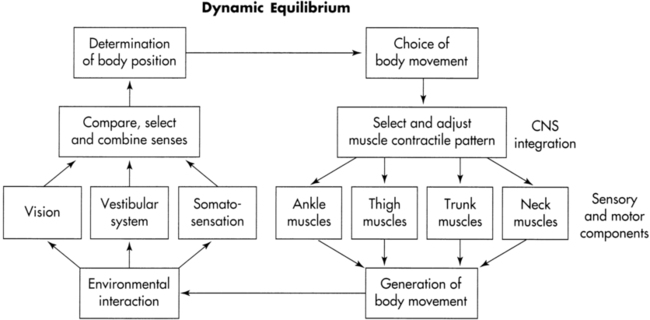
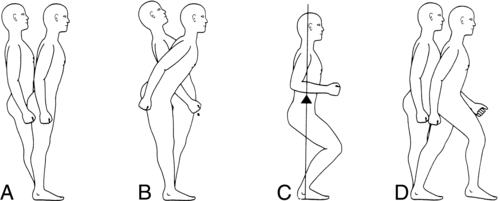
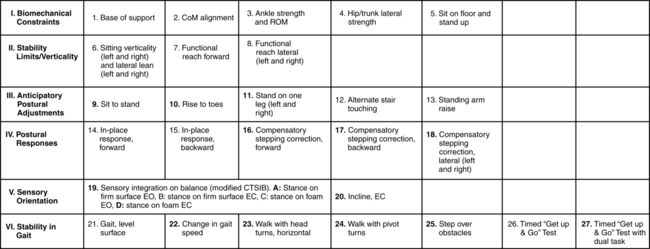
LESLIE K. ALLISON, PT, PhD and KENDA FULLER, PT, NCS After reading this chapter the student or therapist will be able to: 1. Describe both central and peripheral sensory and motor components of the postural control system. 2. List common postural control impairments found in clients with neurological problems. 3. List commonly used balance tests, and distinguish which are appropriate for clients at low, moderate, and high levels of function. 4. Differentiate how test results are used to identify body system impairments and activity limitations that limit participation. 5. Analyze the interaction of individual, task, and environmental factors that affect balance. 6. Describe how to plan and progress balance exercise programs to increase the use of, or compensation with, available sensory inputs. 7. Describe how to plan and progress balance exercise programs to facilitate anticipatory postural adjustments to prevent balance loss and provoke automatic postural responses to regain balance after unexpected disturbances. 8. Describe how to plan and progress balance exercise programs to increase the control of center of gravity in upright postures and during gait. 9. Describe how to increase the difficulty level of balance exercise programs in order to promote the automaticity of postural control during functional activities. 10. Identify and analyze the function of the vestibular system. 11. Describe how to facilitate adaptation and central nervous system reorganization to regain control of balance and decrease dizziness. 12. Identify patterns of recovery that influence choices of intervention. Balance Function and Disorders No matter what the neurological diagnosis, a disease or injury that affects the nervous system is likely to compromise one or more of the postural control mechanisms. For example, clients with such diverse diagnoses as stroke, head trauma, spinal cord injury, peripheral neuropathy, multiple sclerosis (MS), Parkinson disease, cerebellar dysfunction, cerebral palsy, and Guillian-Barré syndrome all experience disequilibrium problems. One common thread among all these different medical diagnoses is the presence of balance impairments. Clients with different medical diagnoses may have the same balance impairments, and clients with the same medical diagnosis may have different balance impairments depending on which portions of the postural control system are involved.1 To optimally understand and manage balance problems, a test of each balance component and the interactive nature of the components is important. The traditional medical “diagnostic” model does not provide this information and is not the most beneficial model for planning balance rehabilitation interventions. The medical diagnosis is relevant: knowing whether deficits are permanent or temporary, and whether recovery or progressive decline is expected, is critical. This medical prognostic information will assist physical and occupational therapists in goal setting and intervention planning. The International Classification of Functioning, Disability and Health (ICF) model described in Chapter 1 and illustrated in Figure 1-1 describes the interactions of body function and structure problems (impairments) and activity limitations as seen in clients with balance disorders, and how these functional activity limitations restrict an individual’s ability to participate in life situations, thus decreasing quality of life. Balance impairments negatively affect function, often reducing the individual’s ability to participate fully in life.2 These impairments often restrict activity levels, produce abnormal compensatory motor behavior, and may require devices for support or assistance from another person. Falls can result when imbalance is severe, leading to secondary injuries. To avoid these consequences and advance the functional status of clients, therapists should understand both the demands that various environments and functional tasks place on postural control systems and the impairments that may diminish the ability of those systems to respond adequately. Balance is a complex process involving the reception and integration of sensory inputs and the planning and execution of movement to achieve a goal requiring upright posture. It is the ability to control the center of gravity (COG) over the base of support in a given sensory environment.3,4 The COG is an imaginary point in space, calculated biomechanically from measured forces and moments, where the sum total of all the forces equals zero. In a person standing quietly the COG is located just forward of the spine at approximately the S2 level. With movement of the body and its segments, the location of the COG in space constantly changes. The base of support is the body surface that experiences pressure as a result of body weight and gravity; in standing it is the feet, and in sitting it includes the thighs and buttocks. The size of the base of support will affect the difficulty level of the balancing task. A broad base of support makes the task easier; a narrow base makes it more challenging. The COG can travel farther while still remaining over the base if the base is large. The “shape” of the base of support will alter the distance that the COG can move in certain directions. Any given base of support places a limit on the distance a body can move without either falling (as the COG exceeds the base of support) or establishing a new base of support by reaching or stepping (to relocate the base of support under the COG). This perimeter is frequently referred to as the limit of stability or stability limit.3,5 It is the farthest distance in any direction a person can lean (away from midline) without altering the original base of support by stepping, reaching, or falling. Early studies of postural control mechanisms using selectively lesioned cats and primates focused on reflexive and reactive equilibrium responses that are relatively “hard-wired.”6 These valuable studies brought to light certain stereotypical motor responses to specific sensory stimuli, such as the crossed extension reflex or tonic neck reflexes. There is no doubt that these reflexive and reactive responses—for example, the vestibuloocular reflex (VOR) and the protective extension reactions—are foundational to normal postural control. However, the postural control system encompasses much more than these subcortically driven components. Balance abilities are heavily influenced by higher-level neural circuitry and other systems (e.g., cognitive, musculoskeletal), as well.5 In addition, the nervous system is influenced by and responsive to the demands placed on it by the tasks being accomplished and the environments in which those tasks are performed.7–9 All of these facets are included in a systems approach to dynamic equilibrium.10–12 Examination and intervention methods based on this systems model have consequently evolved.11,13 The dynamic systems model for dynamic equilibrium recognizes that balance is a result of interactions among the individual, the task(s) the individual is performing, and the environment in which the task(s) must be performed. These interactions are represented in Figure 22-1. Within the individual, both sensory inputs and processing systems (left side of figure) and motor planning and execution systems (right side of figure) are critical. Both peripheral components (lower part of figure) and central components (upper part of figure) of the systems are involved in the cycle. The cycle is driven both by purposeful choices of the individual (tasks) and by demands placed on the individual by the environment. Successful function of the sensory systems allows recognition of body position and motion in relation to self and the world. The desired outcome from the motor systems is the generation of movement sufficient to maintain balance and perform the chosen, goal-directed task(s). The three primary peripheral sensory inputs contributing to postural control are the bilateral receptors of the somatosensory, visual, and vestibular systems.4,10 Somatosensory receptors located in the joints, ligaments, muscles, and skin provide information about muscle length, stretch, tension, and contraction; pain, temperature, and pressure; and joint position. The feet, ankles, knees, hips, back, neck, and eye muscles all furnish useful information for balance maintenance. Somatosensation is the dominant sense for upright postural control and is responsible for triggering automatic postural responses (APRs). Somatosensory loss significantly impairs balance. Loss of peripheral somatosensation occurs in clients with loss or disease of or injury to the peripheral sensory receptors or afferent sensory nerves. Examples include clients with diabetic neuropathy, peripheral vascular disease, spinal cord injury, and amputation. Visual receptors in the eyes perform dual tasks. Central (or foveal) vision allows environmental orientation, contributing to the perception of verticality and object motion, as well as identification of the hazards and opportunities presented by the environment.10 For example, a kayaker may see rocks in a stream as a hazard to be avoided, whereas a hiker who wants to cross the stream may see the same rocks as a welcome opportunity. Peripheral (or ambient) vision detects the motion of the self in relation to the environment, including head movements and postural sway. Peripheral vision is largely subconscious, whereas central visual inputs tend to receive more conscious recognition.10 Both are normally used for postural control. Vision is critical for feed-forward, or anticipatory, postural control in changing environments. This includes planning for functional movements such as reaching and grasping, and especially for successful navigation during gait. Vision loss also impairs balance. Loss of peripheral visual inputs occurs in clients with disease of or injury to the eyes or afferent cranial nerves. Examples include clients with cataracts, macular degeneration, glaucoma, or diabetic retinopathy. The vestibular system provides the central nervous system (CNS) with information about the position and motion of the head. The position of the head in relation to gravity is detected through the otolith system. Horizontal and vertical accelerations, as in riding in a car or an elevator, are also detected by the otoliths.14 Movements of the head are detected through the semicircular canals. Head movement stimulates both sets of semicircular canals, so that the vestibular nerve on one side becomes inhibited while the other becomes excited. The vestibular system provides sensory redundancy in the information obtained from each separate vestibular apparatus. If the peripheral vestibular system is damaged on one side, the information can be captured by the intact canals on the opposite side. The vestibular system is critical for balance because it uniquely identifies self-motion as different from motion in the environment. Box 22-1 describes the sensory components of the vestibular system. Vestibular loss also impairs balance. Loss of peripheral vestibular inputs occurs in clients with disease of or injury to the peripheral sensory receptors or afferent cranial nerves. Examples include clients with head injury involving temporal bone damage, acoustic neuroma, benign positional vertigo (BPV), or Meniere disease. For a comprehensive review of the vestibular system and vestibular disorders, please see the vestibular section of this chapter beginning on page 689. The brain processes all the environmentally available sensory information gathered by the peripheral receptors in varying degrees. This processing is usually referred to as multisensory integration or sensory organization.4,10 Central sensory structures function first to compare available inputs between two sides and among three sensory systems. The somatosensory system alone is unable to distinguish surface tilts from body tilts. Also, the visual system by itself cannot discriminate movement of the environment from movement of the body.14 The vestibular system by itself cannot tell if head movement through space is produced by neck motion or trunk and hip motion. Therefore the brain needs information from all three senses to correctly distinguish self-motion from motion in the environment. When changes in the environment occur, the relative availability, accuracy, and usefulness of information from the three sensory systems may also change. Sensory organization also includes an adaptive process, called multisensory reweighting, that permits the CNS to prioritize the sources of sensory information when environmental conditions change.15,16 Available, accurate, and useful information is “upweighted,” whereas unavailable, inaccurate, or less-useful information is “downweighted.” For example, in dark environments, vision would be downweighted and somatosensory and vestibular information would be upweighted. This adaptive process is imperfect, however, and balance is not as well controlled when any sense must be downweighted as it is when all three senses are available and accurate. Individuals with peripheral sensory loss or central sensory processing deficits may have difficulty reweighting quickly and fully. This impairs their ability to adapt to, and remain stable in, changing environments.17 Intrinsic central sensory processing impairments also can produce sensory conflict. An adult hemiplegic patient with pusher syndrome illustrates an inability to integrate visual, vestibular, and somatosensory inputs for midline orientation. Within a single system, discrepancies between the sides are also problematic. Unequal firing from opposite sides of the vestibular system, as in unilateral vestibular hypofunction, produces a mismatch that is subsequently interpreted as head rotation when head movement does not occur. This spinning sensation is known as vertigo.14 Vertigo is resolved if the brain is able to adapt to the mismatch. For further information on vertigo, refer to the section on the vestibular system. Finally, the central processing mechanisms combine any available and accurate inputs to answer the questions “Where am I?” and “How am I moving?” This includes both an internal relation of the body segments to one another (e.g., head in relation to trunk, trunk in relation to feet) and an external relation of the body to the outside world (e.g., feet in relation to surface, arm in relation to handrail). CNS disease or trauma involving the parietal lobe may impair these processing mechanisms so that even available, accurate sensory inputs are not recognized or incorporated into determinations of position and movement.18,19 Impairments of central sensory processing may occur after stroke, head trauma, tumors, or aneurysms; with disease processes such as MS; and with aging. Whereas sensory processing allows the interaction of the individual and the environment, motor planning underlies the interaction of the individual and the task. Aside from reflexive activity such as breathing and blinking, most motor actions are voluntary and occur because some goal is to be achieved. That is not to say that reflexes occur separately from volitional movements; for example, the vestibuloocular reflex is active concurrently with visual tracking activity, but most actions occur because of some purposeful intent.14 These task intentions precede motor actions.10,20 Wrist and hand movements vary depending on what is to be grasped (a cup versus a doorknob); foot placement and trunk position vary depending on what is to be lifted (a heavy suitcase versus a laundry basket). The initiation of volitional motor actions depends on intention, attention, and motivation.10,21 Once an objective (“Where do I want to be?” “What do I want to do?”) has been chosen, the next step in motor planning is to determine how to best accomplish the goal given the many options that are potentially available. For example, when the task demands fine skills or accuracy, the dominant hand is preferred; when the task involves lifting a large or heavy object, both hands are preferred. In addition to which limbs, joints, and muscles will be used, motor planning also adjusts the timing, sequencing, and force modulation. This can be demonstrated in various reaching tasks. Reaching to remove a hot item from the oven will occur slowly, whereas reaching to put an arm through a sleeve will occur more quickly. Optimal motor plans are developed with knowledge of self (abilities and limitations), knowledge of task (characteristics of successful performance), and knowledge of the environment (risks and opportunities).21 Clients with CNS disorders often have central motor planning and control system problems. After a stroke, clients may have hypertonus and poor reciprocal inhibition; clients with head trauma may have difficulty initiating or ceasing movements; clients with Parkinson disease exhibit bradykinesia; and those with cerebellar ataxia display modulation problems.22 Movement is accomplished through the bilateral joints and muscles. Normal range of motion (ROM), strength, and endurance of the feet, ankles, knees, hips, back, neck, and eyes must be present for the execution of the full range of normal balance movements. Decreased ankle dorsiflexion ROM, for example, restricts the forward limits of stability. Strength deficits are a primary cause of movement abnormalities in both central and peripheral nervous system disorders. In addition, weakness may be the result of force modulation deficits or disuse.11 Balance is directly affected by loss of strength. For example, weakness of the hip extensors and abductors will impede successful use of a hip strategy for upright trunk control. Initially adequate toe clearance may diminish with fatigue. Many clients with neurological issues also have stiffness and contractures as a result of persistent weakness or hypertonus. Restrictions in ROM also limit balance abilities. The ability to achieve static postural alignment, although necessary for normal balance, is not sufficient to allow volitional functions. Adequate strength (to control body weight and any additional loads) through normal postural sway ranges is needed to permit dynamic balance activities such as reaching, leaning, and lifting. Postural control demands are increased during gait because the forces of momentum and the interaction between recruitment, timing, and velocity also must be regulated.23 Traditionally considered orthopedic problems, deficits in strength, ROM, posture, and endurance have a great impact on balance abilities. Attention must be given to these musculoskeletal system problems in examination of and intervention for clients with neurological diagnoses. Balance abilities are also influenced by other systems. Attention, cognition and judgment, and memory are critical for optimal balance function and are often impaired in hemiplegic and head-injured clients as well as those who have progressive neurological disorders. Attentional deficits reduce awareness of environmental hazards and opportunities, interfering with anticipatory postural control.12 When balance is threatened, an inability to allocate attention to the necessary task of balance versus a secondary, less necessary task increases the risk of falls. Cognitive problems such as distractibility, poor judgment, and slowed processing also increase the risk of falls. Memory loss may preclude recall of safety measures. Depression, emotional lability, agitation, or denial of impairments also can increase the risks for loss of balance. In addition to having a direct impact on balance abilities themselves, these cognitive and behavioral problems impede motor learning processes, which are crucial for the relearning of balance skills. The systems model of postural control previously presented illustrates the constant cycle that simultaneously occurs at many levels. Attention and intention allow feed-forward processing for active sensory search of the environment and motor planning, both of which are needed for anticipatory postural control. Movements are initiated and executed with resultant sensory experiences and error detection, or feedback. Successful movements are repeated and refined; unsuccessful ones are modified. The nature of this cycle presents the clinician with opportunities for intervention after the appropriate examination of sensory, motor, and cognitive functions. Through feedback and practice, balance abilities can improve.24 Many levels of neuromuscular control must be functioning to produce normal postural movements. At the most basic level, reflexes and righting reactions support postural orientation. The VOR and the vestibulospinal reflex (VSR) contribute to orientation of the eyes, head, and body to self and environment.10 When motion of the head is identified by the semicircular canals, it triggers a response within the oculomotor system called the vestibuloocular reflex. This causes the eyes to move in the opposite direction of the head but at the same speed. Stimulation of the otoliths drives the eyes to respond to linear head movement. Quick movements of the head will trigger the VOR.25 The VOR allows the coordination of eye and head movements. When the eyes are fixed on an object while the head is moving, the VOR supports gaze stabilization. Visuo-ocular responses often work concurrently with the VOR. They permit “smooth pursuit” when the head is fixed while the eyes move and visual tracking when both the eyes and the head move simultaneously.10 The VSR helps control movement and stabilize the body. Both the semicircular canals and the otoliths activate and modulate muscles of the neck, trunk, and extremities after head movement to maintain balance. The VSR permits stability of the body when the head moves and is important for the coordination of the trunk over the extremities in upright postures. Righting reactions support the orientation of the head in relation to the trunk and the head position relative to gravity and include labyrinthine head righting, optical head righting, and body-on-head righting.10 At the next level, automatic postural responses operate to keep the COG over the base of support. They are a set of functionally organized, long-loop responses that act to keep the body in a state of equilibrium.3,4 Functionally organized means that the responses, although stereotypical, are matched to the perturbing stimulus in direction and amplitude. If the stimulus is a push to the right, the response is a shift to the left, toward midline. The larger the stimulus, the greater the response. Automatic postural responses always occur in response to an unexpected stimulus and are typically triggered by somatosensory inputs. Because they occur rapidly, in less than 250 ms, they are not under immediate volitional control. Four automatic postural responses have been described. Ankle strategy describes postural sway control from the ankles and feet. The head and hips travel in the same direction at the same time, with the body moving as a unit over the feet (Figure 22-2, A). Muscle contractile patterns are from distal to proximal (i.e., gastrocnemius, hamstrings, paraspinals). This strategy is used when sway is small, slow, and near midline. It occurs when the surface is broad and stable enough to allow pressure against it to produce forces that can counteract sway to stabilize the body. Ankle strategy is typically used to control anterior-posterior sway, because most of the degrees of freedom at the ankle are in this direction. Hip strategy involves postural sway control from the pelvis and trunk. The head and hips travel in opposite directions, with body segment movements counteracting one another (Figure 22-2, B). Muscle contractile patterns are from proximal to distal (i.e., abdominals, quadriceps, tibialis anterior). This strategy is observed when sway is large, fast, and nearing the limit of stability or if the surface is too narrow or unstable to permit effective counterpressure of the feet against the surface. Hip strategy is used to control both anterior-posterior and medial-lateral sway. Hip strategy in the medial-lateral direction involves weight shifts from foot to foot; any client with difficulty weight-shifting quickly and accurately will have difficulty with medial-lateral hip strategy. Suspensory strategy involves a lowering of the COG toward the base of support by bilateral lower-extremity flexion or a slight squatting motion (Figure 22-2, C). By shortening the distance between the COG and the base of support, the task of controlling the COG is made easier. This strategy is often used when a combination of stability and mobility is required, as in windsurfing. Stepping and reaching strategies involve steps with the feet or reaches with the arms in an attempt to reestablish a new base of support with the active limb(s) when the COG has exceeded the original base of support (Figure 22-2, D). A successful stepping strategy is the best way to avoid a fall after a slip or trip. Misconceptions about these APR strategies are common. First, these strategies do not function in daily life as separately as they are described in the early research literature. In quiet standing, for example, frequency analysis of unperturbed postural sway in healthy adults reveals that both ankle and hip strategies occur in combination, simultaneously.26 In perturbation studies, mixed use of strategies is often seen unless the perturbation is clearly below or above certain-sized thresholds. Second, these strategies occur in response to disturbances from all directions, not just in pure anterior-posterior or medial-lateral directions.27 Third, although these strategies are stereotypical in humans, great individual variation in strategy selection and performance comes from other influential factors. For example, many people use stepping strategy for most perturbations unless specifically instructed not to step or unless the conditions do not permit a step. An anxious person may reach or step much sooner than a relaxed person with similar physical deficits. Last, all these strategies do not occur in sequence with every balance disturbance.28,29 In other words, individuals normally do not try ankle strategy and wait until it fails before trying hip strategy, then wait until it fails before trying stepping strategy (although early learning may involve such exploration). Because these responses must occur extremely rapidly to prevent balance loss, such a sequential approach would be inefficient and ineffective. Instead, the normal response is the emergence of the single strategy best suited to the particular perturbation, the limitations of the individual, and the conditions in the environment. Abnormal use of automatic postural responses is often observed in individuals with neurological disorders. Clients with vestibular deficits typically rely on ankle strategy, which permits the head to remain aligned with the body and sustains congruence between vestibular and somatosensory inputs. Use of hip strategy may be modified or limited because when the head is moving in the opposite direction as the COG, vestibular and somatosensory inputs are not congruent. Activities that require use of hip strategy, such as standing in tandem or on one leg, can be a problem for clients with bilateral vestibular loss or an uncompensated vestibular lesion. However, some cases involve excessive use of hip strategy on a level surface (when an ankle strategy would suffice).30 This may reflect abnormal integration of the somatosensory and vestibular information. If peripheral somatosensation is impaired, as in diabetic neuropathy, or central sensory weighting of somatosensory inputs is inadequate, hip strategy may dominate. Anticipatory postural adjustments are similar to automatic postural responses, but they occur before the actual disturbance.20 If a balance disturbance is predicted, the body will respond in advance by developing a “postural set” to counteract the coming forces. For example, if an individual lifts an empty suitcase thinking it is full and heavy, the anticipatory forces generated before the lift (to counter the anticipated weight) will cause excessive movement and brief instability. Failure to produce these anticipatory adjustments increases the risk of sudden balance loss, creating the need to use rapid, reactive automatic postural responses to prevent a fall. For clients with deficits in reaction time or automatic postural responses, superior use of anticipatory postural control can help the client avoid the unexpected perturbations that make automatic postural responses necessary. When present, activity limitations need to be identified and measured. Functional scales are typically used to determine the presence and severity of these limitations, not necessarily why those limitations exist. From these functional tests, decisions can be made about whether to treat and, if so, what tasks need to be practiced. If treatment is indicated, clinicians must make judgments about what to treat. Further testing to identify and measure impairments is then necessary to know what systems are involved. A comprehensive evaluation of balance includes both functional and impairment tests.12 No single quick-and-easy test of balance can adequately cover the many multidimensional aspects of balance, although many such tests have great value as screening tools. However, a comprehensive test battery, called the Balance Evaluation Systems Test (BESTest), based on the systems model has been developed that provides clinicians with a thorough examination at the impairment level (Figure 22-3).31 The BESTest takes more time to administer than, for example, a single-leg stance test, but results from the BESTest give the clinician a far more complete and accurate picture of the client’s balance impairments than any single-item test or screening test can. Armed with these results, the clinician can develop interventions specifically targeted to the impaired systems. For clients whose primary problems include imbalance, the clinician’s investment of time to perform this comprehensive test battery yields a valuable outcome. A shorter version of this test, the mini-BESTest, has subsequently been published.32 It takes less time to administer but likewise provides a less complete picture of the client’s balance systems. Specifically, it does not include any items from the biomechanical constraints or stabilities limits categories. Even so, it is superior to single-item tests or screening tests that are not based on the systems model and do not identify balance system impairments that should be addressed in the intervention plan. No single, simple test for balance is possible because balance is such a complex sensorimotor process.33 Many relatively simple balance tests exist, but not all tests are appropriate for all clients. Different tests may be needed to answer specific questions. For example, several good tests have been developed to determine the risk of falls in elderly people. These would be insufficient to discern whether an injured dancer can resume practice or an injured roofer is ready to return to work. Clinicians should understand the advantages and limitations of different balance tests to be able to select appropriate evaluative tools. Because so many balance tests are available, several questions must be asked to determine whether a test is appropriate for use.33 For what purpose and population was the test designed? Can that test be used legitimately for a different purpose or with a different population? Is it valid? Is it repeatable by different examiners or by the same examiner multiple times? Are results reliable? In what populations are they reliable? What is the threshold for this test—that is, how large must performance changes be before this test can detect them? Are normative data available for comparison? These questions are being investigated but have not yet been answered for many of the clinical balance tests commonly used by therapists with the many different neurological populations they treat. Some of the evidence already reported may be frustrating to clinicians. For example, the Timed Up-and-Go test (TUG) predicts falls in community-dwelling older adults but not in acute-care hospital populations.34,35 For several balance tests such as the Functional Reach Test, the Berg Balance Scale, and others, the cutoff scores used for accurate prediction of falls in clients with Parkinson disease are different from the cutoff scores used in older adults without Parkinson disease.36 These examples make it clear that clinicians must understand their clients and the characteristics of the various balance tests in order to select the most appropriate tests and interpret test results for each client. Balance tests can be grouped or classified by type. Different types of tests measure different facets of postural control (Table 22-1). Quiet standing (static) refers to tests in which the client is standing and the movement goal is to hold still. Disturbances to balance, called perturbations, may or may not be applied. Active standing (dynamic) tests also position the patient standing, but the movement goal involves voluntary weight shifting. Sensory manipulation tests use altered surface and visual conditions to determine how well the CNS is using and reweighting sensory inputs for postural control. Functional balance, mobility, and gait scales involve the performance of whole-body movement tasks, such as sitting to standing, walking, and stepping over objects. A few test batteries offer a combination of the preceding tests. The BESTest is the most comprehensive test battery to date. Dual-task tests have been developed to examine the effect of concurrent activities and divided attention on balance and mobility performance. A commonly accepted test for sitting balance in adults is not yet available, although clients with neurological problems often need sitting balance retraining in early stages. Clinicians typically modify standing tests or pediatric sitting tests to assess sitting balance in adult clients with neurological conditions. For example, the Functional Reach Test has been used to measure excursion in seated individuals with spinal cord injuries.37 TABLE 22-1
Balance and vestibular dysfunction
Balance
Definitions of balance
Human control of balance
The systems approach
Peripheral sensory reception
Central sensory perception
Central motor planning and control
Peripheral motor execution
Influence of other systems
Constant cyclic nature
Motor components of balance
Reflexes
Automatic postural responses
Anticipatory postural adjustments
Clinical assessment of balance
Objectives of testing
Types of balance tests

TYPE
TESTS
Quiet standing (with or without perturbation)
RombergSharpened Romberg or tandem Romberg
One-legged stance test (OLST)
Timed stance battery
Postural sway
Nudge or push
Postural Stress Test
Motor Control Test
Active standing
Functional Reach TestMulti-Directional Reach Test
Limits of stability
Sensory manipulation
Sensory Organization Test (SOT)Clinical Test of Sensory Interaction and Balance (CTSIB)
Vestibular
Vertiginous positionsHallpike-Dix maneuver
Nystagmus
Semicircular canal function
Visual-vestibular interaction
Visual acuity
Oculomotor tests
Fukuda Stepping Test
Dizziness Handicap Inventory
Functional scales
Berg Balance ScaleTimed Up-and-Go Test
Tinetti Performance-Oriented Assessment of Balance
Tinetti Performance-Oriented Assessment of Gait
Gait Assessment Rating Scale (GARS)
Dynamic Gait Index
Functional Gait Assessment
Combination test batteries
Fregly-Graybiel Ataxia Test BatteryFugl-Meyer Sensorimotor Assessment of Balance Performance
Dual task
Stops walking when talkingMultiple Tasks Test ![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Balance and vestibular dysfunction
Only gold members can continue reading. Log In or Register to continue