12 Complications of Trochanteric Fractures
Analysis of complications, mainly mechanical complications and disturbances of fracture healing, is an important source of information. The incidence of these complications indicates, for example, the number of trochanteric fractures treated in a given department, surgeons’ experience both in general and with various implants, and mastery of the learning curve. Another possible variable is the mean duration of the surgical procedure. Unfortunately, analysis of complications of operative treatment of trochanteric fractures has been infrequently reported.1–4 Few detailed studies have undertaken such analysis.5–15 Most investigators simply list the complications encountered without analyzing the causes and interactions of these complications.
Another problem is the method of analysis of complications. The terminology used to describe trochanteric fractures is imprecise and confusing. Different fracture patterns are designated by the same term, and different terms are used for the same fracture pattern. To avoid this terminologic uncertainty, the Arbeitsgemeinschaft für Osteosynthesefragen/Orthopaedic Trauma Association (AO/OTA) classification is followed strictly in this chapter.16,17 The term trochanteric fractures is used for all fractures of the trochanteric segment, the term pertrochanteric fractures for the group of 31A1 and 31A2 fractures, and the term intertrochanteric fractures for the group of 31A3 fractures.
Also problematic is the use of different, incompatible classifications.16–20 All this confusion significantly complicates comparison of results reported by various investigators and invalidates the results of multicenter studies.21–23 Evaluation of the basic fracture pattern, its instability, quality of reduction, or position of the lag screw in the femoral head is highly subjective. A frequent mistake in fracture evaluation is the grouping together of 31A2 and 31A3 fracture types.
Inadequate Reduction
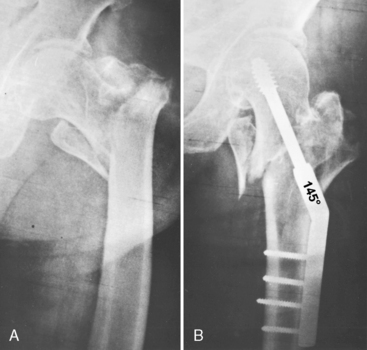
Pertrochanteric fractures (31A1 and 31A2) can, in most cases, be reduced without great difficulty. An exception is the type of fracture described by Moehring et al24 (Fig. 12-1). In unstable pertrochanteric fractures, it is useful to perform valgus reduction in the anteroposterior (AP) projection,25 especially when the fracture is to be fixed with a dynamic hip screw (DHS) (Fig. 12-2). In the lateral projection, the fragments must be coaxial, and antegrade or retrograde curvature must be avoided. Larsson et al26 recommended reduction of the fragments in such a way as to make the medial cortex of the proximal fragment overlap the medial cortex of the distal fragment. This technique may partially prevent collapse of fragments and medial displacement of the shaft (Fig. 12-3).
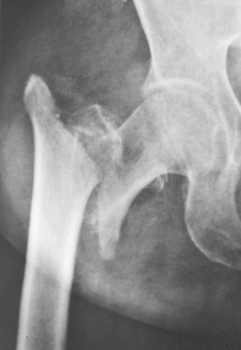
Figure 12-1 Irreducible pertrochanteric fracture, as described by Moehring.
(From Moehring HD, Nowinski GP, Chapman MW, Voigtlander JP. Irreducible intertrochanteric fractures of the femur. Clin Orthop Relat Res 1997;339:197–9.)
Intertrochanteric fractures (31A3) require anatomic reduction in both the AP and lateral views.10 This reduction may be difficult to achieve in certain types of these fractures. Percutaneous insertion of a Steinmann pin, mounted in a T-handle, and open reduction of fragments through a short incision are useful techniques.27
When reducing trochanteric fractures, possible malrotation of the limb should be taken into account. Malrotation, usually external, is often revealed only postoperatively. Some investigators consider rotation of more than 10 degrees a complication,28 whereas other investigators use 20 degrees as a criterion for malrotation.29 The incidence of this complication ranges between 1.3% and 2.5%.28,29 In the postoperative period, malrotation occurs only in intertrochanteric fractures (31A3) without distal locking.30 Excessive malrotation, particularly in younger patients, must be treated by refixation in the correct position or by intertrochanteric osteotomy after the fracture has healed.
Injury of Pelvic Vessels by Guidewire
Injury of pelvic vessels by overpenetration of the guidewire is a rare complication, described using both the DHS and the Gamma nail.31,32 In the two reported cases, this injury was caused by a lag screw guidewire that penetrated the femoral head and acetabulum as far as the pelvis. In the first case, the external iliac vein was injured, and the patient subsequently died.32 In the second case, an injury of the obturator artery was successfully treated by selective angiography and metal coil insertion.32 Therefore, when inserting a lag screw, and particularly during reaming, the surgeon must check the correct position of the guidewire in the femoral head and acetabulum frequently with an image intensifier. The technique for removal of a broken guidewire from the hip joint was described by Heal and Spencer.33
Incorrect Position of the Lag Screw in the Femoral Head
The position of the lag screw in the femoral head is one of the most significant factors influencing the stability of internal fixation of trochanteric fractures. Even a minor inaccuracy may result in failure of fixation, especially in patients with osteoporosis. Incorrect insertion of the lag screw is often caused by inadequate reduction, mainly in the lateral view, and inaccurate control using the image intensifier. The anterolateral segment of the femoral head is critical in this respect. Insertion of the lag screw into this segment significantly increases the risk of cutout.34,35
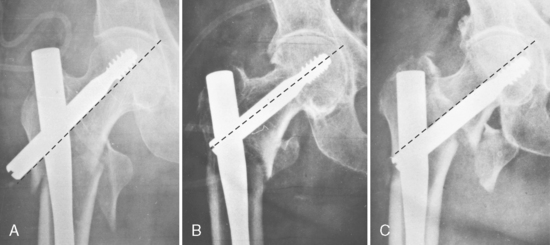
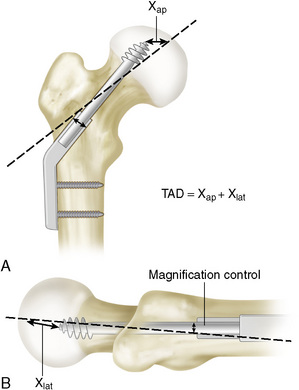
In implants with one lag screw, the screw should be inserted centrally in both AP and lateral views (i.e., in the long axis of the femoral neck and head) (Fig. 12-4). The tip of the screw should be seated deeply to the subchondral bone, within 5 mm of the joint line (Fig. 12-5); however, care must be taken to avoid central perforation of the femoral head. Baumgartner et al36 defined the tip-apex distance, to allow a determination of the ideal position of the lag screw in the femoral head (Fig. 12-6). This distance is a reliable predictor of cutout,37 although this determination does not provide any information about the relationship of the lag screw with the femoral head-neck fragment axis. The implant angle must respect the angle of reduction (i.e., the femoral neck-shaft angle), to prevent malalignment between the lag screw and the femoral neck-head axis (Fig. 12-7). Where the angle of the implant is greater than the angle of reduction, the lag screw will, as a rule, be inserted into the superior segment of the femoral head.37 This situation significantly increases the risk of cutout. Where the angle of reduction is greater than that of the implant, there is a danger of rotation of the proximal fragment on the lag screw with subsequent varus displacement (Fig. 12-8).
When two lag screws are used, two different configurations of their insertion are possible (Fig. 12-9). In the AP view, if the proximal screw is inserted proximal to the long axis of the proximal fragment, it must be slightly shorter than the distal screw.
Rotation of the Femoral Head During Insertion of the Lag Screw
Rotation of the femoral head during insertion of the lag screw is generally encountered in hard bone (i.e., in younger patients). The high speed of the drilling machine or an eccentric position of the guidewire in the femoral head may also cause this complication.8 Rotation may damage the extraosseous vessels supplying the femoral head and may lead to AVNFH.38 Rotation can be prevented by inserting an antirotation pin into the proximal fragment before insertion of the lag screw (proximal femoral nail [PFN], Synthes, Targon-Aesculap) or by fixing the proximal fragment with a Kirschner wire inserted into the acetabulum (DHS, Gamma nail).
Incorrect Length of the Lag Screw
When an intramedullary hip nail (IMHN) is used, the lateral end of a short lag screw placed correctly in the femoral head remains deep in the nail body and does not pass through the lateral cortex of the shaft. This placement may obstruct sliding of the lag screw and, consequently, compression of fragments.28 Similarly, when the DHS is used, a short lag screw has insufficient engagement in the barrel of the side-plate, and this placement increases friction forces between the barrel and the lag screw and creates the risk of jamming the sliding mechanism. The lateral end of a short screw may even slip out of the hole in the nail, or DHS barrel, medially and cause disengagement of the implant and total failure of internal fixation.8,39,40
Problems During Nail Insertion
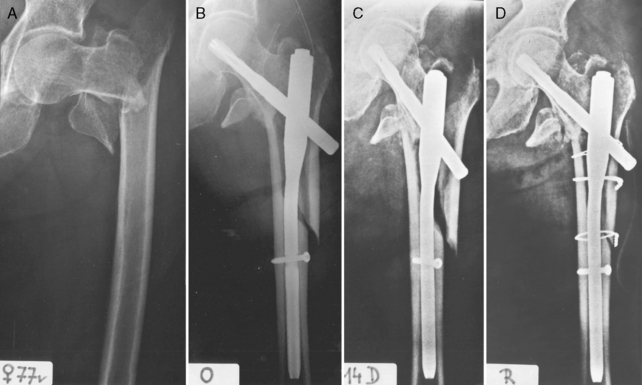
Problems during nail insertion into the diaphyseal fragment may have several causes. One reason for this complication is the small radius of curvature of the proximal end of the femur, in both frontal and sagittal planes, found typically mainly in Asian patients.41 Abnormal curvature may also develop in patients with certain bone diseases or with fractures in the subtrochanteric region of the femur. The same applies to abnormal narrowing of the medullary canal. Younger, or smaller, patients also have a narrower medullary canal. The medullary canal may be compromised by hardware from previous surgical procedures (plate, retrograde nail) (Fig. 12-10).
Also important is the location of the entry point.42 Problems with insertion of the nail into the correct position in the diaphyseal fragment have a negative impact on the subsequent insertion of lag screws into the femoral head (Fig. 12-11). Therefore, the preoperative AP radiograph must always cover the whole length of the nail inserted into the proximal femur, and the curvature of the femur in the frontal plane and the width of the medullary canal must be assessed. Reduction performed on a fracture table always requires a careful check of the medullary canal in the lateral view. The diameter and length of the nail must be chosen with regard to the diameter and curvature of the medullary canal. If any doubts exist about the risks of insertion of the intramedullary nail, an extramedullary implant should be used instead. The surgeon must never use hammer blows for insertion of the nail. If the nail jams, it will be necessary to choose a smaller-diameter nail, to ream the medullary cavity carefully, or to convert to an extramedullary implant procedure.
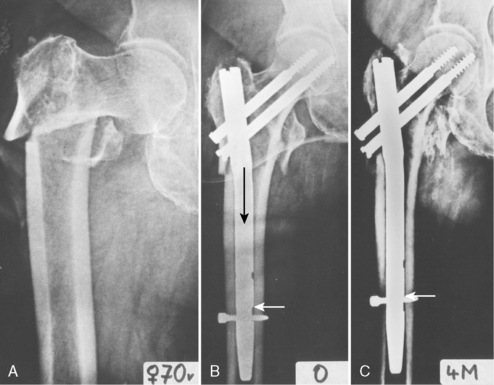
During nail insertion, reduction may be lost when the nail inserted across the fracture site separates the two fragments41 (Fig. 12-12). Forced insertion may result in secondary fracture of the femoral shaft. This injury was one of the most severe complications encountered in the past with the use of the Gamma nail. The femoral shaft may also be fractured in the presence of an unrecognized occult fissure extending as far as the subtrochanteric part.10 When the femoral shaft is fractured during operation, use of a long and thinner nail is recommended (Fig. 12-13). Sometimes, forced insertion of the nail can result only in fissure of the cortex that is not revealed during operation, but also in postoperative fracture of the femoral shaft.
A less severe complication is fracture of the lateral cortex.41,43 It may be caused by siting the entry point too laterally or by a greater mediolateral curvature of the nail. If the fragment is stable and displaced only minimally, no additional treatment will be needed. However, the nail must be always locked distally.42 Where the fragment is displaced, it has to be fixed (Fig. 12-14). Sometimes during insertion of the nail, “only” a fracture of the greater trochanter may occur.44 Such a fracture usually does not require any treatment.
Problems with Distal Locking
Problems with distal locking were the most frequently reported complications after introduction of the Gamma nail into clinical practice; investigators reported a frequency of this complication of up to 15%.8–10,12,14,30,45 Such a high frequency of distal locking problems was not seen with any of the later IMHNs.47–52 The surgical complications of thigh pain and frequent fractures of the femoral shaft in the region of the nail tip were even considered by some investigators to contraindicate the use of the Gamma nail in all trochanteric fractures.41,46,53,54 There were two reasons for this experience. First, the Gamma nail was the first globally available IMHN, and most investigators used it for mastering the learning curve.43,53–67 Second, because of the design of the Gamma nail, the distal part of the nail had to be prereamed, and this made the diaphyseal cortex thinner at the level of the tip of the nail. The short distance of the two locking screws from the tip of the nail and the shape of the tip led to stress concentration in this region.
The insertion of locking screws is associated with certain difficulties. Causes of these complications include insufficient tightening of the bolt that fixes the nail to the targeting device, damage to the contact surfaces of the targeting device, deformation of the targeting device, incorrect inclination of the drill guide sleeve caused by soft tissue tension associated with a small or inaccurately situated incision, and manipulation with the targeting device during drilling.19 Mismatch between the targeting device and the nail may occur in unreamed IMHNs by deformation of the nail caused by its forced insertion. With greater bowing of the femur, the drill bit is not perpendicular to the cortex, mainly during insertion of the more distal locking screw, slips along the cortex and misses the hole of the nail.10,14
By the same token, the danger of damage to the cortex of the femoral shaft increases the risk of postoperative fracture in the region of the nail tip. Lacroix et al66 described a fissure of the lateral cortex when an awl was hammered in to start the hole for distal locking. Eccentric drilling may weaken the anterior, or posterior, cortex of the femoral shaft. Repeated drilling of locking holes has the same effect.12 Therefore, if the first attempt is not successful, it is recommended that the surgeon proceed to the next hole.
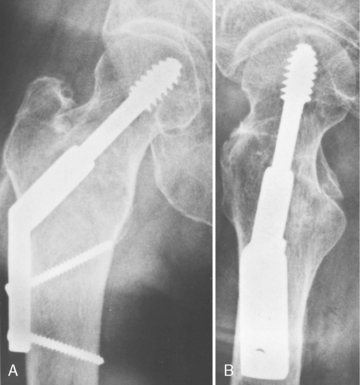
In view of frequent problems, some investigators do not consider distal locking necessary.14,46,68–70 This view applies only to pertrochanteric fractures (31A1 and 31A2). One or more lag screws may be inserted through the lateral cortex into the distal fragment and thereby stabilize the fracture and prevent its rotation (Fig. 12-15). Distal locking is always required in pertrochanteric fractures in patients with an unusually wide medullary canal, comminution of the lateral cortex of the femoral shaft, a large posteromedial fragment, or a secondary fracture line extending as far as the subtrochanteric region. A different situation obtains in intertrochanteric fractures (31A3). In the absence of distal locking, the diaphyseal fragment may rotate on the nail and cause malrotation of the limb.
A serious mistake in the treatment of intertrochanteric fractures (31A3) is locking the nail in distraction of the two main fragments. The result is impaired fracture healing, fatigue breakage of the nail, or, preferably, breakage of the locking screws, with resulting spontaneous dynamization and healing of the fracture.10 For these reasons, Bartoníček prefers dynamic locking for treatment of intertrochanteric fractures (31A3) (Fig. 12-16).
Problems with the Instrumentation Set
Distal locking may be complicated by insufficient tightening of the bolt fixing the nail to the targeting device, damage of the contact surfaces of the targeting device, or deformation of the targeting device.9,13,41,61 It is necessary to check the instrumentation set thoroughly and to take great care in attaching the targeting device correctly to the IMHN.
Reported complications also include breakage of the targeting device,9,13 the drill bit,9,41,61 the guidewire,33 or the reamer.61 Another rare complication is incorrect insertion, or insufficient tightening, of the set screw in the Gamma nail; in one reported case, this complication resulted in loosening and migration of the set screw.9
Wound Healing Disturbances and Infection
Wound healing disturbances, including seroma, hematoma, superficial infection, and deep infection, are reported in 1% to 16% of cases.44,70–73 The reports vary widely, depending on the number of surgical cases and the experience of individual investigators. Hematoma occurs in up to 10% of cases, and when nails are used, it develops very often in the incision for insertion of the lag screw. Superficial infection after nailing accounts for up to 6%51 and deep infection for 1% to 3% of hematomas.44,51 Late, mostly low-grade infections may also occur, even after the fracture has healed.9,10,38,53 On radiographs, these infections are demonstrated by osteolysis around the locking screw or the lag screw or by a periosteal reaction (Figs. 12-17 and 12-18).
Prevention
Antibiotic prophylaxis reduces the incidence of infections in hip fracture surgery.74–76 Of great importance in this respect is surgical technique and especially careful handling of the soft tissues during dissection or nail insertion. The use of wound drains remains controversial.77 Drainage is always indicated in patients who are in danger of postoperative bleeding.
Treatment
Hematoma in the wound must be evacuated as soon as possible. Prompt surgical revision is also required in patients with acute infection. If internal fixation is stable, the implant should be left in place for later removal after the fracture has healed.9,78 When the infection cannot be managed, or the implant is no longer stabilizing the fracture, it is necessary to remove the implant, heal the infection, and subsequently perform refixation. As a last resort, the Girdlestone operation may be indicated. Heinz and Vécsei9 managed seven cases of nine early infections by surgical revision; these investigators used both general and local antibiotic treatment. A late low-grade infection must be considered in patients with unexplained groin or thigh pain that persists even after the fracture is healed. After removal of the implant, a late infection usually heals without complications.
Mechanical Failure of Internal Fixation
Mechanical complications of internal fixation of trochanteric fractures, particularly varus angulation, are the most frequent and troublesome complications of operative treatment.1–15
Levels of Mechanical Failure
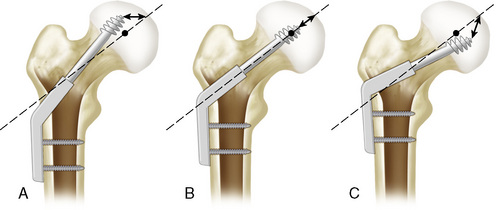
Mechanical failure of internal fixation may occur on three levels: proximally between the implant and the proximal fragment, at the level of fracture, and distally between the implant and the diaphyseal fragment79 (Fig. 12-19).
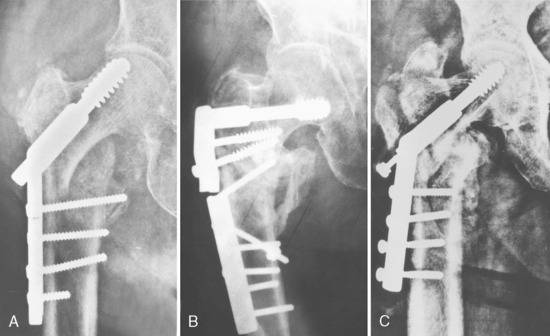
Figure 12-19 Three levels of mechanical failure of internal fixation. A, Proximal level. B, Fracture site level. C, Distal level.
Proximal Level
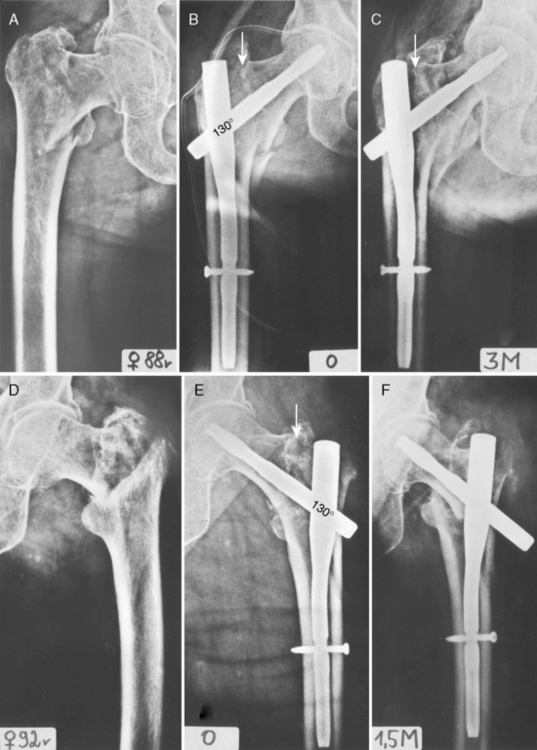
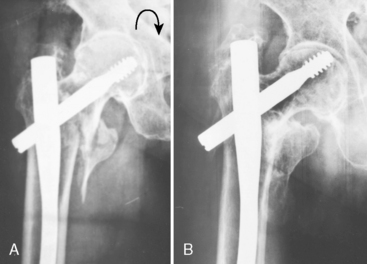
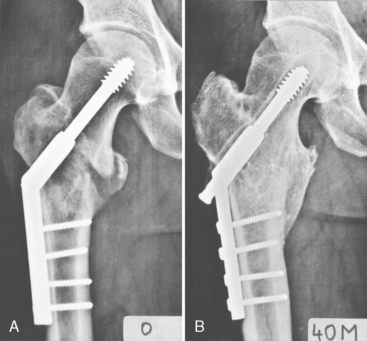
At the proximal level, the incidence of mechanical failure is the highest. Save for a few exceptions, varus tilt of the proximal fragment develops in the first few postoperative days. Cutout after several weeks, or months, is indicative of delayed union, nonunion, necrosis of the femoral neck, subcapital fracture of the femoral neck, or AVNFH (see later). The most frequent reasons for this complication are incomplete reduction and poor positioning of the lag screw in the femoral head. In less severe cases, the patient has only slight varus tilt of the proximal fragment, and the fracture may heal in this position (Fig. 12-20). If varus rotation continues, the tip of the lag screw gradually will cut out of the femoral head (Fig. 12-21).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree