Direct Anterior Primary Total Hip Arthroplasty
Wadih Y. Matar and William J. Hozack
Key Points
• Setup in the supine position is easy.
• The DA approach allows for intraoperative hip stability and accurate leg length measurements.
Introduction
Total hip arthroplasty (THA) can be performed through various approaches to the hip. The direct anterior (DA) approach has recently gained some popularity because it provides a safe approach to the hip joint with the advantage of being intermuscular without abductor muscle disruption, and it can allow for patients’ early mobilization and fast recovery. Critics of the DA approach argue that the specialized table (e.g., Judet traction table) advocated as a means of performing this procedure is awkward and expensive and can lengthen operative time. We present here the direct anterior approach performed in the supine position but on a regular operative table. Advantages of performing THA through the DA approach in this manner (on a regular table) include easier setup time compared with the lateral position, lack of need for a specialized table, and an easy way to check for intraoperative hip stability and leg length discrepancy compared with the DA approach with a traction table.
Smith-Petersen was the first to describe the anterior approach to the hip in 1917 for congenital hip reduction, and subsequently in 1949, when he used the approach for mold arthroplasty.1,2 The incision spanned from the middle of the iliac crest to the anterior superior iliac spine (ASIS) and then deviated slightly laterally along the medial border of the tensor fascia lata (TFL). Distally, the interval between the sartorius and the TFL is used, whereas proximally, the interval between the abdominal and gluteal muscles is developed down to bone, resulting in medial reflection of the abdominal muscles, the sartorius, and Poupart’s ligament, and lateral reflection of the gluteus medius, the gluteus minimus, and the TFL. Smith-Petersen also advocated that motor nerve fibers to the rectus femoris originating from the femoral nerve must always be exposed before the rectus muscle and the acetabular origin of the iliacus muscle are incised. Finally, the approach also included an osteotomy of the anterior inferior iliac spine (AIIS) and the anterior acetabular wall.
This classic approach has been modified over the years by many surgeons.3–8 These variations have revolved around the location and length of the incision, as well as handling of the TFL.8 In France, Judet and Judet (1950) used a similar approach credited to Hueter to perform hip arthroplasty using a polymethylmethacrylate prosthesis.5 In contrast to the Smith-Petersen approach, Judet and Judet used a traction table, allowing hip dislocation with traction, extension, and external rotation of the hip. Surgically, this approach included only the lower half of the Smith-Petersen approach and was vertical from the ASIS, passing between the TFL and sartorius muscles. Unlike the traditional Smith-Petersen approach, which detached the TFL from the iliac crest, Hueter’s approach left the insertion of this muscle intact and allowed access to the hip by retraction of this muscle laterally.
During the latter part of the 20th century, the DA approach regained popularity among arthroplasty surgeons as they looked for tissue-sparing incisions that provided a safe way to perform THA with little muscle or tendon disruption.9–11 The contemporary DA approach most resembles that described by Hueter. However, as surgeons became more comfortable with the approach, specialized retractors were developed, allowing the incision size to be decreased from the classic 15 cm to 6 to 8 cm.12 The smaller incision is more aesthetically appealing to the patient; however, it is important to note that the underlying dissection remains the same as one would expect with a larger incision, and that, if needed, surgeons should not hesitate to enlarge the incision if exposure is compromised by the smaller incision. That being stated, the DA approach remains an acceptable tissue-sparing approach to THA.
Indications and Contraindications
All patients scheduled for THA according to its classic indications are candidates to undergo their replacement via the DA approach. The easiest patient from a technical standpoint is one who is thin, flexible, and nonmuscular with good bone quality and femoral head offset. It is imperative that the surgeon have expertise with hip replacement, along with different approaches to the hip, and that he or she can work with a knowledgeable and dedicated team to avoid unnecessary complications. Of course, this is true of all surgical procedures.
Few absolute contraindications are known; they include skin irritation or active infection over the incision site, abnormal proximal femoral anatomy requiring correction, and retained hardware that needs removal via the lateral approach. Lack of availability of specialized instruments should be considered as a relative contraindication, because the DA approach is performed more easily and less traumatically with the help of these instruments.12–15 Patients with a high body mass index (BMI) should be evaluated individually because it may be significantly easier to perform THA through a DA approach. The depth of adipose tissue is significantly less anteriorly as compared with lateral or posterior locations, especially in female patients. Roue and associates prospectively compared two groups of patients: one with BMI less than 25, and the second with BMI of 25 or greater, who underwent THA through a 7-cm DA incision with the use of a Judet traction table.16 Results showed that bleeding and operative time correlated with BMI, and that incision extension and abrasions were noted in the group with BMI of 25 or greater, possibly owing to stronger traction and reamer injury. Socket position was unaffected by BMI, and the authors did not find a higher complication rate related to skin breakdown or infection in the group with BMI greater than 25. Our only concern is the obese patient with abdominal tissue that overhangs the incision area, which may affect wound healing in these patients. Muscular patients pose the biggest technical challenge for the DA approach to THA (but this is true for the other approaches as well). Surgeons should start with a longer incision and should decrease its length as they become more comfortable with the approach, to a length that allows the surgery to be carried out safely.
Preoperative Planning
Preoperative workup of patients undergoing THA through the DA approach is similar to the workup conducted for a standard THA. Preoperative clinical evaluation consists of an examination for range of motion (ROM), abductor strength, and leg length, and complete neurovascular evaluation of both lower extremities. The patient’s body habitus should be considered because central obesity around the abdomen can render the procedure more difficult during femoral canal preparation. On the other hand, increased adipose tissue around the thighs can affect the lateral and posterior approach to the hip but not necessarily the DA approach, prompting the surgeon to favor this approach.
Preoperative radiographs include an anteroposterior (AP) view of the pelvis showing both hips and the proximal two thirds of the femur, along with a cross-table or a frog-leg lateral of the affected hip. Radiographs are examined for proximal femur anatomic abnormalities. Femoral offset should be evaluated carefully because decreased femoral offset or significant femoral retroversion can increase the technical difficulty of the DA approach. Preoperative templating is done in similar fashion to that carried out for a standard THA (Fig. 17-1). We are currently using relatively short femoral implants that require no reaming and have a recessed lateral shoulder, which makes their insertion through the DA approach easier.
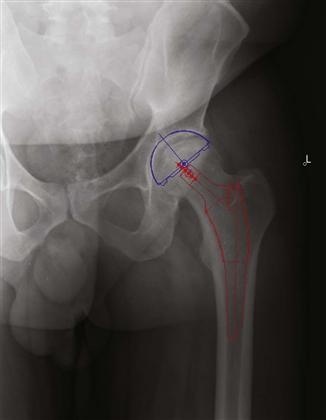
Figure 17-1 Preoperative anteroposterior (AP) view of a left hip after templating. The AP view is examined for appropriate implant fit, and the level of resection should be marked out. The varus/valgus angle should be chosen to closely match normal anatomy and reestablish the patient’s femoral head offset. The acetabular implant is positioned at 45 degrees of abduction against the medial wall at the level of the teardrop.
Operative Technique
The patient is placed in the supine position on a regular operative table with care taken to ensure that all bony prominences of the upper extremity are well padded. The supine position places the pelvis in a neutral position, facilitating cup placement, and permits more accurate intraoperative evaluation of hip stability and leg length. An additional arm board is placed longitudinally on the nonoperative lower aspect of the table, allowing abduction of the contralateral side and adduction of the operative side during femoral preparation. A 1-inch-high rectangular bump is placed under the pelvis, and the hip is positioned along the axis of flexion of the operative table. Before proceeding, the surgeon should verify that table flexion results in proper hip extension because this is helpful during femoral preparation. The limb is then prepped and draped to include the lower abdominal quadrant of the operative side.
The hip is approached through a 10- to 12-cm straight incision starting approximately 3 cm laterally and 3 cm distally to the ASIS; the starting point of this incision is approximately halfway between the ASIS and the greater trochanter (Fig. 17-2). The ASIS is easily identified from distal to proximal to avoid placing the incision too proximal. The incision is centered over the TFL and is directed laterally toward the lateral aspect of the distal femur. The placement of this incision makes it more lateral than the classic incision described by Smith-Peterson. Incision length can be increased as needed: Proximal extension improves femoral exposure, and distal extension facilitates acetabular exposure. Superficial dissection is then carried down to the fascia covering the TFL. The surgeon should properly identify the TFL to avoid injury to the lateral femoral cutaneous nerve (LFCN). This can be carried out by feeling for the muscle belly of the TFL between the surgeon’s two thumbs. Also, the fascia covering the TFL is thicker and whiter medially along the interval between the TFL and the sartorius. Finally, this fascia is usually perforated by several blood vessels coming from lateral to medial. These vessels should be identified and cauterized before proceeding (Fig. 17-3).
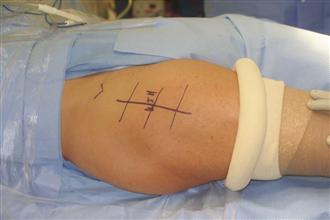
Figure 17-2 Starting 3 cm laterally and 3 cm distally to the anterior superior iliac spine (ASIS), a 10- to 12-cm straight incision is centered over the tensor fascia lata (TFL) and is directed in an oblique fashion laterally toward the lateral aspect of the distal femur.
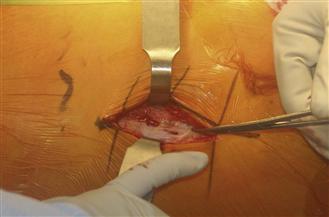
Figure 17-3 Perforating vessels (held with hemostat) through the fascia covering the tensor fascia lata (TFL). These vessels can be used to identify the TFL and are usually oriented from lateral to medial.
To avoid injury to the LCFN, which lies on the sartorius muscle, the fascia overlying the TFL is incised longitudinally along its fibers at a distance 1 cm lateral to the TFL/sartorius interval represented by the thicker and whiter fascia medially. The medial fascial flap is then separated from the underlying fibers of the TFL in a parallel fashion to the muscle fibers (Fig. 17-4). A subfascial exposure is performed by retracting the fibers of the TFL laterally to expose adipose tissue that is covered by a thin layer of deeper fascia overlying the vastus muscles. The surgeon then may use his index finger to find the space proximal to the neck of the femur superior to the hip capsule at the proximal end of the incision; the first narrow blunt Cobra superior retractor is introduced into that space and is used to retract the gluteus minimus and the superior part of the TFL muscle. A second sharp Hohmann lateral retractor is introduced lateral to the greater tuberosity through the lateral intramuscular septum and is used to retract the TFL muscle fibers laterally. The sartorius muscle is retracted medially with a Hibbs retractor to expose the deep thin fascia. Cautery is then used in a superficial fashion to release the fascia; the fascial release can be extended over the rectus femoris to improve visualization distally. Caution should be taken to avoid penetration of the underlying pericapsular fat with the cautery, because this area contains the ascending branches of the lateral circumflex vessels (Fig. 17-5). These should be dissected from the surrounding fat and cauterized individually before proceeding. After homeostasis is achieved, the remaining pericapsular adipose tissue may be removed with a rongeur, exposing the anterior hip capsule.
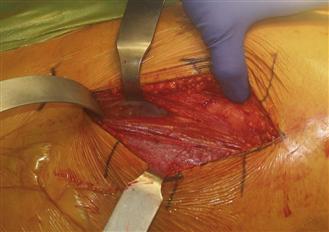
Figure 17-4 The fascia of the tensor fascia lata (TFL) is incised longitudinally 1 to 2 cm lateral to the TFL/sartorius interval, and the muscle fibers are retracted laterally to expose the deeper fascia covering the rectus femoris and vastus medialis muscles.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








