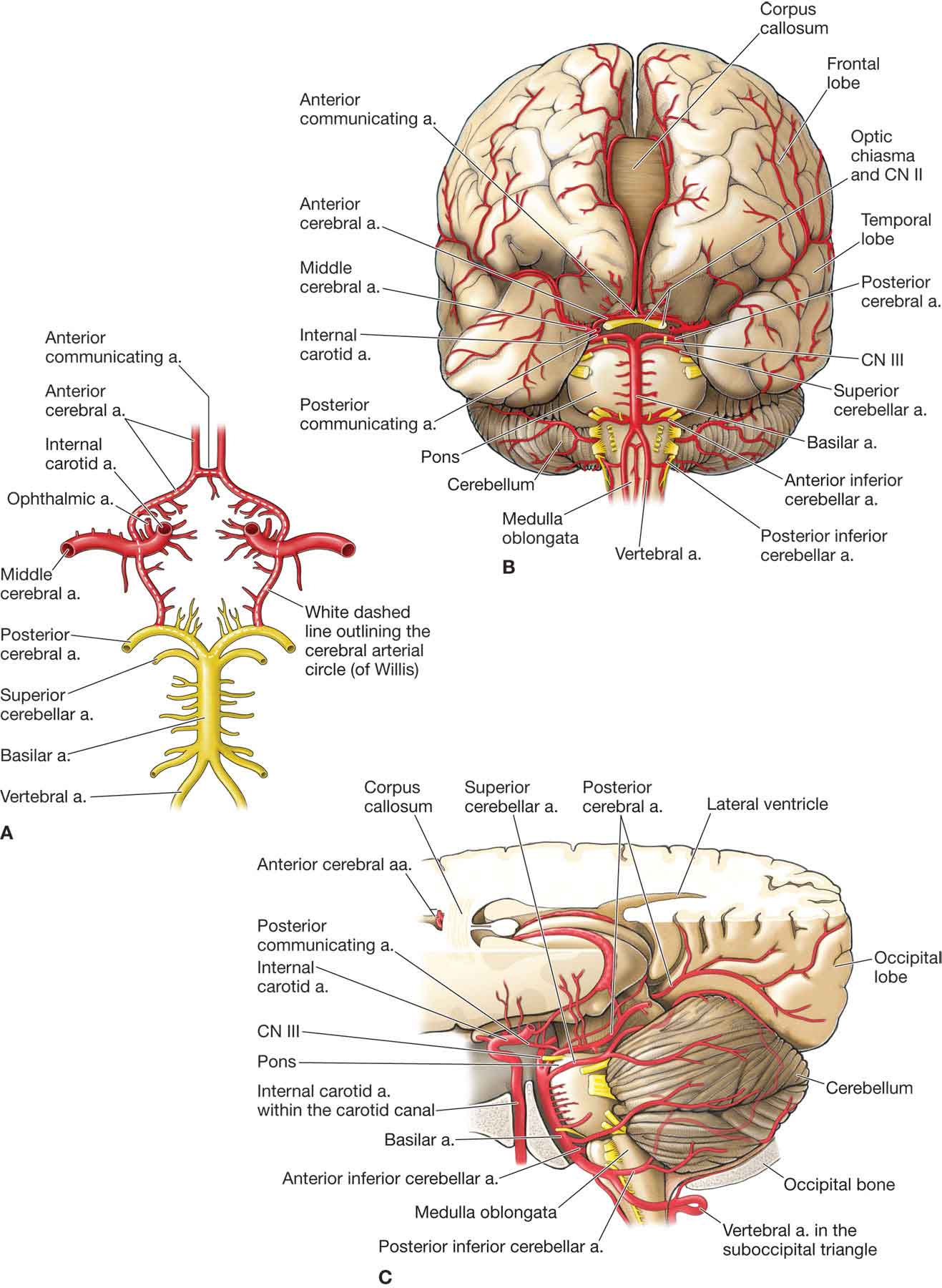
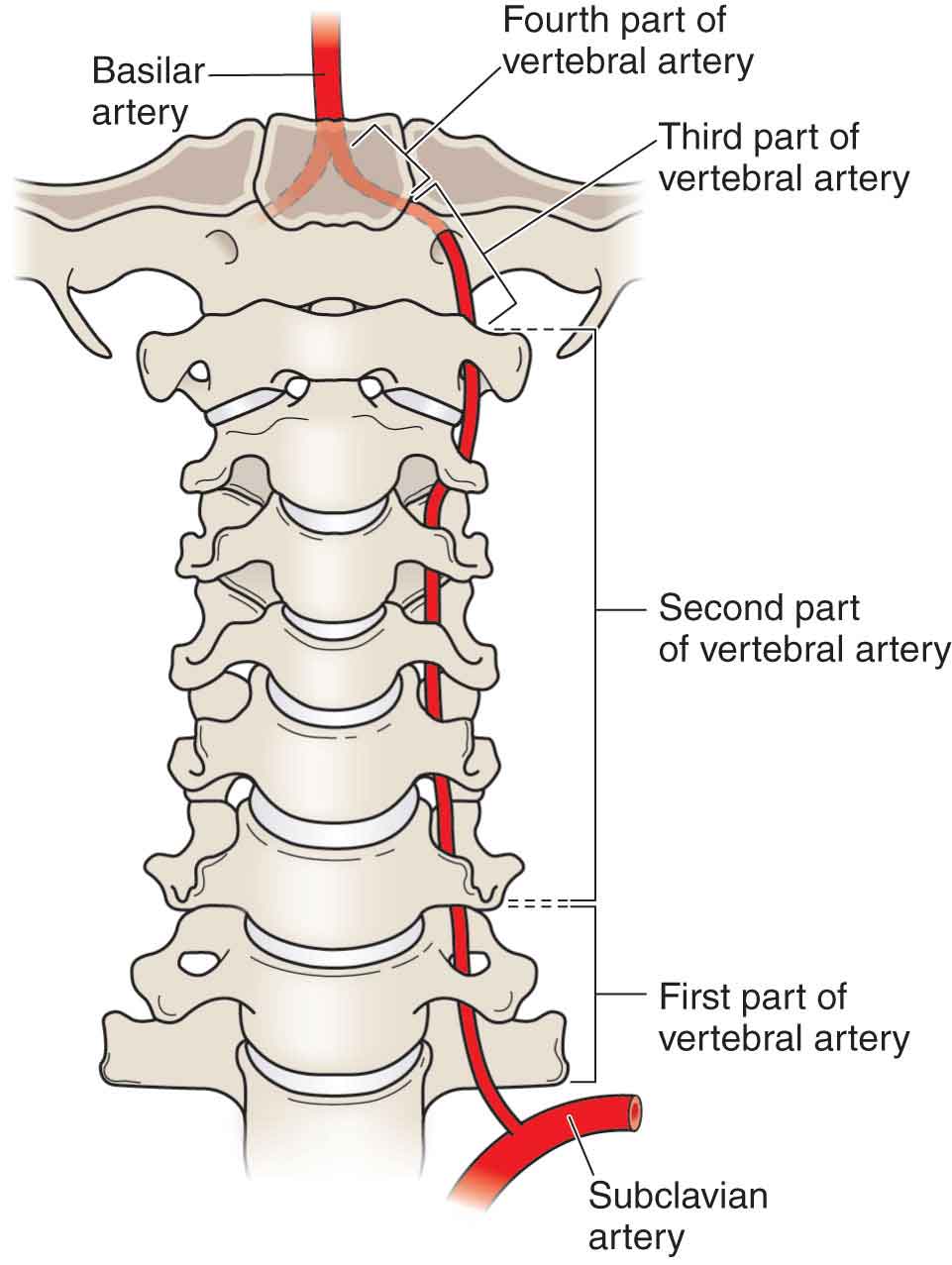
The vertebral artery (VA), a component of the vertebrobasilar artery (VBA) system, supplies 20% of the blood to the brain (primarily the posterior cranial fossa), with the remaining 80% being supplied by the carotid system.1 The first studies of the VA were recorded as far back as 1844.2 Since that time, recognition of the importance of the VA has continued to grow, and it is now discussed in more detail than any other artery by physical therapists. For this reason, the VA is afforded its own chapter. To fully comprehend its significance, a review of its anatomy and function is in order. The VBA system consists of three key vessels: two VAs and one basilar artery. The basilar artery is formed by the two VAs joining each other at the midline (Fig. 24-1). FIGURE 24-1 The vertebral artery and its relationship to the cranial arteries. (Reproduced, with permission, from Chapter 16. Brain. In: Morton DA, Foreman K, Albertine KH. eds. The Big Picture: Gross Anatomy. New York, NY: McGraw-Hill; 2011.) Along its course, the artery can be viewed as having four portions: proximal, transverse, suboccipital, and intracranial.3,4 This portion runs from the origin of the artery to its point of entry to the cervical spine. The VA usually originates from the posterior surface of the subclavian artery, but it can also originate from the aortic arch and common carotid artery.5 The VA runs vertically, slightly medial, and posteriorly lateral to the longus colli and medial to the anterior scalene muscles to reach the transverse foramen of the lower cervical spine, although its exact direction is dependent on its exact point of origin. The artery’s anomalous origin in this region has been suggested as a potential factor increasing the chance of blood flow compromise due to compression by the longus colli or scalene muscles. In approximately 88% of individuals, the artery enters the transverse foramen of C6, but it has been shown to enter as far superior as the transverse foramen of C4.6 The second portion of the VA runs from the point of entry at the spinal column to the transverse foramen of C2 (Fig. 24-2). As already described, the origin of this part of the artery is typically at the C6 level, but this may vary between individuals and even from side to side in the same individual. FIGURE 24-2 The left vertebral artery showing the four parts of its route. Throughout this section of the spinal column, the artery travels vertically in a true canal called the transverse canal (TC). The TC is formed by the bony transverse foramina at each spinal level and the overlying anterior and posterior intertransverse muscles, the scaleni, and the longus colli muscle. The dimension of the TC is proportionate to the diameter of the artery which itself is variable. Within the TC, the artery is surrounded by a periosteal sheath that is adherent to the boundaries of the canal and affords protection for the artery. However, the artery is in close proximity to the uncinate processes of each vertebral body on its medial aspect and is prone to compression from osteophyte formation or subluxation from the zygapophyseal joint.4,7 The VA in the transverse foramen is also adjacent to the anterior spinal roots. Arterial enlargement by an intramural hematoma or a dissecting aneurysm may cause radiculopathy by compressing or stretching the spinal root.8 Anomalies in this portion of the artery, which can include looping within the intervertebral foramina, can occur because of an abnormal origin of the artery from the aorta.9 The proximal and suboccipital portions of the artery are more elastic and less muscular than the transverse part.10 This variation is believed to be an adaptation to the greater mobility required in the proximal and transverse portions of the artery. This portion of the artery extends from its exit at the axis (C2) to its point of penetration into the spinal canal. This portion can be further subdivided into four parts: Although the artery is affected by cervical motion in the lower cervical region, it is affected even more between C2 and the occipital bone.14 In addition, because the transverse foramen of C1 is more lateral than that of C2, the artery must incline laterally between the two vertebrae. At this point, the artery is vulnerable to impingement from the following: This portion of the VA that runs from its penetration of the dura mater into the arachnoid space at the level of the foramen magnum to the formation of the basilar artery by the midline union of the two arteries at the lower border of the pons (Fig. 24-1). After its penetration of the cranium, the VA inclines medially toward the medulla oblongata. It courses up the front of the medulla to reach the lower border of the pons, where the artery from each side unites with its partner to form the basilar artery. A major change in the structure of the VA occurs as it becomes intracranial.4 The tunica adventitia and tunica media become thinner, and there is a gross reduction in the number of elastic fibers.10 This decrease in elasticity can result in the distortion of the VA during cervical extension and rotation.14,16,19 Intracranially, the VA first generates small meningeal branches that supply the bone and dura mater of the cerebellar fossa. It is possible that ischemia of these tissues, which occurs with VA occlusion, could be responsible for the suboccipital pain that often accompanies damage to the artery.15 Each of the vertebral arteries gives off single branches (Fig. 24-1), which fuse to form the anterior spinal artery (ASA) that descends in the median anterior fissure and is additionally supplied by anterior radicular arteries (typically two to four). While the ASA is bilaterally derived, the anterior radicular arteries may arise exclusively or predominately from one VA. This helps to explain how a unilateral insufficiency of the VA may cause bilateral spinal cord infarction. The paired posterior spinal arteries (PSAs) originate superiorly from the vertebral arteries or posterior inferior cerebellar arteries (PICAs). The PSAs are also supplied by posterior radicular arteries (usually two or three), which themselves arise exclusively or predominately from one VA, again demonstrating how a unilateral VA dissection can lead to bilateral spinal cord infarction. The PSAs supply the posterior one-fifth to one-quarter of the spinal cord including the posterior columns, the posterior (dorsal) horns, and parts of the corticospinal and spinothalamic tracts. The ASA is the exclusive arterial supply to the gray matter of the cord. The watershed area between the PSA and ASA encompasses the anterior (ventral) horns and part of the corticospinal and spinothalamic tracts. The muscular branches arise from the suboccipital part of the artery as it winds around the superior articular process of the atlas. They supply the deep suboccipital muscles and anastomose with the occipital and cervical arteries. The PICA (see Fig. 24-1) is the largest branch of the VA, usually being formed opposite to the medulla oblongata about 1 cm below the formation of the basilar artery. It supplies, either directly or indirectly, the medulla and the cerebellum and, via the PSAs, the posterior (dorsal) portion of the spinal cord. The formation of the basilar artery at the lower border of the pons marks the termination of the VA. The basilar artery runs in a fissure on the anterior surface of the pons (see Fig. 24-1). Directly and indirectly, the basilar artery supplies the pons, the visual area of the occipital lobe, the membranous labyrinth, the medulla, the temporal lobe, the posterior thalamus, and the cerebellum. Fortunately, there is an inherent redundancy in the vascular supply to the brain. The posterior and anterior vessels, and the vessels stemming from the internal carotid arteries form an anastomotic network via the circle of Willis. Thus, occlusion of the left VA may be compensated for by perfusion of the right VA, the occipital artery, the ascending and deep cervical arteries, and the internal carotid arteries.21,22 In fact, there is evidence that suggests that blood flow velocity and blood flow volume can increase in the arteries to compensate for occlusion in another vessel.23 It is worth considering that palpation of the carotid pulse would give the clinician information regarding the ability of the carotid to perform its normal function, and if the pulse appears excessively strong, this could be an indication that the carotid artery is compensating for loss of VA flow.24,25 Damage and occlusion of the VA are felt to occur because of the close proximity of the VA and the bony and ligamentous structures of the cervical spine.26 Trauma to this area may lead to thrombosis, dissection, transection, transmural hematoma, pseudoaneurysm, and spasm of the VA. VA insufficiency may also occur because of atherosclerotic involvement of the artery, sickle cell disease (see Chapter 5), rheumatoid arthritis, arterial fibroplasia, an arteriovenous fistula, and a number of congenital syndromes. Whatever the cause of VA compromise, the diagnosis requires a high index of suspicion for prompt recognition and intervention. Vertebrobasilar insufficiency (VBI) is associated with signs and symptoms of focal neurologic compromise that are of sudden onset and brief duration and relate to the specific areas that are normally supplied by the vessels. The VA is subject to occlusion from external and internal causes. Extracranial compression of the VA may cause neurologic symptoms depending on the acuteness of the occlusion or the presence of underlying pathologic conditions such as atherosclerosis, sickle cell disease, fibromuscular dysplasia, rheumatoid arthritis, or osteogenesis imperfecta. Many blood flow studies have demonstrated a reduction in blood flow in the contralateral VA during cervical rotation.27–30 Other studies, however, have found no change in blood flow.31,32 What is known is that the greatest mechanical stress affecting the contralateral artery occurs at a position of cervical rotation and extension. Furthermore, if this position is sustained, the arterial flow takes longer to return to normal.32 In addition to the C1–2 portion, the VA is vulnerable to compression in the portion that courses through the transverse foramen from C6 to C1. Because of its fixation to the spine in this segment, subluxations of one vertebral body on another may exert undue tension and traction on the artery. Positions of the cervical spine can cause compression of the VA.19,33 Rotation–extension–traction appears to be the most stressful, followed by rotation–extension, rotation alone, side flexion alone, extension alone, and then flexion.19,33,34 If the main restraint to atlantoaxial rotation, the alar ligament, is ruptured, then the degree of C1–2 rotation has been shown to increase by 30%.35 Insufficiency of the alar ligament has been shown to follow a rear-end collision in motor vehicle accidents, and it may also exist because of a congenital defect of the dens.36 Other contributing factors to the preponderance of lesions occurring at the second cervical joint level are the fixation of the periosteal sheath of the artery to the dura mater, the superficiality of the artery in this region, and the hard neural arch beneath the artery. Unilateral occlusion of the VA rarely results in a neurologic deficit because of the collateral supply through the contralateral vertebral and PICAs.40
CHAPTER 24
Vertebral Artery
OVERVIEW
ANATOMY
Proximal Portion
Transverse Portion
Suboccipital Portion
 Cervical extension at the craniovertebral joints, such as that which occurs with a forward head posture.11
Cervical extension at the craniovertebral joints, such as that which occurs with a forward head posture.11
 Excursion of the transverse mass of C1 during rotation. Approximately 50% of the cervical axial rotation occurs between C1 and C2; hence, there is a large excursion of the transverse mass of C1 with rotation. The artery is stretched during this process, and the size of the lumen can be reduced.14,16 Any reduction in the size of the lumina is more profound in the presence of arterial disease.
Excursion of the transverse mass of C1 during rotation. Approximately 50% of the cervical axial rotation occurs between C1 and C2; hence, there is a large excursion of the transverse mass of C1 with rotation. The artery is stretched during this process, and the size of the lumen can be reduced.14,16 Any reduction in the size of the lumina is more profound in the presence of arterial disease.
 The atlantoaxial membrane. Ossification of this membrane can occur.
The atlantoaxial membrane. Ossification of this membrane can occur.
Intracranial Portion
Branches
Spinal Branches8
Muscular Branches
Posterior Inferior Cerebellar Artery
Basilar Artery
Collateral Circulation
VERTEBROBASILAR INSUFFICIENCY
Occlusion
External Causes
Extracranial Compression
Musculoskeletal Key
Fastest Musculoskeletal Insight Engine
