CHAPTER 30 The Shoulder in Athletes
Repetitive throwing and contact sports place great stress on the shoulder and often at extreme ranges of motion. As a result, the shoulder is a common site of pathology, with associated disability in athletes. Addressing shoulder injuries in athletic patients requires an understanding of the biomechanics and pathology associated with their particular sport. Throwing athletes, for example, repeatedly accelerate and decelerate their shoulder over a wide arc of rotation, causing repetitive microtrauma to the static and dynamic stabilizers of the glenohumeral and scapulothoracic joints. Collision athletes, on the other hand, are prone to sudden macrotrauma to the stabilizing static and dynamic elements of the shoulder. This chapter presents the pathophysiology, evaluation, and management of shoulder injuries specific to the repetitive throwing and collision athletes.
SPORTS-SPECIFIC BIOMECHANICS
Overhead Throwing
Many sports require overhead motion, and the stresses on the shoulder vary tremendously in magnitude and anatomic location depending on the sport. The baseball pitch has been studied extensively and is often used to extrapolate implications for other overhead sports.1
The predicament of the pitcher’s shoulder, the thrower’s paradox,2 is to have enough mobility to foster extreme rotations while maintaining sufficient stability to prevent subluxation of the humeral head. In addition, the shoulder must withstand large repetitive forces during a pitch. Professional pitchers generate up to 92 N • m of humeral rotation torque, greater than the torsional failure limit in human cadaveric shoulders.3 During the development of young throwers, adaptive changes in shoulder anatomy have been observed. These anatomic changes are attributed to the exposure to the tremendous stresses of throwing during the skeletal maturation process. These factors must all be considered when evaluating and treating these athletes.
Kinetic Chain
In general, overhead athletes must preserve the kinetic chain that efficiently coordinates transmission of force from their legs and trunk to the force-delivery mechanism of their arm. The legs and trunk generate rotational and linear momentum, producing a significant portion of the energy in the overhead motion. For example, the legs and trunk are responsible for 50% to 55% of the total force generation and kinetic energy in the tennis serve.4 Numerous studies have demonstrated that poor flexibility or muscle imbalances throughout the kinetic chain are common in patients with shoulder injuries including shoulder impingement,5–7 rotator cuff tears,7,8 and instability.8,9 In one study examining physical features in 64 throwers with labral tears, 46 (72%) showed infraspinatus and teres minor weakness on resisted external rotation, 31 (48%) demonstrated lower back inflexibility, 28 (44%) showed trunk and hip core musculature weakness by failing a Trendelenburg test, and 25 (39%) had asymmetrically decreased internal rotation of the nondominant hip.10 Injuries to the foot and ankle, tightness of the muscles crossing the hip and knee joint, weakness of hip abductors and trunk stabilizers, and conditions altering spine alignment can all influence kinetic chain transmission.
More specifically, as the kinetic chain transmission of force is disengaged, the overhead athlete often increases lumbar lordosis during the acceleration phase, placing the arm behind the body and the scapular plane, in a figuratively described slow arm position.11,12 The shoulder is forced to assume a hyperabducted, externally rotated position that moves the arm out of the safe zone of glenohumeral angulation described by Jobe and colleagues13 This position creates a series of problems. Violent acceleration out of the late cocking position increases compression loads and shear and traction on the rotator cuff, glenoid, and capsulolabral complex. These forces can injure the posterior capsule, tear and peel the labrum off of the glenoid, tear and delaminate the rotator cuff, and tear and stretch the anterior restraints.
Baseball Pitching
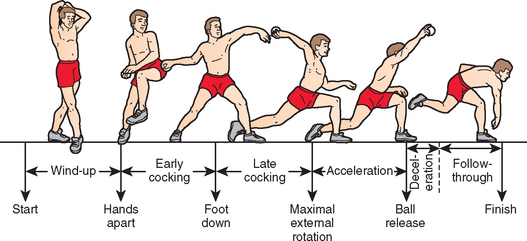
The phases of the baseball pitch have been extensively examined (Fig. 30-1). Most pitchers incorporate their own style into pitches, particularly during the wind-up and follow-through phases. Regardless of the look of the pitch during these phases, correct fundamental pitch mechanics are paramount during the entire pitch for effective throwing and prevention of injury. Improper mechanics at any stage during this energy transfer can lead to injury. An experienced coach educated in proper throwing mechanics is invaluable to the young athlete in preventing and recovering from injury by detecting and correcting subtle abnormalities in form. High-speed video evaluation gives pitchers concrete visual feedback about their technique. The following sections describe in more detail the correct mechanics of the separate pitching phases along with the poor form that can occur during each phase and its associated pathology.
Wind-Up
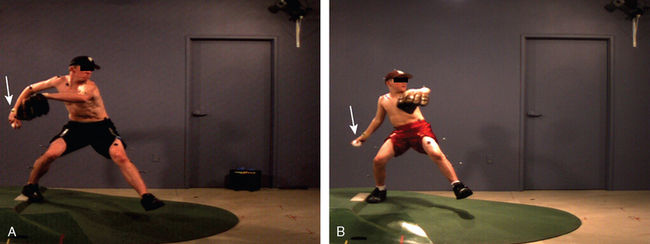
During the wind-up (Fig. 30-2A), the tone is set for the rest of the pitch, and poor mechanics in this phase can propagate through the rest of the pitch. The feet are positioned parallel to each other and perpendicular to the rubber on the mound while the pitcher faces the batter. The right-handed pitcher then places the right foot parallel to the rubber. The left leg is brought up, and the pitcher keeps the hips level with the ground and points them toward home plate, while maintaining good balance. The hips begin driving forward toward the plate (Fig. 30-3A). The right hand with the ball then exits the left hand glove. Inexperienced throwers often have flawed form with poor trunk tilt and less hip advancement (see Fig. 30-3B) toward home plate.
Early Cocking
The hand comes out of the glove while maintaining a position on top of the ball. The shoulder remains internally rotated (see Fig. 30-2B). As the hand brings the ball back and lateral, the shoulder is elevated in the scapular plane past 90 degrees and externally rotated to approximately 45 degrees. The hips are driven toward home plate but the pelvis does not rotate. The phase ends with the left foot landing on the mound, which decelerates the driving lower extremity and trunk.
Two common errors should be avoided in this phase: “pie throwing” and “opening up” too soon. First, if the hand is rotated under the ball (the pie-throwing position seen in Fig. 30-4B) instead of remaining on top (see Fig. 30-4A), the humerus externally rotates and places the humeral head in a vulnerable position for anterior subluxation and instability. Second, the lead foot should land pointing toward home plate (Fig. 30-5A). Flaws observed in inexperienced pitchers include abduction of the lead leg when landing on it. For example, a right-handed pitcher with poor form would place the lead left foot on the first-base side of the mound (see Fig. 30-5B). This opening up too soon causes premature pelvis rotation with a consequent loss of velocity and increased anterior shoulder strain.1,14 Movement of the high-mass lower extremity and trunk creates maximal energy in the lower body that is transferred to the upper extremity and finally to the ball. This requires timed and delayed upper body rotation to allow lower extremity and trunk energy to develop.
Late Cocking
The left foot hits the ground pointing in the direction of home plate, leaving the legs stretched apart (see Fig. 30-2C). The weight of the body is evenly distributed on both legs, and the torso balances in an upright position between the legs. Trunk rotation is delayed as long as possible while the right humerus externally rotates from about 45 degrees to 170 degrees in its position in the scapular plane At this time, the periscapular muscles, including the trapezius, rhomboids, levator scapulae, and serratus anterior, keep the scapula in optimal position, and the biceps keeps the elbow flexed at a little more than 90 degrees. Eccentric contraction of the subscapularis muscle decelerates the externally rotating humerus.
Most injured pitchers experience pain during the late cocking phase. During this phase, at maximal external rotation (nearing 170 degrees), the arm should be abducted 90 to 100 degrees. Throwing with reduced external rotation at the time of foot contact has been shown to increase strain on the anterior shoulder during acceleration and ball release.
Periscapular muscles can affect shoulder pathology during the late cocking phase. The serratus anterior is significantly less active in pitchers with shoulder instability than in pitchers with normal shoulders.15 To compensate for diminished serratus anterior strength, the thrower might drop the elbow, thus decreasing the degree of scapular rotation and elevation needed. If the pathologic process continues, the player might attempt to compensate further by moving the humerus behind the scapular plane. If symptoms arise, the player decreases the amount of external rotation so as to protect against pain and arches the back into hyperlordosis as a way of compensating for the decreased humeral external rotation. Early recognition of muscle imbalances such as these in the thrower can allow the surgeon to institute an early, focused physical therapy program to strengthen the affected structures and fight against a vicious cycle of compensatory pathologic throwing.
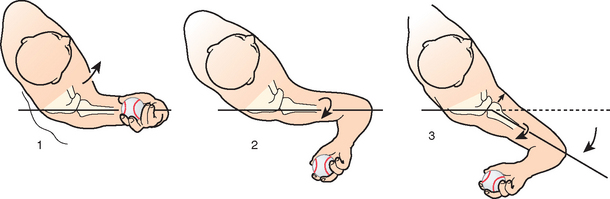
The elbow should reach its highest point in late cocking (Fig. 30-6A); immature throwers often have their elbows in a suboptimal lower position (see Fig. 30-6B).
Acceleration
Once the humerus reaches maximal external rotation, the hand carrying the ball accelerates in a rapid arc of internal rotation (see Fig. 30-2D). The lower extremity and trunk energy is transferred through the shoulder to the elbow and wrist as the body falls forward. Just before ball release, the arm internally rotates 80 degrees, reaching peak angular velocities near 7000 deg/sec. Within 0.05 seconds, the ball is released with speeds exceeding 90 mph.16
Leading with the elbow, or decreasing horizontal abduction while increasing elbow flexion to bring the ball closer to the shoulder, might also be employed by the pitcher with a painful shoulder during the acceleration phase. Although this maladaptive position decreases the load on the shoulder, it increases the load on the medial elbow, predisposing it to injury.1 If the thrower opens up too quickly, positioning the elbow behind the plane of the scapula, then the glenohumeral joint hyperangulates, resulting in more-pronounced internal impingement (Fig. 30-7).
Deceleration
After the ball is released, the right hip rises up and over the left leg. The right foot lifts off the mound and the body does a controlled fall forward (see Fig. 30-2E). During this phase, the teres minor, infraspinatus, and scapular rotator muscles contract eccentrically to dissipate kinetic energy that was not imparted to the ball. The glenohumeral distraction force at this time, absorbed by the capsule and posterior rotator cuff, reaches 1 to 1.5 times body weight.17
Follow-through
The arm continues to descend, and the right leg lands on the ground in a controlled fashion (see Fig. 30-2F). Eccentric contraction by the scapular rotator muscles continues to decelerate the arm, and the posterior capsule experiences tension as the arm adducts. During the follow-through, the shoulder should internally rotate and horizontally adduct across the body. If the arm ends up facing home plate instead, increased stresses will act on the shoulder.
Tennis
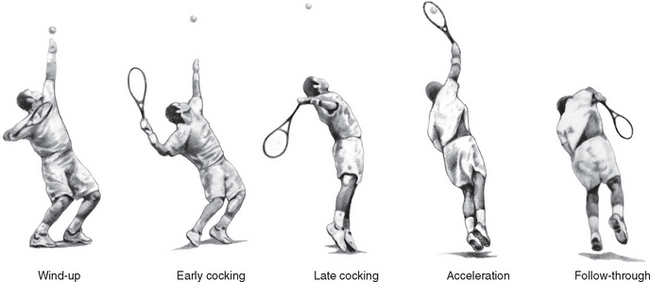
The tennis serve has five different phases (Fig. 30-8), similar to the baseball pitch: wind-up (the knees are flexed and the trunk is rotated), early cocking, late cocking (where the shoulder is maximally abducted and externally rotated), acceleration, and follow-through.
Swimming
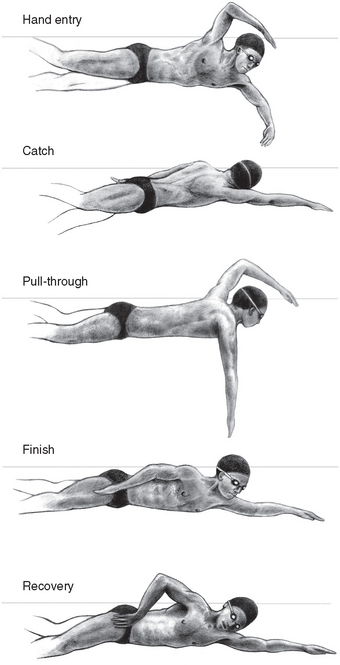
The demands on the shoulders of competitive swimmers are immense, and the number of strokes exceeds 500,000 per arm per year.18 The freestyle swimming stroke has been subdivided into five distinct phases: hand entry, catch, insweep, finish, and recovery (Fig. 30-9). Swimming strokes repetitively place the shoulder in the impingement position described by Neer and Welsh.19 Consequently, shoulder pain and dysfunction in swimmers has traditionally been equated with subacromial impingement and rotator cuff tendinitis.
More-recent biomechanical analyses of shoulder function have found that swimmers suffer from a variety of problems common to all overhead athletes.20 Impressive shoulder laxity is observed in swimmers, placing them in the spectrum of multidirectional instability, and is a consequence of tremendous forces on soft tissue stabilizers and extreme motion requirements combined with swimmers’ propensity for baseline ligamentous laxity. Associated muscle imbalances, therefore, can contribute to pathologic instability processes in these shoulders. As in throwing, the swimmer’s shoulder must maintain the narrow margin between having enough flexibility to generate body propulsion and developing frank instability. Proper strength and coordination of the dynamic scapular stabilizers (levator scapulae, rhomboids, trapezius) and glenohumeral stabilizers (rotator cuff) are critical to prevent symptomatic instability.
Swimming Phases
Hand Entry
Yanai and Hay have recommended four technique changes to reduce impingement during this phase. The first three–streamlining hand entry, strengthening muscles that resist forcible elevation (latissimus dorsi, pectoralis major, teres major, biceps brachii), and bending the elbow to decrease moment arm length–all decrease the forcible moment arm. The fourth involves externally rotating the scapula on hand entry to decrease the angle subtended by the axis of the humerus and the superior border of scapula, lessening subacromial impingement.21,22
Catch
During the catch phase, the shoulder is adducted and internally rotated. A common technical fault during this phase is the dropped elbow. Counsilman and coworkers demonstrated that the dropped-elbow stroke combines external rotation and adduction at the shoulder, whereas the correct high-elbow technique combines internal rotation with abduction.23 Richardson found that the increased glenohumeral external rotation placed the muscles of propulsion (latissimus dorsi and triceps) at a mechanical disadvantage.24
Although the correct high-elbow technique does improve mechanical advantage, it also increases the percentage of the stroke during which the shoulder is left in the impingement position.22 Swimmers might adopt the faulty dropped-elbow technique at the onset of incipient impingement in an attempt to curtail pain during the stroke (or secondary to fatigue). Accordingly, biomechanical studies have measured decreased activity in the anterior and middle deltoids when the elbow is dropped, suggesting that the faulty technique uses less energy.25
Insweep
As the hand reaches the deepest point, the downward motion shifts to an upward, inward, and backward motion, and the hand pushes toward the midline of the body and toward the swimmer’s chest. Problems in this phase relate to the stabilizing periscapular muscles, particularly the serratus anterior in the overhead motion. In the swimmer with a painful shoulder, serratus anterior muscle activity drops considerably.25 This is likely secondary to fatigue due to constant splinting of the painful shoulder. The rhomboids attempt to stabilize the scapula, but because they are, in fact, antagonists of the serratus anterior, normal synchronous scapular rotation is disrupted.
Recovery
The recovery phase begins with the hand exiting the water. As the hand exits the water, the shoulder abducts and externally rotates as it is brought forward for arm entry. Shoulder impingement occurs during a large part of this phase, particularly if the shoulder is kept internally rotated.22 Codman first described the prerequisite of externally rotating the shoulder in order to achieve full abduction.26 Otherwise, the greater tuberosity comes into contact with the acromion at about 90 degrees of abduction. Externally rotating as early as possible in the recovery phase decreases the amount of time that the shoulder spends in an impingement position.21,22
Instability
The biomechanics of swimming favors swimmers with higher degrees of shoulder laxity.27 As a result of this self-selection, elite swimmers tend to be hyperlax at baseline and are more at risk for shoulder pathology related to it.28 Fine-wire electromyography (EMG) studies have demonstrated that swimming strokes require the shoulder adductors and internal rotators to produce the majority of propulsive force, and they minimally tax the external rotators.29–33 Therefore, like throwers, swimmers and water polo players significantly increase their internal rotator and adductor–to–external rotator and abductor strength ratio.30,31 Whereas a normal shoulder might compensate for these muscle imbalances, a shoulder with excessive laxity might not be able to. As a result, the glenohumeral joint can have subluxation episodes, leading to other painful chronic injuries such as labral tears, subacromial impingement, and bicipital tendinitis.27,34
During the swimming stroke, the force applied to the hand by the water results in an anteriorly directed vector thrust at the shoulder.27 In a lax shoulder, this force can shift the humeral head excessively, injuring the labrum or the joint surface itself. The external rotators attempt to restrain the humeral head from anterior translation, becoming fatigued and prone to develop tendinitis. Some authors have cited overworked external rotators as a cause of the posterior shoulder pain commonly seen in swimmers with anterior instability.27 A rehabilitation program aimed at maintaining normal rotator cuff strength ratios and periscapular muscle strengthening is the mainstay of treatment and has been effective in ameliorating pain and dysfunction.35 Open and arthroscopic surgical stabilization treatments for elite swimmers with sympto-matic instability have not been as successful as for other athletes with instability.
Impingement
Swimmer adaptations to this provocative shoulder arc of motion can affect pathology and convalescence. For example, unilateral breathing increases impingement on the shoulder ipsilateral to the breathing side.21 Having the swimmer switch to bilateral breathing can decrease the risk of developing clinical symptoms. Maintaining a high elbow on recovery, avoiding an extended position of the arm before hand entry, and increasing body roll all also decrease the percentage of the stroke that the shoulder is in the impingement position. Other conservative measures, such as rest, during which a kickboard can be implemented, ice, nonsteroidal antiinflammatory drugs (NSAIDs), and a structured rehabilitation program usually yield successful results. Refractory cases might respond to subacromial decompression, although this is not routinely done.36,37
Golf
Chronic shoulder overuse injuries can affect golfers, especially because elite-level and some recreational players perform up to 2000 swings per week.38 Ninety percent of shoulder problems in golfers involve the lead arm (the left arm in a right-handed golfer).39,40
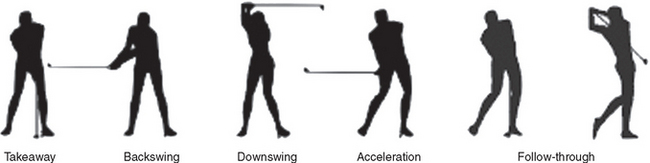
The golf swing is divided into five phases (Fig. 30-10): the takeaway (from address until the club is horizontal), the backswing (from horizontal to the top of the backswing), the downswing (from top of backswing until the club is horizontal), acceleration (from horizontal club to impact), and follow-through (from ball contact until end of swing).41
Repetitive swinging of the golf club can eventually overwhelm normal shoulder restraints, especially when performed incorrectly or erratically. Fine-wire EMG studies have demonstrated that whereas professional golfers consistently activate the same sequence of muscles with every swing, recreational golfers tend to produce different muscle-activation patterns and do not duplicate their swing with each shot.40,42 The following section presents the most typical golf injuries affecting the shoulder.
Subacromial Impingement and Rotator Cuff Injury
The golfer’s lead shoulder is placed in the position of impingement at the extremes of motion: the top of the backswing or the end of follow-through. Furthermore, a patient who already has preexisting rotator cuff dis-ease has a weak takeaway, which can exacerbate poor swing mechanics and worsen impingement. During the backswing, the lead shoulder is subjected to subacromial impingement, acromioclavicular compression, and, less commonly, coracoid impingement. During the downswing, impact, and follow-through, the trailing shoulder is subject to stress on the superior labrum, coracoid impingement, and humeral head chondral injury.
Several reports have examined impingement in golfers. In those with golf-related shoulder symptoms, studies have found rotator cuff or subacromial disease in 26%43 to 93%44 of patients. Although one study suggested that surgical treatment for rotator cuff tears in overhead athletes did not consistently return these athletes to their previous level of play, golfers may be more amenable to successful surgical treatment compared with other overhead athletes, such as throwers, because of the relatively lighter demands placed on their shoulders. Vives and colleagues found that of 29 recreational golfers with subacromial disease and rotator cuff tears, acromioplasty and mini-open repair returned all but 3 patients to playing with their previous handicaps and driving distances within 3 years.45 Another case report describes successful arthroscopic subacromial decompression for impingement in a professional golfer that allowed him to return to competitive play.38
Acromioclavicular Joint Disease
Acromioclavicular joint disease is also prevalent in golfers. Those who complain of symptoms cite the top of the backswing, when the lead arm assumes a cross-body adduction position and compresses the acromioclavicular joint. In a study of 35 elite golfers, of whom about half had acromioclavicular joint arthritis, all but 1 returned to competitive play after treatment.43 Treatment consisted of physical therapy, swing modification, or, in refractory cases, distal clavicle excision.
Glenohumeral Instability
Golfers can be susceptible to glenohumeral instability, especially because generating a powerful swing requires maximizing the shoulder turn relative to the hip turn.46 Posterior instability has been described, occurring in up to 12% of golfers with shoulder pain. Some authors have hypothesized that in these patients, the subscapularis is relatively stronger than the rest of the rotator cuff, rendering the glenohumeral joint susceptible to posterior forces, worsened by fatigue to the serratus anterior.47 Symptoms of pain and instability appear in the lead arm at the top of the backswing, when it is placed in maximal adduction.
Physical examination findings in these patients demonstrate posterior instability on load and shift and posterior apprehension with loading in internal rotation and adduction. Smaller case series have described successful treatment of posterior instability with therapy, posterior capsulorrhaphy, and subacromial decompression, if indicated.47 A posterior labral (reverse Bankart) lesion has been successfully treated with arthroscopic repair.48 Although the patient did not demonstrate signs of posterior instability, he did report pain on posterior load and shift and posterior apprehension tests.
Anterior instability may also occur in golfers, particularly with the lead arm in the follow-through phase of the swing, when it is in maximal abduction and external rotation. Physical therapy consisting of rotator cuff and scapular stabilizer strengthening is often successful in treating this entity in golfers,38,39 with surgical treatment reserved for refractory cases.38
Superior Labrum and Biceps Disease
Superior labrum anterior and posterior (SLAP) lesions and biceps tendon disorders occurring in golfers have not been extensively reported in the literature, but they do occur.41 Patients with SLAP tears complain of pain in the lead shoulder at the end of the backswing or beginning of the downswing, when the shoulder is loaded and the arm is adducted across the body. Occasionally, the golfer complains of mechanical symptoms such as clicking or catching. Isolated biceps tendinitis causes anterior shoulder pain during the end of follow-through when the lead arm shoulder is extended, maximally abducted, and externally rotated.
Arthritis
Up to 25% of golfers in the United States are 65 years or older, and thus glenohumeral arthritis is a common condition in the golfer population. Total shoulder arthroplasty has been successful in returning golfers to their sport. One study found that 23 of 24 patients were able to resume playing golf at an average of 4.5 months after surgery, the majority actually improving their scores at an average of 53 months of follow-up and without component loosening.49
ASYMPTOMATIC THROWING SHOULDER ADAPTATION
Overall Motion
The dominant shoulder of a thrower exhibits adaptive changes. It is well documented that in a thrower, with the shoulder abducted to 90 degrees, external rotation significantly increases as much as 10 degrees compared to the contralateral arm, and internal rotation is diminished, a finding that has been branded glenohumeral internal rotation deficit (GIRD).2,50–56 The gain in external rotation is often associated with an equal loss in internal rotation. In asymptomatic throwers, therefore, the total arc of shoulder motion is maintained, but it is shifted in external rotation by 10 degrees.57–59 Controversy exists regarding the anatomic changes that are responsible for the observed glenohumeral rotation changes, with studies examining soft tissue and bone adaptations.
Bone Adaptations
Developmental changes in the proximal humerus occur in young throwers. Mair and colleagues found that 55% of asymptomatic and 62% of symptomatic skeletally immature baseball players had radiographic evidence of physeal widening.60 Krahl and coauthors observed that pitching arms had a significant increase in humeral length.61 The developmental bone changes also include increased humeral retroversion, shifting the shoulder arc of motion in young throwers, with the greatest change occurring in those aged 13 to 14 years.57 These early changes lead to permanent change in proximal humerus anatomy. Crockett and colleagues62 showed that professional pitchers’ dominant shoulders have 17 degrees of greater humeral retroversion compared to their nondominant shoulders.71
Because the normal humeral retroversion angle actually decreases from 78 degrees to 30 degrees during development, Yamamoto and colleagues63 hypothesized that repetitive throwing did not increase retroversion in dominant shoulders but, rather, restricted the physiologic derotation of the humeral head during growth.64–66 Humeral osseous adaptation, therefore, may explain the decrease in internal rotation and the majority of the increase in external rotation in asymptomatic throwers.
Capsuloligamentous Changes
Posterior Capsular Contracture Theory
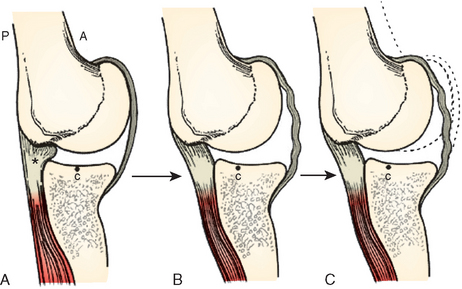
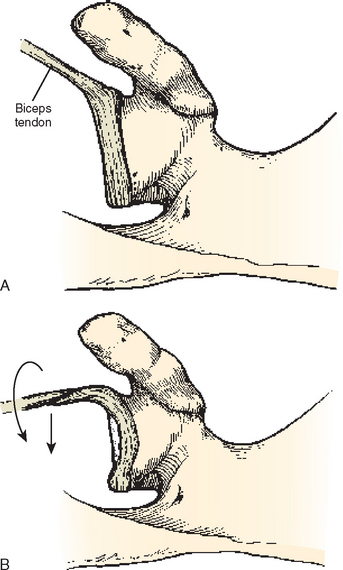
Burkhart and colleagues have proposed that a fundamental adaptation in throwers is a posterior capsular contracture that, though initially asymptomatic, can eventually have significant pathologic implications. They reason that in the overhead thrower, the posterior capsule must withstand tensile forces of up to 750 N during the deceleration and follow-through phases.67 These posterior tensile forces are resisted by the eccentric contraction of the rotator cuff, primarily the infraspinatus, and by the posteroinferior capsule (posterior band of the inferior glenohumeral ligament) (Fig. 30-11). With repetitive infraspinatus eccentric contraction during deceleration and follow-through, the muscle belly loses active tension, gains passive muscle tension, and develops disturbed proprioception.68 As a result, higher loads are imposed onto the posteroinferior capsule which then becomes hypertrophied and stiffer.
The theory proposes that this posterior contracture shifts the center of rotation of the shoulder to a more posterosuperior location, creating posterosuperior instability and functional consequences for the shoulder in abduction and external rotation. Grossman and colleagues69 created a posterior capsular contracture in a cadaveric model and found that the shoulder center of rotation did in fact shift posterosuperiorly in abduction and external rotation, allowing increased clearance of the greater tuberosity over the posterior glenoid rim. The humeral head can consequently externally hyperrotate, producing increased shear in the rotator cuff tendon and more pronounced internal impingement.
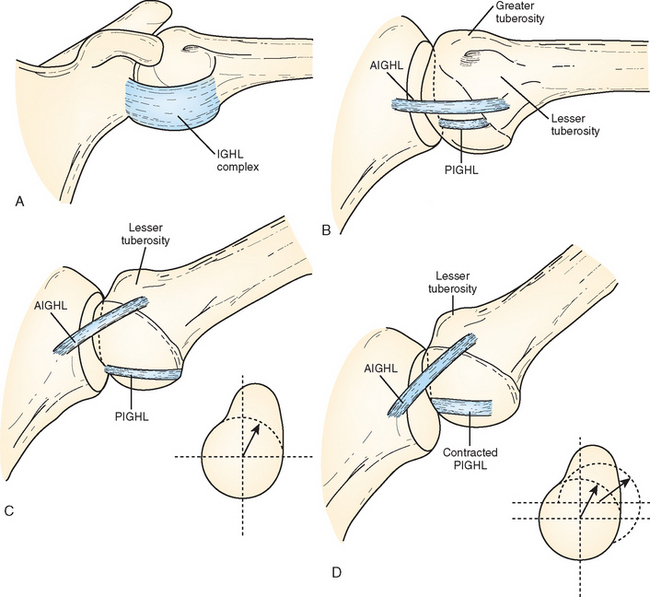
The rationale for this hypothesis is based on O’Brien’s concept of the inferior glenohumeral ligament complex (Fig. 30-12) acting as a hammock to support the humeral head with the arm in abduction.70 In abduction and external rotation, the posterior band of the inferior glenohumeral ligament is shifted under the humeral head. Posterior band contracture exerts a posterosuperior force on the humeral head, shifting it in that direction. The shift creates a relative anteroinferior capsular redundancy. The net effect of the capsular changes (contracted posterior capsule and relative lengthening of the anteroinferior capsule) and the posterosuperior humeral head shift is increased external rotation and decreased internal rotation. Nevertheless, other studies have documented significant posterior laxity instead of tightness in throwers,59,62,71,72 supporting the idea that GIRD likely arises from both ligamentous and osseous adaptations.62
Adaptive Capsular Laxity Theory
Other authors believe that repetitive shoulder microtrauma to the anterior capsule, particularly during the cocking phase of throwing, can lead to stretched anterior capsuloligamentous structures. The stretched anterior capsule allows the greater external rotation routinely seen in overhead throwers and can also lead to symptomatic anterior microinstability.52–54 These authors attribute the loss of internal rotation to two entities: the aforementioned osseous adaptation of the humerus and posterior muscle tightness arising as a result of eccentric posterior muscle contraction during the deceleration phase of thowing.62
Several studies have quantified capsular laxity in the context of throwing. Sethi and colleagues found an increased anteroposterior glenohumeral translation in pitchers’ dominant shoulders of more than 3 mm compared to the nondominant arm.59 Borsa and colleagues found that posterior translation was consistently greater than anterior translation in the thrower’s dominant shoulder.71,73 These studies suggest that throwing shoulders are generally lax instead of stiff and contradict the theory that posterior capsular tightness is a universal phenomenon in the asymptomatic thrower.
Muscle Strength and Proprioception
Pitchers have been shown to exhibit decreased external rotation strength and increased internal rotation strength in their dominant shoulder compared to their nondominant one.74–76 Magnusson and coworkers77 showed that professional baseball pitchers had weaker external rotation and supraspinatus strength in their throwing shoulder compared to both their nondominant shoulder and the dominant shoulder of age-matched unathletic controls. Some authors have proposed that if external rotator muscle strength is not between 65% and 75% of internal rotator strength, the glenohumeral joint becomes unbalanced and destabilized during throwing.76,78 Periscapular musculature also responds to repetitive throwing. Most throwers have hypertrophied scapular elevator and protraction muscles on their throwing side.
It has been shown that proprioception is significantly diminished in shoulders with excessive laxity.79 However, in these same shoulders, proprioception is heightened to at least normal levels in extreme external rotation.2,80 Elite pitchers retain a proprioceptive sense of the degree of external rotation (the slot) they must achieve to produce the required pitch velocity.
Scapulothoracic Motion
The scapula plays a critical role in transferring energy from the trunk to the humerus. In the asymptomatic thrower, adaptive scapulothoracic changes leading to scapular asymmetry have been described.2,81–84 Altered static and dynamic scapular mechanics arise from overuse and weakness of scapular stabilizers and posterior rotator cuff muscles.17 The major findings are as follows: With the arm hanging at the side, the throwing shoulder’s scapula has increased upward rotation (abduction), internal rotation (protraction), ante-tilting in the sagittal plane, and inferior translation (Fig. 30-13). During forward arm elevation, the scapula upwardly and internally rotates and retracts. Scapular upward rotation has been theorized to be a key adaptation to the cocking phase of throwing. During cocking, when the humerus is termi nally externally rotated and abducted, upward scapular rotation helps maintain glenohumeral articular congruency.84 This altered scapular positioning, though initially asymptomatic, can nevertheless predispose the shoulder to injury.
THROWING SHOULDER CONDITIONS
Various paradigms and terms have been used to describe the constellation of injuries and pathologic syndromes in the throwing shoulder. The concepts of instability and impingement apply uniquely to the thrower’s shoulder. Instability and internal impingement in throwers should be viewed as syndromes of collective common pathologies occurring in the static and dynamic stabilizing elements of the shoulders that ultimately lead to pain with throwing. The injury cascade tends to form a continuum of pathology and pathomechanics. Although when viewed independently, some of the current popular theories regarding the etiology of specific throwing-related shoulder injuries might seem at odds with each other, they complement each other when they are considered as elements of a pathologic continuum.
Tissue pathology in the throwing shoulder occurs secondary to repetitive microtrauma, which causes attrition and gradual failure. Typical sites of pathoanatomy are observed: the superior and posterior-superior labrum, the articular surface of the supraspinatus and infraspinatus, and the posterior capsule. Our current understanding of conditions of the throwing shoulder is the result of biomechanical analysis of sports-specific shoulder motions, intraoperative correlation with symptoms, and imaging and clinical studies reporting the outcomes of different treatments.1,11,53,54,67,85
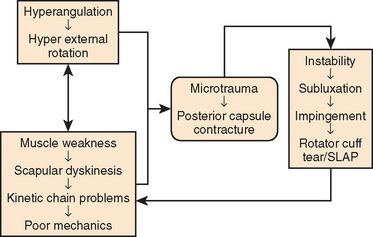
Injury to the thrower’s shoulder joint occurs most commonly during the late cocking or early acceleration phases. When pain or symptoms disturb the throw’s acceleration, velocity, or efficacy, the symptomatic shoulder has been labeled a dead arm.67 Historically, the cause of the dead arm has been ascribed to a multitude of pathologic processes. These have included psychiatric disease involving voluntary dislocators,86 acromial osteophytes,87 coracoacromial impingement,88 rotator cuff tendinitis and tears,89 biceps tendinits,90 acromioclavicular joint pathology,91 microinstability52,92 posterior glenoid calcifications,93,94 and SLAP lesions. At present, the exact etiology and sequence of injury in throwers has not been confirmed in vivo. However, recent evidence shows that a combination of abnormal scapulothoracic and glenohumeral motion can injure the superior and posterosuperior labrum as well as the undersurface of the rotator cuff and posterior capsule.1,2,53,54,67,95 Several distinct processes appear to play a role in the development of throwing pathology, and the process has been considered a continuum (Fig. 30-14).
Internal Impingement
Walch and colleagues95 initially described internal impingement as occurring in the 90-degree abducted and 90-degree externally rotated position. In this position, the posterosuperior rotator cuff presses against the posterosuperior glenoid labrum and can be pinched between the labrum and greater tuberosity (Fig. 30-15). Although physiologic in a static position, excessive contact of the undersurface of the rotator cuff and the superior labrum during overhead activity can lead to partial-thickness rotator cuff tears and SLAP lesions.53,95–98 Labral and undersurface rotator cuff lesion commonly coexist in throwers. Andrews and coauthors99 noted that labral tears were present in 100% of 36 competitive athletes with articular-sided partial-thickness rotator cuff tears of whom 64% were baseball pitchers. Guidi and colleagues100 found superior labral fraying in 90% of patients with partial-thickness rotator cuff tears.
Initially, Jobe extrapolated internal impingement to throwing athletes and detailed a spectrum of injury that included rotator cuff, glenoid labrum, and bone pathology.53 He also suggested that with repetitive throwing, internal impingement might be aggravated by gradual stretching of the anterior capsuloligamentous structures, and he recommended anterior capsulolabral reconstruction when surgery was indicated.53,54,101
Some authors have questioned the pathologic implications of internal impingement in throwing athletes. Some believe that if impingement is pathologic, it should occur in nearly all throwers, which it does not.102 Moreover, they have argued that the existence of internal impingement is physiologic and that it is instead the loss of internal rotation allowing hyperexternal rotation with fatigue failure of rotator cuff fibers, that can lead to a pathologic state.103 Others have pointed to a significant coexistence of undersurface rotator cuff tears and labral fraying (73.3%) in nonoverhead athletes as evidence that internal impingement might not be a phenomenon unique to throwers.104
Posterior Capsular Contracture
The theory describing adaptive changes to the posterior capsule has been outlined earlier. In the context of throwing pathology, the contracture initiates a cascade that some authors believe explains most overhead arm pathology. Once posterosuperior instability is present, and the humeral head is shifted posterosuperiorly, kinetic chain dynamics are affected. The arm loses even more internal rotation, and arm acceleration and therefore ball velocity is lost. Over time, posterior SLAP tears can occur from posterosuperior contact of the labrum and the greater tuberosity. The posterior cuff undersurface begins to fail, and the picture of internal impingement arises. With continued throwing, attenuation of the anterior capsule occurs, leading to eventual permanent deformation and anterior microinstability in a small cohort of usually older patients.17
Glenohumeral Internal Rotation Deficit
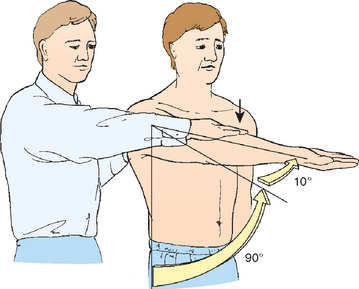
As described in the discussion on shoulder adaptations to throwing, with time, the throwing shoulder develops increased external rotation and disproportionately decreased internal rotation (GIRD). By convention, glenohumeral rotation is measured with the patient either supine or sitting and with the shoulder abducted 90 degrees in the plane of the body. The scapula must be stabilized either against the examination table, if the patient is supine, or by the examiner’s hand, if the patient is sitting. Glenohumeral rotation is then measured up to the point that the scapula begins to move on the posterior chest wall or provides resistance (Fig. 30-16). Failure to stabilize the scapula incorporates scapulothoracic motion into the total rotational arc, leading to confounding measurements.
GIRD resulting in a loss of total rotational arc of greater than 20 degrees compared to the contralateral side puts the shoulder at risk for injury.67,81 Indeed, severe GIRD is more prevalent in symptomatic shoulders. Verna studied 39 professional pitchers with GIRD greater than 35 degrees (25 degrees or less of total internal rotation) during a baseball season.105 He found that 60% of them developed shoulder problems that required them to stop pitching. Kibler found that in a case series of overhead athletes with arthroscopically proven type 2 SLAP lesions, severe GIRD (average, 33 degrees; range, 26-58 degrees) was present in all of them.67
Symptomatic GIRD likely has a component of posterior capsular or muscular contracture. In a prospective study, Kibler and colleagues reported that tennis players who performed daily posterior-inferior capsular stretching to minimize GIRD increased their dominant shoulder internal rotation and had a 38% decreased incidence of shoulder problems compared to those in a control group who did not stretch.106,107 Burkhart and coworkers reported that 90% of throwers with symptomatic GIRD (>25 degrees), and almost all young collegiate or high school athletes, respond well to a posteroinferior capsular stretching program (over as little as 2 weeks) and decrease GIRD to an acceptable level (defined as either <20 degrees or <10% of the total rotation in the nonthrowing shoulder).67
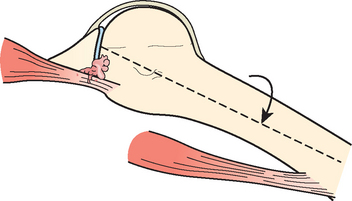
Peel Back
With the arm in the externally rotated and abducted position, the biceps is brought into a more posterior and vertical position. With further external rotation it transmits a torsional force to the posterior labrum, peeling it back. (Fig. 30-17) This peel-back phenomenon has been observed reliably in throwers with posterior and combined anteroposterior SLAP lesions.108 With repetitive throwing, the biceps tendon can further peel the biceps anchor off the glenoid lip. Panossian demonstrated in a cadaver model that creation of a type II SLAP lesion resulted in increases in both humeral internal-to-external rotation and anterior-to-posterior translations.109 After arthroscopic repair, total range of motion, internal rotation, external rotation, and translation significantly decreased, returning to expected values. These findings suggest that type II SLAP lesions cause significant glenohumeral instability, which can be effectively treated with current arthroscopic repair techniques.
SICK Scapula and Scapular Dyskinesis
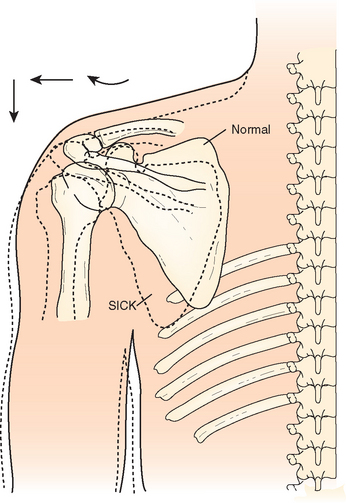
The scapula has three main functions during throwing that maximizes force transmission from trunk and torso to the humerus while avoiding risk of labral and rotator cuff injury.90 First, it must optimize the position of the glenoid with respect to the rapidly rotating humeral head. Second, it must fluidly retract and protract around the thoracic wall as the arm moves through the phases of throwing, maintaining a safe zone of glenohumeral angulation. Third, it must act as a stable base for the origin of the extrinsic and intrinsic shoulder muscles that provide glenohumeral compression and regulate arm motion. These functions require optimal strength and coordination of the periscapular muscles. Weakness, inflexibility, or imbalance of the periscapular and posterior rotator cuff muscles disturb the normal anatomic static and dynamic relationships of the scapula. The abnormally positioned thrower’s scapula has been labeled SICK scapula (scapular malposition, inferior medial border prominence, coracoid pain, and dyskinesis of scapular movement) by Burkhart and colleagues.11 Aberrant scapulothoracic motion has been called scapular dyskenesis.81,110
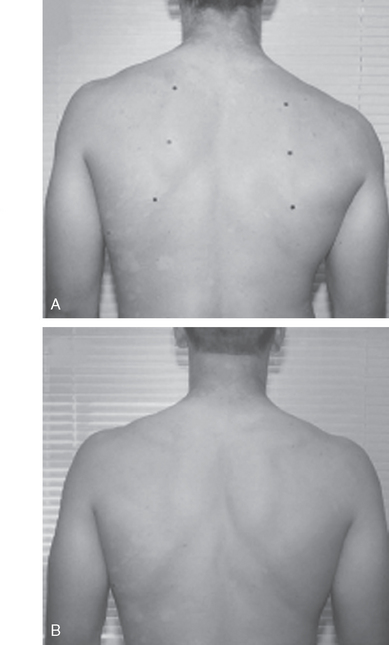
The SICK scapula is an extreme form of scapular dyskinesis. Morgan has also used the term SICK scapula to specifically define the static asymmetrical position of the thrower’s scapula, in contrast to scapular dyskinesis, which describes abnormal scapular motion.17 The hallmark of the syndrome is an asymmetrically drooping throwing shoulder and medial scapular winging (Fig. 30-18A). The scapular malposition is a combination of four changes in position: upward tilting, protraction, forward tilting in the sagittal plane, and inferior translation. Burkhart and colleagues have described three different subtypes of this syndrome depending on which structures are fatigued. The first two are associated with posterosuperior labral tears and internal impingement, and the third one has been associated with rotator cuff tears. Type I stems from weak lower trapezius and serratus anterior muscles and inflexibility of pectoralis major and minor. This causes inferomedial scapular winging at rest and greater winging on cocking. Type II is predominantly caused by upper and lower trapezius and rhomboid weakness and does not have a large inflexibility component.11 It is identified by complete medial winging at rest which also worsens with cocking. Type III is associated with impingement lesions and has superomedial winging of the scapula.
The SICK scapula predisposes the shoulder to labral and rotator cuff tears because the scapula sits in a more protracted and upwardly tilted orientation, positioning the glenoid so it faces more anterior and superior. This position leads to three developments: anterior tension, posterior compression, and increased glenohumeral angulation. First, with glenoid protraction, the anterior band of the inferior glenohumeral ligament tightens, limiting anterior translation of the humeral head and, over time, becoming susceptible to chronic strain.9 Second, simultaneously, the posterior edge of the glenoid is brought toward the humerus, placing the posterosuperior labrum and rotator cuff at risk for injury. Finally, excessive protraction increases glenohumeral angulation. The thrower with increased glenohumeral angulation will find that the arm lags behind the body.
Excessive external rotation in this setting has two deleterious consequences: It exacerbates the aforementioned biceps peel-back effect11 and, with preexisting scapular protraction, external rotation and abduction produce posterosuperior glenoid impingement.81,82 One study examined throwers with proven posterosuperior labral tears and found that a total of 60 out of 64 (94%) had patterns of dynamic scapular dyskenesis.10
A cascade of events has been described that explains many pathologies associated with the SICK scapula: coracoid pain due to pectoralis minor traction tendinopathy, superior medial angle scapular pain from levator scapulae insertional tendinopathy, subacromial origin pain from acromial malposition and decreased subacromial space from upward tilting, acromioclavicular joint pain caused by anterior joint incongruity, sternoclavicular pain, thoracic outlet syndrome radicular pain, and subclavian vascular problems such as arterial pseudoaneurysm or venous thrombosis.17
Treatment for SICK scapula consists of scapular stabilizer muscular strengthening, and reeducation.11,17,107,111,112 The kinetic chain is incorporated into the rehabilitation. The involved side is addressed first using closed-chain exercises followed by open-chain exercises. Scapular rehabilitation has been successful in returning patients with SICK scapula to their previous level of competitive play (see Fig. 30-18B).
EVALUATION OF THE OVERHEAD ATHLETE
Examination
Palpation
Several structures can be easily palpated, including the glenohumeral joint lines, the acromioclavicular joint, the long head of the biceps tendon, and the coracoid process. Tenderness over the acromioclavicular joint indicates acromioclavicular joint pathology. Tenderness over the long head of the biceps tendon suggests tendinitis or a SLAP tear. Coracoid process tenderness suggests pectoralis minor tendinitis or tightness, which has been correlated with scapular protraction and dyskenesis.11
Range of Motion
Examination of the scapula should include observing cervical and thoracic posture, scapular symmetry at rest and on ascending and descending arm motion in both flexion and abduction, active scapular retraction and elevation, and lateral slide measurements. The latter, devised by Kibler,81 measures scapular asymmetry by comparing the distance from the inferior angle of the scapula to the spinous process of the thoracic vertebra in the same horizontal plane (the reference vertebra) in three test positions. In position 1, the arm is at the side. In position 2, the humerus is internally rotated and abducted 45 degrees, as the hands are placed on the hips. In position 3, the shoulder is abducted farther to 90 degrees. An asymmetrical difference of greater than 1.5 cm determines a positive lateral scapular slide test.81
Strength
Manual muscle strength testing should aim to isolate the muscle being tested and compare the injured with the uninjured side. The supraspinatus can be isolated in the empty can position. The subscapularis is best assessed by either the lift-off test described by Gerber and Krushell113 or by the internal rotation lag sign, which is more sensitive.114
Internal Impingement
Apprehension Relocation
The patient is placed supine on a table. The shoulder is brought into the classic position of internal impingement (≥90 degrees of external rotation, ≥90 degrees of abduction). An anteriorly directed force applied on the posterior aspect of the shoulder will elicit pain but not apprehension. The pain is then relieved with a posteriorly directed force applied by the examiner’s hand on the anterior aspect of the shoulder.
Active Compression Test
The active compression test, also known as the O’Brien test (Fig. 30-19), unmasks pathology of the biceps and labrum complex. The shoulder is brought to 90 degrees of forward flexion and 15 degrees of adduction. Resisted forward elevation is then performed with the thumb pointing down (internal rotation) and with the thumb pointed up (external rotation). Deep pain in internal rotation but not in external rotation indicates a biceps–labrum complex problem. Pain on top of the shoulder is thought to be from acromioclavicular joint pathology.
TREATMENT
Posterior Capsule Contracture
Nonoperative Treatment
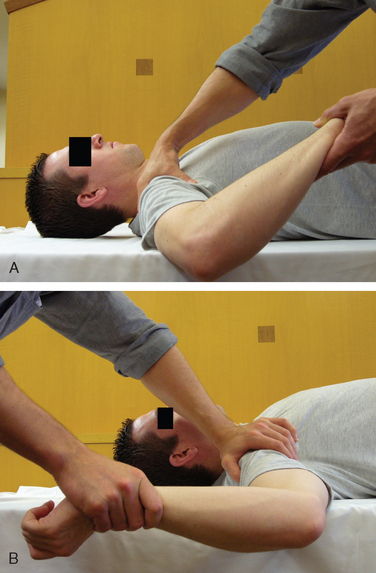
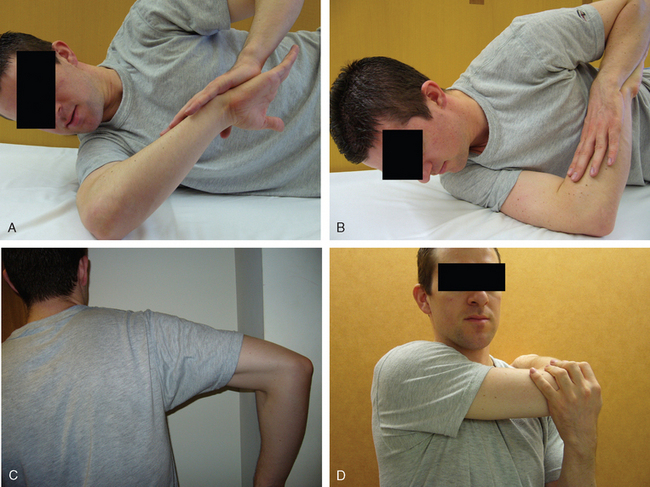
Nonoperative management has proved successful in managing excessive GIRD, reported as greater than 20 degrees.115 Some authors have detailed a series of exercises that, theoretically, improve posterior capsular contracture and fairly reliably decrease GIRD. These include sleeper stretches (Fig. 30-20) in which the athlete lies on one side with the shoulder in 90 degrees of flexion, in neutral rotation, with the elbow in 90 degrees of flexion as well. The shoulder is then passively internally rotated by pushing the forearm toward the table around the fixed point of the elbow.11
Other authors have recommended stretches to improve posterior shoulder flexibility, although they have cited posterior muscle contracture rather than capsule tightness as the component that requires stretching.2 These stretches include the internal rotation stretch and the horizontal adduction stretch. In the internal rotation stretch, the arm is placed in the throwing (cocked) position and then internally rotated to stretch the posterior rotator cuff. In the horizontal adduction stretch the arm is horizontally adducted while the scapula is stabilized. The pectoralis minor should also be stretched. This can be done by placing a rolled towel between the supine athlete’s shoulder blades and steadily pushing posteriorly on the shoulders. In addition to the aforementioned stretches, the trapezius muscle and the periscapular retractor and protractor muscles should be strengthened.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree