Femoral Osteotomy
Miguel E. Cabanela
Key Points
Introduction
It is now well established that degenerative arthritis of the hip is generally the consequence of sometimes subtle, sometimes obvious morphologic abnormalities of the joint that produce articular cartilage loads in excess of what the cartilage can tolerate. These abnormalities often become mildly symptomatic early in life. However, although they can be very limiting in the life of a young active adult, they often are not symptomatic enough to justify joint replacement. Furthermore, the longevity of joint replacement in young patients is limited by problems of polyethylene wear and resulting osteolysis, and new bearing surfaces have shown their own set of problems.
Consequently, there has been a resurgence of interest in joint preservation surgery. If a symptomatic joint deformity that reduces the cartilage surface area and results in excessive loads on the articular cartilage above what the cartilage can tolerate for proper viability and function can be corrected by a geometric operation that would increase the area of cartilage available for load and therefore decrease the load per unit area, this would potentially obviate the need for a joint replacement or may delay such surgery. The objectives of the osteotomy most often are to correct the anatomic abnormality, optimize hip congruity, decrease cartilage load/unit area to a level compatible with good function, and improve joint biomechanics. In addition, osteotomy can make the range of motion more functional and can help eliminate fixed deformities.
From a clinical perspective, osteotomy should reduce patient symptoms, help delay the development or progression of osteoarthritis, and therefore delay the need for joint replacement. Thus by its nature, osteotomy often is a temporizing operation, and its results, which are somewhat unpredictable and temporary, are correlated with the fact that the biological capacity of the cartilage to regenerate is not fully predictable or understood. Perhaps the results of osteotomy should not be judged by the same parameters used to judge replacement surgery.
Osteotomy about the hip can be performed on both sides of the joint, that is, the pelvis and the proximal femur. Currently, pelvic osteotomy is far more popular because as techniques have reached significant maturity, the corrective power of the procedure is greater, and the number of patients who can benefit from the procedure is larger. Furthermore, in most patients with hip dysplasia, the anatomic abnormality is more severe on the pelvic side of the joint. In this chapter, we will discuss the remaining few indications for an osteotomy of the proximal femur, an operation that is older than pelvic osteotomy but is more limited in scope of applications and usefulness.
Historically, the operation is almost 200 years old. Barton,1 in 1827, reported on an intertrochanteric osteotomy performed on a sailor with a post-traumatic deformity of the proximal femur. Kirmisson,2 in 1984, described an osteotomy through the proximal femur to treat developmental dysplasia. Surgeons from Germany and Austria introduced modifications to the Kirmisson osteotomy in the first part of the 20th century. Names such as VonBaeyer,3 Lorenz,4 and Schanz5 are associated with developmental dysplasia of the hip (DDH). The first report of a proximal femoral osteotomy to treat osteoarthritis was that of McMurray6 in 1935. He attempted to change the line of load by a large medial displacement of the distal fragment, thereby unloading the articular cartilage. He also introduced the concept of the vascular effect of the osteotomy, whereby increased vascularity brought about by osteotomy healing would have a beneficial effect on the articular cartilage.
It was Pauwels7–9 in 1950 who clearly revolutionized the concept of femoral osteotomy by introducing the concept of valgus and varus osteotomies to increase the weight-bearing surface area of the hip joint. Bombelli,10 in the 1970s, further expanded the Pauwels doctrine by introducing the concept of correction in the sagittal plane by adding flexion or extension to the varus or valgus angulation in an effort to further increase the weight-bearing surface area of the hip joint. Modern day femoral osteotomies are based on the ideas of Pauwels and Bombelli.
Current Indications of Femoral Osteotomies
Patients considered good candidates for femoral osteotomies are those with morphologic hip joint abnormalities in which realignment of the proximal femur would increase the joint contact area. The prime indication is developmental dysplasia with coxa valga. Patients with avascular necrosis and small lesions occasionally can be helped by femoral osteotomy. Those with post-traumatic deformities such as femoral neck nonunion or proximal femoral malunion also may be good candidates for the procedure. Patients with other conditions such as the residua of slipped capital femoral epiphysis (SCFE) or Perthes, or leg length inequality, may be treated occasionally by proximal femoral osteotomy.
Inflammatory arthritis, severe stiffness, and active infection contraindicate the procedure.
Factors that should be considered in decisions regarding an osteotomy are patient age, weight, and occupation (manual laborer vs. sedentary), the condition of the lumbar spine and ipsilateral knee, and leg lengths.
Developmental Dysplasia
The most common anatomic abnormality in dysplasia is found in the acetabulum. Its abnormal slope and deficiency causes the center of rotation of the hip to displace laterally and the femoral head to be poorly covered laterally, anteriorly, and superiorly. This problem is helped by pelvic osteotomy. Sometimes however, associated excessive anteversion and valgus of the proximal femur is the dominant deformity. In this instance—coxa valga luxans of Bombelli—a femoral osteotomy can improve head coverage, medialize the center of rotation, improve function, and, by decreasing the load per unit area of cartilage, decrease pain.11
Prerequisites for a varus intertrochanteric osteotomy include the presence of a spherical femoral head, an increased neck shaft angle, relatively minor acetabular involvement, and good to excellent range of motion. The patient should have no pain with the hip in an abducted position. Radiologically, improvement of femoral head coverage in abduction is a favorable sign, as is satisfactory anterior head coverage in the false profile view. Mild deficiency of anterior coverage can be helped by adding a little extension to the abduction or varus osteotomy.
Varus osteotomy potentially produces marked limb shortening, but this can be minimized by a straight osteotomy made transversely across the proximal femur at the level of the lesser trochanter, followed by repair of the proximal fragment after it is abducted, without removal of a wedge of bone. The resultant gap reliably fills with bone over time. Because of shortening of abductor muscles that occurs with this surgery, abductor weakness persists for a long time, even up to a year, and it is advisable to place patients on a prolonged abductor strengthening exercise program. Finally, it is important to recognize that the osteotomy is unlikely to be the final operation; therefore, it is advisable to avoid producing significant deformities of the proximal femur, which may make the subsequent arthroplasty very difficult. Thus, extending the proximal fragment more than 20 degrees and/or abducting it more than 20 to 25 degrees is not recommended. If greater abduction is necessary, simultaneous greater trochanteric osteotomy and advancement is necessary. Otherwise, the trochanter would overlie the femoral canal, and it would be necessary to osteotomize it at the time of arthroplasty to avoid abductor muscle injury (Fig. 57-1).
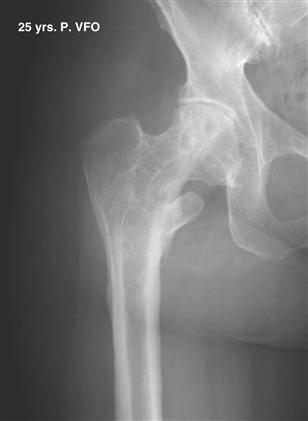
Figure 57-1 Anteroposterior radiograph of the hip of a 72-year-old woman 25 years after a varus intertrochanteric osteotomy. She has become symptomatic enough to undergo joint arthroplasty. Note the position of the trochanter overlying the femoral canal. A trochanteric osteotomy may be advisable for arthroplasty.
When a varus osteotomy of the proximal femur is performed, medial displacement of the distal fragment is necessary to preserve the mechanical axis of the extremity and avoid eccentric knee loads.
It could be said that the results of varus femoral osteotomies correlate with the severity of the pathology treated. If the operation is performed in patients with no or minimal degenerative disease, good to excellent results have been reported in 70% to 90% of patients with follow-up longer than 10 years.12–16 As occurs with osteotomies about the knee, results deteriorate with the passage of time.
Adduction or valgus intertrochanteric osteotomy for dysplasia is done very rarely today in North America. The classical indication is the “out-of-round” femoral head with a large medial osteophyte (Bombelli called this the capital drop osteophyte), an increased neck shaft angle, poor acetabular coverage, and a proximally migrated greater trochanter. An adduction (valgus) and extension osteotomy in this situation would improve joint congruity, unload the superior lateral joint space, and improve joint mechanics by loading the medial osteophyte. Bombelli thought that adduction of the proximal fragment would increase tension on the lateral capsule, and that this might stimulate cartilage metaplasia on the acetabular rim with the passage of time.
Candidates for this osteotomy should have adequate range of hip motion and particularly should be comfortable or should experience reduced pain with the legs crossed in extension (hip adducted). Radiologically, the preoperative x-ray in adduction should show improved joint congruity.
Because valgus osteotomies are done in patients who already have degenerative joint disease, they fall into the category of salvage procedures. Results therefore are less predictable than those of varus osteotomies and typically of lesser quality. Survivorship of the procedure before conversion to arthroplasty at 5 years has been reported in the realm of 50% to 70%.17,18 Patients therefore should be carefully selected, and realistic expectations should be emphasized before this operation is begun.
In truth, these surgeries are performed far less frequently today, when it appears that the results and longevity of arthroplasty in young patients have become more predictable.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








