Femoral Revision
Uncemented Extensively Porous-Coated Implants
Bryan P. Springer and William L. Griffin
Key Points
• Extensively porous-coated stems can be used to treat most femoral defects.
• Clinical results show excellent midterm to long-term survivorship in the revision setting.
Introduction
The success of primary total hip arthroplasty is well documented in the literature with survival rates greater than 90% at 15-year follow-up.1–6 As our population ages, the number of total hip arthroplasties performed is increasing dramatically. Unfortunately, some of these procedures are not successful and require revision. Despite improvements in implant materials and surgical techniques, the number of revisions for failed total hip replacement has not decreased. In addition, expansion of indications to younger, more active patients and improved life expectancy for patients with total hip replacement have increased the number of revisions, and this trend is not expected to decrease. In fact, recent projections indicate that the burden of revision total hip arthroplasty is expected to increase by 137% over the next 25 years.7 In addition, the cost and resource utilization for revision procedures are substantially higher than those for primary procedures.8
The current epidemiology of failed total hip arthroplasty is gathered mainly from large cohort studies and registry data in Europe, Canada, and Australia. These reports indicate that aseptic loosening, osteolysis/wear, and instability are the major causes of failure for total hip arthroplasty.
Springer and associates reviewed a series of 1100 hips that underwent revision total hip arthroplasty over a 20-year period at their institution.9 The most common reasons for failure of the primary total hip arthroplasty were aseptic loosening and instability. These two diagnoses accounted for 61% of all failed total hip replacements. In addition, instability and aseptic loosening accounted for more than 65% of failures of revision total hip arthroplasty leading to re-revision, indicating an area where improvement is needed.
Dobzyniak and colleagues evaluated early failures of primary total hip arthroplasty defined as those requiring revision within 5 years of the index arthroplasty.10 Of 745 revision procedures, 39% occurred within the first 5 years following index total hip arthroplasty. Instability (33%) was the major reason for early failure, requiring revision followed by aseptic loosening (30%) and infection (14%).
Utilizing the Nationwide Inpatient Sample, Bozic and coworkers reviewed 51,345 revision total hip arthroplasties performed in the United States over a 1-year period (October 2005 through December 2006).11 The purpose of this study was to determine the epidemiology of revision total hip arthroplasty. The most common causes of failed total hip arthroplasty requiring revision were instability/dislocation (22.5%), aseptic loosening (19.7%), and infection (14.8%). In addition, full component revision (femoral and acetabular components) was the most common procedure performed to treat failed arthroplasty (41.1%).
Managing the revision femur following failed total hip arthroplasty remains technically challenging. Extensive bone loss from aseptic loosening, sepsis, and osteolysis can lead to a variety of bony defects and a multitude of clinical scenarios. The goals of revision total hip arthroplasty are (1) to obtain rigid initial stability of the implants, (2) to engage the healthy remaining bone proximally or distally with the implant, and (3) to bypass stress risers.
Implant options for the revision femur are numerous and include cemented and cementless fixation. Cemented fixation allows for immediate fixation, is adaptable to a variety of femoral defects, and allows the use of antibiotic-impregnated cemented materials. In many instances, however, a sclerotic endosteal surface leads to poor cement penetration into bone and a decrease in the strength of the bone-cement interface. Clinical results of cemented femoral stems in revision total hip arthroplasty have been poor, with mechanical failure rates as high as 64%.
Cementless stems may engage the proximal metaphysis (proximally coated stems) or may achieve distal fixation in the diaphysis. Femoral revision using proximal fixation with nonmodular, broached systems has met with poor results. Difficulty matching the implant with variable femoral geometry, often with insufficient proximal supports and poor rotational control with lack of distal fixation, has led to high failure rates.12,13 At 8-year follow-up, Berry reported that only 20% of proximally coated implants were free of aseptic loosening.14
In addition, structural allograft (allograft prosthetic composite) or impaction grafting techniques may be utilized in certain clinical circumstances. These implants and techniques are technically demanding, and their use and indications are covered in Chapters 95 and 99.
No one single implant is appropriate for all revision situations, and each case should be considered individually based on the clinical situation and radiographic evaluation. The ideal femoral revision implant would be easy to insert, would have reproducible results, and would be able to handle most revision situations. Extensively porous-coated stems have a long track record of success in revision total hip arthroplasty. These stems are able to handle most femoral defects with reliable clinical results. Meticulous preoperative planning and surgical technique are essential for success. This chapter will focus on the indications, preoperative planning, surgical technique, and results of extensively porous-coated implants in revision total hip arthroplasty.
Indications for Extensively Porous-Coated Stems
A femoral bone defect classification allows for systematic evaluation of the host bone and the amount of bone loss and assists in standardizing treatment of various femoral defects. Although several classifications exist, the system described by Paprosky and Della Valle is treatment oriented and describes the progression of bony defects.15 This classification system is based on an evaluation of the bone and available areas for fixation of implants:
• Type 1: minimal bone loss in the metaphysis and an intact diaphysis (Fig. 96-1A through C)
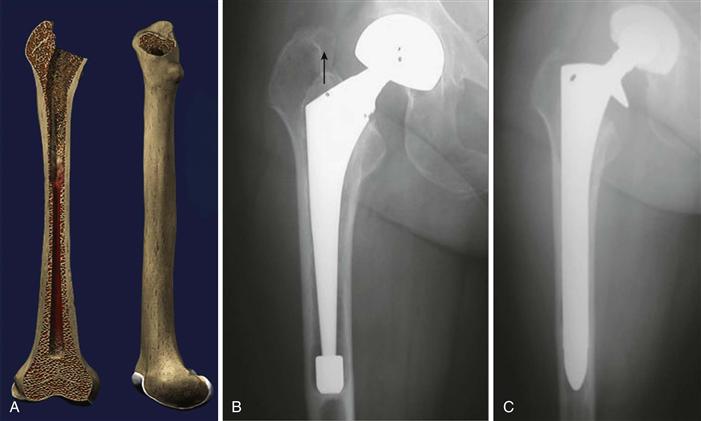
Figure 96-1 Illustration and preoperative and postoperative revision radiographs of a Paprosky type 1 defect treated with a fully porous-coated stem.
• Type 2: extensive loss of metaphyseal bone with an intact diaphysis (Fig. 96-2A through C)
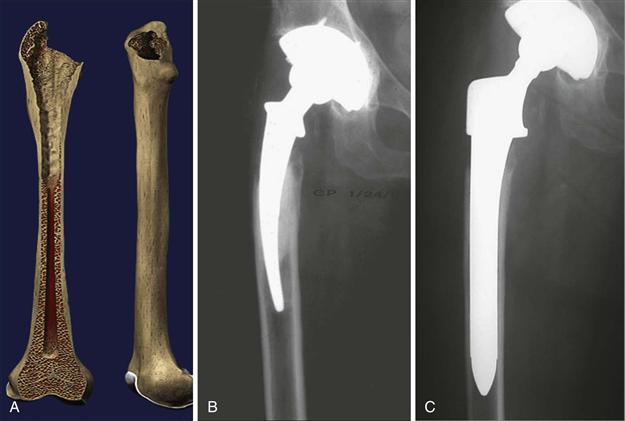
Figure 96-2 Illustration and preoperative and postoperative revision radiographs of a Paprosky type 2 defect treated with a fully porous-coated stem.
• Type 3A: the metaphysis is damaged and unsupportive; a minimum of 4 cm of intact cortical bone is present in the diaphysis at the isthmus (Fig. 96-3A through C)
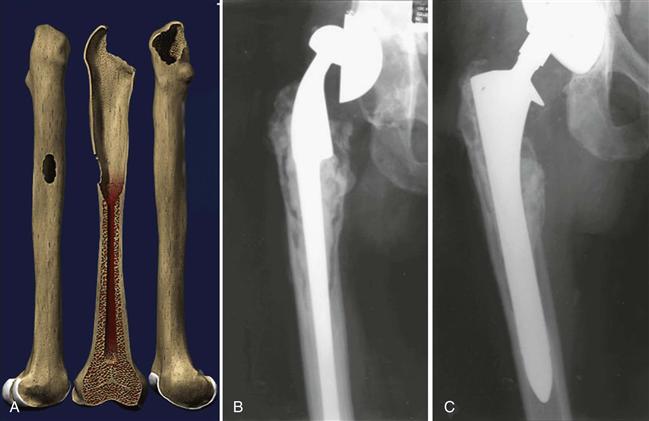
Figure 96-3 Illustration and preoperative and postoperative revision radiographs of a Paprosky type 3A defect treated with a fully porous-coated stem.
• Type 3B: the metaphysis is damaged and unsupportive; intact cortical bone measuring less than 4 cm is present distal to the isthmus (Fig. 96-4)
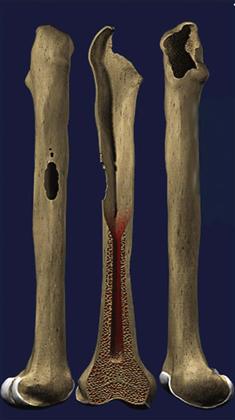
Figure 96-4 Illustration of a Paprosky type 3B defect.
• Type 4: extensive metaphyseal and diaphyseal damage; the femoral canal is widened and is not supportive (Fig. 96-5A through C)
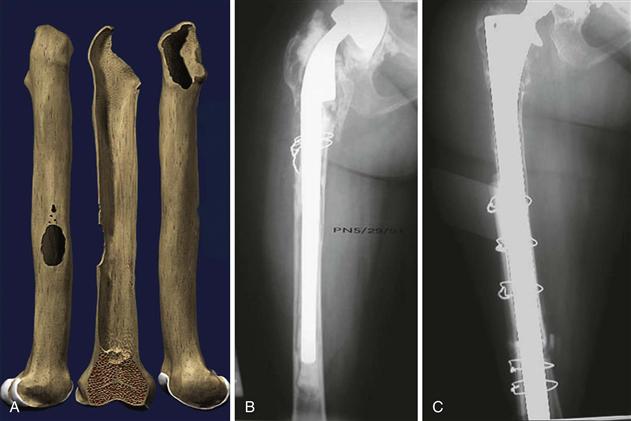
Figure 96-5 Illustration and preoperative and postoperative revision radiographs of a Paprosky type 4 defect treated with a fully porous-coated stem.
Fully porous-coated stems are indicated for use in the revision femur for Paprosky type 1 through 3A femoral defects. Success is dependent on achieving initial implant stability that will allow adequate bony ingrowth to provide long-term fixation. In general, a minimum of 4 to 6 cm of diaphyseal bone should be available to allow for stable fixation. The term “scratch fit” is used to describe the mechanical fit of the cylindrical stem into the host diaphyseal bone. This scratch fit is dependent on meticulous canal preparation and selection of an appropriately sized implant based on preoperative templating and intraoperative findings.
Contraindications
As with any surgical procedure, revision with a fully porous-coated stem is contraindicated in patients with active and ongoing infection. A thorough history, physical examination, and laboratory testing are required to exclude the possibility of infection before proceeding with revision surgery. In addition, medically infirm patients who are too ill to undergo revision surgery should be medically optimized before surgical intervention is provided.
Because the success of fully porous stems in revision total hip arthroplasty is dependent on achieving intimate fit in the diaphysis over a minimum of 4 cm, these types of stems are contraindicated in patients with severe diaphyseal bone loss. The type 4 femur is characterized by significant diaphyseal damage with a capacious medullary canal. In these situations, attaining initial implant stability to achieve bony ingrowth is difficult, if not impossible. The type 4 femur is best treated with alternative means of reconstruction, including impaction grafting, allograft prosthetic composite, fluted tapered modular stems, and proximal femoral replacement.
Sporer and associates reported on the limits of fully porous-coated stems in revision total hip arthroplasty.16 In this study, hips reconstructed with fully porous-coated stems in type 3B and 4 femurs were evaluated. Patients with fully porous stems greater than 19 mm in diameter with 3B femoral defects had a mechanical failure rate of 18%. In patients with type 4 femoral defects and stems greater than 19 mm, the mechanical failure rate was 37.5%. The authors speculate that these patients with poor bone stock and large canals do not have appropriate bony support to allow for initial axial and rotational stability. In these situations, the authors recommend using alternative techniques for femoral fixation.
Preoperative Planning
A reproducible surgical technique starts with a careful preoperative plan.
Most preoperative planning is performed with x-ray evaluation. However, clinical assessment should include an assessment of leg length discrepancies and prior surgical approaches. Leg lengths should be measured by radiographs but should be confirmed with leg length blocks to ensure that the patient is comfortable with the anticipated leg length. Prior surgical approaches may influence the approach used for revision, but whichever approach is used, it should be easily converted to an extensile approach to the femur if needed.
As with any revision, considerable thought should go into planning for component removal. Use of an extended greater trochanteric osteotomy, removal of well-fixed cementless implants, and osteolysis may influence the amount of bone remaining for fixation and allow identification of the appropriate implant needed.
Preoperative radiographs should include an anteroposterior (AP) x-ray of the femoral component and femur distal to the isthmus, along with a true lateral radiograph to assess the extent of femoral bowing (Fig. 96-6). X-ray technologists need to be instructed in the technique for obtaining a true lateral radiograph of the femur. A Lowenstein lateral of the femur positions the patient with both the ankle and the knee flat on the x-ray table, ensuring a true lateral of the femoral bow. This can be critical when planning for a long canal filling femoral component. Magnification markers allow accurate measurement of the diameter of the endosteal canal of the femur and of component length. These measurements help with predicting the size of the femoral component needed at the time of surgery and facilitate intraoperative decision making regarding fit and length. Templates should be applied to the radiographs with the goal of achieving 4 to 6 cm of intimate endosteal contact “scratch fit.” The first step in templating is to select a stem of appropriate diameter to achieve a tight scratch fit. The templated stem is then adjusted axially to provide appropriate leg lengths. The third step is to choose the best stem length to bypass any stress risers and engage the area of scratch fit, while avoiding the anterior cortex of the bowed femur. Stem diameters from 10.5 mm to 21.0 mm and lengths of 6 inches, 8 inches, and 10 inches in straight or bowed configurations are available to best fit the femoral geometry.
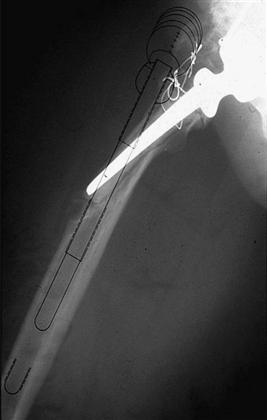
Figure 96-6 Preoperative lateral radiograph should be evaluated and templated to assess the amount of femoral bowing.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








