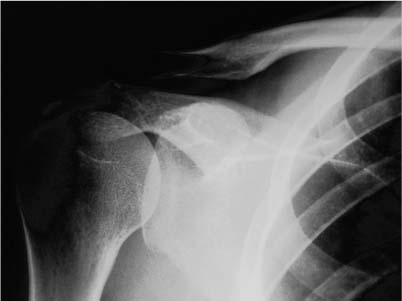
Case 28 A 43-year-old woman presents with a 6-month history of right shoulder pain without specific incident. She states that her symptoms have increased dramatically over the last 3 to 4 days, making even activities of daily living difficult. She has been unable to sleep very well and complains of moderate to severe shoulder pain. She denies any numbness in her upper extremity or any other significant complaint. Range of motion appears to be limited significantly by pain. Active forward flexion is 60 degrees and passive is 130 degrees. Passive external rotation is normal, although any motion of the shoulder causes moderate pain. Stability testing is difficult secondary to pain, but appears to be normal. She is neurovascularly intact. No tenderness is present about the shoulder except over the area just lateral and inferior to the lateral acromion, in the area of the greater tuberosity. No swelling or localized redness can be seen. This patient does have a markedly positive impingement sign and a positive Hawkins impingement sign. 1. Partial-thickness rotator cuff tear 2. Full-thickness rotator cuff tear 3. Calcific tendinitis 4. Bicipital tendinitis 5. Anterior labrum tear An anteroposterior (AP) view of the shoulder is obtained (Fig. 28–1). Figure 28–1. An anteroposterior (AP) radiograph of the affected shoulder. PEARLS • Use of a spinal needle in the subacromial space at the time of arthroscopy can help to identify calcific deposits. Puncture of the rotator cuff tendon will allow for a “snowstorm” appearance as the calcium deposits are flushed into the subacromial space. • Use of a high-quality fluoroscopic unit intraoperatively can help ensure that complete calcium deposit removal has been accomplished. Also, persistent calcifications can be identified and effectively localized with these fluoroscopic units. • Despite the surgeon’s best efforts, some calcific deposits may remain, and it is important to counsel the patient of this possibility preoperatively. Calcific Tendinitis. The history of impingement-related symptoms, the acute worsening of her symptoms without specific injury, and the tenderness over the greater tuberosity suggest a rotator cuff tear or calcific tendinitis. Radiographs confirm calcific tendinitis. The calcific deposits are relatively easy to see on the radiographs in this patient. But deposits are often less apparent or obscured by the humeral head, depending on their location within the substance of the rotator cuff tissue. Internal and external rotation films can sometimes aid in localizing the position of the calcific deposits when their position is difficult to ascertain on a routine shoulder series. Also, an axillary view and/or a scapular Y view can assist in localizing calcific deposits, particularly within the infraspinatus or subscapularis tendons. Patients with calcific tendinitis generally complain of a several-month or -year history of either recurrent or persistently mild shoulder pain that intermittently worsens. Although such symptoms are compatible with recurrent rotator cuff tendinitis, the acute flare-ups typically cause much more pain and localized tenderness over the greater tuberosity than does recurrent tendinitis. Likewise, patients with calcific tendinitis can often localize their maximum point of tenderness in the area of the greater tuberosity, and in the authors’ experience this is unusual in patients with rotator cuff tendinitis. The treatment of calcific tendinitis should initially be nonoperative. Management is based on the recognition and localization of the calcific deposit as a source of shoulder pain. The patient generally presents with symptoms compatible with impingement syndrome. Radiographs then confirm intratendinous calcifications. These calcifications presumably cause an intrinsic tendonopathy that reduces the size of the supraspinatus outlet due to both tendinous swelling and localized reactive bursitis. Patients with a long history of recurrent acute flare-ups of calcific tendinitis probably are experiencing recurrent, acute-phase reactions within the calcium deposit itself as resorption occurs. Another possible explanation for the acute-phase symptoms involves the possible rupture or extravasation of calcifications into the subacromial space. Regardless of the etiology of the acute-phase symptoms, the patients present with moderate to severe pain that limits not only activities with the shoulder but also their ability to rest and perform normal duties. Patients presenting with an acutely symptomatic calcific tendinitis are often dramatically improved by the injection of subacromial anesthetic instilled along with corticosteroid. Not uncommonly, “needling” the calcific deposit and subacromial injection can completely alleviate the patient’s pain. The consistency of the calcific deposits vary according to their phase and chronicity. Occasionally, an amorphous deposit of calcific granules can be aspirated using a large-bore needle. More often, calcific deposits are chalky in consistency and cannot be aspirated. The consistency of the calcific deposits can often be appreciated at the time of needling as evidenced by a gritty sensation. The mechanism by which localized needling of the deposits improves symptoms is not fully understood, but may be related to the introduction of vascular ingrowth channels, which facilitates the process of resorption. Patients with calcific tendinitis must also be encouraged to perform range of motion exercises on the shoulder. This is done to maintain motion and prevent complications such as adhesive capsulitis. Generally, the acute phase abates over time with the introduction of local anesthetic and corticosteroids, supplemented by nonsteroidal antiinflammatory medications and exercises. Calcific tendinitis that is refractory to these nonoperative measures, or calcific tendinitis that continues to recur despite repeated attempts at nonoperative treatment, may respond to surgical intervention. PITFALLS • Careful radiographic assessment of the shoulder is sometimes necessary to identify calcific deposits within the rotator cuff tendon. Patients with symptoms compatible with calcific tendinitis should have their X-rays viewed under a “hot light” if difficulty is encountered in visualizing the area of concern using normal radiographic lighting. • Excellent visualization in the subacromial space is required to identify and adequately remove the calcific deposits within the tendon. Failure to perform a complete bursectomy or to achieve adequate hemostasis may result in inadequate removal of the deposits. Also, care must be taken to identify both radiographically and arthroscopically multifocal areas of calcific deposits. • Removal of large calcific deposits often leaves a large partial-thickness defect in the rotator cuff tendon that may require repair. Identification and proper repair of this defect is important in preventing progressive tearing of the tendon and persistent symptoms. • Calcific tendinitis can often occur in conjunction with other common shoulder conditions such as a symptomatic acromioclavicular joint or intraarticular pathology. Careful preoperative assessment will allow for an accurate evaluation of the conditions present within the shoulder.
History and Physical Examination
Differential Diagnosis
Radiologic Findings
Diagnosis
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree