PATHOPHYSIOLOGY
Normal Skin
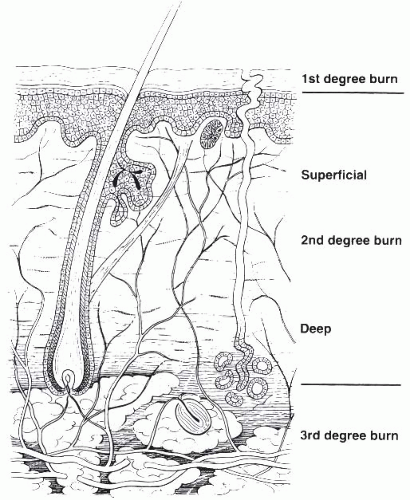
The skin is the largest organ of the body. It serves multiple functions; it acts as a protective barrier to the external environment, regulates temperature and fluid homeostasis, plays a key role in sensation, and contributes to our sense of identity and communication. Skin is a complex organ composed of two layers, the epidermis and dermis (
Fig. 43-2).
The outermost epidermis consists of stratified squamous epithelium. This layer contains no blood vessels and the cells are nourished by diffusion from capillaries in the upper layers of the dermis. Cells are formed through mitosis at the basal layer (stratum basale). In addition to forming the bottom layer of the epidermis, the stratum basale lines the hair follicles and sweat glands. (Hair follicles and sweat glands are a source of epidermal cells that enable partial thickness burn injuries to heal spontaneously.) The mitotic daughter cells migrate toward the surface changing shape and composition as they die due to isolation from their blood source. The cytoplasm is released and the protein keratin is inserted. They eventually reach the outer layer and desqaumate. This process is called keratinization and takes approximately 30 days. This keratinized layer of skin (stratum corneum) is responsible for keeping water in the body and keeping harmful chemicals and pathogens outside the body, making skin a natural protective barrier.
The dermis resides beneath the epidermis and consists of a vascular connective tissue that supports and provides nutrition to the epidermis and skin appendages. The dermis contains nerve endings, capillaries, lymphatic vessels as well as appendages that include hair follicles, sweat glands, and sebaceous glands. The eccrine sweat glands release heat from the body’s surface though sweat, thereby contributing to thermoregulation. The sebaceous glands secrete an oily substance called sebum that protects the skin and hair and moisturizes the skin.
Classification of Burn Injury
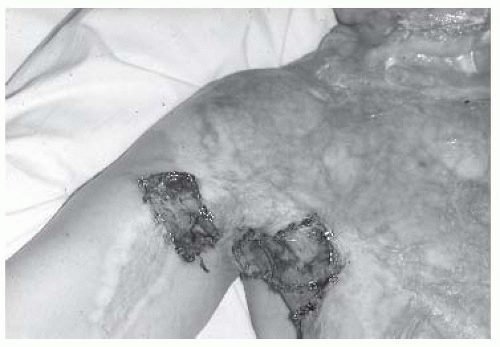
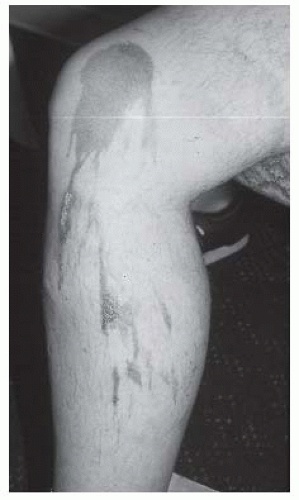
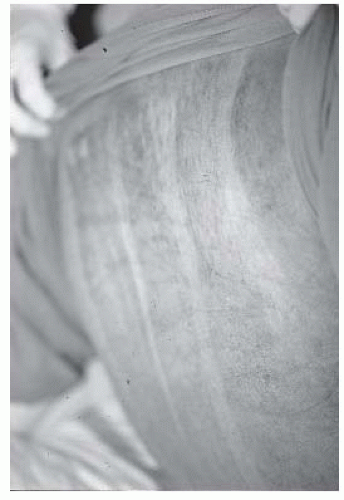
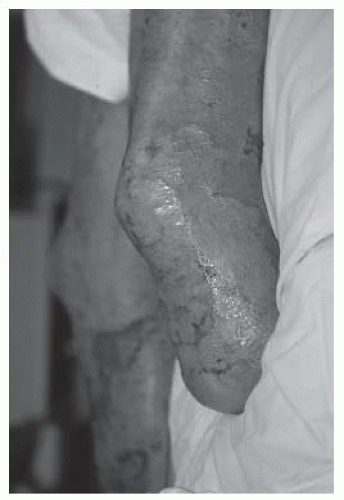
One of the most common classification systems uses depth of injury to categorize the severity of the burn. Superficial injuries, previously termed first-degree burns, solely affect the epidermis. The category of second-degree burns is now divided into superficial and deep partial thickness burns. The former interrupt the epidermis and superficial dermis and present with blistering, moist and painful skin that blanches with
pressure. The latter involve the epidermis and deep dermis, including skin appendages, affecting some degree of sensory and sweat gland function. Deep partial thickness burns present with a dry or waxy appearance and are less painful than more superficial burns. Full thickness burns, formerly third-degree burns, affect the entire epidermal and dermal layers and result in complete loss of skin appendages. They present as white waxy to leathery gray to charred black appearance, are insensate to pain, and do not blanch to pressure. Deep injuries may affect muscle, tendon, and bone. Such deep injuries are not part of the newer classification system, but were previously classified as fourth-degree burns (see
Fig. 43-2;
Table 43-1).
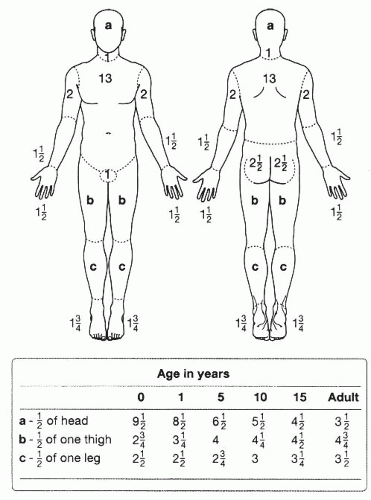
Burn injuries are also classified by size. Lund and Browder (
8) diagrams provide a systematic method for calculating total body surface area (TBSA) burned for both adults and children. In contrast to an adult, a child’s head represents proportionally more and their legs represent proportionally less of their body surface area (
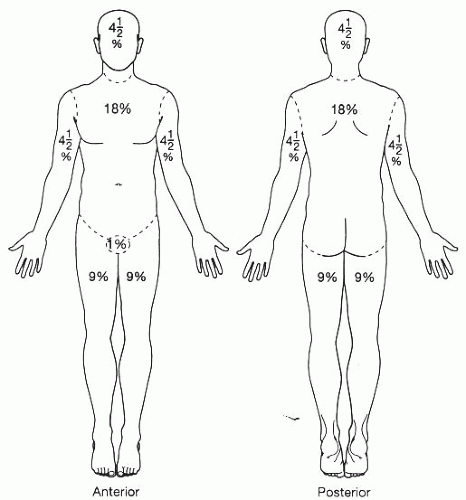
Fig. 43-3). The rule of nines is used clinically as a quick estimate of TBSA (
Fig. 43-4).
Many burn injuries are best treated in specialized burn centers. The American Burn Association in consultation with the American College of Surgeons has developed clinical criteria for referral to a burn center (
9) (
Table 43-2).
Effects of Thermal Injury
In thermal injury, the extent of tissue damage is related to the location, duration, and intensity (temperature) of heat exposure. Also of significance, those at the extremes of age have fewer protective layers of epithelium; therefore the same location, duration, and intensity of heat will produce a more serious burn injury in children and elderly than in other adults.
After burn injury a cascade of physiologic processes affect the thermal injuries ultimate impact. There is a complex interplay of local and circulating mediators, including histamine, prostaglandins, thromboxane, kinins, serotonin, catecholemines, oxygen free radicals, platelet aggregation factors, angiotensin II, and vasopression. Initially, there is vasoconstriction at the site of injury mediated by release of norepinepherine and serotonin. A few hours after injury vasoconstriction turns to vasodilation, increased capillary permeability, and leakage of plasma into the extravascular space. Histamine is released. Damaged cells swell. Fluid shifts result in increased extravascular edema and intravascular hypovolemia. Platelets and leukocytes aggregate, leading to thrombotic ischemia (
10,
11). In severe burn injuries, inflammatory mediators are released and compromise cardiovascular function. Burn shock ensues, resulting in decreased intravascular volume, increased systemic vascular resistance, decreased cardiac output, end-organ ischemia, and metabolic acidosis. Resuscitation treatment helps reverse this potentially deadly cascade.
Damaged skin results in impairment in most major functions of the integumentary system. In areas of burn injury, skin loses its ability to act as a protective barrier and homeostatic regulator. This may lead to significant losses of body fluid, impaired thermoregulation, and increased susceptibility to infection. In large burns, loss of fluid by evaporation contributes to the development of hypovolemia and shock.
Release of catecholemines plays a key role in the development of a catabolic state after burn injury. Tachycardia, increased nutritional demand and weight loss typically ensue. Gastric dilation and gastrointestinal ileus are common in the first few days after burn injury. Also, immune function is impaired. The arachidonic acid and cytokine cascades alter the function of lymphocytes, macrophages, and neutrophils. As a result, patients are at increased risk of infection. Inhalation injury is commonly associated with fire injuries. Noxious gaseous components of smoke directly damage the respiratory tract. Patients are at risk for carbon monoxide intoxication, upper airway edema and obstruction, pneumonia, and dependence on mechanical ventilation (
11,
12).
Skin Regeneration and Scarring
Spontaneous reepithelialization is impossible with a full-thickness burn injury because of destruction of the dermal appendages. Full-thickness burns result in hair loss, sensory impairment, loss of normal skin lubrication, and heat intolerance because of destruction of sweat glands.
Healing and regeneration of skin in partial-thickness burns arise from the epithelial linings of the hair follicles and sweat glands (stratum basale). Depending on the depth, healing is completed within 14 to 21 days. The new skin again functions as a temperature regulator and a protective barrier against bacteria. After epithelialization there is continued healing with regeneration of the peripheral nerves, sometimes associated with symptoms of neuropathic pain and itching. Although epithelium covers the wound, dermal scarring occurs in the burn wound on a continuous basis for several months after injury. The healing process is ongoing from 6 months to 2 years until the skin is mature. By that point the vascularity of the wound has returned to near normal, and there is no further collagen deposition in the wound.
ACUTE MEDICAL MANAGEMENT
Acute Care of Burn Wounds
While the long-term goals of burn wound care are to restore skin integrity, function, and appearance, the immediate goals post resuscitation are to prevent infection, decrease pain, prepare wounds for grafting, prevent contracture and scarring, and maintain strength and function.
Debridement, the removal of eschar and necrotic tissue, prepares a viable base for wound healing and grafting. Eschar is a composite of coagulum and other tissue debris. Like necrotic tissue, eschar provides an excellent environment for bacterial growth. Since eschar has no microcirculation, bacterial invasion cannot be resolved with systemic antibiotics.
Debridement is performed by several methods. Water immersion, water spray, and wet to dry dressing are examples of mechanical debridement. Commercially available topical enzymes are available for debridement and include substances such as sutilains that induce proteolysis, fibrinolysis, and collagenolysis.
There are different types of surgical debridement. Sequential, also called tangential, debridement is the process of removing thin slices of necrotic tissue. Tissue is removed until a viable tissue bed is reached. Fascial debridement surgically removes tissue down to fascia. In this type, a viable wound bed is assured but a significant soft-tissue defect results. Circumferential fascial debridement places patients at high risk for chronic edema.
Deep skin burns are inelastic and the injured skin does not accommodate to the massive edema associated with acute burn injury. In a circumferential burn, the inelastic tissue acts as a tourniquet. The tourniquet effect can lead to a compartment syndrome, defined as compartmental pressure of atleast 40 mm Hg. If this occurs, escharotomy is indicated. Escharotomy, surgical decompression of the compartment, is urgently performed to avoid necrosis of the underlying tissues that results from sustained elevated pressure. Escharotomy incisions are performed along the medial and lateral aspects of the extremity. This procedure is critical in situations involving full-thickness circumferential injuries of the chest, arms, or legs. If escharotomy does not successfully reduce the elevated pressure, a fasciotomy is indicated.
Grafting
The introduction of early excision and grafting in the last 40 years has contributed significantly to decreased length of hospitalization as well as improved survival rates, cosmesis, and functional outcome.
Homografts, tissue taken from one’s own species, include cadaveric tissue and human fetal membranes. Heterografts, also known as xenografts, are tissues taken from nonhuman species that are used as human grafts. These biological tissues, most commonly porcine tissues, provide wound closure, modulate metabolic needs, and reduce evaporative fluid. These temporary grafts also act as a mechanical barrier to infection and aid pain relief. Temporary grafts are useful as “test grafts” to determine if the wound bed will accept an autograft. Typically, homografts and heterografts are removed or replaced after several days because the patient’s immune system rejects them. It is not routine to use immunosuppressant therapy in conjunction with grafting.
Synthetic wound dressings are available, including polyvinylchloride, polyurethanes, and other plastic membranes. They are vapor and gas permeable. Such grafts are employed until autografting is feasible or the wound heals. Bilaminate analogs composed of thin sheets of silastic as well as epidermal and dermal components are available. Biobrane and Integra are the two most common biosynthetic dressings.
In the world of skin substitutes and biologic dressings, autografts are the gold standard. The bioengineered substitutes can be used as a temporary covering prior to autografting, or as a neodermal base on which the autograft is placed.
Pham, in a recent evidence-based literature review of bioengineered skin substitutes, concluded that Biobrane, TransCyte, Dermagraft, and allogeneic cultured skin are at least as safe and effective as other wound dressings or allografts for partial thickness wounds. The authors concluded that Integra is best used for smaller burns; evidence suggests that burns of 45% or greater experienced higher infection rates. TransCyte provides good coverage in areas of high contour such as the face (
13).
Autografts are harvested from the patient’s own skin. In this process, skin is surgically removed from one’s own body and is relocated to another site (grafted) (
Figs. 43-5 and
43-6). Autografts are placed on a wound bed clean of any nonvital tissue or debris and without evidence of infection.
Split thickness grafts are applied in sheets or may be meshed prior to application. Cutting small regularly staggered parallel slits in the sheet of harvested skin creates a meshed skin graft. This expands the size of the graft to several times its original surface area. Meshed grafts are less cosmetic than full-thickness grafts. Meshed grafts heal quickly, and the epithelialization that occurs in the interstices creates a meshlike appearance to the healed skin (
Fig. 43-7).
Full-thickness skin grafts are not meshed and result in a more cosmetic appearance. They are typically applied to cosmetically critical areas such as the face, neck, and hands. In addition, full-thickness grafts are used almost exclusively in reconstructive surgery.
Dysphagia
Dysphagia is a common problem with large burn injuries and complicates the delivery of adequate nutrition for healing and recovery. Burn induced hypermetabolism increases the caloric needs of the patient. Weakness, inhalation injury, tracheostomy, medication, oral motor dysfunction, and multiple other factors contribute to the development of dysphagia. Tracheostomy is associated with aspiration, pneumonia, and the development of tracheal-esophageal fistulae. Vocal cord paresis is associated with inhalation injury and endotracheal intubation.
Vigilant monitoring is required to recognize dysphagia early and prevent aspiration and associated morbidity. Edelman et al. (
14) demonstrated the importance of evaluating patients swallowing function.
In this study, dysphagia was initially assessed by bedside swallowing evaluation, and, if abnormal, followed by modified barium swallow examination. They found that oral phase dysphagia is usually due to impaired range of motion (ROM), weak mastication, and impaired oral seal from burn wounds or scar formation. Esophageal dysfunction is a secondary complication of intubation or tracheostomy. Pharyngeal phase dysphagia is usually a result of inhalation injury, complications of tracheostomy, intubation, or burn scar. Pharyngeal dysphagia is associated with the highest risk of aspiration.
Interventions include evaluating endotracheal tube position, size, and location. Selection of appropriate food consistency and positioning, including head and neck positioning, are successful measures to reduce the risk of aspiration.
REHABILITATION
Restoration of independent function is the ultimate goal of rehabilitation. Functional restoration includes all aspects of the human life such as strength, ROM, mobility and self-care, reintegration into family and community, adaptive psychosocial responses, and self-determination.
Rehabilitation after a severe burn injury is a multistage process that may take years. Acute rehabilitation goals include interventions to facilitate wound healing, achieve pain
control, prevent joint contracture and weakness, and promote independent mobility and activities of daily living (ADL). Details of the injury, age, premorbid functional level, and health are determinants of an individual’s rehabilitation plan. Therapy is individualized according to burn location, depth, and size as well as other associated injuries or complications. Successful rehabilitation involves multiple disciplines working collaboratively with the patient to achieve the highest level of functioning possible.
Positioning
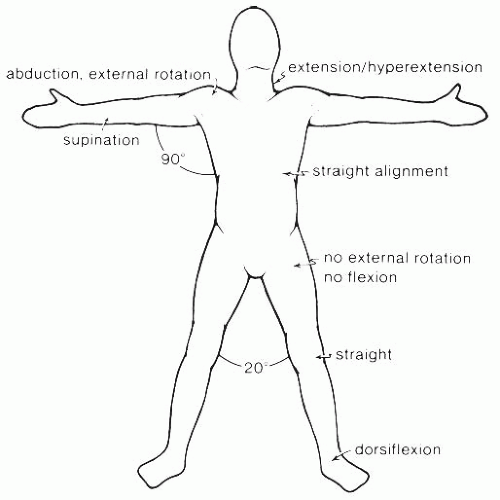
Contractures are a common complication of deep partial and full-thickness burn injuries. Proper positioning is a basic tenet of contracture prevention. Proper positioning also helps prevent other complications such as pressure ulcers and compression neuropathies (
Fig. 43-8;
Table 43-3).
Contracture prevention is based on the principle of tissue elongation. Patients often prefer to position injured tissue in a shortened, nonstretched state for comfort. Typically, this is a position of flexion and adduction. Such positions of comfort lead to contracture. Positions of extension and abduction are usually indicated to counter the position of comfort. One must prescribe positioning in accord with the location of the injury and direction of the contracture. Joints with overlying deep burns are placed in a position of tissue elongation. For example, a deep burn of the elbow is kept in extension to avoid a flexion contracture that would impede reaching.
Contractures are not limited to joints. Other areas, such as the soft tissue of the lips and mouth, require stretching, exercise, and therapeutic devices to maintain tissue length and function.
Splinting
Splints are commonly employed for burn injuries. These devices provide multiple functions including facilitating proper positioning, preventing joint contractures, protecting skin grafts or fragile wounds, or assisting desired motion.
Splints are fabricated from many materials. Low-temperature thermoplastic orthotics are most common. Low-temperature plastics have several advantages including the ability to be warmed at the bedside in heated water and fitted to the patient immediately. These plastics are conformable at low temperatures and therefore can be readily remodeled and adjusted as needed in the clinic or at bedside.
Custom splints can be designed for virtually all parts of the body. Hand injuries commonly require custom splints. Custom splints are advantageous for difficult to fit areas and for sites that require unique design or built-in features, such as facilitating motion at a single joint. They are costly, require experienced staff for construction and maintenance, and necessitate that materials are available on site for fabrication.
Commercially available prefabricated splints may be cost-effective; however, these splints often require modification to fit properly or to achieve the intended purpose. Some clinicians believe that the commercially available prefabricated splints are best used for positioning the knee and ankle. Splints that are simple and straightforward in design and function are “user friendly.” Such splints are more likely to be applied correctly and compliantly. An incorrectly applied splint can lead to further injury, including nerve damage, loss of skin graft, and other skin trauma. A properly designed and fitted splint avoids pressure over bony prominences and is compatible with wound dressings and topical medications. It is often desirable to fabricate the splint with moldable materials that can be modified as a patient’s needs change.
The basic rule of splinting is to splint the body part in a position opposite of the expected deformity. Factors to consider when prescribing a splint include burn size, burn location, burn type, functional goals, and patient activity level.
The wearing schedule for splints is individualized. In the case of the comatose patient, splints should be worn for 2 to 4 hours and then removed for a similar length of time and then reapplied. The wearing schedule can be modified as the patient’s level of participation is increased. Splints may be worn to maintain the gains made in therapy.
If normal ROM of a joint is preserved, a splint is not indicated unless a joint or tendon is exposed or the patient is noncompliant with positioning. Common splints include the knee extension splint to prevent knee flexion contracture and posterior foot drop splint to maintain neutral ankle positioning.
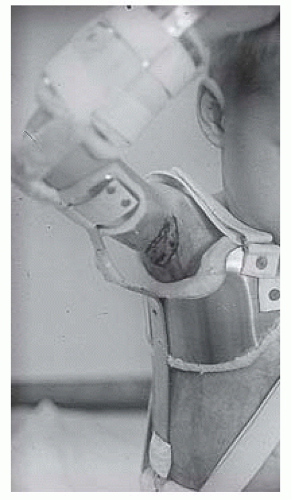
The upper extremity is the most common site for contractures. For axillary burns, an “airplane” splint is used to prevent shoulder adduction contracture. An “airplane” splint holds the upper extremity in approximately 15 degrees of horizontal adduction
and 90 degrees of abduction. This splint prevents shortening of the anterior and posterior axillary folds. Modifications or inserts are used to maintain the contours of the axillary apex and increase ROM as tolerated (
Fig. 43-9). In injuries of other upper-extremity joints, splints are fabricated to meet the specific positioning demands of the elbow, forearm, and wrist.
To correct a contracture various static progressive splints or orthoses are designed to provide a slow progressive sustained stretch. The literature documents success using serial casting to achieve contracture correction as well (
15). Staley and Serghiou (
16) summarized serial casting use in burn injury:
Long duration of stretch with minimal force.
Protection of exposed tendons
Mechanical forces to remodel scar
Cost-effective
Treatment useful in children and noncompliant patients
Treatment option when an open wound is present.
Splints are also valuable in the postacute period to prevent contractures until the tissue length is stabilized, after surgical release of a contracture, or after skin grafting.
Hands
Hands require special attention. When evaluating the burned hand, individual joint motion should be assessed. Limitations in ROM results from decreased tendon sliding, decreased muscle strength, tendon shortening, skin/muscle/ligament/tendon tightness, joint restriction, or a combination of these processes.
During the acute phase, the hands are positioned and splinted to prevent shortening of the joint capsules, collateral ligaments, and muscle tendons. Edema can complicate care as it accentuates metacarpophalangeal (MCP) joint extension and interphalangeal (IP) joint flexion. The resulting combination of MCP hyperextension and IP joint flexion produces the intrinsic minus deformity of the hand, also called claw hand.
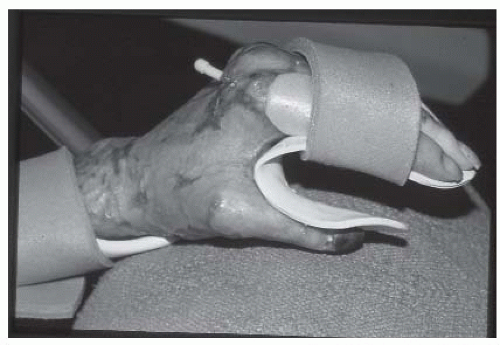
The hand is splinted with the wrist in slight extension, the MCP joints in 70 to 80 degrees flexion, IP joints in extension, and the thumb abducted from the palm. Fingers are positioned in abduction (
Fig. 43-10). If the burns are limited to the palmar aspect, then the MCP and IP joints are positioned in extension, fingers abducted, and the thumb abducted from the palm. Palmar splints may need modifications to maintain the palmar arch. Elastic wraps or straps are employed to secure the splint. Elastic wraps are applied in a figure of eight formation to avoid circumferential constriction. Straps should be soft and applied in a crisscross orientation.
Circumferential hand burns often damage the web spaces of the hand. Preservation of the web spaces is important for hand rehabilitation. For example, loss or shortening of the first web impairs thumb opposition and abduction and interferes with grasp (
17). Early intervention is critical. In addition to abduction, exercise to all the digits, web space dressings, and soft inserts or straps are placed in the web spaces. Also, thermoplastic inserts may be customized and fitted in these areas. Compression gloves may be used in conjunction with the splints. In mild cases, compression gloves may be sufficient to preserve web spaces and function.
Exposed tendons require splinting in a slack position. The tendon should be kept moist to avoid desiccation and denaturation. With time, the tendon may revascularize and become functional. If the exposed extensor hood of the fingers is not kept slack, the central slip can fail and lead to a boutonniere deformity. In cases of extensor hood rupture, the finger is positioned in extension. In approximately 6 weeks, scar tissue may form to bridge the extensor surface and act as a functional substitute. After that time, active ROM can be initiated (
18).
For exposed joints, a splint is prescribed to provide protection. Gentle ROM is performed to maintain motion. If the joint capsule is violated, the joint is at risk for ankylosis. In such cases, the joint is best placed in a function position.
Edema can cause a claw hand. After 12 to 18 hours, edema changes consistency to a gelatinous substance secondary to lymphatic vessel occlusion and impaired fluid clearance. This gellike quality makes the edema more difficult to resolve. In the acute stage after injury, the upper extremity and hand are typically suspended above the patient’s head to aid fluid return and reduce edema. Care is taken not to stretch the brachial plexus or damage the ulnar nerve.
The resting hand splint, with the inclusion of wrist extension, contributes to edema control of the hand (see
Fig. 43-10). This splint stretches the normally redundant dorsal skin, thereby limiting space for edema collection. Edema formation coupled with the flexor tendon pull increases flexion at the IP joints resulting in a claw hand deformity.
Once skin closure is achieved, a compression glove is prescribed to assist with edema control (
Fig. 43-11). Passive exercise and scar suppression are also employed to assure restoration and maintenance of normal ROM.
Exercise
In burn rehabilitation, one of the earliest goals of exercise is to maintain or achieve normal ROM. For the obtunded or comatose patient, passive ROM exercises emphasizing the end ROM is appropriate. Alert and cooperative patients can participate in active and active-assisted exercise. With children, developmentally appropriate exercise and play activities are indicated to achieve the therapy goals.
Surgical anesthesia can provide an opportunity to perform ROM exercises and determine objective measurements of
range. In this setting, one can perform ROM without concern for pain. The opportunity to assess ROM under anesthesia is valuable in the case of a child, an uncooperative patient, or if pain is inhibiting ROM exercise.
Stretching exercises are prescribed when ROM is abnormal. The biomechanics of skin and muscle are different; therefore, the two tissues are stretched differently. Stretching of injured skin or scar tissue requires a slow sustained mechanical stretch to enhance elongation of collagen and underlying fibers. When a prolonged stretch is performed, the stretch is maintained until the tissue blanches. Blanching indicates that the tissue is near its yield point, the point at which the skin is at risk of tearing (
19,
20).
After burn injury, muscular weakness, fatigue, and deconditioning are serious problems. These sequelae interfere with function, such as ambulation, ADL skills, and endurance. Loss of muscle mass and, in children, the additional loss of bone mass, interfere with the restoration of function, return to work or school (
21,
22).
Literature indicates that a structured exercise program composed of aerobic and resistance training leads to increased function as measured by increased muscle mass, strength, and cardiovascular endurance (
23). Suman and Herndon (
24) demonstrated the efficacy of a supervised exercise program for children, ages 7 to 18 years, that included resistance and aerobic exercise. His team trained children in eight basic exercises, including bench press, leg press, and triceps curls under the supervision of a physical therapist in an outpatient setting. The control group was instructed in a home exercise program. The participants of the supervised resistance and aerobic program required significantly fewer surgical releases up to 2 years after the intervention (
25). Suman et al. (
26) also demonstrated that children had increased lean body mass and muscle strength with structured exercise and the concurrent administration of the anabolic steroid, oxandrolone, for 1 year after injury. Anabolic agents, such as oxandrolone and human growth hormone, have been demonstrated to reduce the effects of hypermetabolism while also increasing muscle mass and strength and decreasing resting energy expenditure in children and adults (
27,
28,
29,
30,
31).
St-Pierre et al. (
32) demonstrated that individuals with small burns did not differ from those without injury in muscle strength. However, for those with greater than 30% TBSA burn produced less torque, work, and power in their quadriceps when compared to matched controls. de Lateur et al. (
33) reported that a structured aerobic exercise program, consisting of three times a week aerobic treadmill training for 12 weeks combined with a standard burn therapy program, achieved improved aerobic capacity. This literature suggests that regular exercise after burn injury, like in other adults, results in improved flexibility, endurance, balance, and strength. Such gains are important for returning to full independence and function. Other likely benefits are reduced anxiety and an improved sense of well-being (
34).
Gait
Independent walking may be the single most important factor in determining discharge disposition after severe burn injury. Farrell et al. (
35) found that independent ambulation predicted discharge from the acute burn unit to home.
As soon as the patient’s condition permits, ambulation should begin. In addition to reducing the risk for contractures, deconditioning and deep venous thromboses, early gait training maintains balance, lower extremity ROM, strength, and endurance. Physical therapists use a tilt table to perform graduated upright positioning. Literature indicates that muscles of the lower extremities, particularly the gastrocsoleus and quadriceps, are the first muscles to lose strength with bed rest. These same muscles experience a greater proportional loss of muscular torque when compared to other skeletal muscles (
36,
37).
The physical therapist can initiate gait training and determine appropriate assistive devices; however, physical therapy sessions should not be the only time the patient walks. Nurses, family, and others can learn how to assist and provide needed guarding during walking. Walking reduces the effects of bed rest and improves aerobic conditioning.
Many consider new autografts to the lower extremities a contraindication to ambulation. Typically, ambulation is not initiated until the surgeon is confident that the graft will tolerate a dependent position. At 5 to 7 days after grafting, patients are instructed to begin lower extremity-dependent positioning. Dangling the lower extremities is a preambulation exercise that helps determine if the graft tolerates the dependent position. The application of elastic wraps or other elastic devices are used to minimize venous pooling and decrease the risk of graft loss. The typical protocol for dangling begins for 5 minutes two to three times per day. If inspection of the graft after dangling shows no signs of intolerance, the duration is progressively increased. Once the graft shows tolerance for dependency, ambulation is initiated. Supportive dressings such as ace wraps are often employed. Like dangling, the time spent walking is methodically increased as the graft tolerates.
Gait deviations are common after burn injury. Some are transient while others persist. Early correction of abnormal stance and gait reduces the risk that the deviation will be long-standing. Deviations result from pain, location of injury, deconditioning, weakness, contractures, and sensory and central nervous system dysfunction. Gait devices are commonly used to protect injured areas, reduce pain, or assist with weight bearing. Devices are also employed to correct or prevent poor posture or gait deviations secondary to injury to the trunk or other areas.
During times that the patient is unable to ambulate, wheelchairs provide mobility and are easily adapted to the patient’s specific needs. Adaptations include attaching splints or wedges to elevate the arm or adding lower-extremity positioning devices.
SURGICAL RECONSTRUCTION
The surgical goal is to minimize surgery and maximize results. If multiple areas are involved, an overall plan and timetable are
developed that prioritize the fewest number of surgeries with the maximal functional benefit to the patient.
The timing of surgical release of a contracture varies. Some surgeons believe that surgery should wait 6 to 12 months after injury. However, there is limited evidence to support this recommendation. Other literature supports early intervention (
38,
39,
40). There is evidence that early release does not worsen outcome, and surgery is indicated with the development of secondary deformities (
41). Tendon and ligament injury impacts the completeness of the release that can be performed. Age, severity of the deformity, and time since injury impact surgical outcome (
39,
42).
Many reconstructive procedures are utilized in the burn-injured patient. Listed in the order of complexity are Z-plasty, skin graft, local skin flaps, local muscle flaps, fasciocutaneous flaps, free flaps, and cross limb flaps (
38).
Simple excision is indicated for scars that are limited in size and location. Z-plasties are employed to limit or correct joint contractures caused by hypertrophic scarring. Contractures of soft tissue that disrupts appearance or tissue flexibility are also treated with Z-plasty. For example, this technique is employed to correct hypertrophic scarring over the chin that prevents adequate mouth closure (
43). Release and skin grafting typically involves a fish-mouth incision and graft placement. Scar pressure therapy and silicone application are often combined with surgery to maximize outcome.
Severe axillary contractures are difficult to treat (
Fig. 43-12). For tight bands formed near unburned skin, five flap releases are used (
44). Local flaps are often used if anterior or posterior axillary fold contractures are present (
39). Contractures that are broader and involve the entire axilla require fasciocutaneous or similar flap procedures (
45).
Contractures at the elbow are often complicated by heterotopic ossification (HO) and this is taken into consideration during the surgical plan (
46). A Z-plasty or five flap release is used to treat a thin band of scarring (
45). Surgical intervention for hand contractures requires expertise and experience. Full-thickness grafts are commonly used. Correction of flexion contracture of the MCP joint has a higher success rate than an extension deformity. K wires are placed for 2 to 4 weeks after surgery for joint stabilization (
47). Like the MCP joint, extension contractures of thumb exhibit poor outcomes. Contractures associated with dislocated or subluxed joints have the worst results (
45,
48,
49).
In recent years, face transplantation has garnered significant interest in the lay press. The first reported human face transplantation was performed in 2005 (
50). To date, there are only a few case reports in the literature (
50,
51,
52). These investigators utilize a cadaveric facial allograft that requires lifelong immunosuppressive treatment. There are unresolved questions regarding ethical, immunological, and psychological issues. Does the improvement in quality of life justify the long-term risks of immunosuppression, including cancer, infection, and renal toxicity? Will the recipient experience graft rejection? What are the psychological consequences of a transplanted face? These and other issues are only beginning to be addressed in the literature (
53,
54,
55).