CHAPTER 20 Lateral and Posterior Approaches to Lumbosacral Spine
Minimally Invasive Lateral Approach to Spine
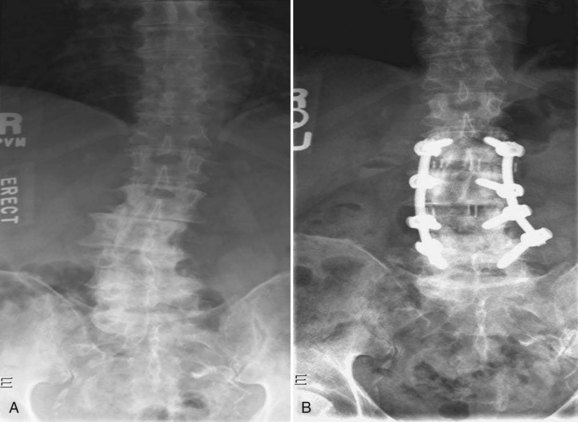
The concept of minimally invasive spine surgery is attractive to patients and surgeons. Decreased postoperative pain, shorter hospital stay, and quicker return to activities support the use of minimally invasive techniques when achievable. One technique is the lateral access to the spine.1,2 This technique can be used for multilevel interbody fusions to correct kyphoscoliosis, for interbody support when treating adjacent segment degeneration or multilevel fusions, or to drain a psoas abscess (Fig. 20–1). With this approach, access to the spine from T7 down to L4-5 is possible. L4-5 is often difficult to reach, however, because of a high-riding iliac crest, and the means to access L5-S1 laterally has not been developed.
Technique
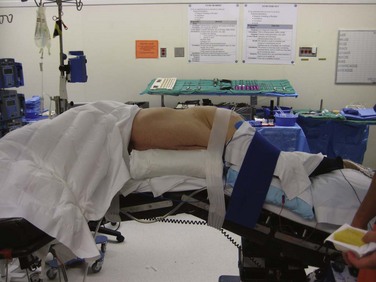
After the patient has been intubated and prophylactic antibiotics have been given, the patient is placed in the lateral decubitus position. When correcting a kyphoscoliosis, it is easier to perform the lateral approach on the side of the concavity. The table should be flexed to increase the distance between the iliac crest and the rib cage, and the patient should be secured with tape over the greater trochanter and chest wall (Fig. 20–2). The leg on top should also be flexed to relax the psoas. A cross-table anteroposterior radiograph should be taken, and the table should be rotated to place the patient in a true anteroposterior position. A corresponding lateral fluoroscopic image should also be taken to verify that access to the disc space is possible. Minor adjustments should be made to the table to obtain a true lateral image.
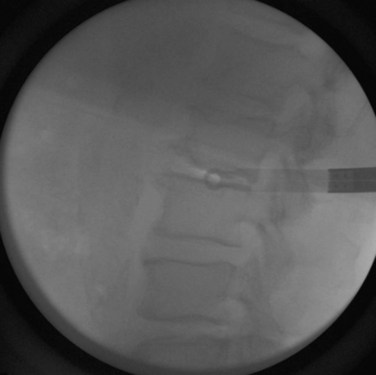
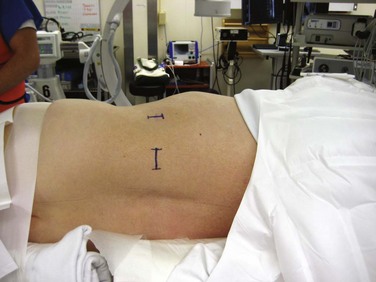
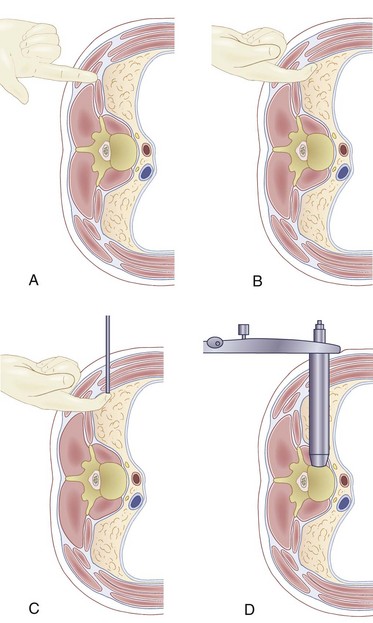
After the patient has been prepared and draped, the lateral image is obtained first. A radiopaque marker is placed over the center of the affected disc space (Fig. 20–3). When this point has been identified, a mark is made. Through this mark, a small incision is made for insertion of the dilators and an expandable retractor, which provides access to the lateral spine. A second mark is made posterior to this first mark at the border between the erector spinae muscles and the abdominal oblique muscles. At this second mark, a transverse incision about 2 cm long is made to accommodate the surgeon’s index finger (Fig. 20–4). Finger dissection is used down to the lumbodorsal fascia. A clamp, or scissors, can be used to spread the fascia and muscle fibers and provide entry into the retroperitoneal space.
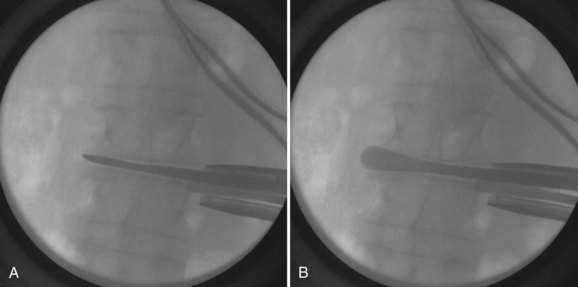
When an opening is created, the index finger is used to sweep the peritoneum anteriorly and to palpate the psoas muscle (Fig. 20–5A and B). The surgeon uses the index finger to sweep inferiorly to feel the inner table of the iliac crest (if in the lower lumbar spine) to verify that he or she is in the abdominal cavity. When the psoas is identified, the index finger is swept up to the previously made direct lateral mark. A 2-cm incision is made; the external and internal oblique muscles and the transverses abdominis muscles are split, and dilators are placed through this opening. The index finger, which is already in the retroperitoneal space, guides the initial dilator onto the psoas (Fig. 20–5C). The fibers of the psoas are split with the dilator using neurologic monitoring as a safety measure, if desired. A lateral radiograph should be obtained to verify the central position of the dilator at the desired disc space. After the position of the initial dilator is secured by placing a Kirschner wire through the dilator and into the disc space, larger dilators are used to spread the psoas under neurologic monitoring, and then an expandable retractor is placed over the dilators (Fig. 20–5D).
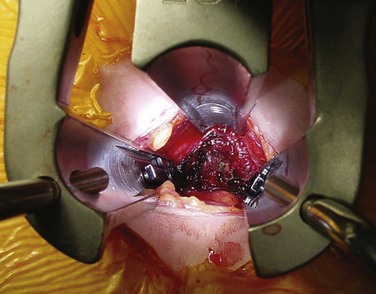
After the retractor is secured to the table, the dilators are removed to provide lateral access to the disc (Fig. 20–6). A neurologic monitoring probe can be used to check for any nerves that may be crossing the working window of the retractor. If a nerve is detected, the Kirschner wire should be repositioned away from the nerve, and the psoas should be redilated. If this fails, conversion to another means of interbody fusion should be considered because repeated positioning of the retractor, or pressure on the nerve, could result in postoperative paresthesias or palsies.
Anteroposterior and lateral radiographs should be taken at this point to verify that the retractor is docked on the disc space and that the retractor is positioned over the center of the disc. When appropriate positioning has been confirmed, the retractor should be secured in place. A lateral discectomy is performed in standard fashion with shavers, curets, and rasps. A Cobb elevator should be used to release the contralateral anulus (Fig. 20–7). Releasing the contralateral anulus loosens the spine in the coronal plane and aids in the correction of coronal plane deformities. Sizers and trials are used to determine the optimal implant size. The implant is filled with the surgeon’s graft or fusion enhancer of choice and impacted across. The wound is closed in layers. No drains are typically necessary.
Posterior Approach to Lumbar Spine
The posterior approach through a midline longitudinal incision is the most common approach to the lumbar spine.3 It provides direct access to the spinous processes, laminae, facets, and even pedicles and lateral aspects of the vertebral bodies at all levels of the lumbar spine. The pedicle starting holes and transverse processes can be reached by dissecting and retracting the paraspinal muscles laterally. Through this approach, it is possible to perform most of the spine procedures currently practiced today, including microdiscectomies, laminectomies, and most fusion procedures. The posterior aspect of the vertebral body and disc space over the lower lumbar levels can be reached after laminectomy by retracting the dura, but the exposure is limited.
Technique
A midline incision is made between the spinous processes of the levels to be exposed, and the erector spinae and multifidus muscles are dissected from the bony elements (spinous processes, interspinous ligaments, laminae, facet joints, and transverse processes) as needed for the levels that must be visualized, using electrocautery or sharp dissection (Fig. 20–8). The paraspinal muscles should be elevated subperiosteally to minimize blood loss. Care should be taken not to injure the facet joint capsules and interspinous ligaments in areas where motion would be expected after the operation. If the transverse processes must be reached, dissection is continued down the lateral side of the facet joints and onto the transverse process itself. The vessels supplying the paraspinal muscles segmentally are close to the facet joints and the pars interarticularis. If these vessels are cut, they can bleed vigorously. Cauterization is necessary to stop these bleeders. The posterior primary rami of the lumbar nerves run with these vessels.
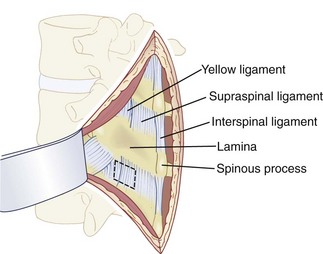
FIGURE 20–8 Dorsal subperiosteal exposure of lumbar spine.
(From Benzel E: Spine Surgery: Techniques, Complication Avoidance, and Management. Philadelphia, Churchill Livingstone, 2004.)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree