Anesthesia for Hip Surgery
Options and Risks
Carlos B. Mantilla
Key Points
Introduction
Patients undergoing hip surgery pose specific challenges to the anesthesiologist. Old arthritic and young trauma patients may require hip surgery. The breadth of the patient population with its diverse comorbid conditions demands detailed preoperative preparation. Ambulatory or inpatient procedures and multistage surgeries add particular anesthetic requirements. Furthermore, the varied surgical techniques, treatment approaches, and positioning needs, as well as the assortment of postoperative analgesic and rehabilitation strategies, are important perioperative considerations that are best approached in a comprehensive way, starting with the anesthetic plan.
Health care practitioners providing anesthesia for orthopedic surgery, including hip surgery, must keep pace with the growing number of surgical techniques while maintaining a broad range of skills in advanced airway management, regional anesthesia, intraoperative blood salvage, and invasive physiologic monitoring of hemodynamic and neurologic function. Perioperative thromboprophylactic strategies require detailed knowledge of their interaction with anesthetic agents and techniques. It is important to note that the number of hip surgeries performed annually has continually risen over the past several decades,1,2 and this number is expected to increase further with the aging of the population, and as improved perioperative care of the hip surgery patient allows ever older patients to undergo surgery.
This chapter reviews the options and risks associated with anesthesia for hip surgery. Specific consideration is given to patient and procedural characteristics that may influence perioperative care and long-term outcomes. Available evidence is discussed, and areas of uncertainty are highlighted as they relate to anesthetic options and risks. Related topics such as perioperative transfusion, analgesic and medical management, and morbidity and mortality after hip surgery are addressed in other chapters of this book.
Anesthetic Techniques for Hip Surgery: Options
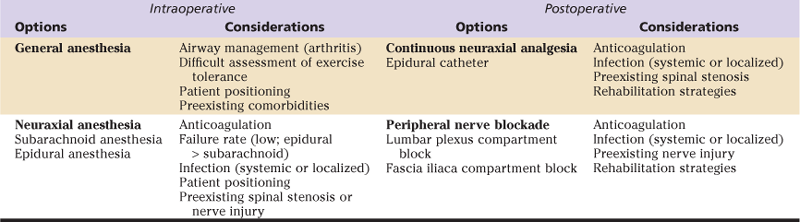
Surgery of the hip lends itself to regional anesthetic techniques, and the relative risks and benefits of regional versus general anesthesia have been the subject of intense debate. General anesthesia is safe and universally effective, whereas regional anesthesia offers advantages in specific surgical populations and is associated with a low failure rate in expert hands (Table 24-1). When combined in a postoperative multimodal analgesic regimen, regional anesthesia can provide additional benefits, minimizing patient discomfort while permitting early rehabilitation and hospital discharge in a cost-effective manner.3,4
Table 24-1
Anesthetic Options and Perioperative Management Considerations for Patients Undergoing Hip Surgery
Preoperative evaluation of the patient scheduled for hip surgery must address a number of specific and important factors present in this surgical population.5,6 Underlying pathology and conditions necessitating surgery will affect preoperative preparation of the orthopedic patient. For instance, preparation for emergency surgery in a young, presumably healthy patient with traumatic hip fracture clearly differs from that for elective joint replacement in an elderly patient with multiple comorbidities. Identifying patient-specific conditions that may place the patient at higher risk for perioperative complications is particularly important in formulating the anesthetic plan.
The presence of arthritis (e.g., rheumatoid arthritis, osteoarthritis, ankylosing spondylitis) may indicate potential difficulties in airway management and patient positioning. In particular, involvement of the cervical spine and the temporomandibular joint may limit cervical range of motion and mouth opening, respectively, requiring adjunct airway management strategies beyond direct laryngoscopy (e.g., use of a fiberoptic bronchoscope, videolaryngoscopy). Laryngeal involvement may predispose patients to vocal cord dislocation with intubation or placement of laryngeal airway devices (e.g., laryngeal mask airway). Limited shoulder or contralateral hip range of motion may limit the ability of a patient to tolerate lateral decubitus or other positions (e.g., lithotomy) needed for a specific surgical approach. These positioning requirements are not circumvented with the use of general anesthesia because both neurologic and vascular injuries may occur if patients are positioned in ways that they would not tolerate while awake.
The functional impact of cardiovascular disease (e.g., coronary artery disease) may be difficult to ascertain in patients who are limited by joint pain and who do not routinely exert themselves physically. These patients may necessitate specific cardiac evaluation, including imaging studies (e.g., dobutamine stress echocardiography), or beta blocker therapy for control of intraoperative heart rate, depending on the presence of cardiovascular risk factors.7 Risk factors include (1) history of myocardial infarction (longer than 1 month before surgery) or abnormal Q waves on electrocardiogram; (2) history of prior or compensated congestive heart failure; (3) diabetes mellitus requiring insulin treatment; (4) renal insufficiency (serum creatinine >2 mg/dL); and (5) history of cerebrovascular disease (defined as transient ischemic attack or stroke).7,8 Although advanced age is no longer included as a clinical risk factor for cardiovascular risk, patients older than 70 years of age commonly have coexisting diseases that may place them at higher risk for perioperative complications9–11 and may affect long-term outcomes after hip arthroplasty.12,13
General Anesthesia
General anesthesia provides safe and effective anesthesia for surgical procedures around the hip. Adult patients are commonly induced using intravenous agents and are maintained with a combination of inhaled volatile anesthetic agents and intravenous opioid analgesics with optional neuromuscular blocking agents. Deep levels of muscle relaxation are possible with the use of general anesthesia and are sometimes necessary for final reduction of the hip joint. General anesthesia is universally effective and thus may be resorted to after failed regional anesthesia. Induction of general anesthesia can be accomplished in a short time, although in patients with suspected difficult airways (e.g., cervical spine or temporomandibular joint arthritis), additional time may be required. Although regional anesthesia may avoid issues related to airway manipulation in such patients, the low rate of failed regional blocks may require that the airway be secured. In this sense, patient positioning and accessibility may dictate pre-emptive airway management and use of general anesthesia despite the possible use of a regional technique. For instance, obese patients with a suspected difficult airway may be best approached by using general anesthesia with awake fiberoptic intubation rather than risking failed regional anesthesia and emergent intraoperative airway management in the lateral decubitus position. These considerations must be weighed individually on the basis of patient and surgery-specific conditions.
Newer general anesthetic agents offer significant advantages for short procedures in that their effects can be closely titrated; thus general anesthesia is now commonly employed for outpatient surgical procedures. Furthermore, laryngeal airway devices that avoid laryngoscopy and endotracheal tube placement may allow safe general anesthesia to be provided with ease in multiple settings.14 Aggressive perioperative management of nausea, vomiting, and pain may facilitate discharge and minimize unanticipated hospital admissions.15,16
Regional Anesthesia
Regional anesthesia can be performed at the level of the central neuraxis or peripheral nerves. Regional anesthetic techniques offer several advantages over general anesthetic techniques, including reduced intraoperative blood loss, respiratory or cardiac derangements, and analgesic requirements, as well as a decreased incidence of postoperative nausea or vomiting.3,17-20 The use of regional anesthesia should be considered in the absence of absolute contraindications (e.g., patient refusal, infection at the site of needle puncture or its path, ongoing systemic anticoagulation).
A large, systematic review of 141 clinical trials that included 9559 patients (of which 43 trials and 3617 patients underwent lower extremity orthopedic surgery) compared outcomes of patients randomized to neuraxial blockade versus general anesthesia.17 Overall, patients randomized to neuraxial blockade experienced fewer adverse events, including deep venous thrombosis, pulmonary embolism, and death. Patients in the neuraxial block group had less blood loss and reduced requirement for transfusion of two or more units. These effects were similar in the orthopedic surgery subgroup. In keeping with these findings, a meta-analysis of 10 studies involving 678 patients after elective total hip arthroplasty reported that the risk for deep venous thrombosis and pulmonary embolism was reduced in patients randomized to neuraxial blockade (odds ratio [OR], ≈0.26).18 Intraoperative blood loss was also significantly reduced in patients undergoing neuraxial blockade (on average, by 275 mL per case). Furthermore, substantially similar results were recently reported in a meta-analysis of total knee and hip replacement surgeries21 and in a systematic review of total hip arthroplasty patients designed to reflect contemporary practice by including only studies conducted from 1990 onward.22 Regional anesthesia (including neuraxial and peripheral nerve blockade) reduced postoperative pain scores, systemic opioid requirements, and nausea and vomiting.22
Regional anesthetic techniques can be used in concert with general anesthesia. It is important to note that regional anesthesia should be avoided in the anesthetized patient because intraneural needle or catheter placement may go unnoticed. Thus, any regional anesthetic techniques should be performed before induction of general anesthesia. This aspect is particularly relevant to the pediatric practice, where performance of regional anesthesia may not be possible in unanesthetized patients. A recent report including 2236 regional anesthetic procedures performed in 1809 children under general anesthesia (1169 between the ages of 6 months and 12 years) described only two complications possibly related to peripheral nerve blocks.23 The relative safety of performing regional anesthetic procedures in children while anesthetized may reflect the type of anesthetic blocks selected. Central neuraxial blocks may be associated with a very small risk for neurologic complications in these patients.24,25 However, future studies should explore whether differences in the risk of performing regional anesthesia in anesthetized patients may depend on patient age and the regional anesthetic procedure selected, and whether nerve stimulation or ultrasound guidance might affect this risk.
Central Neuraxial Anesthesia
Sensory innervation of the hip and thigh is provided by branches of the lumbar plexus and the sacral plexus.26–28 Thus neuraxial anesthesia above this level can provide adequate conditions for surgery around the hip joint. Spinal (subarachnoid) anesthesia can be performed safely with high success rates in most patients. However, in some patients, the onset of sympathetic block might result in dangerous reductions in blood pressure and venous return, and even death.29 The use of subarachnoid catheters to permit gradual titration of local anesthetic agents was stopped because of safety concerns after reports of neurologic complications, including cauda equina syndrome, with small-diameter catheters (24-gauge).30 Although placement of large-bore catheters (e.g., 18- or 19-gauge) is possible, their use for continuous spinal anesthesia is associated with a high rate of postdural puncture headache. Placement of an indwelling epidural catheter might allow gradual dosing and incremental titration of local anesthetic agents to achieve the desired anesthetic level. Most anesthesiologists are expert at placement of spinal or epidural anesthesia, and these techniques are used extensively for orthopedic surgery of the lower extremities.
Several major issues must be appraised when neuraxial blockade is considered. Infectious and hemorrhagic complications may occur as a result of needle placement.31 Therefore patients must be screened for signs or symptoms of systemic or localized infection at the site of needle puncture, as well as for anticoagulant use. Sympathetic blockade may result in significant reductions in blood pressure, which are compounded by concomitant general anesthesia.32 In addition, anesthesia of the contralateral (nonsurgical) extremity and urinary retention may delay discharge from the postanesthesia care unit. In this regard, concomitant use of peripheral nerve blocks (e.g., psoas or fascia iliaca compartment block) and neuraxial anesthesia may permit substantial reductions in the dose of local anesthetic necessary to provide an adequate level of surgical anesthesia.19 The addition of subarachnoid opioids may permit the use of lower doses of local anesthetic agents.33,34 Unfortunately, although undesirable effects of neuraxial blockade can be minimized by reductions in the dose of local anesthetic, they cannot be prevented entirely. The choice and dose of local anesthetic agent (e.g., bupivacaine, ropivacaine) must be tailored individually according to patient, surgeon, and procedural characteristics. If adequate surgical anesthesia must be ensured (e.g., in an obese patient with suspected difficult airway), then larger anesthetic doses may be needed, even if this results in delayed discharge from the postanesthesia care unit. Additional studies into the safety and efficacy of short-acting local anesthetic agents for use in the central neuraxis are needed, because significant, even transient, neurologic symptoms have been reported with subarachnoid lidocaine.30,35
Combined spinal-epidural techniques are possible that combine the near-complete success rate of spinal anesthesia with the flexibility of additional dosing provided by the epidural catheter. Prolonged intraoperative anesthesia is possible, and if desired, postoperative analgesia can be provided via an epidural infusion.
Peripheral Nerve Blockade
The lumbar plexus is located within the psoas muscle and is formed by the ventral rami of segmental lumbar nerves from L2 to L4.26,36 Branches of the lumbar plexus include the lateral femoral cutaneous nerve of the thigh (formed by L2 and L3 nerves), the obturator nerve (L2 to L4), and the femoral nerve (L2 to L4). The lumbar plexus also contributes to the genitofemoral nerve (with L1, L2, and sometimes T12 nerves) and the sciatic nerve (with L4 and L5 nerves, and sacral nerves S1 through S3).
The lumbar plexus provides near-complete sensory innervation to the hip joint. In a detailed anatomic study of the innervation of the hip joint,27 anterior and medial portions of the joint capsule were found to be innervated by articular branches of the femoral and obturator nerves, and it was noted that the posteromedial capsule is innervated at least in part by articular branches from nerves to the quadratus femoris. However, the posterior capsule is also innervated by articular branches from the sciatic nerve, and the posterolateral capsule receives innervation from the superior gluteal nerve (L5-S1 nerves). Therefore surgical anesthesia requires anesthesia of both the lumbar plexus and the sacral plexus.31
Peripheral nerve blockade for hip surgery can thus be performed by a posterior approach to the lumbar plexus within the psoas compartment (Fig. 24-1) or by an anterior approach at the fascia iliaca or femoral compartment (Fig. 24-2). These approaches have been shown to enhance postoperative analgesia and reduce opioid analgesic requirements during the perioperative period,37–40 but some studies suggest that the functional benefit may be limited.41–44 Some anterior approaches do not consistently produce anesthesia of the obturator or lateral femoral cutaneous nerve.45 In this sense, a posterior approach seems more reliable in producing anesthesia of all three nerves, although epidural spread may not be uncommon (≈10%).38 However, neither approach to the lumbar plexus resulted in sacral plexus anesthesia in a small prospective study involving 80 patients.45 At this point, definitive, multicenter, randomized studies involving a large number of patients are lacking. It seems that the choice of peripheral nerve blockade must reflect the surgical approach, the expected surgical duration, and the specific technique. Future studies should address these issues directly.
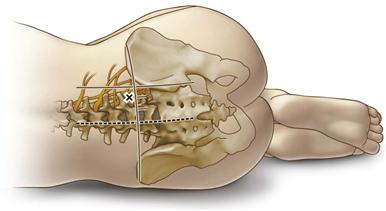
Figure 24-1 Anatomic landmarks for blockade of the lumbar plexus at the psoas compartment. (Redrawn from Hebl JR, Lennon RL: Mayo Clinic atlas of regional anesthesia and ultrasound-guided nerve blockade, Rochester, Minn, 2010, Mayo Clinic Scientific Press, p 373.)
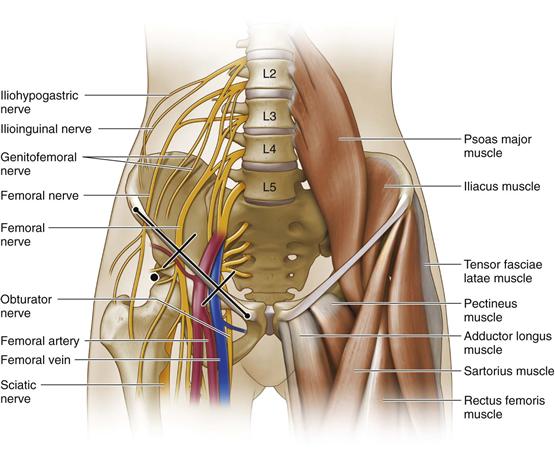
Figure 24-2 Anatomic landmarks for fascia iliaca compartment block. (Redrawn from Hebl JR, Lennon RL: Mayo Clinic atlas of regional anesthesia and ultrasound-guided nerve blockade, Rochester, Minn, 2010, Mayo Clinic Scientific Press, p 339.)
Psoas compartment blockade can be achieved via different landmark-based approaches (see Fig. 24-1). In general, these are performed with the patient in a lateral decubitus position,26,36 with the use of a nerve stimulator and a needle with an uninsulated tip. The intercristal line (between the iliac crests bilaterally) and a line parallel to the lumbar spinous processes passing through the ipsilateral posterior superior iliac spine are used as general landmarks. Needle placement is such that a perpendicular path results in contact with the L5 transverse process. In this regard, careful examination of routine hip x-rays that include this anatomic area is useful in determining the exact needle entry site relative to the cutaneous landmarks. A motor response is sought using peripheral nerve stimulation (starting current ≈1.2 to 2.0 mA, depending on patient comfort), and once a “twitch” in the appropriate distribution (anterior thigh) is elicited, current is gradually reduced to approximately 0.5 mA. A twitch in both the anterior and the posterior thigh would suggest stimulation of lumbosacral roots epidurally and necessitates needle redirection. An indwelling catheter is usually placed within the belly of the psoas muscle.
Fascia iliaca compartment blockade can be accomplished easily in most patients while supine, without the need for repositioning (see Fig. 24-2). Needle insertion occurs 1 cm inferior to the point between the lateral and middle thirds of a line between the anterior superior iliac spine and the pubic tubercle.39,46,47 Resistance is felt upon passing first the fascia lata and subsequently the fascia iliaca, at which point a single injection of 20 to 40 mL of local anesthetic solution and/or insertion of an indwelling catheter can be performed. Ultrasound-guided visualization may improve the reliability of block placement.48 In a randomized, double-blind, placebo-controlled study of 44 patients scheduled for hip arthroplasty surgery,39 fascia iliaca compartment blocks were associated with reduced morphine consumption for up to 24 hours postoperatively. Fascia iliaca blocks may also facilitate patient positioning and improve comfort following hip fracture before surgery. In a randomized, placebo-controlled trial involving 48 patients with suspected hip fracture upon emergency room admission,47 patients randomized to a single-injection fascia iliaca compartment block with 40 mL of 1% mepivacaine reported superior analgesia at rest and with movement compared with those given 0.1 mg/kg intramuscular morphine.
Although a more traditional, paravascular approach to the femoral nerve (“3-in-1” block) has been advocated in some studies,41,49 this anterior approach commonly results in sparing of the obturator and lateral femoral cutaneous nerves.45,46 However, it seems that failure to provide adequate anesthesia with this approach is related to difficulty in controlling the final position of the indwelling catheter (if one is used). In a prospective study of 100 patients receiving a continuous paravascular nerve block, the course of the catheter could not be predicted, and only 23 catheters were documented with the use of fluoroscopy and contrast injection as placed in direct proximity to the lumbar plexus.50 In this sense, use of a stimulating catheter (a special indwelling catheter that permits continuous stimulation via the catheter and thus fine-tuning of the position of the tip) may improve the quality of the anesthetic block.51 Additional studies are needed to evaluate the clinical implications of using stimulating catheters in the perioperative management of patients undergoing hip surgery.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







