CHAPTER 70 Arthrodesis
INTRODUCTION
Experience with elbow arthrodesis is often related to injuries seen from military conflict.2 Most civilian experience with elbow fusion has come from spontaneous arthrodesis subsequent to infection, trauma, or rheumatic disease of the elbow (Fig. 70-1). One of the prerequisites for elbow fusion is satisfactory function of the shoulder; yet, studies from our laboratory have clearly shown that the increased shoulder motion cannot compensate for loss of elbow motion (Fig. 70-2).17
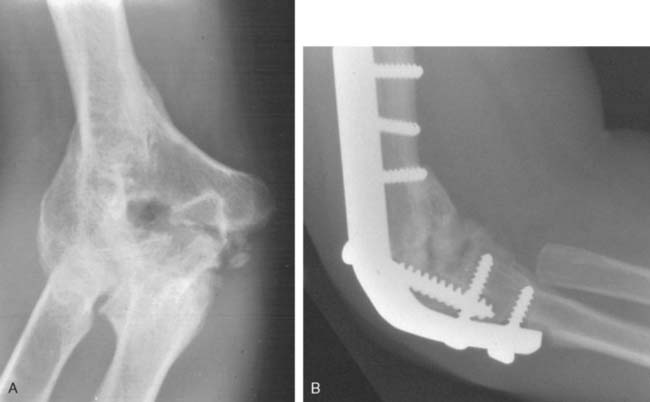
FIGURE 70-1 Spontaneous arthrodesis (A) is more common than surgically performed fusion (B) in a civilian population.
Biomechanical and clinical studies have demonstrated that compensatory spinal column and wrist motions are used to improve function after elbow arthrodesis.17 Thus, limited function (motion) in these areas may be a relative contraindication to elbow arthrodesis. When disease involves both the elbow and the shoulder, arthroplasty must, therefore, be selected. In addition, arthrodesis is not indicated for bilateral elbow disease because the functional limitations are too great. If bilateral arthrodesis is performed, one elbow should be fused in 90 degrees of flexion for personal care and hygiene functions and the other in 45 to 65 degrees of flexion for other uses.9,17 Functionally, a limited range of 100 degrees in midposition is enough for most daily activities, but removing all elbow motion restricts the majority of necessary daily functions.14 Hence, some patients request fusion take-down and total elbow even after many years (see Chapter 58).
POSITION
The optimal position for fusion depends on associated joint involvement, gender, the patient’s occupation, or specific functional requirements. Traditionally, 110 degrees is a more functional position.26 For men, 90 degrees of flexion is probably the best position of arthrodesis in a dominant arm that has good shoulder and wrist motion.16 In this position, the hand can reach the mouth with adaptive neck, shoulder, and wrist motion, and writing may be done comfortably. This has recently been challenged by one recent study suggesting special needs for the nondominant arm may prompt fusion in 30 degrees or 60 degrees of flexion, if, for example, bench work or assistive movements are required.17,22 If power is not an issue, a position of 70 degrees may be desirable.
INDICATIONS
Because of the limitations mentioned earlier, arthrodesis of the elbow is not often indicated. In fact, although shoulder fusion was employed in 23 of 144 patients with brachial plexus injury, elbow fusion was not preferred in a single patient.21 If it has a place in the surgeon’s armamentarium, it is for younger patients with post-traumatic unilateral arthrosis of the elbow who require a strong and stable joint.2 In patients older than 45 years who have bilateral disease and limited shoulder or wrist motion, arthroplasty, with or without joint replacement, is preferable. For unilateral postinfectious arthrosis, Rashkoff and Burkhalter proposed plate fixation of contaminated traumatic injuries of the elbow with chronic sepsis.13,20 Arthrodesis may be difficult to achieve after failed total elbow arthroplasty and is rarely indicated.11,27 It has yet to be performed at the Mayo Clinic after more than 1700 elbow replacements.
TECHNIQUE
Most of the limited reports on arthrodesis deal with the various techniques.1,3,11,15,18 The elbow is one of the most difficult joints to fuse surgically. The hand and the forearm act as a long lever arm that produces strong bending forces across the potential fusion site. Success rates have improved considerably with adjunctive internal fixation and intramedullary bone grafting.11
HISTORICAL SURGICAL TECHNIQUES
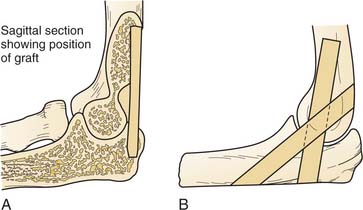
Steindler25 described a single posterior tibial cortical graft keyed into the olecranon for fusion (Fig. 70-3A). Brittain developed a technique of crossed grafts through the elbow joint5,7 (see Fig. 70-3B). Noting that gravitational forces tended to compress the ends of the graft, he believed that the crossing of the grafts was important. Koch and Lipscomb12 have described a modification of this technique in which a tibial graft is placed through a large drill hole in the humerus and ulna, and other cancellous bone grafts are added to the joint.
Staples24 uses a corticocancellous iliac graft through the posterior portion of the elbow and oblique hum-eral and olecranon intra-articular resection (see Fig. 70-3C).
STABILIZATION
Today, rigid fixation with supplemental autogenous or allograft bone is preferred. In the presence of active infection, external skeletal fixation has been preferred; however, fusion with plate stabilization, antibiotics, and an open wound can also succeed.13,20 In the presence of long-standing sepsis or arthrosis with limited motion and minimal deformity, arthrodesis may be achieved with limited internal fixation (screws), with or without bone grafts.11 If significant instability or deformity is present preoperatively, internal fixation with screws and supplemented with external skeletal fixation or plates should be used. Today, data clearly favor use of internal fixation.10 External fixation alone was successful in only five of nine in a recent series from Germany.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree