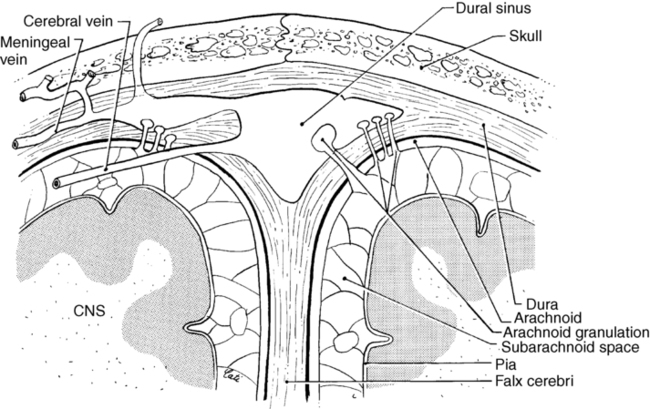
JUDITH A. DEWANE, PT, DSc, NCS After reading this chapter the student or therapist will be able to: 1. Identify and comprehend the terminology for classifying different types of inflammatory and infectious disorders within the brain. 2. Discuss the range of neurological sequelae that occur. 3. Discuss the components of the comprehensive evaluation process and their interrelationships. 4. Structure the examination process to gather the information required to generate an appropriate plan of care. 5. Discuss the general goals of the intervention process. The inflammatory process may be a localized, circumscribed collection of pus; may involve primarily the leptomeninges; may involve the brain substance; or may involve both the meninges and the brain substance. The infecting agents may be bacteria, viruses, prions, fungi, protozoa, or parasites. The most common agents producing meningitis are bacterial; the most common agents producing encephalitis are viral. However, bacterial encephalitis and viral meningitis also are disease entities. The following overview of the inflammatory processes within the brain is organized based on the anatomical location of the infection. More comprehensive discussions based on specific infecting organisms can be found in the references at the end of the chapter.1 The site of the infection will determine the signs and symptoms of the CNS infections, whereas the infecting organism determines the prognosis, including the time course and severity of the problems.2 The site and size of the abscess influence the initial symptoms. Evidence of increased intracranial pressure, a focal neurological deficit, and fever are described as the classic presenting triad.3 However, the classic triad occurs in less than 50% of patients.4 Most individuals experience an alteration of consciousness. In 47% of the cases, the frontal, parietal, or temporal lobe is involved.4,5 Medical management of the abscess typically consists of antibiotic therapy (depending on the infecting agent and size and site of the abscess) and, often, surgical aspiration or excision. Bharucha and colleagues3 describe neurological sequelae in 25% to 50% of the survivors, with 30% to 50% having persistent seizures, 15% to 30% having hemiparesis, and 10% to 20% having disorders of speech or language. The diagnostic categorization of meningitis depends on the infecting agent (e.g., Haemophilus influenzae meningitis, Streptococcus pneumoniae meningitis, and viral meningitis) and on the acute or chronic nature of the meningitis (acute, subacute, or chronic meningitis). The term acute bacterial meningitis denotes infections caused by aerobic bacteria (both gram-positive and gram-negative).5,6 The most common infecting organism producing acute bacterial meningitis varies according to the age of the population. During the neonatal period and in the older adult, infections by gram-negative enterobacilli, especially Escherichia coli, and group B streptococci occur most frequently. Typical causative agents in children include H. influenzae, Neisseria meningitidis, and S. pneumoniae.7 S. pneumoniae, N. meningitidis, and H. influenzae are the most common causes of community-acquired meningitis.5,7,8 Individuals with a condition such as sickle cell anemia, alcoholism, or diabetes mellitus and individuals who are immunosuppressed are at increased risk.1,9 Meningococci have been implicated in meningitis that strikes young children most often but can also infect adolescents and young adults. Freshman who live in dormitories are almost four times more likely to get meningitis than other college students. The circulation of CSF spreads the infecting organism through the ventricular system and the subarachnoid spaces (Figure 26-1). The pia and arachnoid maters become acutely inflamed, and as part of the inflammatory response, a purulent exudate forms in the subarachnoid space. The exudate may undergo organization, resulting in an obstruction of the foramen of Monro, the aqueduct of Sylvius, or the exit foramen of the fourth ventricle. The supracortical subarachnoid spaces proximal to the arachnoid villi may be obliterated, resulting in a noncommunicating or obstructive hydrocephalus caused by the accumulation of CSF. As the CSF accumulates, the intracranial pressure rises. The increased intracranial pressure produces venous obstruction, precipitating a further increase in the intracranial pressure. The rise in the CSF pressure compromises the cerebral blood flow, which activates reflex mechanisms to counteract the decreased cerebral blood flow by raising the systemic blood pressure. An increased systemic blood pressure accompanies increased CSF pressure. Clinical features of acute bacterial meningitis include fever, severe headache, altered consciousness, convulsions (particularly in children), and nuchal rigidity. Nuchal rigidity is indicative of an irritative lesion of the subarachnoid space. Signs of meningeal irritation are painful cervical flexion, the Kernig sign, the Brudzinski sign, and the jolt sign.10 Cervical flexion is painful because it stretches the inflamed meninges, nerve roots, and spinal cord. The pain triggers a reflex spasm of the neck extensors to splint the area against further cervical flexion; however, cervical rotation and extension movements remain relatively free. The Kernig sign refers to a test performed with the client supine in which the thigh is flexed on the abdomen and the knee extended (Figure 26-2, A). Complaints of lumbar or posterior thigh pain indicate a positive test result.10 This movement pulls on the sciatic nerve, which pulls on the covering of the spinal cord, causing pain in the presence of meningeal irritation. The same results are achieved with passive hip flexion with the knee remaining in extension. This is the same procedure described by Hoppenfeld11 as the straight leg raising test for determining pathology of the sciatic nerve or tightness of the hamstrings. Passive hip flexion with knee extension can be painful because of meningeal irritation, spinal root impingement, sciatic nerve irritation, or hamstring tightness. The Brudzinski sign refers to the flexion of the hips and knees elicited when cervical flexion is performed10 (see Figure 26-2, B). These signs will not be present in the deeply comatose client who has decreased muscle tone and absence of muscle reflexes. The signs may also be absent in the infant or elderly patient. Finally, the jolt test, which has the patient turn his or her head from side to side quickly (two to three rotations per second), has a positive result if the maneuver worsens the patient’s headache.10 Even with optimal antimicrobial therapy, bacterial meningitis continues to have a finite mortality rate, which varies with the infecting organism, age of the individual, and time lapse to initiation of treatment, and has the potential for marked neurological morbidity. Neurological sequelae occur in 20% to 50% of the cases.1,9 Bacterial meningitis is considered a medical emergency; delays in initiation of antibacterial therapy increase the risk of complications and permanent neurological dysfunction.1,9 Reports of the long-term outcome of individuals with bacterial meningitis indicate that up to 20% have long-term neurological sequelae.1,5 The sequelae may be the result of the acute infectious pathological condition or subacute or chronic pathological changes. The acute infectious pathological condition could result in sequelae such as inflammatory or vascular involvement of the cranial nerves or thrombosis of the meningeal veins. Cranial nerve palsies, especially sensorineural hearing loss, are common complications. The risk of an acute ischemic stroke is greatest during the first 5 days.9 Weeks to months after treatment, subacute or chronic pathological changes may develop, such as communicating hydrocephalus, which manifests as difficulties with gait, mental status changes, and incontinence.10,12 Approximately 5% of the survivors will have weakness and spasticity.6 Focal cerebral signs that may occur either early or late in the course of bacterial meningitis include hemiparesis, ataxia, seizures, cranial nerve palsies, and gaze preference.1,13 Cognitive slowness has been found in 27% of clients after pneumococcal meningitis, even with good recovery as documented by a Glasgow Outcome Scale score of 5.14 Aseptic meningitis refers to a nonpurulent inflammatory process confined to the meninges and choroid plexus, usually caused by contamination of the CSF with a viral agent, although other agents can trigger the reactions. The symptoms are similar to those of acute bacterial meningitis but typically are less severe. The individual may be irritable and lethargic and complain of a headache, but cerebral function remains normal unless unusual complications occur.5,15 Aseptic meningitis of a viral origin usually causes a benign and relatively short course of illness.16,17 A variety of neurotropic viruses can produce aseptic (viral) meningitis. The enteroviruses (echoviruses and the Coxsackie viruses), herpesviruses, and HIV are the most common causes.5,7,18 The primary nonviral causes of aseptic meningitis are Lyme Borrelia and Leptospira.19 The diagnosis of this type of aseptic meningitis may be established by isolation of the infecting agent within the CSF or by other techniques. The glucose level of the CSF in bacterial meningitis is usually depressed; however, the glucose level in viral meningitis is normal.2 The pathological condition includes destruction or damage to neurons and glial cells resulting from invasion of the cells by the virus, the presence of intranuclear inclusion bodies, edema, and inflammation of the brain and spinal cord. Perivascular cuffing by polymorphonuclear leukocytes and lymphocytes may occur, as well as angiitis of small blood vessels. Widespread destruction of the white matter by the inflammatory process and by thrombosis of the perforating vessels can occur. Increased intracranial pressure, which can result from the cerebral edema and vascular damage, presents the potential for a transtentorial herniation. The likelihood of residual impairment of neurological functions depends on the infecting viral agent. Patients with mumps meningoencephalitis have an excellent prognosis, whereas 55% of the individuals with herpes simplex encephalitis treated with acyclovir have some neurological sequelae.6 Because of the slow recovery of injured brain tissue, even in patients who recover completely, return to normal function may take months.20 Plum and Posner21 discuss viral encephalitis in terms of five pathological syndromes. Acute viral encephalitis is a primary or exclusively CNS infection. An example would be herpes simplex encephalitis, in which the virus shows a partiality for the gray matter of the temporal lobe, insula, cingulate gyrus, and inferior frontal lobe. Other examples are the mosquito-borne viruses, such as the St. Louis encephalitis, California virus encephalitis, and most recently the West Nile virus (WNV). From 1999 to 2005 in the United States, the incidence of infection from the WNV has increased from 62 cases to 3000 cases.22 Currently all states have some level of WNV activity, and only four states are without human cases (Figure 26-3). The majority (80%) of people infected by the WNV will be asymptomatic; of the remaining people infected, less than 1% will develop severe illness.23 Risk of neuroinvasive disease from WNV is 40%; neuroinvasive disease involves meningitis, encephalitis, or poliomyelitis, with wide variety in clinical presentation (Figure 26-4).24 Parainfectious encephalomyelitis is associated with viral infections such as measles, mumps, or varicella. Acute toxic encephalopathy denotes encephalitis that occurs during the course of a systemic infection with a common virus. The clinical symptoms are produced by the cerebral edema in acute toxic encephalopathy, which results in increased intracranial pressure and the risk of transtentorial herniation. Reye syndrome is an example. Global neurological signs, such as hemiplegia and aphasia, are usually present, rather than focal signs. The clinical symptoms of the previous three syndromes may be similar. Specific diagnosis may be established only by biopsy or autopsy. Progressive viral infections occur from common viruses invading susceptible individuals, such as those who are immunosuppressed or during the perinatal to early childhood period. Slow, progressive destruction of the CNS occurs, as in subacute sclerosing panencephalitis. The final category of encephalitis syndromes consists of “slow virus” infections by unconventional agents (the prion diseases) that produce progressive dementing diseases such as Creutzfeldt-Jakob disease and kuru.25 The medical management of virally induced encephalitis has been, and with many infecting agents remains, primarily symptomatic. In some cases, intensive, aggressive care is necessary to sustain life. Pharmacological interventions are available to treat some viral infections, such as herpes encephalitis. The probability of neurological sequelae differs according to the infecting agent. Aggressive management of increased intracranial pressure is required because persistently elevated intracranial pressure is associated with poor outcome.1,26 Further information concerning the clinical features, medical management, and potential for neurological sequelae of a specific type of encephalitis should be sought in the literature based on the infecting agent. An individual within the acute phase of meningitis or encephalitis or with residual neurologic dysfunction from these disorders may demonstrate signs and symptoms similar to those of generalized brain trauma, tumor disorder, or other identified abnormal neurological state. The variability in the clinical picture is reflected in the inclusion of the category “infectious diseases that affect the central nervous system” in the Guide to Physical Therapist Practice.27 Practice patterns for physical therapists that apply to this population include the following: 5C: Impaired Motor Function and Sensory Integrity Associated with Nonprogressive Disorders of the Central Nervous System—Congenital Origin or Acquired in Infancy or Childhood 5D: Impaired Motor Function and Sensory Integrity Associated with Nonprogressive Disorders of the Central Nervous System—Acquired in Adolescence or Adulthood 5I: Impaired Arousal, Range of Motion, and Motor Control Associated with Coma, Near Coma, or Vegetative State 5A: Primary Prevention/Risk Reduction for Loss of Balance and Falling The following discussion of the specific considerations within the examination process does not necessarily represent the temporal sequence to be used during the data collection process. As different items are discussed, suggestions for potential combinations of items will be made. The sequence of the process is best determined by the interaction of therapist and client. Figure 26-5 outlines the components that should be considered during the evaluation process and provides a synopsis of the following discussion. Acute bacterial meningitis and various forms of viral encephalitis may result in changes in the client’s level of consciousness. Consciousness is a state of awareness of one’s self and one’s environment.21 Coma can be defined as a state in which one does not open the eyes, obey commands, or utter recognizable words.28 The individual does not respond to external stimuli or to internal needs. The term vegetative state is sometimes used to indicate the status of individuals who open their eyes and display a sleep-wake cycle but who do not obey commands or utter recognizable words. DeMeyer29 presents a succinct description of the neuroanatomy of consciousness and the neurological examination of the unconscious patient. Plum and Posner21 also provide extensive information in this area. Several scales have been developed to provide objective guidelines to assess alterations in the state of consciousness. The Glasgow Coma Scale28 assesses three independent items: eye opening, motor performance, and verbal performance. The scale yields a figure from 3 (lowest) to 15 (highest) that can be used to indicate changes in the individual’s state of consciousness. The evaluation format is simple, and the scale demonstrates both interrater and intrarater reliability. Refer to Box 24-4 for the specific scale. The Rancho Los Amigos scale assesses level of consciousness and behavior.28 The therapist can use assessment tools such as the Glasgow Coma Scale and the companion Glasgow Outcome Scale to determine if the intervention program has resulted in any recordable changes in the client’s level of consciousness. Ideally, the client with decreased levels of consciousness will be monitored at consistent intervals to determine changes in status. Any carryover or delayed effects of the intervention could then be noted. The record of the client’s level of consciousness might also display a pattern of peak awareness at a particular point in the day. Scheduling an intervention session during the client’s peak awareness time may maximize the benefit of the therapy. Deficits in cognition may be evident as problems in the area of explicit (declarative) or implicit (procedural) learning. Explicit learning is used in the acquisition of knowledge that is consciously recalled. This is information that can be verbalized in declarative sentences, such as the sequential listing of the steps in a movement sequence. Implicit or procedural learning is used in the process of acquiring movement sequences that are performed automatically without conscious attention to the performance. Procedural learning occurs through repetitions of the movement task (refer to Chapter 4). Because explicit and implicit learning use different neuroanatomical circuits, implicit learning can occur in individuals with deficits in the components underlying explicit learning (awareness, attention, higher-order cognitive processes) (refer to Chapter 5 for additional information regarding implicit and explicit learning).
Inflammatory and infectious disorders of the brain
Overview of inflammatory disorders in the brain
Categorization of inflammatory disorders
Brain abscess
Meningitis
Bacterial meningitis
Clinical problems.
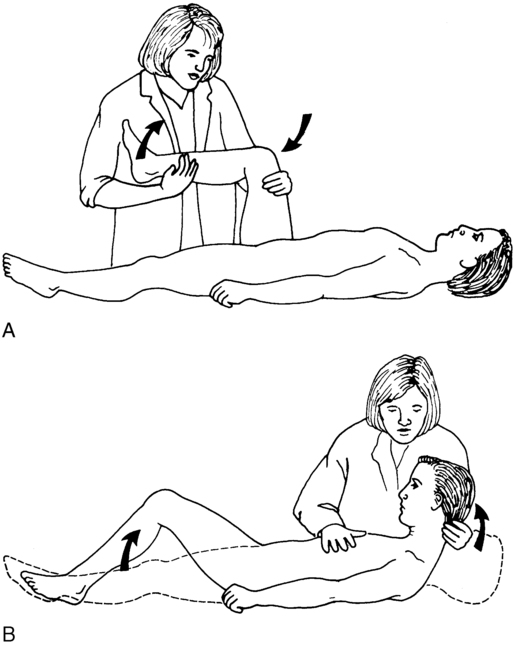
 A, Kernig sign. B, Brudzinski sign.
A, Kernig sign. B, Brudzinski sign.
Potential neurological sequelae.
Aseptic meningitis.
Encephalitis
Clinical problems.
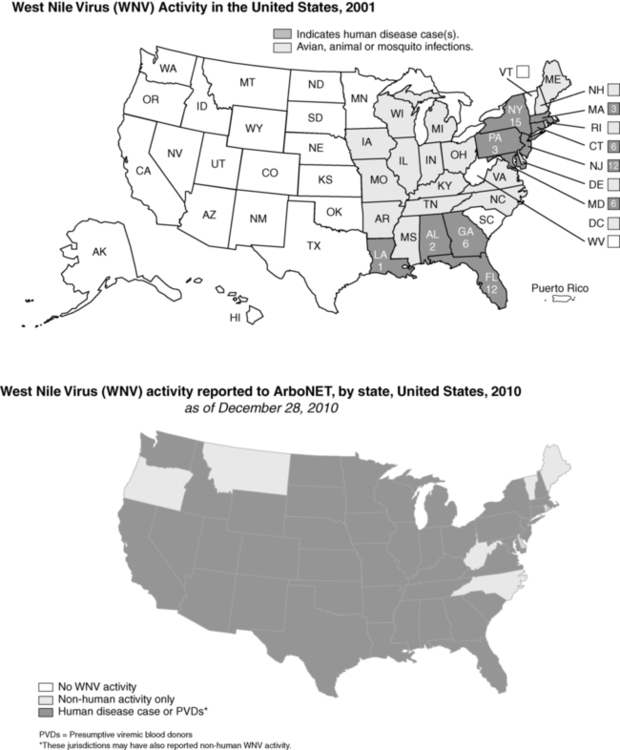
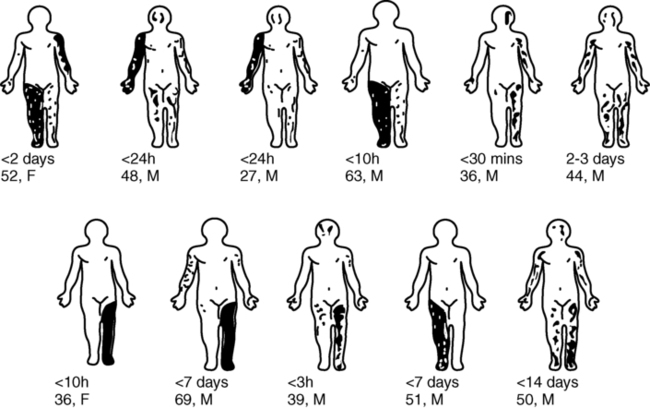
 West Nile virus (WNV) activity in the United States. (From www.cdc.gov/ncidod/dvbid/westnile/Mapsactivity/surv&control10MapsAnybyState.htm.)
West Nile virus (WNV) activity in the United States. (From www.cdc.gov/ncidod/dvbid/westnile/Mapsactivity/surv&control10MapsAnybyState.htm.)
Medical management.
Clinical picture of the individual with inflammatory disorders of the brain
Examination and evaluation process
Observation of current functional status
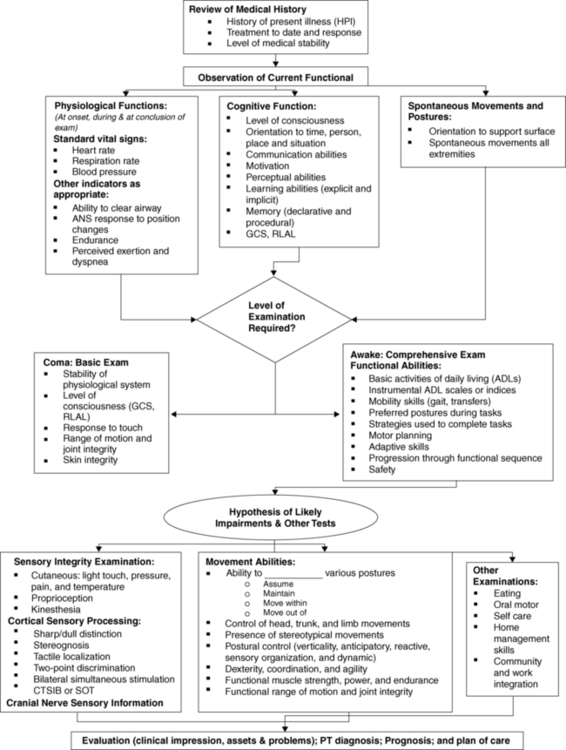
 Flow chart of the evaluation process.
Flow chart of the evaluation process.
Evaluation of cognitive status
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree