CHAPTER 22 Triangular Fibrocartilage Débridement and Arthroscopically Assisted Ulnar Shortening
ANATOMY
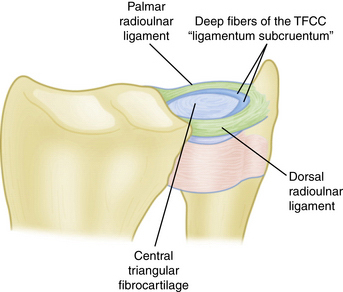
The triangular fibrocartilage is the primary stabilizer of the distal radioulnar joint. It attaches radially on the distal lip of the sigmoid notch. Ulnarly, the triangular fibrocartilage inserts at the base of the ulnar styloid by means of a continuation of the dorsal and palmar radioulnar ligaments and the fibers of the ligamentum subcruentum (Fig. 22-1).1,2
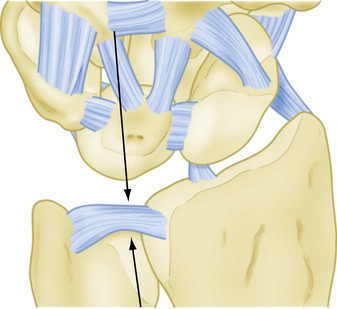
A patient with an ulnar abutment syndrome typically presents with a central tear of the TFCC. Chondromalacia can be seen at the ulnar aspect of the lunate and the distal radial surface of the ulnar head. Ulnocarpal synovitis is usually present (Fig. 22-2).
PATIENT EVALUATION
History
Tears of the triangular fibrocartilage are typically the result of a fall on the outstretched upper extremity. The ulna is driven distally and compresses the TFCC between itself and the lunate, producing a central or radial tear of the articular disk. This same mechanism can result in lunatotriquetral tears and peripheral TFCC tears, neither of which is discussed further here.
An ulnar abutment syndrome can develop as a result of settling of a distal radial fracture fragment. The radial collapse leads to a relative lengthening of the ulna. Palmer and colleagues2 demonstrated an increase in the ulnocarpal load with increasing ulnar variance.
Physical Examination
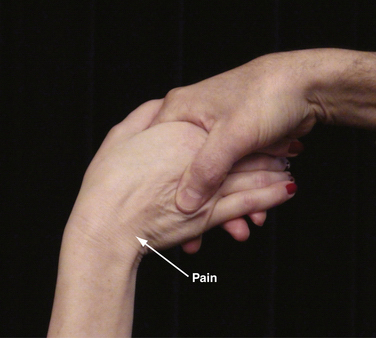
The ulnocarpal compression test (Fig. 22-3) is particularly helpful in assessing the patient with a suspected ulnar abutment syndrome. In this test, the patient sits in front of the examiner with the wrist in supination. The wrist is simultaneously ulnarly deviated and axially loaded while the forearm is supinated and pronated. The patient with an ulnar abutment syndrome experiences pain at the ulnocarpal joint, with or without popping and grinding, during this maneuver.
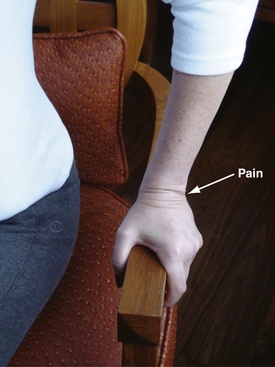
A variation of the ulnocarpal compression test is the Lester press test (Fig. 22-4).3 In this test, the patient sits in a chair with sturdy arms and lifts himself or herself off the chair seat. Pain at the ulnocarpal joint is considered pathognomonic for a TFCC tear.
Diagnostic Imaging
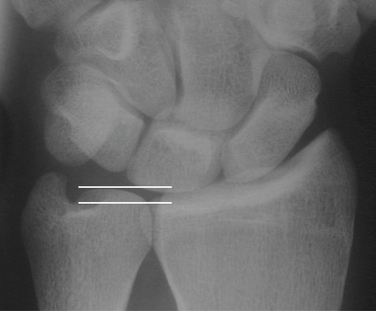
The radiographic evaluation of a patient with an ulnar abutment should include a standard wrist series and a Palmer 90 × 90 view (Fig. 22-5). The Palmer 90 × 90 view places the forearm in neutral rotation while the elbow is flexed to 90 degrees and the shoulder is abducted to 90 degrees.4 The ulnar variance is calculated from this view. An ulnar abutment can be suspected in a patient with an ulnar-zero or ulnar-minus variance. The ulnar aspect of the lunate should be carefully examined for subchondral cysts.
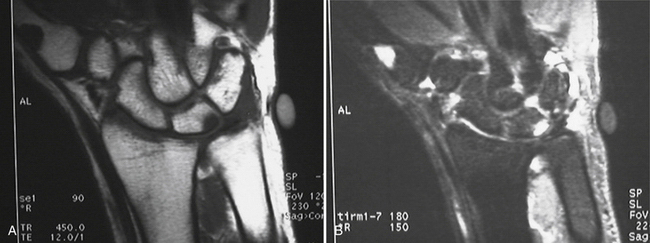
Magnetic resonance imaging (MRI) should be considered when evaluating the patient for ulnar abutment. MRI demonstrates increased signal in the lunate on T2 images (Fig. 22-6), corresponding to a cyst or intraosseous edema. The triangular fibrocartilage can also be evaluated on the MRI images. Whether a magnetic resonance (MR) arthrogram is needed is a function of the MR resolution. The accuracy of lower-resolution MR is increased with the addition of an intra-articular gadolinium injection.