Acetabular Rim Damage
Paul E. Beaulé and Michael Leunig
Key Points
Introduction
Klaue and coauthors1 were the first to coin the term acetabular rim syndrome, which encompasses pathologic loading and resulting damage to the labrum, acetabular cartilage, and/or bony rim. In their study of acetabular dysplasia, a spectrum of pathologies ranging from a torn labrum to an acetabular rim fracture, as well as cysts within the acetabular bony rim or adjacent soft tissues, was described. Until recently, diagnosis and imaging of these lesions were difficult and often required operative intervention to confirm the diagnosis.2–6 With the advent of more advanced surgical (open hip dislocation) and imaging techniques such as magnetic resonance arthrography,7,8 the knowledge base and understanding of the origin of damage to the acetabular labral-chondral complex, as well as its role in degenerative arthritis, have greatly evolved over the past two decades. Despite recent advancements in imaging and in operative techniques, patients with acetabular rim damage still are often misdiagnosed.9 This chapter will review the causes and pathomechanisms of acetabular rim damage, as well as its diagnosis and treatment.
Etiology
In hip dysplasia, Klaue and associates1 introduced the term acetabular rim syndrome as a precursor of secondary osteoarthritis, wherein intrinsically normal intra-articular soft tissue structures are exposed to loading joint forces that physically exceed their tolerance level, resulting in hip damage. The frequently enlarged acetabular labrum in dysplastic hips10 initially aids in maintaining the femoral head within the joint; however, the unstable femoral head potentially translates and eventually subluxes secondary to deficient coverage. If these chronic “inside-out” shear stresses do persist, labral soft tissue compensation will fail and the labrum can tear off the acetabular rim or can avulse with an osseous fragment; this is described as rim fracture.1
Although management of damage/degeneration to the acetabular rim is still evolving, consistency in the location of damage within the acetabular rim has been demonstrated in several studies, both cadaveric and in vivo. Peripheral damage to the hip joint was first brought to attention in the classic studies of osteoarthrosis conducted by Harrison and colleagues11 and Byers and coworkers.12 This was further supported by the work of Bullough and associates,13 who emphasized the importance of the shape of the hip joint in the form of minor incongruencies leading to failure of articular cartilage at the acetabular rim within normal daily contact. Despite these early reports documenting the acetabular rim as an early site of hip damage, specific disorders such as hip instability due to dysplasia (Fig. 37-1) and, more recently, femoroacetabular impingement (FAI) (Fig. 37-2) were underappreciated as causative factors for hip osteoarthritis (OA). The acetabular labrum and adjacent cartilage are early structures to fail in acetabular rim disorders secondary to localized stresses. This notion was more recently confirmed by Leunig and colleagues,14 who compared cadaveric findings and noted anterior acetabular quadrant damage with associated insufficient femoral head-neck offset. Seldes and coworkers15 further characterized acetabular rim damage as two main types of rim degeneration correlating with our current understanding of FAI.14
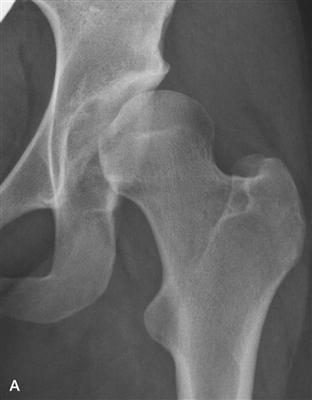
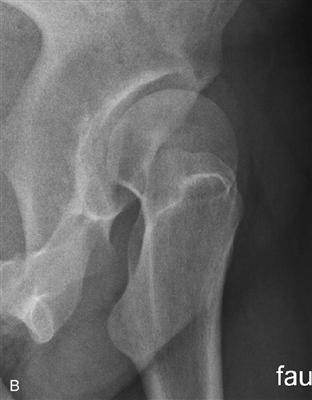
Figure 37-1 A, Acetabular rim damage as exemplified by an anteroposterior hip (taken from a correct anteroposterior [AP] pelvis) (B) and faux profile radiographs of classic anterolateral hip dysplasia. As the consequence of a short and steep acetabular roof, the femoral head translates anterolaterally, resulting in high “inside-out” shearing forces leading to secondary joint incongruity and static rim overload.
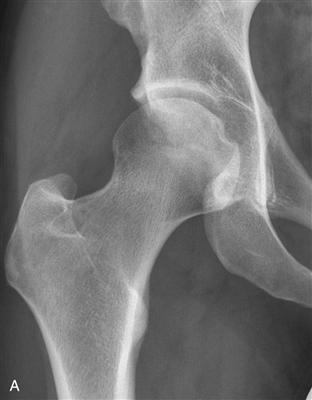
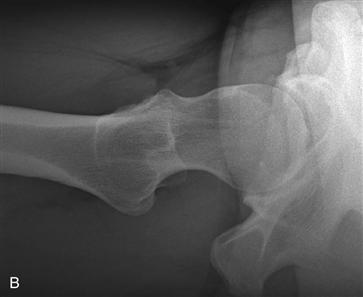
Figure 37-2 A, Acetabular rim damage exemplified by anteroposterior hip (taken from a correct anteroposterior [AP] pelvis) (B) and cross-table lateral radiographs of femoroacetabular impingement. As the consequence of primary incongruity of the hip caused by femoral head overcoverage and/or asphericity, hip motion with “outside-in” shearing forces will result in dynamic rim overload.
In FAI, the femoral head is well centered, but the free arc of hip motion is limited by a deep or malorientated acetabulum, producing pincer FAI or a misshaped proximal femur (insufficient head-neck offset, nonspherical head causing cam FAI). It is not uncommon that a combination of cam and pincer FAI exists. In FAI, articular damage initially occurs by point or regional loading of the femoral neck against the acetabular rim. The site of hip damage is similar to that of acetabular rim damage seen in hip dysplasia; however, failure mechanisms are almost the opposite. Furthermore, damage patterns of pincer and cam FAI differ substantially when one of these two types exists as an isolated deformity. In pincer FAI, pathology is more localized to the labrum, and in cam FAI, damage takes place at the cartilage with “outside-in” abrasion and/or delamination, with the occasional rim fracture.16 An osseous rim fragment in FAI may be seen in athletes with a combined type and pronounced acetabular malorientation. Speed, force, and degree of hip motion, in addition to the quality of tissue at the labral-chondral junction, might contribute to enhanced vulnerability at the anterosuperior rim.17
To date, our knowledge indicates that hip dysplasia and FAI are the two major bony deformities associated with the development of osteoarthritis in the hip. Alterations in hip joint mechanics represent a continuum between “undercoverage” (dysplasia) as described by Klaue and associates1 and, as introduced more recently, “overcoverage” (FAI). As our understanding of these morphologic alterations of the hip has improved, it has become clear that combinations of these mechanical factors frequently lead to reactive pain within the periarticular soft tissues such as trochanteric (abductors) and/or groin pain (hip flexors/adductors).
Acetabular Rim Damage and the Labrum
The acetabular labrum is triangular in cross-section, with the base applied to the acetabular rim and the apex being the free margin.15 The joint capsule attaches to its external edge, creating a potential recess between the capsule and the labrum. The labrum can be subdivided into two distinct zones: the extra-articular side, consisting of dense connective tissue, is well vascularized at its junction with the joint capsule, whereas the intra-articular portion is largely avascular.18 In addition, recent embryologic studies of the hip joint show that the anterior and posterior acetabular-labral chondral junctions have different morphologic appearances.19,20 In a study of 11 human embryos, Cashin and associates19 found that the anterior labrum has a rather marginal attachment to the acetabular cartilage with an intra-articular projection, whereas the posterior labrum is attached and continuous with the acetabular cartilage. In addition, anteriorly the labral-chondral transition zone is sharp and abrupt, while posteriorly it is gradual and interdigitated. These most recent findings contrast with those of Petersen and associates21 and Seldes and colleagues,15 who initially described the acetabular labrum as continuous with the articular cartilage throughout the acetabulum.21 This abrupt anterior transition zone would make the labrum more susceptible to tearing and corresponds to some extent to the so-called watershed lesion.22 Based on intraoperative observations of a large number of hip arthroscopies for labral tears, as well as cadaveric dissections, McCarthy and associates22 described the anterior labrum as an at risk zone because of potentially inferior mechanical properties, higher mechanical demands, and relative hypovascularity, and proposed that a labral tear alters the biomechanical environment of the hip, leading to degeneration of the articular cartilage and eventual osteoarthritis.23
In terms of its predilection for failure, Dorrell and Catterall24 correlated the occurrence of a labral tear with abnormal shear stresses transmitted by the uncovered femoral head, as may occur in acetabular dysplasia. From this clinical situation, they postulated that the enlarged labrum contributes to stability of the femoral head within the acetabulum in adulthood. This aspect of load sharing was later supported by the work of Kim and associates,25 who demonstrated that the labrum contributed to growth and development of the acetabular roof. Although a role of load sharing, similar to that of the meniscus in the knee, may be correct in cases of dysplasia, more recent work by Konrath and associates26 shows that the labrum does not have an important load sharing role. Instead, based on a finite element analysis and cadaveric investigation, Ferguson and colleagues27 found that the labrum acts as a seal, ensuring more constant fluid film lubrication within the hip and limiting the rate of fluid expression from the articular cartilage layers of the joint, as noted by greater hydrostatic fluid pressurization within the intra-articular space with an intact labrum. In addition, because the labrum adds extra resistance to the flow path for interstitial fluid expression, cartilage consolidation was significantly quicker without the labrum.27,28 Consequently, disruption of the labral seal could be detrimental to the overall nutrition of the cartilage, leading to its premature degeneration.29 Takechi and coworkers30 showed the labrum contributing to stability of the hip joint through its valve effect and structure. Both of these mechanisms were dependent on the fit of the labrum against the femoral head.28 Similarly, Crawford and associates31 reported that loss of the labral seal is the critical event leading to destabilization of the hip, shifting the hip center of rotation and making the hip susceptible to increased impact loading and repetitive trauma through loss of the protective function provided by the intact labrum and its seal.
It is interesting to note that the morphologic appearance of the labrum can differ on the basis of its underlying mechanism of failure: dysplasia or femoroacetabular impingement.32,33 Klaue and colleagues1 and Leunig and coworkers32 showed that in dysplasia, the labrum is distinctly hypertrophic with myxoid degeneration and/or detachment from the bony rim, whereas in femoroacetabular impingement, the labrum is more commonly characterized by an undersurface tear with no hypertrophy.32 These findings can be helpful in establishing the dominating underlying bony abnormality when in the presence of mixed deformities such as dysplasia and FAI.
In terms of pincer-type FAI, Seldes and associates15 described labral damage extending perpendicular to the surface of the labrum and in more severe cases to the subchondral bone with associated endochondral ossification within the labrum; this is consistent with operative findings seen in pincer impingement. With acetabular rim damage associated with cam-type FAI, Seldes and colleagues15 described disruption of the transition zone between the fibrocartilaginous labrum and the acetabular cartilage perpendicular to the articular surface, leading to cleavage/disruption at the anterior labral-chondral junction.
Diagnosis
Clinical Evaluation
In most patients with acetabular rim damage, the chief complaint will be anterior groin pain made worse by long periods of standing, sitting, walking, or getting into and out of a car. The pain can be referred to the gluteal area or the trochanteric region. Although no specific clinical findings differentiate dysplasia from FAI, the vast majority of patients with dysplasia will have symptoms ranging from early fatigue to clear weakness of the abductors, with irritation over the greater trochanter. In addition, some patients may experience a catching phenomenon similar to that caused by meniscal disease of the knee; this occasionally requires manipulation of the lower limb, usually in the form of a “shaking-free” movement.34 As symptoms increase in frequency, residual pain may result in a slight limp, whereas patients with FAI will complain of chronic/recurring “groin” injury, as well as limited hip flexibility, but with well-preserved muscle function. Onset of pain in most cases is insidious,35 with patients often unable to recall a specific traumatic event.5 Among patients with labral tears in general, Burnett and associates9 found that only 9% (6 of 66 patients) had a major traumatic episode as a causative factor for acetabular rim damage. The pain was often sharp in nature and was aggravated by activity such as walking and pivoting on the affected side. Mechanical symptoms such as clicking and catching are highly variable and are not necessarily indicative of intra-articular hip pathology.5 On history, it is critical to inquire about childhood hip diseases such as dysplasia,25 Legg-Calvé-Perthes (LCP),36 and slipped capital femoral epiphysis (SCFE),37 all of which are known causes of osteoarthritis.38,39
On physical examination, the most reliable sign of labral pathology35 is pain reproduced with flexion past 90 degrees, combined with internal rotation and adduction. This is referred to as the impingement sign.1 Others have found that forced external rotation with hip extension can irritate the damaged rim40 and is more commonly reported in patients with dysplasia. In addition, in dysplasia, Leunig and associates34 describe the bicycle test, whereby trochanteric irritation reflects abductor muscle insufficiency. This test is performed with the affected hip up; a bicycle pedaling maneuver is then performed as the lateral and posterior margins of the trochanter are palpated. Increasing the load on the pedaling foot may exacerbate the pain. Tenderness is most commonly palpated along the posterior border of the gluteus medius muscle. As for patients with FAI, they typically will have limited internal rotation (usually less than 20 degrees) with the hip flexed at 90 degrees.
Although labral pathology is now recognized as a common cause of hip pain, it is important to include in the differential diagnosis other causes of hip pain such as osteonecrosis, stress fracture, and snapping psoas tendon. In cases of abnormal physical findings and normal or equivocal radiologic findings, an anesthetic block of the symptomatic hip may provide important diagnostic information in terms of delineating intra-articular versus extra-articular hip pathology. Temporary pain relief represents a positive finding for intra-articular hip pathology.41
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








