Chapter 39 Orthoses for myelomeningocele
Myelomeningocele is a neural tube defect and a major birth defect. It is an embryological abnormality that results in a myriad of complex neuromuscular problems. Children with spina bifida can be classified according to the level of neurological involvement or functional impairment. Myelomeningocele occurs in approximately 0.4 per 1,000 live births.69 The incidence of myelomeningocele is slightly higher in females than males, at a ratio of 1.3:1. With a high prevalence of Chiari II malformation and hydrocephaly, myelomeningocele is characterized by a variation of motor impairments, ranging from minimal muscle weakness to complete paralysis. Spasticity may be present.37 Musculoskeletal deformity and sensory deficits are common and, depending on the level of involvement, can adversely affect the child’s abilities and functioning in the community. Folic acid is important in preventing this birth defect. Reports indicate that folic acid intake in the preconception period can prevent up to 85% of spina bifida cases.48 This success rate underscores the need to develop worldwide programs that will effectively manage and eradicate this neural tube defect.
Because of the complexity of this major birth defect, orthotic management is critical for the child’s function and is a challenging endeavor for the orthotist. Successful orthotic treatment is based on a comprehensive understanding of the disease and on reasonable expectations for the goals of orthotic care as identified by the medical team. These goals and expectations must be clearly defined for the families so that they may appreciate the degree to which orthotic treatment can or cannot be successful. Success is predicated on a number of clinical issues that may include one or all of the following: (1) level of neurological involvement; (2) degree of musculoskeletal deformity; (3) sensory impairment; (4) acquired obesity; (5) existing muscle strength; (6) visual and motor perception impairment; (7) patient motivation; and (8) family support.2,11,13,58 Consideration of these issues will result in more predictable outcomes for patient developmental milestones; postural control; mobility; age-specific function; protection of the insensate foot; and management of musculoskeletal deformities.
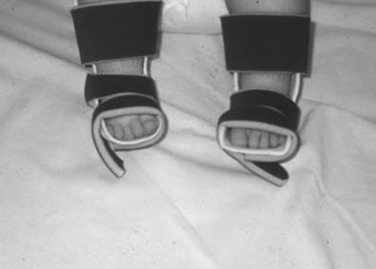
For the child with spina bifida, the capacity and degree to which function and ambulation can be achieved are based on their level of motor function and functional mobility.2,18,28,40,63 Contractures, limited sitting balance, and obesity are factors that may adversely affect the child’s ability to walk with or without orthoses. These factors in addition to the child’s motor function level can strongly influence how effectively orthotic management improves functional ambulation. Early patient examination and orthotic intervention are important first steps if future ambulation is to be achieved. Specific issues that warrant particular attention include (1) hip disorders (e.g., dislocation, subluxation, contractures), (2) knee flexion/extension contractures, and (3) foot/ankle deformities (e.g., equinovarus, clubfoot). In these cases, the orthotic goal(s) should be preventing deformity and maintaining proper joint alignment in order to achieve appropriate muscle balance during development. Achievement of these goals can facilitate the initiation of proper weight bearing and future ambulation (Fig. 39-1).
Thoracic/high lumbar level
Lesions at motor levels designated as thoracic/high lumbar reveal a significant compromise of muscle strength to the lower limbs and some weakness of the upper limbs.25 In addition, this patient population is likely to have hydrocephalus, Arnold-Chiari malformation, and often develops scoliosis, hip dislocation, and contractures of the hip and knee.59 As a result of the higher-level lesion, the attributes of normal kinematic gait not only are compromised for the foot and knee but are dramatically compromised at the hip and pelvis compared to lower-level lesions. This is evident by the magnitude of compensatory motion during gait resulting from specific muscle deficits involving the hip joint.67 For this lesion level, motor activity of the knee, ankle complex, hip extensors, and hip abductors typically exhibits muscle grade ≤ 2 on a five-point scale. Some sparing at the hip is evident for hip flexors and hip adductors exhibiting muscle grade ≥ 3. Some level of community ambulation can be achieved up to early adolescence with appropriate orthotic management; however, the ability for community ambulation quickly declines in adulthood as energy cost becomes too high for meaningful ambulation.12 Functional ambulation in this group is further compromised as spinal deformity and contractures of the lower extremity become more clinically significant.3
The goal of mobility is important, but the manner of mobility for this level of myelomeningocele remains controversial. At the center of the controversy is a divide between assisted standing/ambulation through orthotic management (i.e., standing frame, parapodium, hip–knee–ankle–foot orthosis [HKAFO], reciprocating gait orthosis [RGO]) and use of mobility aids such as wheelchairs. Advocates for orthotic management have described physiological and psychological benefits with regard to upright standing and ambulation, including cardiac and pulmonary function, bowel and bladder function, issues related to the musculoskeletal system, and greater independence at a later age.8,41,54 In an investigation of children with spina bifida by Mazur et al.,36 children who had received orthotic management at an early age to facilitate ambulation exhibited fewer fractures and pressure sores compared to children who did not ambulate and receive orthotic management at an early age. However, proponents of wheelchair use have found that individuals are more energy efficient when using a wheelchair compared to orthotic management.1 Liptak et al.29 found no significant difference between early ambulators and wheelchair users in the areas of (1) severity of hip flexion contractures, (2) degree of urinary tract complications, (3) frequency of decubitus ulcers,1 and (4) activities of daily living (ADLs). Because evidence suggests that both standing and wheelchair use can be beneficial, it is more paramount that mobility not be relegated to a strict choice between these two methods of mobility.31 Mobility programs that incorporate advising on multiple options allow the family and child to determine which mobility option is most functional for the task or activity at hand. Many are less likely to give up ambulation completely.6
Orthotic management
Orthotic management for children with thoracic/high lumbar lesions strives to achieve age-specific goals consistent with sitting balance, standing, ambulation, and independent function. When standing and some level of ambulation are the goals for these children, then certain orthotic design requirements must be fulfilled in order to achieve effective management. According to Rose,54 stabilization and alignment across the hip, knee, and ankle are essential for standing and ambulation in an orthosis. Acceptable forms of ambulation include swing through, swing to, swivel, and reciprocal, and are based in part on proper orthotic design and assistive device application. Orthoses for this population have unique design characteristics that, when applied correctly and to the right candidate, can offer greater functional capacity.
Standing frame
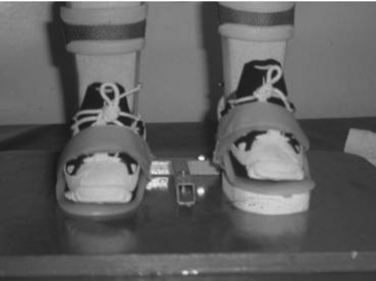
A child 12 to 24 months old with a thoracic/high lumbar lesion, good head control, and good sitting balance may be a candidate for a standing frame.7,39 The standing frame promotes standing activities that are consistent with normal development (e.g., postural control, trunk strength, balance, and righting reactions) and allows for free use of the upper extremities. Stabilization in the standing frame occurs through four-point stabilization across the hip and knee joints.55 In conjunction with the standing frame, control should be considered for the foot and ankle complex, which can be managed effectively with bilateral solid ankle–foot orthoses (AFOs). This design can offer sagittal control of the ankle joint and coronal control of the subtalar joint in order to maintain appropriate antagonist–agonist muscle balance and foster a better base of support (Fig. 39-2).10
Parapodium
Designed by Motloch,43 the parapodium uses many of the same design principles and force applications observed with the standing frame but has the additional capability to allow for sitting. Moreover, the parapodium supporting base can be modified to include a swivel component for an alternative means of forward ambulation for the child. The parapodium is a modular system that provides upright stability across the hip, knee, and, to a lesser degree, the foot and ankle complex. As in the case of the standing frame, if additional foot and ankle control is warranted, bilateral solid AFOs should be considered along with the parapodium. The parapodium itself has an aluminum alloy baseplate with the ability to support the feet and increase the base of support. Attached to the baseplate are shin and thigh tube sections that can rotate about a vertical axis.61 Integrity of the vertical tubes is maintained by knee and pelvic bearing brackets that allow for appropriate joint alignment and stable upright standing. Housed within the vertical tubes are mechanical hip and knee joints whose axes, when parallel to the frontal plane, allow the joints to unlock for sitting. This position allows the child to sit while stability is maintained across the aforementioned anatomical joints.
Ambulation is possible with the addition of the swivel walker.60 The swivel walker can be attached distally and underneath the supporting base of the parapodium. Ambulation occurs with the patient in an erect posture as he or she rocks laterally from side to side. The center of mass of the system is positioned just anterior to the swivel bearing in order to foster easier forward progression for the child. Although beneficial, the swivel walker is used less frequently now because of the availability of alternative reciprocal designs. According to Stallard,61 several indications for the swivel walker include younger children who have initiated upright posture, patients with upper limb weakness in whom assistive devices are not an option, and patients with limited mobility who require free upper limbs for function.
Hip–knee–ankle–foot orthosis
The HKAFO functions as either a fixed and/or dynamic orthosis. The orthosis has a pelvic band that is attached bilaterally to a knee–ankle–foot orthosis (KAFO) via left and right mechanical hip joints. For patients who lack motor function about and distal to the hip joint, it may be necessary to hold motion across the hip, knee, and ankle in order to provide stability during standing and mobilization.22 Swing-through and swing-to gait patterns may be obstructed in some patients when hip motion is restricted in conjunction with a longer vertical pelvic interface. Dynamic HKAFOs are likely to be used in their more sophisticated form, the RGO. In both cases ideal motor function should, at a minimum, include hip flexor strength in order to initiate step ability for ambulation (i.e., swing-through, reciprocal). To achieve forward mobility, some form of assistive device is required.
Reciprocating gait orthosis
The RGO provides a means for reciprocal ambulation in individuals with marked lower extremity muscle weakness. The RGO design at a minimum requires active hip flexion to facilitate extension of the contralateral limb and ultimately drive the reciprocal gait pattern.71 The dynamic capability of the RGO occurs via the hip joints. The hip joints can function independently from one another or, with a more sophisticated design, the mechanical hip joints work in unison via a cable or central posterior pivot point. Irrespective of the design, a comprehensive evaluation of the patient is critical to determining the likelihood of RGO utilization and ambulation. When motivation and family support are low, access to therapy is difficult, donning/doffing is problematic, and routine travel for appointments is not possible, consistent evidence suggests that the child probably will not continue wearing and using the RGO.19,51 The medical team should consider these issues when evaluating children as candidates for an RGO.
Clinical factors are no less important and should be included in the overall assessment of the child to determine the appropriateness of the RGO. Considerations for RGO use include (1) upper limb strength,33 (2) hip and knee flexion contractures less then 30 degrees, (3) active hip flexor strength, (4) no obesity, and (5) no significant spinal deformity. These factors are assessed in order to determine the likelihood of successful management with the RGO. In a study by Stallard et al.,62 34% of patients with myelomeningocele and a complete lesion level at or above L1 were able to attain community ambulatory status. Another study reported that children with mild spinal deformities, hip dislocation, and hip/knee contractures less then 30 degrees were able to function within an RGO.16 Other studies have compared velocity in the RGO to other HKAFO designs and found that velocity increased more when the RGO was used compared to the HKAFO.35,38,71 The results from these studies suggest that, under the right circumstances, RGOs can facilitate better functional mobility. With a comprehensive evaluation of the patient, the likelihood is greater that decisions will be made and tailored to the specific individual in order to effectively meet the needs of that patient.
Low lumbar level
A child with a lower lumbar lesion typically exhibits a functional level consistent with active hip flexors, hip adductors, knee extensors, and knee flexors. Motor deficits include hip extensors, hip abductors, and ankle plantarflexors and dorsiflexors. The resulting gait pattern is a combination of gait deviations that extend from the foot and ankle complex up to and including the trunk. Gait deviations typically include a posterior trunk lean throughout swing and stance, excessive pelvic rotation and obliquity, exaggerated stance phase hip abduction (lateral trunk lean), increased hip and knee flexion, and increased stance phase dorsiflexion.14
Hip extensor weakness is evident in gait with the appearance of a posterior trunk lean and increased anterior pelvic tilt. Posterior trunk lean is necessary for the child’s stability at the hip as he or she provides an externally generated hip extension moment in an effort to reduce the demand on the already deficient hip extensors. This deficiency also results in a loss of sagittal pelvic control that ultimately presents as an exaggerated anterior pelvic tilt during ambulation.70 The hip extensor weakness and unopposed action of the hip flexors lead to further hip flexion contractures, increased hip flexion in terminal stance, and diminished step length during gait. Also evident is deficient hip abductor strength and the associated lateral trunk lean. This lateral trunk lean to the ipsilateral side is a necessary action in order to decrease the external hip adduction moment, an event that normally requires subsequent hip abductor strength that, in this case, is not present.
As with lateral trunk lean, frontal plane assessment typically reveals a valgus stress at the knee in the stance phase limb. Several factors identified as contributing to this valgus stress are lateral trunk lean, closed-chain hyperpronation (internal hip rotation, increased knee flexion, ankle dorsiflexion, hindfoot valgus), and medial tibial torsion (Fig. 39-3).20
During normal walking, plantarflexor activity progressively increases from loading response to peak activity at terminal stance. As the center of pressure propagates anteriorly along the plantar aspect of the foot, an external dorsiflexion moment progressively increases as ground reaction force moves further in front of the ankle joint axis. To oppose this external dorsiflexion moment, an internal moment is generated through eccentric plantarflexor activity. A child with a low lumbar lesion will exhibit weakness of the plantarflexors. As a result of this weakness, the soleus is unable to oppose the external dorsiflexion moment and the tibia is allowed to progress anteriorly, ultimately leading to excessive dorsiflexion, knee flexion, and hip flexion in stance phase (Fig. 39-4). Temporospatial data suggest a 60% decrease in walking velocity compared to normal.68 Orthotic management for this functional level varies from solid polymer AFOs to KAFOs.
< div class='tao-gold-member'>
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree