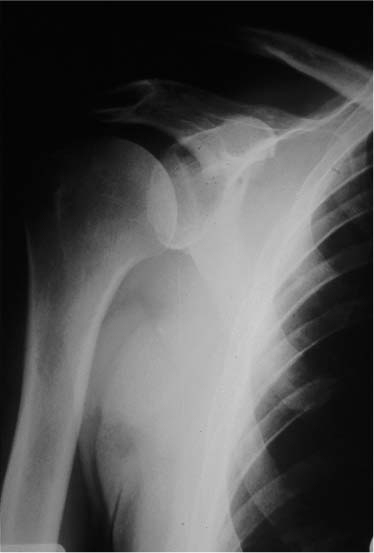
Case 19 A 45-year-old, right-hand dominant, manual laborer presents with a 2-year history of superior shoulder pain following a fall onto his right shoulder. He complains of tenderness in the area of the acromioclavicular (AC) joint and asymmetry. He denies any numbness or weakness of his right upper extremity or any instability symptoms. Range of motion and strength of the shoulder are normal. He has a mildly positive impingement sign. Translation testing demonstrates normal anterior, posterior, and inferior translation. The shoulder is nontender except directly over the AC joint. There is a relative prominence of the distal clavicle in the area of the AC joint as well. An acromioclavicular loading test performed by applying a downward force on the 15-degree adducted and 90-degree forward flexed shoulder is positive for pain in the area of the AC joint. Figure 19–1. An anteroposterior (AP) radiograph of the patient. 1. Chronic acromioclavicular joint separation 2. Rotator cuff tear 3. Bicipital tendinitis An anteroposterior (AP) view of the shoulder demonstrates irregularity and asymmetry of the AC joint (Fig. 19–1). Chronic Acromioclavicular Joint Separation. The patient’s history and physical examination, in combination with the radiographs, demonstrate an AC joint separation. His history of injury 2 years before and his persistent symptoms since confirm the chronic nature of the injury. Nonoperative management of this chronic separation is unlikely to lead to permanent improvement. His symptoms have been persistent since the injury and are likely due to both the soft tissue injury that occurred at the time of the separation as well as the permanent AC joint incongruity. Nonoperative measures that may be considered include nonsteroidal antiinflammatory medications and/or injection of corticosteroids into the area of the AC joint. An exercise program is likely to fail, as this man, accustomed to heavy manual labor, does not demonstrate atrophy or weakness of the shoulder musculature. Surgical considerations center around the desirability of the reapproximation of the AC joint versus simple excision of the distal clavicle. Also, if the AC joint is reapproxi-mated, controversy exists about the necessity for excision of the distal end of the clavicle at the time of reapproximation. Some studies suggest that simple excision of the distal clavicle results in inadequate relief of symptoms, particularly when displacement is greater that a type II separation. Other studies have suggested that reducing chronic AC joint separations without excising the distal clavicle will lead to an increased incidence of postoperative AC joint pain. This is presumably due to the degeneration of the articular cartilage that has occurred subsequent to the original injury. The authors have found that operative intervention using a modified Weaver-Dunn procedure, which combines resection arthroplasty of the AC joint and fixation of the clavicle in a reduced position, has been very helpful in treating these patients. The patient is placed in the beach chair position and the involved extremity is draped, maintaining control of shoulder motion. The AC joint and the coracoid are approached through a saber type of incision originating just superior and 2 cm medial to the AC joint and terminating at the coracoid process. Skin flaps are created by undermining the subcutaneous tissue. This promotes visualization of both the anterior deltoid and trapezial insertions along the clavicle, as well as of the AC joint. The deltotrapezial fascia is incised in the interval between the anterior deltoid and trapezius, in line with the superior cortex of the distal clavicle and the AC joint. Anterior and posterior flaps are developed, including the trapezial and anterior deltoid attachments, and capsule of the AC joint. The dissection proceeds inferiorly by splitting the anterior deltoid muscle in line with its obliquely running fibers. Only a limited deltoid split of 2 to 3 cm is necessary. Suture anchors will allow for firm fixation to the coracoid without the necessity for extensive exposure as required when passing sutures around the coracoid base. One centimeter of distal clavicle is then resected using an oscillating saw and the fibrocartilaginous disk is excised. Removal of larger amounts of the distal clavicle may jeopardize the ability to transfer the coracoacromial (CA) ligament into the medullary canal of the distal clavicle. The lateral cortex of the distal clavicle is smoothed and the arm is placed through a full range of motion including adduction. Care is taken to observe the AC joint to ensure that no impingement of the distal clavicle occurs with the medial acromion. In the event of impingement, it is helpful to resect a small portion of the medial acromion so as to allow for the required clearance. The entire CA ligament is visualized and then carefully freed from the undersurface of the acromion either with or without an attached block of bone from the undersurface of the acromion. The ligament is dissected distally to the coracoid process, leaving its origin attached. A no. 2 nonabsorbable suture is then passed through the ligament using a modified Kessler stitch (Fig. 19–2). The clavicle is reduced in relation to both the acromion and the coracoid. Two 2.5-mm bi-cortical drill holes are placed in the central portion of the clavicle just superior to the coracoid process. Two additional unicortical drill holes are made more laterally on the superior border of the clavicle and are angled in the direction of the resected distal tip of the clavicle. Two suture anchors loaded with no. 5 nonabsorbable suture are then placed in the base of the superior portion of the coracoid process. One limb of each of the sutures is then independently passed through one of the previously drilled holes just superior to the coracoid process. Next, each free end of the no. 2 nonabsorbable suture previously passed through the CA ligament is passed through one of the two more laterally placed drill holes but left untied. The AC joint is then held reduced by an assistant. The no. 5 suture limbs are tied so that the knots are located along the anterior and inferior cortical margin of the clavicle. Passing and tying these sutures using this method minimizes their prominence on the superior cortical margin of the clavicle. It also minimizes the tendency of the sutures to translate the distal clavicle anteriorly. Next, the lateral sutures are pulled taut, so as to advance the resected CA ligament well into the medullary canal of the distal clavicle and this suture is then tied (Fig. 19–3). Following reapproximation of the AC joint, the deltotrapezial fascia, superior capsule of the AC joint, and periostium are repaired in one layer with no. 1 absorbable suture. The split in the anterior deltoid is likewise repaired by approximating only the anterior deltoid fascia. A drain is not usually required. Subcutaneous tissues and skin are closed in a routine fashion. These procedures are routinely performed on an outpatient basis. PEARLS • Use of suture anchors obviates the need for passage of suture around the base of the coracoid process. This also allows for a minimal deltoid splitting incision and a smaller skin incision. • Taking the shoulder through a full range of motion while directly visualizing the resected acromioclavicular joint ensures that no persistent impingement of the acromioclavicular joint with the resected distal end of the clavicle will occur postoperatively.
History and Physical Examination
Differential Diagnosis
Radiologic Findings
Diagnosis
Surgical Management
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree