CHAPTER 5 Femoroacetabular Impingement: Pincer
Femoroacetabular impingement (FAI) was first reported over 70 years ago.1 However, it was not until recently was it described as a cause of hip osteoarthritis.2–4 Multiple forms of proximal femur and acetabular dysplasias have been described,5–7 but two specific mechanisms of lesion are acknowledged as being responsible for FAI, cam and pincer. Cam impingement occurs when an abnormally shaped femoral head contacts a normal acetabulum, particularly during flexion and internal rotation. Pincer impingement involves a normal femoral head contacting an abnormally shaped, deep, or retroverted acetabulum. The patterns of intra-articular soft-tissue injury resulting from the impingement appear to be unique to the distinct type of deformity.8
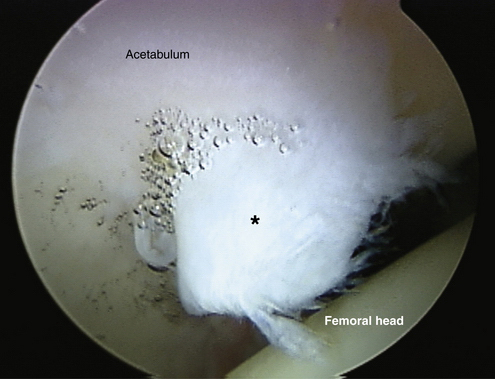
In cam impingement, the “bump” at the femoral head-neck junction produces a shearing force, displacing the labrum toward the capsule and the adjacent articular cartilage into the joint.2,8 Softening of the articular cartilage can be observed as a wave sign when arthroscopically probed before frank chondral delamination.9 With repeated insults, the labrum may completely detach from the acetabular rim, and the cartilage may fully delaminate (Fig. 5-1).
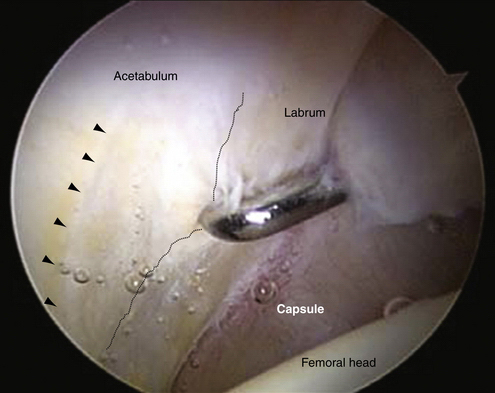
In pincer impingement, the labrum is essentially trapped between the bony structures; thus, it often bruises and flattens.2,8 With persistent pincer impingement, the labrum may degenerate, with cyst formation or ossification of the fibrocartilage. Persistent pincer impingement may lead to a chondral defect (a contrecoup lesion) at the posteroinferior acetabulum or posteromedial femoral head. The chondral injuries resulting from a pincer impingement are typically less severe than those resulting from a cam impingement (Fig. 5-2).
Demographically, cam impingement seems to be more common in young male athletes and pincer impingement in female athletes.2,10,11 Cam and pincer impingement rarely occur in isolation, and the combination has been termed mixed cam-pincer impingement. With this disorder, an abnormal femoral head or head-neck junction articulates with an abnormal acetabulum. In one epidemiologic study of 149 hips with impingement, 26 (17.4%) had isolated cam impingement, 16 (10.7%) had isolated pincer impingement, and 107 (71.8%) had combined cam-pincer impingement.8
CLINICAL PRESENTATION
Pincer impingement may be caused by general acetabular overcoverage (coxa profunda) or acetabular retroversion and has been shown to be associated with osteoarthritis of the hip.2–4,7 During flexion of the hip, the edge of the anterior wall and the anterosuperior roof of a retroverted acetabulum are vulnerable to impingement because they tend to lie directly in the path of the femoral neck.
Reynolds and colleagues7 have described the clinical presentation of acetabular retroversion. In this condition, there is not necessarily any change in the range of movement of the hip. When the retroversion is marked, however, there is a demonstrable alteration in the pattern of hip flexion in the neutral line. This may be limited to as little as 90 degrees, progressing to a full range only when allowed to move simultaneously into external rotation and abduction in a Drehman sign–like pattern.12,13 The contact of the femoral neck to the edge of the acetabulum on maximum flexion and the need to contour its retroverted mouth to continue the full range of motion explains that phenomenon.7 In these individuals, the limb tends to lie at rest in a position externally rotated at the hip. The range of external rotation, especially in the flexed position, is more generous than usual, often exceeding 60 degrees. The range of internal rotation may be limited proportionally. Asked to sit on the floor, such patients are comfortable only with their hips flexed, abducted, and externally rotated. Some describe a dislike of sitting in a chair with legs crossed, especially with the symptomatic leg crossed over the other. In some cases of coxa profunda, abduction may be limited by the lateral impingement of the femoral neck to the acetabulum.14
In the early presentation, the impingement test usually will elicit discomfort felt in the groin.7,15–17 The onset of the symptoms may be related to a new athletic activity, and females seem to be particularly susceptible. The pain is often intermittent and exacerbated by an excessive demand on hip flexion, such as occurs with athletic activities and in very flexible hips. In many cases, individuals take part in athletic activities or have occupations in which some discomfort is accepted as part of the activity. For that reason, a delayed diagnosis is not uncommon.7 Despite the recent attention directed to this condition, some patients have even had surgery in other sites because of a missed diagnosis.
The late presentation will be found in the age range of 30 to 50 years.7 Usually, the patient will remember few or no troublesome symptoms from their younger years, but direct questioning may reveal otherwise. In the impingement test, passive internal rotation induces shear forces at the labrum and will create a sharp pain when there is a labral and/or chondral lesion.2,15–18 Patients with impingement can have pain with athletic activities and even while sitting with the hip extremely flexed. Mechanical symptoms and limitations to athletic and daily activities may be present; these usually indicate intra-articular soft-tissue damage related to the impingement.11 Degenerative signs may predominate after a prolonged time without treatment.19,20
IMAGING
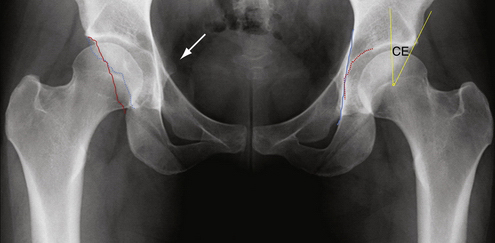
Pincer impingement is the result of overcoverage of the hip. It is commonly associated with acetabular protrusion, coxa profunda, or a retroverted acetabulum.7 Pincer impingement is also the result of a linear contact between the acetabular rim and femoral head-neck junction because of general or focal acetabular overcoverage (Fig. 5-3).7,13
Normally, general acetabular overcoverage is correlated with the radiologic depth of the acetabular fossa. A normal hip appears on an anteroposterior pelvic radiograph with the acetabular fossa line lying laterally to the ilioischial line. A coxa profunda is defined with the floor of the acetabular fossa touching or overlapping the ilioischial line medially. Protrusio acetabuli occurs when the femoral head is overlapping the ilioischial line medially. Both forms relate to an increased depth of the acetabulum; however, at this stage, no clear information exists that the two entities are a continuation of each other.13 Generally, a deep acetabulum is associated with excessive acetabular coverage that can be quantified with the lateral center edge angle or the acetabular index.20 Another parameter for quantification of femoral coverage is the femoral head extrusion index.21 An additional observation on plain radiographs may be juxta-articular fibrocystic changes (herniation pits) at the anterosuperior aspect of the femoral neck.22
The lateral center edge angle is the angle formed by a vertical line and a line connecting the femoral head center with the lateral edge of the acetabulum. A normal lateral center edge angle varies between 25 (which defines a dysplasia)20 and 39 degrees (which is an indicator for acetabular overcoverage).6
The acetabular index is the angle formed by a horizontal line and a line connecting the medial point of the sclerotic zone with the lateral center of the acetabulum. In hips with coxa profunda or protrusio acetabuli, the acetabular index (also called the acetabular roof angle) is typically 0 degree or even negative.13
The femoral head extrusion index defines the percentage of femoral head that is uncovered when a horizontal line is drawn parallel to the interteardrop line.21 A normal extrusion index is less than 25%23; however, to our knowledge, no study has defined a minimum extrusion.13
Focal acetabular overcoverage can occur in the anterior or the posterior part of the acetabulum. Anterior overcoverage is called cranial acetabular retroversion or anterior focal acetabular retroversion; it causes anterior femoroacetabular impingement that can be reproduced clinically with painful flexion and internal rotation.7 By careful tracing on an anteroposterior (AP) pelvis radiograph, the anterior and posterior acetabular rims can be identified. A normal acetabulum is anteverted and has the anterior rim line projected medially to the posterior wall line. To distinguish between a too prominent anterior wall and a deficient posterior wall, the posterior wall must be depicted in more detail. These situations can be distinguished by the crossover sign, the ischial spine sign and the posterior wall sign.13,24
A focal overcoverage of the anterosuperior acetabulum causes a cranially retroverted acetabulum. This is defined with the anterior rim line being lateral to the posterior rim in the cranial part of the acetabulum and crossing the latter in the distal part of the acetabulum. This figure-of-eight configuration is called the crossover sign.7
The posterior wall sign was introduced as an indicator for a prominent posterior wall. This can cause posterior impingement with reproducible pain in hip extension and external rotation. In a normal hip, the visible outline of the posterior rim descends approximately through the center point of the femoral head. If the posterior line lies laterally to the femoral center, a more prominent posterior wall is present. In contrast, a deficient posterior wall has the posterior rim medial to the femoral head center.7 A deficient posterior wall is often correlated with acetabular retroversion or dysplasia,23 and an excessive posterior wall can often be seen in hips with coxa profunda or protrusio acetabuli but can also occur as an isolated entity.
The ischial spine sign consists of a pre-eminent projection of that structure to the pelvis on an AP radiograph. It denotes not only global acetabular retroversion, but also the involvement of the whole hemipelvis in the deformity.24
The common use for computed tomography (CT) scans in the evaluation of impingement is to allow three-dimensional reconstruction of the hip joint for detailed definition of femoral head-neck asphericities and reduced offset, which cause osseous impingement, as well as determination of the version of the femoral neck and acetabulum.25,26 Magnetic resonance imaging (MRI) is useful to assess labral injury and the articular cartilage and to evaluate concomitant conditions.26
TECHNIQUE
Surgical Setup
Arthroscopy of the hip can be performed with the patient in a lateral or supine position.27,28 Our preference is the modified supine approach.29 We recommend a combination of general anesthesia with a lumbar plexus sciatic regional block for complete muscular paralysis.30 After the induction of anesthesia, the patient is positioned on a standard fracture table that allows independent lower extremity traction.
Portal Placement
Accurate portal placement is essential for optimal visualization of all intra-articular structures and safe access to the hip joint. We used to do three portals to perform FAI surgeries—the anterolateral, anterior, and distal lateral accessory portals.31 Currently, we think that for most cases, only the anterolateral (lateral paratrochanteric) and midanterior portals are required.10
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree