. Early studies have demonstrated minimally invasive fusion to be safe and efficacious.5,10,11
Kim and colleagues12 compared tissue injury markers between minimally invasive posterior lateral lumbar interbody fusion (PLIF) and open PLIF. Significantly larger increases were observed in creatinine kinase, aldolase, IL-6, IL-10, and IL-1ra in the open PLIFs compared with the minimally invasive PLIFs. This confirms less muscle injury in the minimally invasive fusions and may result in a lower systemic inflammatory reaction in the immediate postoperative period, which in turn may lower acute medical morbidity. However, clinical studies have not documented this to date.
Shizas and colleagues4 and Peng and colleagues3 both compared minimally invasive transforaminal lumbar interbody fusion (TLIF) with open TLIF for the treatment of spondylolisthesis and degenerative disc disease. The average hospital stay was 2 days shorter following minimally invasive TLIF as compared with open TLIF. Blood loss was significantly less, but the operative time, at least in the Peng3 study, was 45 minutes longer. Overall the complication rates were similar between open TLIF and minimally invasive TLIF. Schizas and colleagues4 reported two technical complications in each group. However, they found three pseudoarthroses in the minimally invasive group compared with none in the open group. Peng and colleagues3 observed that 80% of the minimally invasive TLIFs were solidly fused compared with 87% of the open TLIFs. Peng and colleagues3 also noted a 7% complication rate in the minimally invasive group compared with a 14% complication rate in the open group. Both Peng and colleagues and Schizas and colleagues found similar improvements in Oswestry Disability Index (ODI) scores. Minimally invasive TLIF ODI scores improved by 22% compared with improvement of 27% in the open TLIF group reported by Schizas and colleagues. These authors observed a 29-point improvement in ODI scores in minimally invasive TLIFs and a 30-point improvement in open cases.
Traditional Pedicle Screws
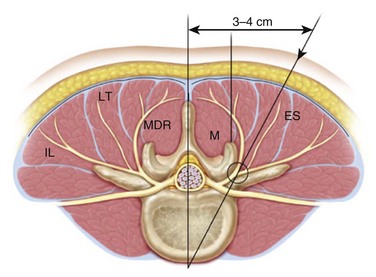
Minimally invasive fusions use the surgical corridor as described by Wiltse13 between the multifidus and longissimus paraspinal muscles (Fig. 57–2). This trajectory is ideal for both pedicle screw placement and interbody work.
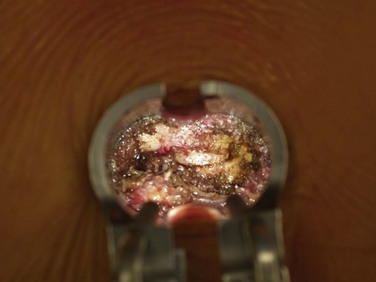
After the appropriate trajectory is localized with fluoroscopy, sequential dilators are passed through the fascia and docked onto the facet joint. A tubular retractor (typically 20 or 22 mm) is then docked and secured over the dilators. The use of an expandable retractor allows the blades to expand cephalad or caudad, creating a corridor for pedicle screw placement (Fig. 57–3). Soft tissue is cleared to expose the standard pedicle screw entry points (Fig. 57–4). Screws can be placed using a variety of methods including free hand, under C-arm guidance, or using navigation depending on surgeon preference. In addition, both posted- and tulip-style screws can be used if working through the tubular retractor systems that are available.
< div class='tao-gold-member'>
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree