Chapter 37 Orthoses for the muscle disease patient
Patients with generalized, trunk, and extremity muscle weakness have a neuromuscular disorder originating in the motor unit. Muscle weakness can result from a disease originating in the motor neurone, the peripheral nerve, the neuromuscular junction, or the muscle tissue itself. Weakness in muscles originating in the muscle tissue is a primary disease of muscle, a myopathy. Muscle weakness secondary to a disorder in the motor unit proximal to the muscle causing muscle atrophy or deterioration is a neuropathy. Muscle disease can also be referred to as motor unit disorder.15
Today most of the conditions discussed—motor unit disorders—are considered genetic disorders in which a defect in the gene causes a structural abnormality of such magnitude that motor unit components and muscle cells are affected. Fortunately, scientific research has allowed development of methods and tools for identifying and precisely determining and/or localizing the area of defect.34 Progress has been made but has not reached a level sufficient for permanent cure of diseases. Interest in the management of such cases is being reported from developing countries.42 The genetic defect can be passed from one generation to the next. Children of such persons manifest problems earlier in life, so treatment, especially in the form of supportive care, has become increasingly more important.7,44,45 Heart transplantation can extend the life of neuromuscular patients.39 Orthoses and modifications made to improve their use and efficiency have been emphasized by clinicians treating patients with progressive weakness and increasing disability. Lightweight materials (see Chapters 3 and 4), improved electronics, engineering advancements, and robotics (see Chapter 50) have led to the development of better tools and devices.
With better recognition of the disease and more accurate early diagnosis, treatment plans require review and modification. For example, after determining the orthopedic disabilities of a child with spinal muscular atrophy, Evans et al.8 developed the principles for generalized management of orthopedic problems. Current literature suggests that unilateral hip subluxation should be managed operatively52; thus, continued review of the topic and of the disease are important. Evidence-based studies are underway, and useful information can be obtained from available and upcoming clinical studies.43
The problem
When a patient has muscle weakness, whether in the trunk, proximal part of the body, or distal extremities, orthoses can be used for support. Depending on the underlying condition, weakness can be generalized or regional, unilateral or bilateral, asymmetrical or symmetrical. Contractures result from weakness around a joint and occur because the extent of the disorder within, or the rate of muscle deterioration between, antagonist or agonist muscle groups is not be the same. Contractures can be influenced by positioning and gravity. The affected part (e.g., the spine or an extremity) may be pulled into a specific direction without significant resistance. When this condition persists over a long period, a fixed contracture can develop. Contractures can result from muscle cell death and fibrosis. For patients with muscle disease, orthoses are designed to support and maintain correction rather than work against a deforming force. In motor unit disorders, there is no increase in muscle tone, so spasticity is not present. Orthoses for this population can be lightweight because there is no requirement for structural rigidity to oppose high tone.
Clinical aspects and diagnosis
Identification of the underlying neuromuscular disorder is an extremely important aspect of the overall planning of treatment and bracing. Many motor unit disorders are associated with a genetic defect.2,5 Knowledge of the family history is important and can help establish the diagnosis. The workup should include information about the time of onset of weakness, its clinical course, and a discussion of progression or stability of the disease process. The diseases that progress slowly or remain stable lend themselves to successful use of orthoses. Diseases that change may require frequent modifications, adjustments, or replacement of orthoses. Areas of weakness must be identified and muscle strength testing recorded using methods developed for manual muscle testing.20 Can a pattern be identified? Is the weakness proximal, distal, or central, or does it affect only a specific area, such as the face, neck muscles, or scapular supporting musculature? Is the weakness focal, caused by parasites of an obstructive vascular disorder? Laboratory studies that determine the activity of enzymes such as creatinine phosphokinase (CPK), which reflects muscle tissue breakdown, provide useful support for the clinical impression. CPK is highly elevated in rapidly progressive muscle disorders with significant muscle tissue breakdown, such as Duchenne pseudohypertrophic muscular dystrophy (DMD), and generally are not elevated in stable conditions such as spinal muscular atrophy and congenital myopathies. Many genetic studies using blood studies have been developed19 and provide accurate information on the nature of the underlying disorder. Other diagnostic tests frequently relied upon include electromyography, nerve conduction studies, ultrasonography, and muscle imaging.29 Muscle biopsy, including histochemical and biochemical studies, and testing for dystrophin, the presence of which rules out DMD, may provide a more definitive answer. Once the diagnosis is established, prognosis and the clinical course of the neuromuscular disorder can be better evaluated. This allows for treatment planning to manage the patient’s immediate and/or long-term problems and determine the extent and need for orthotic care.
Team approach
Long-term disability with loss of function is associated with most motor unit disorders. Polymyositis with severe generalized muscle weakness initially can be treated with steroids and immunosuppressant medications.28 Improvement in muscle strength and function are expected with successful treatment, leading to control of the acute process. Neuropathies and myopathies require long-term management not only from the medical standpoint but also for overall care and maintenance of function. The treatment team must include physicians who have special knowledge of neuromuscular diagnosis and can understand the course of neuromuscular disorders and the disabilities they cause. Expertise in orthopedics, neurology, genetics, laboratory medicine, physical medicine, pulmonary medicine, pediatrics, and geriatrics may be needed to manage neuromuscular disorders. Physical therapists and occupational therapists must understand muscle grading and the affected patient’s functional abilities together with available self-care aids, gait analysis data, mobility devices, and possible environmental adaptations. Psychologists, liaison nurses, social workers, recreational therapists, and community workers and leaders support the patient and family’s needs and help the school and community understand the disabled person’s special problems and concerns. They also interact with the community and special agencies that provide services to assist the disabled person. Governmental programs through schools, disabled workshops, and community centers may be available to help the disabled child’s development and educational programs. The certified orthotist who is knowledgeable about support of weakened limbs and trunk is of utmost importance to the team because of special experience and training in the design, measurement, construction, fitting, maintenance, and repair of supportive and assistive devices or equipment.27a
Spinal orthoses
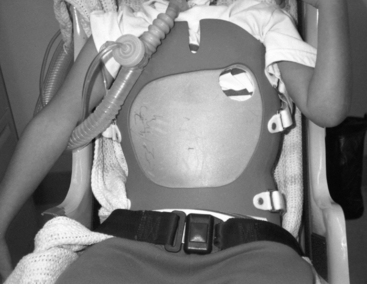
Spinal deformities are frequently seen in neuromuscular patients, whose spines require support. The orthoses used are generally considered containment devices (Fig. 37-1). They have been developed in many centers treating neuromuscular patients by adapting orthoses developed for control of idiopathic and acquired scoliosis.3,10,24,46,50 For children with weak neck muscles, outriggers must be added to support the head.37 Principles developed for the use of orthoses in the treatment of patients with idiopathic scoliosis cannot be directly applied to patients with neuromuscular scoliosis because these patients have weakness of the supportive musculature of the spine and spinal column collapse.27,33
It is important to know the natural history of spinal collapse in the neuromuscular condition being treated.13,22,24,27,31 In the ambulatory person, recognizing the spinal curve pattern and its flexibility becomes important. Encumbering the spine with a corset can interfere with balancing and walking. In a patient with a progressive disease, such as DMD, frequent reassessments of the spine in the seated position should be performed at least every 6 months. A spinal curvature, if present, must be followed closely, with clinical examinations as frequently as every 3 months. If there is doubt about the nature and degree of the spinal curvature, an X-ray examination in the sitting position should be performed. If the curve progresses, it can become fixed and difficult to correct. Thus, a curve less than 35 degrees can be supported using a lightweight body jacket (thoracolumbosacral orthosis [TLSO]), especially in patients with very slowly progressive conditions, such as spinal muscular atrophy and congenital muscular dystrophy. When spinal collapse progresses to the degree where sitting becomes difficult and the arms and hands are supporting the trunk, pressure sores can occur, especially in the elbow, which bears the brunt of the body weight. Spinal fusion is definitely indicated whenever possible.32
It is important to follow the spinal curve clinically and radiographically even though support is provided externally by a TLSO or internally via spinal fusion and instrumentation.9,35,40 In the growing child, posterior spinal fusion can cause arrest of posterior growth centers, resulting in severe lordosis. This presents difficulty in sitting because the head and neck tilt back into increasingly greater extension with age. Modification of the wheelchair or outrigger for support of the head is needed. This lordosis, which results from the “crankshaft phenomenon,” must to be recognized and prevented. Use of an “expanding” rod and surgical implantation of a rod without spinal fusion are important areas of innovation and development. If successful, many of the growing problems of the spine with increasing spinal deformity can be controlled until definitive spinal fusion can be established without significant growth disturbances.47
Spinal fusions that are incomplete, too short, or made on growing spines can result in further progression of scoliosis, know as falling off or the crankshaft phenomenon. The results of such surgical corrections can take the form of deformities and bony prominences, such as a protuberant rib cage, and pain. These cases present special challenges to the orthotist making special customized supports6,36,37 and devices that allow for continued comfortable seating, maintenance of function, and independence.