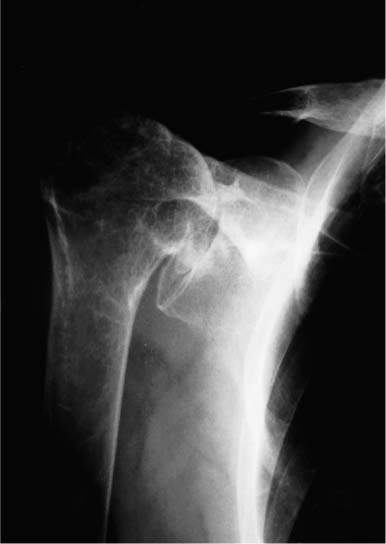
Case 24 A 79-year-old woman presents with a 10-year history of recurrent shoulder pain and weakness that has progressed over the last 2 years. She complains primarily of pain and limited active forward flexion. She reports a number of nonoperative interventions, including a trial of organized physical therapy prescribed by another physician, two different antiinflammatory medicines, and two subacromial steroid injections over the last year. Active forward flexion is limited to 45 degrees. Passive forward flexion is 125 degrees with external rotation actively and passively limited to 10 degrees. She has 3/5 supraspinatus strength and 4/5 external rotation strength. She has crepitation through range of motion of the shoulder that is moderately painful. She is otherwise neurovascularly intact. Figure 24–1. An anteroposterior (AP) radiograph of the affected shoulder. 1. Massive rotator cuff tear 2. Degenerative arthritis of the shoulder 3. Rotator cuff arthropathy An anteroposterior (AP) radiograph of the shoulder is presented (Fig. 24–1). Rotator Cuff Arthropathy. The long history of progressive symptoms combined with the physical examination that demonstrates painful crepitation and severe limitations suggests severe degenerative joint disease possibly combined with a rotator cuff tear. The radiographs confirm significant superior head migration combined with severe degenerative changes of the glenohumeral joint, confirming the diagnosis of rotator cuff arthropathy. Neer and colleagues (1982) originally described this condition and reported on the clinical and operative findings of a group of 26 patients. Superior migration of the humeral head with abutment of the head under the anterior acromion is seen on radiographs. This abutment is combined with severe degenerative changes within the glenohumeral joint itself. Treatment of patients with massive irreparable rotator cuff tears associated with severe glenohumeral joint degeneration and humeral head collapse presents a difficult clinical challenge. Adequate repair of the rotator cuff is rarely possible and subacromial decompression with rotator cuff debridement alone fails to address the severe glenohumeral joint destruction. Total shoulder arthroplasty in these patients has been associated with an increased incidence of glenoid loosening as the superi-orly migrated component distributes its compressive loads abnormally on the superior glenoid surface. The diagnosis is based on the clinical and radiographic findings. Nonoperative measures consisting of a gentle exercise program, nonsteroidal antiinflammatory medications, and occasional shoulder joint corticosteroid injections may improve symptoms. However, once severe migration and humeral head collapse have occurred, operative treatment is often necessary to significantly reduce symptoms. Attempted use of the extremity for overhead-motion activities is generally prohibited because of pain and weakness. Night pain is often very common as well. Clinical findings such as atrophy within the supraspinatus and infraspinatus fossa are common at presentation, and occasionally the humeral head can be palpated in the anterosuperior aspect of the shoulder in its subluxed position. Sophisticated imaging studies such as magnetic resonance imaging and computed tomography (CT) scanning are usually not required as plain radiographs clearly demonstrate the pathology. Subchondral sclerosis, osteophytes, and irregular cystic formation are generally seen. This chronic subluxation of the humeral head also often causes “acetabularization,” as secondary erosions of the glenoid, acromial under-surface, and clavicle occur to accommodate the humeral head. Patients with symptoms unresponsive to conservative measures are candidates for surgical intervention. Hemiarthroplasty is the preferred surgical technique of the authors. A glenoid component not only is ineffective in maintaining a more normal glenohumeral articulation following shoulder replacement, but also has been shown to loosen much sooner in such a situation as a result of asymmetric loading from a “rocking horse” effect. Other important factors to consider when planning a hemi arthroplasty for cuff-tear arthropathy centers on the status of the coracoacromial arch. Previous attempts at rotator cuff repair where the coracoacromial arch is sacrificed as a result of an acromioplasty and coracoacromial ligament resection may compromise the postoperative stability of the humeral replacement. One of the authors (L.D.F.) reported on a group of patients with cuff-tear arthropathy who developed significant anterosuperior instability following an attempt at hemiarthroplasty that was performed following an unsuccessful attempt at rotator cuff repair in which an acromioplasty was performed. This study demonstrated the importance of maintaining an intact arch in such patients. If an attempt at hemiarthroplasty is carried out for cuff-tear arthropathy in patients with an incompetent coracoacromial arch, an attempt at reconstruction of the arch is important to reduce the chances of postoperative instability. The surgical technique for hemiarthroplasty for cuff-tear arthropathy begins with a deltopectoral approach. After the remaining subscapularis tendon is released, the massive rotator cuff tear is identified and debrided of functionless tissue. The undersurface of the coracoacromial arch is also debrided of any excessive fibrous tissue and smoothed, but the coracoacromial ligament is left intact and no acromioplasty is performed. Care is taken in each case to maintain the coracoacromial arch to allow effective articulation of the humeral head component within this arch. If the arch is incompetent as a result of progressive humeral head migration or failed surgeries, an attempt should be made to reconstruct it. This may include the use of autograft tendon or fascia, but such reconstruction is generally carried out intraoperatively only if significant anterosuperior instability occurs after humeral component placement. The humeral head is resected after debridement is completed with the arm in approximately 35 degrees of external rotation. Care should be taken to avoid resection of excessive bone in these shoulders with deformed and collapsed humeral heads. Likewise, the version angle for resection of the humeral head may require adjustment based on glenoid orientation. The appropriate-size humeral stem is then press-fit, and the stability of the implant confirmed. If the stability is questionable, the prosthesis is cemented into position. Varying sizes of modular humeral head trials are then applied to the humeral stem. The most appropriate humeral head replacement size is somewhat controversial and depends on a number of factors. If a significant amount of functional rotator cuff tissue can be mobilized so as to achieve a well-balanced partial rotator cuff repair, then a slightly undersized humeral head component is preferred by the authors. This slightly undersized humeral head component will allow for improved lateralization of the rotator cuff tendinous tissue and will help maintain more normal glenohumeral translations even after partial rotator cuff repair. However, when little if any functional rotator cuff tissue can be identified, the authors prefer to place a slightly oversized humeral head component onto the stem. The goal in this situation is to achieve effective articulation with the coracoacromial arch (Fig. 24–2) while maintaining the ability to translate the humeral head approximately 50% of its width anteriorly, posteriorly, and inferiorly, with the glenoid serving as a reference. Care is taken not to use a humeral head size with a diameter and radius of curvature equal to the coracoacromial arch because this would tend to constrain the head within the coracoacromial arch and thus prevent anterior and posterior translation on the glenoid. Also, oversizing of the humeral head component to “match” coracoacromial arch dimensions will usually cause the humeral head component to translate anteriorly relative to the center of the glenoid, effectively subluxating the humeral head component. Standard closure over a suction drain is then carried out. PEARLS • One of the most critical steps in maximizing function following hemiarthroplasty in this group of patients is accurately assessing and then repairing that portion of the rotator cuff tear that is functional. Simply reapproxi-mating a minimally functional musculotendinous unit to the resected surgical neck is unlikely to improve function or even stability postoperatively. A well-performed partial repair of functional rotator cuff tissue is much preferred to a complete repair of relatively functionless musculotendinous tissue. This determination of the relative repairability of the cuff will often influence the size of humeral head component chosen. • Particular care should be taken during preparation and insertion of the humeral component as these patients generally have significantly more osteopenia than patients without rotator cuff arthropathy and are at increased risk for intra-operative fracture of the humerus.
History and Physical Examination
Differential Diagnosis
Radiologic Findings
Diagnosis
Surgical Management
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree