Extracapsular proximal femur fractures
INTERTROCHANTERIC FRACTURES
Introduction
Hip fractures are associated with mortality, impaired function and decreased quality of life. The 1-year mortality rate after a hip fracture is approximately 20%, with men, patients more than 75 years old and patients in nursing homes at higher risk.1,2 Among patients who were living independently prior to a hip fracture, only about half are able to walk unaided after a fracture,3,4 and many ultimately require care in a long-term facility. The goal of hip fracture treatment is to decrease pain and return patients to their prefracture level of function.
Intertrochanteric hip fractures are extracapsular fractures of the proximal femur involving the area between the greater and lesser trochanters. Such fractures that extend into the area distal to the lesser trochanter are described as having a subtrochanteric component. The intertrochanteric region has an abundant blood supply, which makes fractures in this area much less susceptible to osteonecrosis and nonunion than femoral neck fractures. It is important to distinguish intertrochanteric fractures from fractures that occur just proximal to the intertrochanteric line. These fractures, referred to as basicervical femoral neck fractures, are at greater risk for osteonecrosis (secondary to being intracapsular in some cases) and malunion. However, they may be treated with the same implants used for intertrochanteric fractures.
Internal fixation of intertrochanteric fractures is the mainstay of treatment, although prosthetic replacement is occasionally indicated. Challenges include the combination of often osteopenic or osteoporotic bone and the adverse biomechanics of many intertrochanteric fracture patterns. Other factors include pre-existing osteoarthritis, degree of fracture comminution and pre-existing medical comorbidities.
The literature regarding intertrochanteric fractures points to the difficulty in applying evidence based treatment algorithms. The current evidence is conflicting and does not always support the treatment modalities that are widely used in practice.
Incidence and etiology
Intertrochanteric hip fractures occur in approximately the same demographics as femoral neck fractures. There is a female:male ratio between approximately 2:1 and 8:1. Patients with femoral neck fractures tend to be slightly older than patient with intertrochanteric fractures. Fractures typically occur following a low energy fall from standing height in often osteoporotic patients.
Anatomy
OSSEOUS
The intertrochanteric area extends between the greater and lesser trochanters. It consists of dense trabecular bone. The calcar femorale is an area of dense bone that extends from the posteromedial aspect of the femoral shaft to the posterior portion of the femoral neck (Figure 35.1).
MUSCULAR
Several muscles originate or insert around the hip (Figure 35.2). These muscles account for the typical deformities encountered following injury.
Patient assessment
PHYSICAL EXAMINATION
The patient with a displaced intertrochanteric femur fracture will typically present with inability to ambulate following the fall, pain in the groin, lateral hip and/or buttocks and will have a shortened and externally rotated lower extremity. Neurovascular status should be carefully documented; however neurovascular injuries are rare in isolated intertrochanteric fractures.
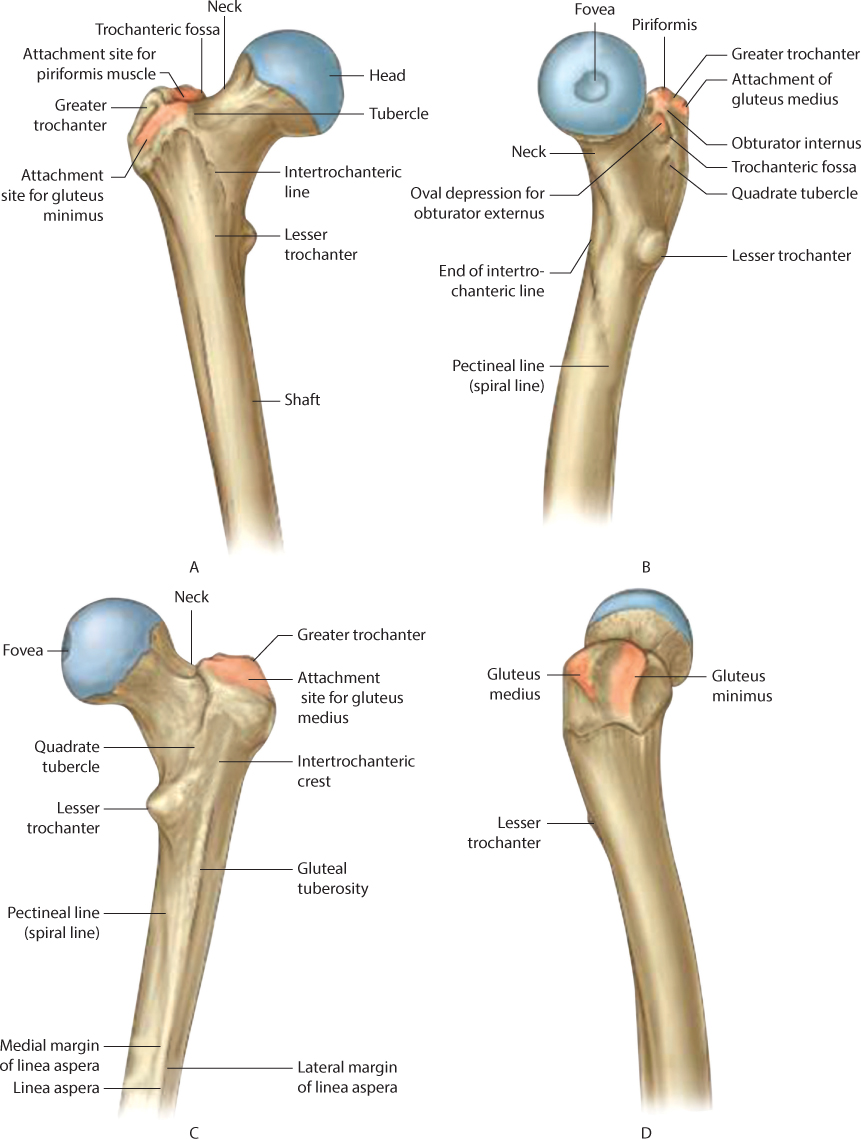
Figure 35.1 Proximal femoral osseous anatomy. (From Drake RL, et al. Gray’s Anatomy for Students. 2nd ed. Philadelphia, PA: Churchill Livingstone/Elsevier; 2009.)
RADIOGRAPHIC ASSESSMENT
Anteroposterior (AP) of the pelvis and AP and lateral views of the affected hip should be obtained in all cases. The contralateral hip on the AP pelvis is used to assist with preoperative planning, allowing the surgeon to ensure implants with appropriate neck-shaft angles are available. In cases where there is concern for subtrochanteric extension or when a long implant is being considered, full-length femur films should be obtained. In the case of suspected fracture with normal X-rays, an MRI should be obtained to assess for nondisplaced fracture.
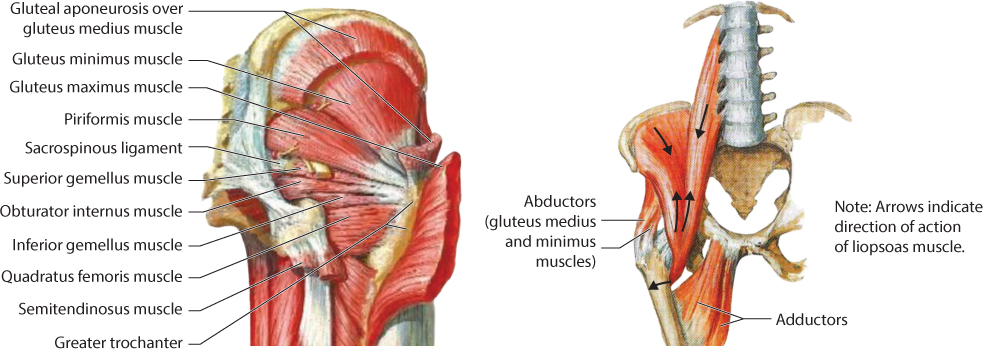
Figure 35.2 Proximal femoral muscular anatomy. Deforming forces affecting alignment of a proximal femoral fracture include the iliopsoas, short external rotators and hip abductors. (From Netter FH. Atlas of Human Anatomy. 4th ed. Philadelphia, PA: Saunders/Elsevier; 2006.)
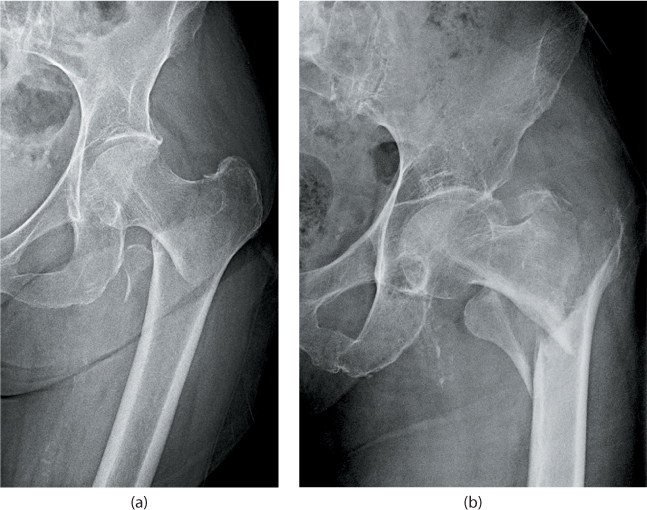
Figure 35.3 Stable (a) and unstable (b) intertrochanteric fracture patterns. Note the minimal involvement of the medial calcar in (a) versus that seen in (b).
Traction-internal rotation views can be obtained to delineate between intertrochanteric and basicervical femoral neck fractures when necessary.
Classification
Most classification systems for intertrochanteric fractures have poor reliability and reproducibility. A simplified system to aid in evaluating treatment algorithms when assessing the literature is based on fracture stability, which is related to the condition of the posteromedial cortex. Fractures are considered stable in the absence of a comminuted posteromedial cortex, reverse obliquity and subtrochanteric extension.
Intertrochanteric fractures are typically classified as stable or unstable. Fractures are generally considered unstable when there is significant involvement of the medial calcar or lateral wall and when a reverse obliquity pattern or subtrochanteric extension is present (Figure 35.3). These fractures may also be classified according to the AO/OTA system (Figure 35.4).5
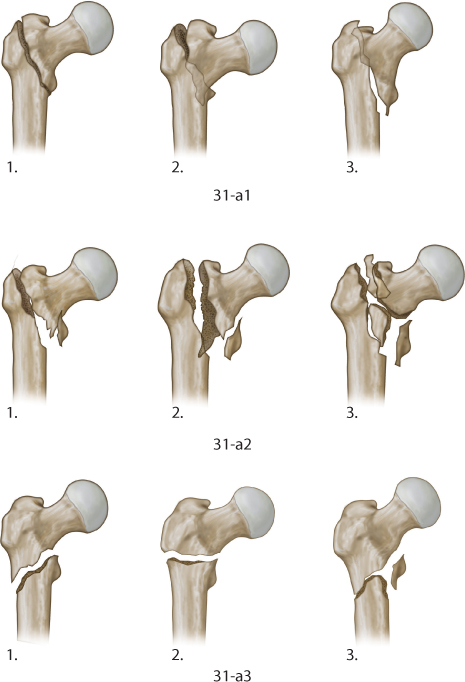
Figure 35.4 AO/OTA classification of intertrochanteric femur fractures. (From Rockwood CA, et al. Rockwood and Green’s Fractures in Adults. 6th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2006.)
Management
NONOPERATIVE
Nonsurgical treatment of intertrochanteric hip fractures is usually reserved for patients with nondisplaced fractures discovered on MRI or comorbidities that place these patients at unacceptable risk from anaesthesia, the surgical procedure or both. Mortality from surgical treatment typically results from cardiopulmonary complications, thromboembolism and sepsis.6
Operative
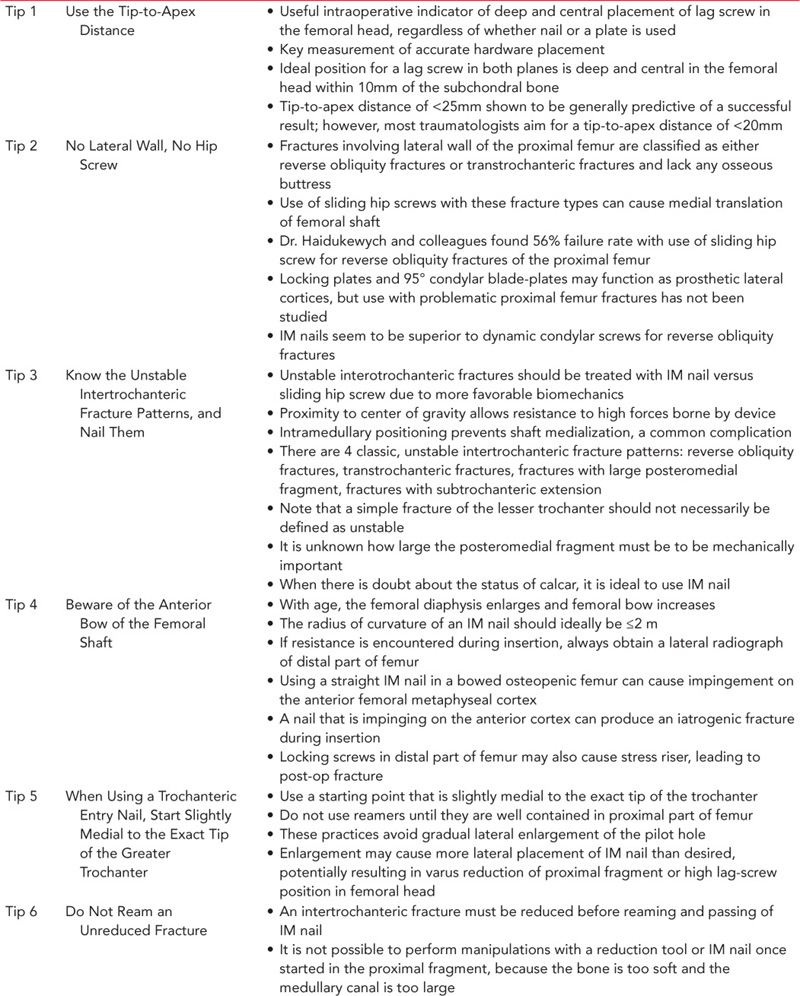
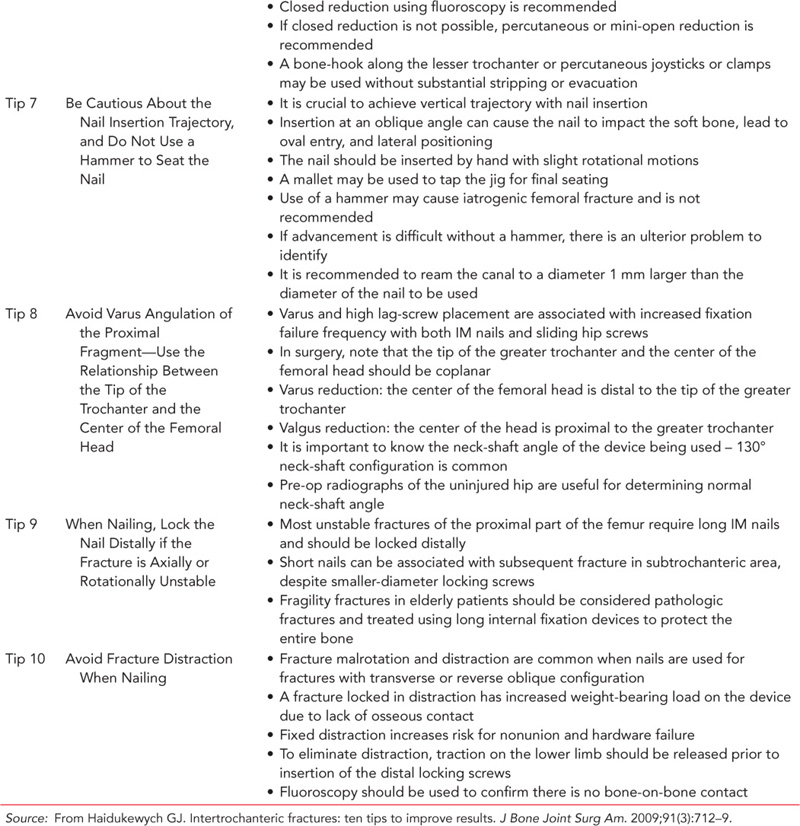
Ten useful tips to consider when fixing intertrochanteric hip fractures are listed in Table 35.1.7
A strong case cannot be made in favor of specific surgical treatments for any type of hip fracture with use of the current randomized trial literature. Patient outcomes associated with different techniques produce only modest differences, if any. Any beneficial effect of one implant class over another appears to reach equivalence within 6 months after surgery. In addition, the literature often does not include important covariates that are essential in order to draw clinically relevant conclusions about the effects of various treatments, given differences in baseline patient characteristics, fracture patterns and provider specific variables that affect treatment quality. The overall strength of the evidence in support of one treatment over another is low. The current randomized trial literature neither sufficiently nor consistently identifies fracture pattern subtypes enough to relate specific fracture patterns to non-mortality outcomes, particularly for intertrochanteric hip fractures. The inconsistency by which surgeons classify the AO/OTA 31A fracture subtypes as stable versus unstable across studies also substantially impedes comparison of results from orthopaedic randomized trials.8
Despite the lack of evidence supporting one fixation method over another, a dramatic change has occurred in surgeon preference for fixation devices, particularly among young orthopaedic surgeons and in training programs.9 A review of the American Board of Orthopaedic Surgery Database found that the use of intramedullary devices increased from 3% in 1999 to 67% in 2006.10 A comparative effectiveness study of Veterans Affairs hospital patients found that intramedullary nail use increased significantly from 1998 to 2005, but did not decrease perioperative mortality or comorbidity compared with standard plate-and-screw constructs. Additionally, this study and others have found wide geographic variation in implant selection.10,11 and 12 Surgeons are clearly selecting implants on the basis of factors other than clinical outcomes evidence. Factors involved may include higher surgeon reimbursement for intramedullary nailing and the fact that surgeon reimbursement remains insulated from the treating hospital’s burden of paying for the higher cost implant under the Medicare payment system.
IMPLANT SELECTION
While some early studies indicated better results with intramedullary nails for unstable fracture patterns,13 more recent randomized trials and case series have failed to clearly define a benefit to utilizing intramedullary nails, reporting similar outcomes with higher costs compared with sliding hip screws.14
The implant decision is sometimes made after positioning the patient and reducing the fracture. Emergency department X-rays are often of suboptimal quality, so verification of the preoperative diagnosis using preoperative traction-internal rotation X-rays or evaluation of the fracture pattern in the operating room with image intensification is sometimes necessary. The stability of the fracture based on the integrity of the lesser trochanter and posteromedial buttress is an important factor. Fractures classified as unstable should be considered for intramedullary nails, whereas stable fractures can be treated adequately with a sliding hip screw. Lateral wall compromise is also critical. It has been found that compromised lateral femoral wall integrity is a significant predictor of reoperation. These patients may not be treated adequately with a sliding hip screw device and may benefit from intramedullary devices.15 If in doubt about the number of parts and stability, a trochanteric stabilization plate can be added to the sliding hip screw or an intramedullary nail device can be utilized.
Table 35.1 Useful tips for fixing intertrochanteric hip fractures
POSITIONING
The patient is positioned supine on the fracture table. The case can also be done on a radiolucent table in select cases (e.g. polytrauma) with or without the addition of a traction arc. The ipsilateral arm is secured across the chest to allow intramedullary nailing if necessary. The injured extremity is placed in traction. The well leg can be placed in either hemilithotomy or scissored position (Figure 35.5).
Prior to prepping and draping, the surgeon must ensure that adequate visualization and reduction can be achieved. Reduction is usually achieved by applying traction to regain length. Excessive traction can lead to pelvic rotation around the perineal post of the fracture table. Next comes internal rotation. The patella should point anteriorly. Abduction/adduction of the hip is then adjusted to ensure the fracture is not in varus. The reduction must be checked in both the AP and lateral with an image intensifier. In case the closed reduction should fail, open reduction will be necessary.
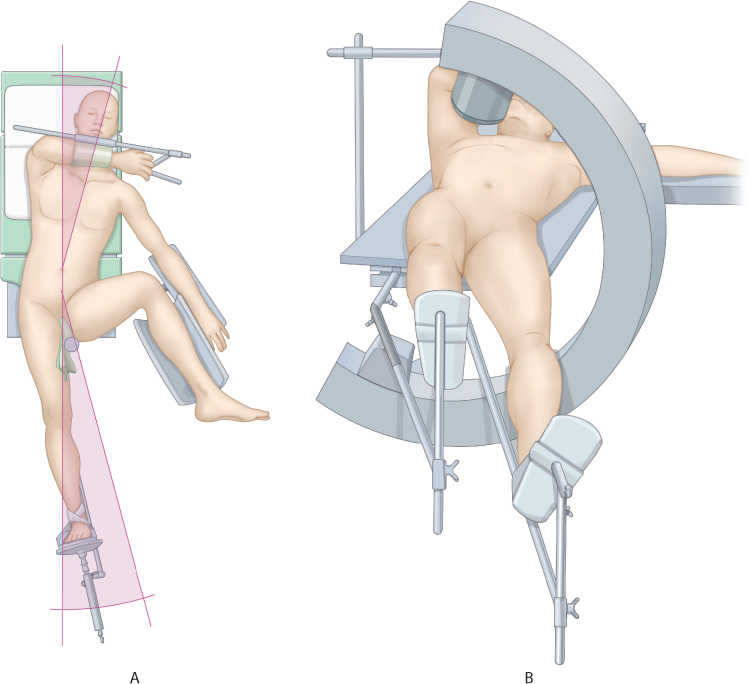
Figure 35.5 Positioning in hemilithotomy (a) and scissored (b). Note in both cases the torso has been shifted to the contralateral side to allow access to the greater trochanter for possible cephalomedullary nailing. (Copyright by AO Foundation, Switzerland. AO Surgery Reference. www.aosurgery.org)
SLIDING HIP SCREW
The lateral approach is used. The incision can be extended proximally to accommodate a trochanteric stabilizing plate. A straight incision is made parallel to the femoral axis. The fascia lata is incised in line with the skin incision and in line with its fibers. The vastus lateralis fascia is incised. The vastus lateralis muscle may be split in line with its fibers or elevated from the posterior leaflet of the fascia and retracted anteriorly. Elevating the vastus lateralis minimizes bleeding. To avoid bleeding, tie off or clip any perforating vessels encountered. A cob elevator is used to expose the footprint of the side plate. Bennett retractors are then placed anterior and posterior to the femur to allow visualization. If necessary for placement of a trochanteric stabilization plate or for open reduction of the fracture, the incision can be extended proximally to the greater trochanter. A pointed reduction clamp can be used to obtain reduction.
Choose the correct aiming device according to the neck-shaft angle as measured from the contralateral hip. Insert the guide wire through the aiming device and advance it into the subchondral bone of the head in a center-center position, stopping 10 mm short of the joint. Position it so that in the AP it is in the caudal half of the neck, and in the axial view in the center of the neck. Determine the length of the sliding hip screw with the help of the measuring device. Select a screw which is 10 mm shorter than the measured length. Adjust the cannulated triple reamer to the chosen length. Drill a hole for the screw and the plate sleeve. The correct screw is mounted on the handle and inserted over the guide wire. Do not push forcefully or you may distract the fracture. In patients with hard bone, it is best to use the tap to precut the thread for the screw. Otherwise the screw may not advance, and you may actually displace the fracture by rotating the proximal fragment as you attempt to insert the screw. The T-handle of the insertion piece should be parallel to the long axis of the bone to ensure the correct position of the plate. It been shown that maintaining tip-apex distance of 25 mm or less prevents screw cutout.15,16 and 17
Place the selected plate and slide it over the guide wire and mate it correctly with the screw. Then push it in over the screw and seat it home with the impactor. Fix the plate to the femoral shaft with an appropriate number and size of plate holding cortical screws. Finally, compression can be achieved by placing the compression screw. If there is concern that the fracture is a transitional type (basicervical), a derotation screw may be added (Figure 35.6).
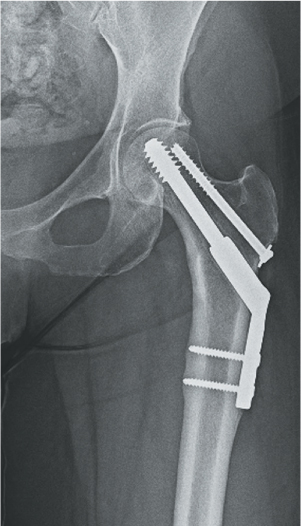
Figure 35.6 Healed intertrochanteric femur fracture. A derotation screw was added as injury was felt to be a transitional variant (intertrochanteric/basicervical femoral neck variant).
CEPHALOMEDULLARY NAILING
It is important to ensure that the ipsilateral greater trochanter is accessible. To accomplish this, rotate the torso 10–15 degrees to the contralateral side when possible. Intramedullary nails for A-type proximal femur fractures enter through the top of the greater trochanter. However, the precise entry point in the greater trochanter depends on the design of the nail.
Make your skin incision in line with the femoral shaft axis and about 5 cm proximal to the tip of the trochanter. Split the fascia in line with the incision. Split the gluteal muscles in line with the fibers. Place the guide wire just lateral to the tip of the greater trochanter on the AP and in line with the middle of the femoral neck on the lateral. Insert the guide wire into the femoral shaft and check its position using the image intensifier. Ideally, the guide wire’s position in the femoral shaft should be central and deviate slightly lateral proximally according to the degree of the lateral bend of the implant in the AP plane. In the lateral view it must be in line with the middle of the femoral neck. Insert the protection sleeve with its trocar over the guide wire and push it through the soft tissues until it abuts against the greater trochanter. Then withdraw the trocar and insert an appropriate drill bit over the guide wire. Ream out the trochanteric area.
Ream by hand or with an awl in osteoporotic patients to avoid damage to the fragile trochanteric metaphyseal bone. In patients with good quality bone, use power reaming. Remove the guide wire after reaming. If the fracture passes through the guidewire entry site, a medially directed force applied to the lateral trochanteric region along with slow advancement of the power reamer helps prevent diastasis of the fracture site by displacing the greater trochanteric segment(s) laterally. This allows proper creation of a channel for the nail, so that its insertion does not distract the fracture and produce varus deformity. Avoiding varus deformity is important to improve fixation and to preserve functionally important anatomy. In most patients the nail, mounted on the insertion device, can be inserted manually. Use the image intensifier as a help and insert the nail to such a depth that it will allow the cephalomedullary fixation to be placed through the middle of the femoral neck.
Mount the aiming arm for the cephalomedullary fixation onto the insertion device. Make a small skin incision at the appropriate place. Insert the drill sleeve assembly through the aiming device and advance it through the soft tissues to the lateral cortex. If you are using a device that takes a column screw, the ideal position of the guide wire in the AP plane is in line with the axis of the neck and slightly in the lower half. In the lateral view it must be in line with the axis of the neck. The guide wire is inserted subchondrally into the femoral head. Its tip should end 5 mm proximal of the joint. Check under image intensification that the femoral neck screw protrudes slightly over the lateral cortex. The cephalomedullary fixation has to be locked with the set screw device. Following this, the compression feature of the device can be used to compress the fracture site. Finally, distal interlocking is performed. With short nails, the radiolucent targeting guide is used. With long nails, distal interlocking screws are inserted using perfect circles techniques through percutaneous incisions (Figure 35.7).
EXTERNAL FIXATION
This technique is useful in special circumstances. A level I prospective randomized study compared pertrochanteric external fixation (PF) with sliding hip screw in 100 consecutive patients. The authors utilized a specially designed Pertrochanteric Fixator (Orthofix, Verona, Italy), which places two threaded half pins into the femoral neck at 110–130 degrees to a subchondral location and two self-drilling half pins into the proximal femur at a 90-degree angle. The authors found that use of PF resulted in significantly less blood loss, shorter operating times, reduced pain, shorter length of stay, earlier mobilization and reduced mechanical complications (P < 0.001). Superficial infection was more common with PF (P < 0.001). No differences were found in healing, mortality or functional outcomes.18
PROSTHETIC REPLACEMENT
Prosthetic hip replacement generally has not been considered a primary treatment option and is usually reserved for revision situations. Unlike femoral neck fractures, which retain some of the femoral neck in addition to the abductor mechanism, intertrochanteric fractures involve more distal femoral bone, and often the greater trochanter and the abductor are not attached to the proximal femur. In this setting, prosthetic replacement requires a more complex surgical procedure with potentially higher morbidity. In the patient with pre-existing symptomatic degenerative arthritis, primary prosthetic replacement may be the best option. It can also be considered for intertrochanteric fractures with severe comminution in severely osteoporotic bone in which internal fixation methods are unlikely to be successful. Calcar-replacing implants are typically required.
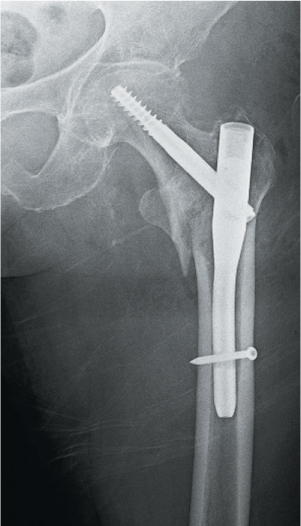
Figure 35.7 Unstable intertrochanteric fracture from the patient in Figure 35.3 stabilized with a short cephalomedullary nail.
A randomized prospective level I study of unstable intertrochanteric fractures in elderly patients comparing long-stem cementless calcar-replacement hemiarthroplasty with a proximal femoral nail (PFN) found no significant differences between the two groups in terms of functional outcomes, hospital stay, time to weight bearing or risk of complications. However, surgical time, blood loss, need for blood transfusions and mortality rates were all significantly lower in the PFN group.19
In another level I study, hemiarthroplasty was compared with the sliding hip screw. No significant difference was found between surgical time, wound complications or mortality rates. However, the hemiarthroplasty group was reported to have higher transfusion rates.20
Special circumstances
NONDISPLACED FRACTURES
As in the case of nondisplaced femoral neck fractures, nondisplaced intertrochanteric fractures are best identified using MRI. Once discovered, treatment is controversial, as patients have been treated successfully with both operative and nonoperative approaches (Figure 35.8).
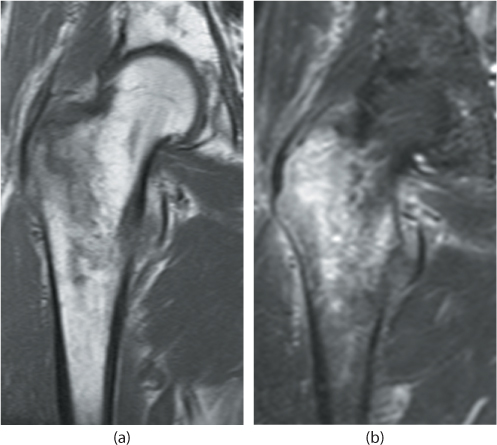
Figure 35.8 T1 (a) and STIR (b) MRI images of a nondisplaced intertrochanteric femur fracture.
REVERSE OBLIQUITY AND TRANSVERSE FRACTURES
These are true intertrochanteric fractures. They are classified according to the fracture pattern. The fracture line passes between the greater and lesser trochanters, above the lesser trochanter medially and below the crest of the vastus lateralis laterally (Figure 35.9).
Reverse oblique fractures often have a typical displacement because of the pull of the abductors, which abducts and flexes the proximal fragment. Be careful in determining the distal extension of the fracture line as nondisplaced fracture lines can propagate distally into the femoral shaft.
Although some studies suggest that these fractures can be treated effectively with sliding hip screws,21 and some studies have reported similar failure rates with sliding hip screws and intramedullary nails,22 other studies have reported failure rates of up to 80% when these fracture patterns are treated with sliding hip screws.23 Although a biomechanical study demonstrated that with anatomic reduction and bone contact a 135-degree hip screw, 95-degree hip screw and intramedullary hip screw performed equally, when a gap was created, the intramedullary hip screw was significantly stiffer with a greater load to failure than the other two implants.24 Also, a randomized prospective study comparing intramedullary nails and 95-degree hip screws found that patients treated with intramedullary nails had shorter operative times, fewer blood transfusions and shorter hospital stays with significantly fewer implant failures and non-unions compared to those treated with the 95-degree hip screw.25 Several other studies have demonstrated excellent results with low complication rates when these fractures are treated with cephalomedullary devices.26
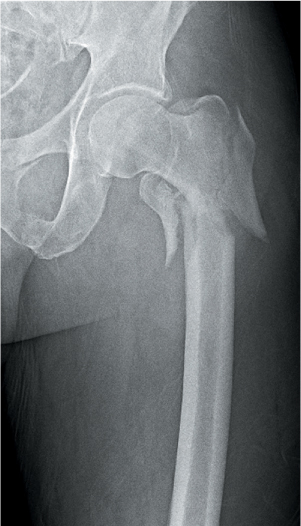
Figure 35.9 Reverse oblique intertrochanteric femur fracture.
Postoperative management
Although surgeons make decisions regarding weight bearing on a case-by-case basis, overall the literature supports immediate weight bearing after internal fixation of appropriately selected extracapsular hip fractures. Immediate weight bearing has demonstrated benefits in patient balance and mobility, which may decrease morbidity and promote greater independence. Patients without dementia can safely be advised to bear weight as tolerated after operative treatment of intertrochanteric femur fractures. Computerized weight bearing and gait analysis has demonstrated that these patients will autoregulate and voluntarily limit loading of the injured limb.27
Koval et al. reported the outcomes of a large cohort of elderly patients who were allowed to bear weight immediately and followed for ≥1 year. The authors reported on 208 patients who had stable or unstable intertrochanteric femur fractures, all of which were managed with sliding hip screws. The rate of revision for loss of fixation was 2.9%, in all cases because of femoral head lag screw cut-out.28 Herrera et al. reported on 551 intertrochanteric femur fractures in elderly patients (average age 82.8 years) who were treated with a short cephalomedullary nail and allowed to bear weight immediately after the procedure. The authors reported a 1.4% rate of screw cutout and a 4% rate of collapse into secondary varus >10 degrees at final follow-up.29
COMPLICATIONS
Maintaining a tip-apex distance of 25 mm or less can prevent screw cutout.17 It has been found that, after adjusting for tip-apex distance and screw position, A3 fractures are at more risk for cutout than A1 fractures.16 Helical blades have also been found to cutout of the femoral head at a low rate.30 Compromised lateral femoral wall integrity has been found to be a significant predictor of reoperation in patients treated with sliding hip screw devices.15 There have also been several reports of helical blade advancement into the pelvis.31 Breakage of cephalomedullary nails at the lag screw site has also been reported (Figure 35.10).
SALVAGE
Most intertrochanteric hip fracture nonunions occur in older patients with poor proximal bone quality and fail by implant cutout from the femoral head. The decision to perform revision internal fixation versus prosthetic replacement is based on patient characteristics, fracture pattern, remaining bone quality and status of the hip joint. Arthroplasty has been found to be an effective salvage procedure with most patients experiencing good pain relief and functional improvement and a low complication rate. Arthroplasty allows earlier patient mobilization and is thus advantageous for rehabilitation (Figure 35.11).32
When hip arthroplasty is performed for salvage of failed intertrochanteric fractures, specific technical considerations must be addressed. The initial decision is whether to perform a total hip arthroplasty or a hemiarthroplasty. It is not uncommon for the cutout of the previous internal fixation to cause secondary damage to the hip joint. Usually, in this circumstance or in patients with markedly severe pre-existing arthritis, a total hip arthroplasty is performed. With well-preserved articular cartilage, hemiarthroplasty may be considered. The same advantages and disadvantages of hemiarthroplasty versus total hip arthroplasty discussed for salvage of femoral neck nonunion also pertain to intertrochanteric nonunion.
Defects from previous internal fixation devices on the lateral femoral shaft create stress risers that can lead to intraoperative fracture of the femur, particularly with torsion. Preliminary dislocation of the hip before hardware is removed may reduce femur fracture risk in these hips, which often are quite stiff and can require much force to dislocate. Frequently, broken screws are present.
Most patients with failed intertrochanteric fracture fixation have bone loss below the standard resection level for a routine, primary total hip arthroplasty. Therefore, many need a calcar-replacing implant to restore leg length and hip stability. To prevent the chance of subsequent fracture when using longer stems, it is considered wise to bypass screw holes in the femur by two cortical diameters. Additionally, it has been found that arthroplasty following failed fixation with intramedullary implants leads to a high risk of greater trochanteric fracture and nonunion.33 Successful femoral component fixation can be obtained with either cemented or cementless implants.
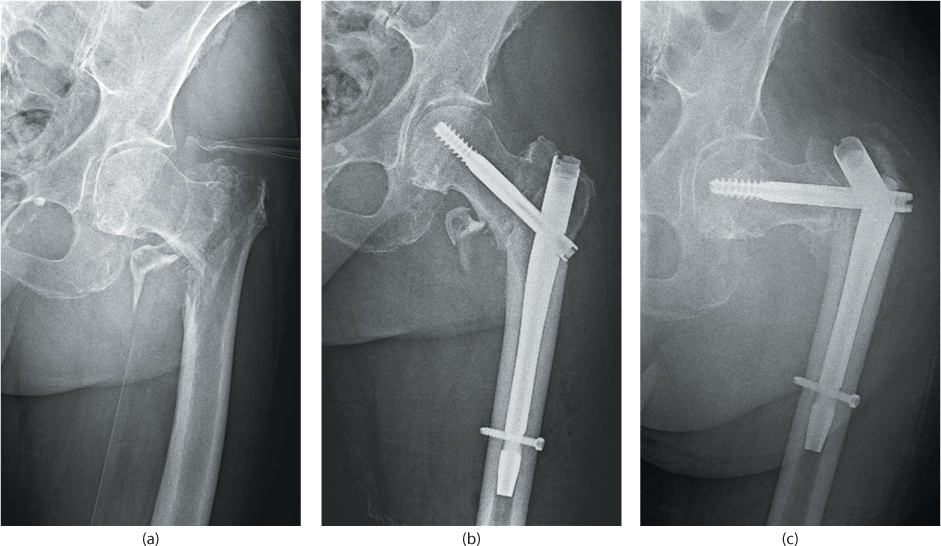
Figure 35.10 Unstable intertrochanteric femur fracture (a) fixed with cephalomedullary nail (b) which went on to failure (c).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








