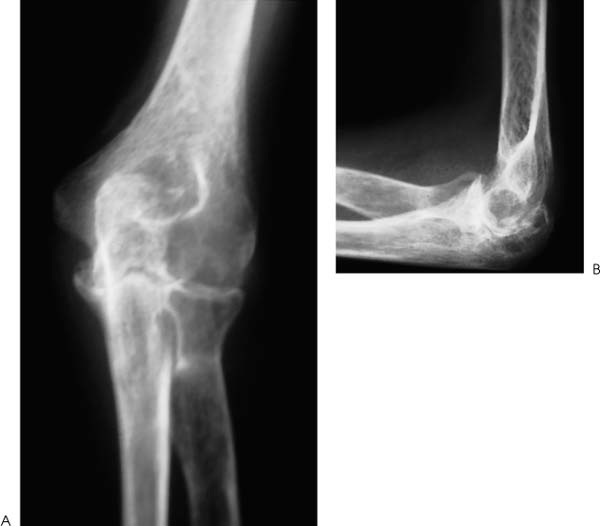
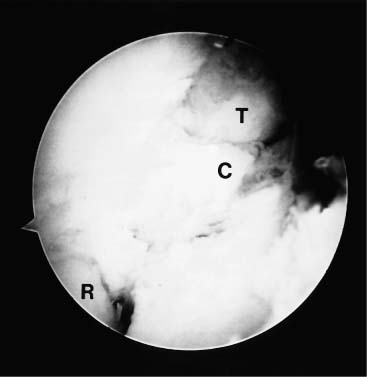
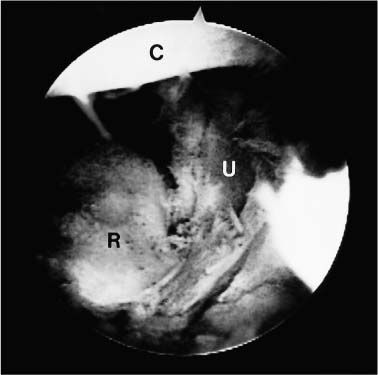
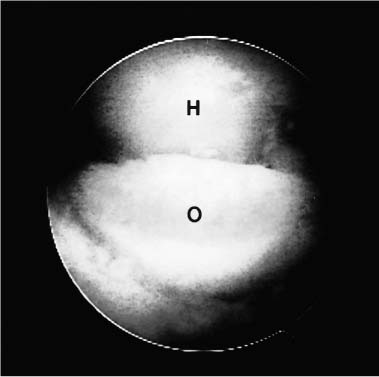
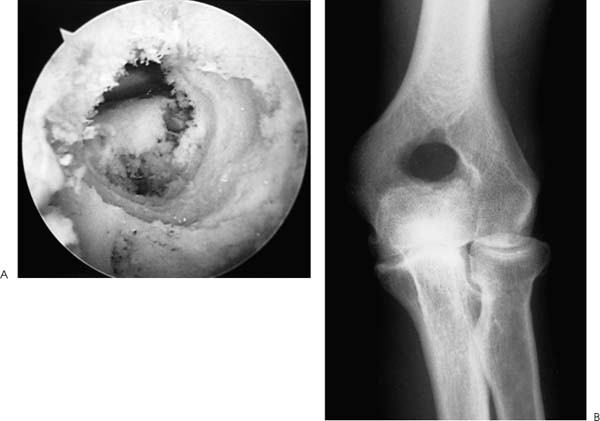
Case 50 A 65-year-old right-hand-dominant man presents with a 1-year history of progressive pain and loss of motion of his left elbow without specific predisposing factors or injury. He denies any significant locking or catching symptoms, but does report crepitation and pain with use. He also denies any significant numbness or weakness in his affected upper extremity. This patient demonstrates a range of motion of 55 to 110 degrees, with 50 degrees of both supination and pronation. His valgus and varus stability is normal, but palpable crepitation is felt through a range of motion. No significant tenderness about the elbow is found except for some mild posterolateral gutter tenderness. Also, a mild effusion is present in the posterolateral gutter. The patient is nerovascularly intact and has normal elbow and forearm strength. Figure 50–1. Anteroposterior (AP) (A) and lateral (B) radiographs demonstrate severe changes in the elbow joint with degenerative joint disease. 1. Arthrofibrosis of the elbow 2. Ulnohumeral arthritis 3. Systemic elbow arthritis Anteroposterior (AP) and lateral radiographs of the elbow are obtained (Fig. 50–1). Ulnohumeral Arthritis. Advanced degenerative arthritis of the elbow can be diagnosed based on this patient’s history and physical examination in conjunction with the classic radiographic findings of advanced degenerative arthritis. Such patients often present with an insidious onset of progressive loss of motion. Some pain is commonly present but often does not lead these patients to seek medical attention. More commonly, they present when their loss of motion becomes a significant functional impairment. This generally occurs when the extension lag exceeds 30 degrees. However, presentation based on loss of extension is variable and is highly dependent on the activity level of the patient. These patients will occasionally complain of locking and catching symptoms due to loose bodies in the elbow. Patients will sometimes improve with the initiation of an exercise program, combined with nonsteroidal antiinflammatory medications. But the disease process is usually advanced upon presentation, often making these interventions inadequate. This is particularly true when the patient not only complains of pain and loss of motion, but also has symptoms compatible with loose bodies. Management options for the arthritic elbow have been limited in the past to a medication and bracing program, open debridement, or elbow replacement surgery. Although each of these may provide significant relief, the advent of arthroscopy has introduced a new option for these patients. Encouraged by the results of open fenestration (Outerbridge-Kashiwagi, O-K) or ulnohumeral arthroplasty, the authors have developed an arthroscopic approach to debridement of these elbows. This systematic approach combines the value of synovectomy, debridement, osteophyte removal, olecranon fossa fenestration, and radial head resection when indicated, with the known advantages of arthroscopy to produce an intermediate step in the management of the arthritic elbow. The patient is placed in the prone position for elbow arthroscopy. A block or arm-holding device is placed under the arm to elevate it away from the arm board. The forearm and hand are allowed to hang free with the elbow flexed at 90 degrees. The elbow is initially entered through an anterior proximal medial portal. A proximal lateral portal is then established. Loose bodies and arthritic debris are removed, and an anterior synovectomy is performed. Osteoarthritic spurs are debrided from the coronoid process with the shaver in the lateral portal (Fig. 50–2). If a radial head excision is necessary due to radiocapitellar degeneration, the anterior aspect of the radial head is then excised while the shaver is in the lateral portal. The arthroscope is left in the proximal medial portal and the posterior soft spot portal is then utilized for instrumentation. Sweeping the shaver medially to laterally, the radial head is excised until adequate clearance is obtained in the radiohumeral interval. The proximal radioulnar joint is then assessed. If further debridement is necessary in the area, additional bone is removed from the proximal radius (Fig. 50–3). The extent of the radial head excision is evaluated by fluoroscopy periodically during this portion of the procedure. Once an adequate debridement of the anterior aspect of the elbow joint is completed, the instrumentation is switched to the posterior aspect of the elbow. Figure 50–2. In this view from the proximal medial portal the debridement of the arthritic coronoid process from the lateral portal is demonstrated. C, coronoid; T, trochlea; R, radial head. (See Color Plate 50–2.) Figure 50–3. The arthroscopic resection of the radial head is completed by placing the shaver in the straight lateral portal and planing the radial head from posterior to anterior. R, radial head; C, capitellum; U, proximal ulna. (See Color Plate 50–3.) The inflow is left anteriorly and the arthroscope is introduced through a standard posterolateral portal. The posterior central portal is then utilized for instrumentation of the olecranon fossa, which is debrided of arthritic spurs and loose bodies. The tip of the olecranon and associated spurs are excised until extension can be achieved (Fig. 50–4). The medial gutter is debrided of the synovium, taking care to keep the blunt aspect of the shaver toward the ulnar nerve and medial capsule at all times. No suction is used when debriding this area. The lateral gutter is then debrided, excising the posterolateral plica. Figure 50–4. Posteriorly, the tip of the olecranon is excised with the shaver in the straight posterior portal working from medial to lateral. Starting medially lessens the risk of ulnar nerve injury. O, olecranon; H, distal humerus. (See Color Plate 50–4.) Through the posterior central portal a 5-mm drill bit is placed in the center of the olecranon fossa. The surgeon then drills from posterior to anterior connecting the olecranon fossa with the coronoid fossa. The drill is centered in the olecranon fossa and angled toward the center of the coronoid fossa. The intersection of the long axis of the humerus with the inflow cannula in the anterior proximal medial portal provides a guide as to the proper orientation of the drill. After assessing the location and depth of this channel connecting the two fossae, a notchplasty blade is used to enlarge the hole until full flexion and extension can be achieved. While developing a concentric hole in the olecranon fossa, care must be taken not to disrupt the medial and lateral columns of the distal humerus (Fig. 50–5). Figure 50–5. Arthroscopic photograph (A) and AP radiograph (B) are arthroscopically performed ulnohumeral arthroplasty. (See Color Plate 50–5A.) At the completion of the procedure, suction drains are placed anteriorly and posteriorly. A continuous passive motion (CPM) machine is initiated in the recovery room and continued during the first 1 to 3 weeks of home care. Patients are usually discharged on the day after surgery. While at the hospital, all patients receive physical therapy instruction for home exercises. No specific functional limitations or restrictions are given, and most patients return to normal activities within 2 months postoperatively. • Use of a drill bit to initiate the arthroscopic ulnohumeral arthroplasty allows for assessment of the depth of the olecranon fossa, which can be helpful in removing an adequate amount of bone. • Advancing the anterior inflow portal so as to be visible in the depth of the crater created by progressive removal of bone in the olecranon fossa indirectly serves to protect the anterior nervascular structures by blocking the advancement of instruments into the anterior elbow joint.
History and Physical Examination
Differential Diagnosis
Radiologic Findings
Diagnosis
Surgical Management
Postoperative Management
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree