Fig. 8.1
Long-line operation
Terrestrial rescue teams usually work in poor weather conditions and at night or when the air-bound intervention teams need technical assistance. During rescue operations medical rescue personnel is frequently facing a hostile environment with cold, wet, windy, and low visibility conditions. In addition, the patient’s condition can already deteriorate by delayed arrival time.
These circumstances complicate the initial assessment and diagnosis and limit medical treatment and outcome. Terrestrial rescue operations require extended activation time, high physical exertion, and environmental hazards during access to the site of the accident and prolonged evacuation time (Fig. 8.2).


Fig. 8.2
Terrestrial transport at night
Medical and technical management must be adapted to the conditions in order not to increase risk to the patient and the rescue team and to improve outcome. Monitoring may be restricted or not possible because devices are not always available and sometimes the weather conditions (freezing monitors), darkness, or certain injuries of the patient, for example, hypothermia, set limits for a continuous monitoring. All injured and sick persons in the mountains are considered hypothermic until the contrary is proved [3]. Further drop of body temperature should be avoided and assessment and treatment should avoid unnecessary undressing and provide proper insulation as soon as possible [4]. Physicians working in the mountains or mountainous environment must be comfortable in exposed situations, conscious of their own and the patient’s safety, and being able to work under extreme conditions. Technical mountain knowledge and experience as well as theoretical and practical skill of climbing in steep terrain in summer and winter conditions are mandatory. Training for doctors must basically include the same technical skills like self-belaying and other rescue maneuvers, transport and management of avalanche victims, canyoning rescues, and other specific emergencies like regular training for all rescuers. Physicians as part of a helicopter crew frequently may be supported by a single (air) rescuer. Thus they must be trained in performing long-line or winch operations without the support of a team. In case of bad weather conditions, the physician must be able to move safely and descend by himself when necessary [5, 6] (Fig. 8.3).


Fig. 8.3
Long-line evacuation of patient
Overall he should consider and accept that medical treatment may be limited and injuries usually survived in urban areas may lead to death in this setting. Despite intensive training, alpine emergency physicians constantly face the situation that mountain rescue personnel does not show the same high level of medical education as in urban emergency medical system, where usually professional staff provides emergency medical assistance [7]. In an urban setting different tasks are performed by professional health-care providers. In mountain rescue operations, emergency physicians must perform usually delegated measures by themselves. Nevertheless, they should not lose track of the overall situation and adapt medical care to the specific situation of the mission. Unnecessary and excessive medical measure (“stay and play”) may delay the entire rescue operation unnecessarily and expose the patient and all team members to additional danger. In rescue operations risk assessment and management is one of the main tasks of the team leader. However, the emergency physician must adjust his actions to the situation and include the objective risk into his considerations. Emergency physician working in the mountains must adapt medical measures to existing human and technical resources. Optimized therapy should have priority over maximized treatment causing delay. Rapid evacuation may be an effective form of treatment. Every therapy, once begun, must be carried out until the patient is handed over to the following team. Adequate supply of medical or technical equipment, drugs, and oxygen is either not possible in reasonable time or might delay the entire rescue operation. Often the entire recovery cannot be brought later to the scene without delaying. In addition changing environmental factors and/or the patient’s condition may force the emergency physician to employ alternative medical strategies or evacuation procedures in cooperation with the team leader. In extreme weather situations, it may be appropriate to stay with a medically stable patient in a safe place (hut or bivouac), until the situation allows terrestrial or air-bound evacuation. In mountain rescue the emergency physician is frequently not the first on the scene either because no doctor was available from the beginning or the first message about the severity of the injury or illness was not correct. In this situation the key question arises: can the patient be treated by first responders sufficiently and transported to the doctor? Or must the emergency physician ascend to the location of the accident? Assessment of symptoms and signs of injury severity can be performed by trained rescuers who act as first responders, and initial steps of treatment can be prioritized by radio or mobile phone. Evacuation time may be shortened, hazards reduced, and medical treatment will start earlier. Increasing numbers of mountaineers seek recreation in mountain regions where the existing rescue resources are far less and the problems much greater than in the situations as described above. Commonly rescuers reach the scene of the accident hours or days later, apart from the fact whether there are any technical and medical options for professional mountain rescue. Expedition medicine in high altitudes or in very remote mountainous areas is beyond the scope of this disquisition.
8.2 Assessment of Victims in the Mountains
In any emergency situation in the mountains, rescuers must first ensure their own safety. Then they must evaluate whether the person is in a safe position and protect him from further injury. Objective risks such as rockfall, avalanches, lightnings, etc., must be kept to a minimum. In dangerous situations it is justified to evacuate the person before assessment and treatment.
Blunt traumas caused by falls are most common in accidents in the mountains. They might affect all parts of the body and result often in combined or multiple trauma with hypovolemic shock and traumatic brain injury. The mechanism of injury gives information about the expected injury pattern and severity. High-impact mechanisms (falls from more than 3 m height) are likely to cause multiple trauma and internal injuries. The mechanism of injury of falls in the mountains is markedly different from falls in urban areas. Falls in mountainous terrain may include periods of free fall interrupted by periods of sliding and falling. The landing surface in the mountains is generally not horizontal in comparison to usually flat surface in urban falls. Impact forces may be reduced substantially by steep slopes or snow. Several impacts and different body positions may occur during the fall. Injuries may be caused by deceleration (resulting from tissue displacement following the sudden arrest of motion during impact) or direct impact-associated injuries [8]. Assessment should follow standardized algorithms and all findings should be recorded. Hypothermia is a severe risk and leads to poor outcome in severe trauma and must not be overlooked [9]. The patient should be monitored continuously, depending on the skills of rescuers and the availability of equipment. In extreme cold situations, monitoring systems may fail due to rapid loss of battery capacity and freezing displays. Every new team, which assumes care of a patient, must perform their own reassessment and must transfer information from earlier teams to following teams until the patient arrives at the hospital.
8.3 Hypothermia
Hypothermia is commonly assessed by clinical findings [10] (Table 8.1).
Swiss staging of hypothermia | ||
|---|---|---|
HT I | Clear consciousness with shivering | 35–32 (°C) |
HT II | Impaired consciousness without shivering | 32–28 |
HT III | Unconsciousness | 28–24 |
HT IV | Apparent death | 24–15 |
HT V | Death due to irreversible hypothermia | <15 (9?) |
Patients should be considered to be hypothermic if they have been exposed to the cold and if they have a cold trunk and a body core temperature <35 °C (95 °F). Hypothermia can be diagnosed clinically by assessment of vital signs using the Swiss staging system. Temperature measurement in intubated patients in the preclinical setting should be measured by insertion of a probe in the lower third of the esophagus. Thermistor probes inserted in the ear canal for epitympanic measurement require a free ear canal without snow or cerumen. Infrared cutaneous, aural, and oral measurements are often inaccurate. It is of great importance to assess every hypothermic patient without vital signs, whether cardiac arrest occurred prior to hypothermia (postmortem cooling) or cardiac arrest is caused by hypothermia. At low temperatures the brain tolerates cardiocirculatory arrest much longer without permanent damage than in normal core temperature. Prehospital treatment of hypothermia should focus on careful handling, basic life support (BLS) or advanced life support (ALS), and external rewarming. Detecting a pulse or breathing in a patient with deep hypothermia may be difficult and should be performed over 1 minute. Every sign of life, like breathing movements, should prompt a watchful waiting and careful transport. In the absence of vital signs, cardiopulmonary resuscitation (CPR) should be started. Full body insulation with chemical heat packs provides a substantial amount of heat to prevent further heat loss. Conscious, shivering patients can be treated in the field. Patients with impaired consciousness but stable circulation require active external rewarming (blankets, forced air heating, or chemical or electrical heat packs) at the closest hospital. Patients with cardiac instability or cardiac arrest should be transported, favorable with helicopter, to a center with the ability of extra-corporal rewarming either with ECMO or cardiopulmonary bypass [3, 10, 11].
8.4 Lightning
In a continuing thunderstorm, evacuation of a victim might be postponed if there is a high risk for rescuers. If rescuers decide to perform a rescue operation, the victim should be moved as fast as possible to an area of lower risk. A person hit by a direct lightning strike in the open is dead in many cases. However, the most common cause of death is cardiorespiratory arrest produced by ventricular fibrillation or asystole caused by current splash either from an object nearby (e.g., tree), a contact with an object hit by a lightning (e.g., fixtures of a via ferrata), or a ground current. Blunt trauma may be caused by a shock wave and consecutive falls by loosing balance during climbing. Respiratory arrest may be prolonged (due to paralysis of the medullary respiratory center) and lead to secondary cardiac arrest from hypoxia. Spontaneous return of cardiac activity is the rule in this case if the patient’s ventilation is maintained and severe hypoxia does not occur. In case of more than one victim hit by a lightning, the normal triage rules for trauma patients do not apply to non-breathing victims. In triage situations with trauma casualties, victims with vital signs are given priority for emergency treatment rather than patients in cardiorespiratory arrest. The rule in lightning strikes is to “resuscitate the apparently dead first” [12].
8.5 Trauma Management in Mountain Rescue Operations
Traumatic injuries are most common in mountain accidents. Approximately 10 % suffer from major trauma with traumatic brain injury (TBI) often in combination with injuries of the trunk, vertebral spine, pelvis, and extremities [8, 13]. Emergency physicians must consider the mechanism of injury to correctly assess pattern and severity of injuries, provide sufficient analgesia, stabilize circulation by control of external bleeding and adapted fluid resuscitation, and organize safe evacuation under constant surveillance and monitoring of the patient. Early pain treatment is not only for the comfort of the patient but allows repositioning of fractures and dislocations, reduces secondary damage to soft tissues, reduces bleeding, and is the first step of circulatory stabilization. Environmental conditions as well as psychological factors, comorbidities and time affect pain. Using a pain score, such as verbal numerical rating, can be helpful. Insufficient treatment of pain not only reduces outcome but also increases the development of post-traumatic stress disorder. Pervading culture and knowledge of health-care providers determine the provision of prehospital analgesia [14]. No analgesic drug will accomplish all expected effects in every situation. Non-pharmacological methods such as splinting and positioning should be taken in consideration especially by nonmedical personnel without the possibility of pharmacological pain treatment [15] (Fig. 8.4).


Fig. 8.4
Rescue of injured patient in steep rock
The number of drugs carried should be reduced to a minimum and tailored to the expected injuries and skills of the health-care provider. All persons administering analgesics should receive appropriate detailed training. Health-care providers should be familiar with the effects of all administered drugs and should be able to manage adverse effects. Sufficient pain relief might be constrained by national laws in countries where health-care professionals do not routinely attend the site of accident and nonprofessionals are not allowed to administer drugs [16]. An intravenous access should be established rapidly, and depending on pain assessment, a potent painkiller should be administered. If intravenous administration is not possible, other parenteral routes such as intraosseous and intramuscular routes may be utilized. Intranasal and buccal administration of opioids, ketamine, and sedative drugs is recommended in situations where no i.v. line can be established [17, 18]. Loco-regional anesthesia offers another way of excellent analgesia. It also may permit patient contribution during difficult and long evacuation or in high-altitude rescue [19, 20]. A combination of analgesic drugs is frequently used but a higher rate of side effects must be expected. Severe adverse effects such as respiratory depression, nausea, and vomiting can become hazardous during evacuation, especially in austere environment. Rescue population becomes older and comorbidities more common. Therefore, analgesia should be individualized to each casualty, and preexisting drug use must be taken into consideration. Hypothermia alters the pharmacokinetics and pharmacodynamics of fentanyl, morphine, ketamine, and midazolam; especially the side effects of ketamine to an irritable hypothermic heart may be harmful [21]. Opioids remain the gold standard for pain management in acute trauma. Hypotension caused by significant blood loss may be limited by reduced initial dose given over a longer period of time [22] (Fig. 8.5).
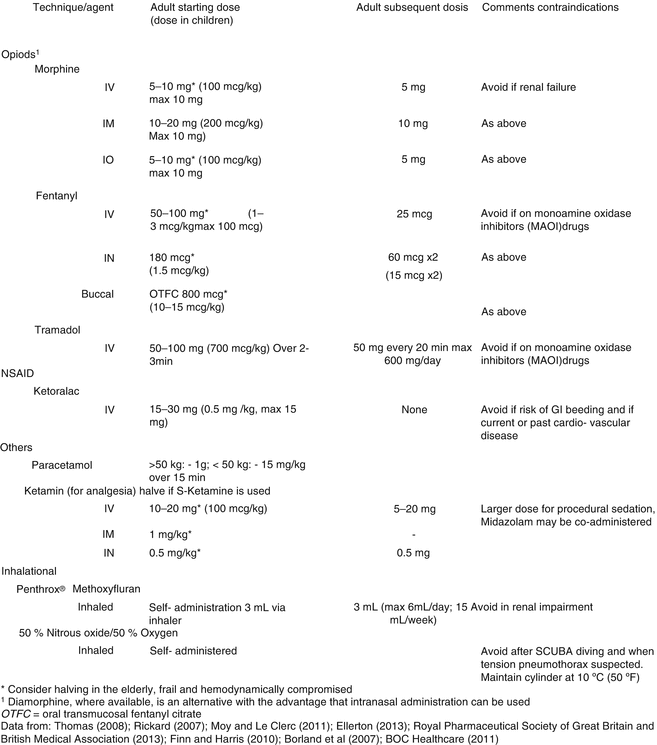

Fig. 8.5
Recommended pharmacological agents for treating moderate or severe pain in mountain rescue [21]
Injuries with severe bleeding, traumatic brain injury (TBI), and multiple trauma require an individualized strategy for each patient. Traumatic shock during terrestrial mountain rescue operation, especially in uncontrolled bleeding and/or TBI, has a poor outcome. Aggressive fluid management in all cases failed to improve survival in most studies [25–27]. Two decisive key conditions must be recognized in suspected major or multiple trauma: severe uncontrolled hemorrhage or presence of traumatic brain injury. Accurate diagnosing could be difficult as symptoms could be masked in the prehospital setting. Rapid deterioration or only transient responding circulatory parameters under initial fluid resuscitation could be caused by pressure-depending hemorrhage. Increasing impaired consciousness may be caused by traumatic brain injury but also by arterial hypotension, hypoxemia, cardiac dysfunction, and hypothermia. Mechanism of injury (e.g., high-velocity trauma) and/or external signs of head injury, anisocoria, and a Glasgow Coma Scale (GCS) below 9 are strong indicators for TBI (Fig. 8.6).


Fig. 8.6
Terrestrial rescue at night
Terrestrial mountain rescue operations in patients with multiple trauma and shock are often characterized by prolonged evacuation time and hostile environment. Reduced diagnostic and monitoring facilities, limited oxygen fluids, and drugs make any medical intervention difficult. Different strategies of prehospital fluid resuscitation are practiced in different regions worldwide, and none of these concepts support them beyond any scientific doubt. Systolic arterial blood pressure (SABP) ≤90 mmHg in trauma may decrease outcome. But in uncontrolled severe hemorrhage (e.g., liver, spleen, and kidney lacerations or ruptured vessels), aggressive fluid resuscitation may increase bleeding and does not show any increase in outcome [27]. Withholding fluid (“delayed resuscitation”) or limiting fluids with aimed blood pressure to just maintain consciousness and/or palpable central pulse (indicating an SABP above 60 mmHg) (“permissive hypotension”) may be a better option for patients in traumatic shock even in prolonged evacuation [28].
In these cases rapid evacuation and transport in combination with sufficient analgesia are the key to improve outcome, and medical interventions should follow the principle: “Load and Go.” Rapid transport may be considered as one form of treatment [29].
If traumatic brain injury or a spinal lesion is suspected, the main goal for prehospital treatment is SABP higher than 110 mmHg in order to ensure adequate perfusion of the central nervous system (Fig. 8.7). Rapid elevation of blood pressure can be achieved by administration of hypertonic solutions followed by isotonic fluids. Catecholamine may be advantageous. After establishing intravenous or intraosseous access airway protection by endotracheal intubation or laryngeal tubes, high flow of oxygen (if available) should follow. Sufficient analgesia is mandatory as it may reduce sympathetic stimulation and hasten evacuation. During transport frequent reassessment of reestablishment of breathing (e.g., deflating a tension pneumothorax) and circulation must take place, and an alternative strategy of fluid resuscitation may be considered. Besides fluid administration control of blood loss by wound management, repositioning, and splinting and prevention of hypothermia is essential [30, 31]. Hypothermic patients in traumatic shock and cerebrospinal injury are prone to hypothermia due to destabilized thermoregulation. Hypothermia increases bleeding by reduced platelet function and consecutive critical coagulopathy below 34 °C with reduced outcome [9, 32].
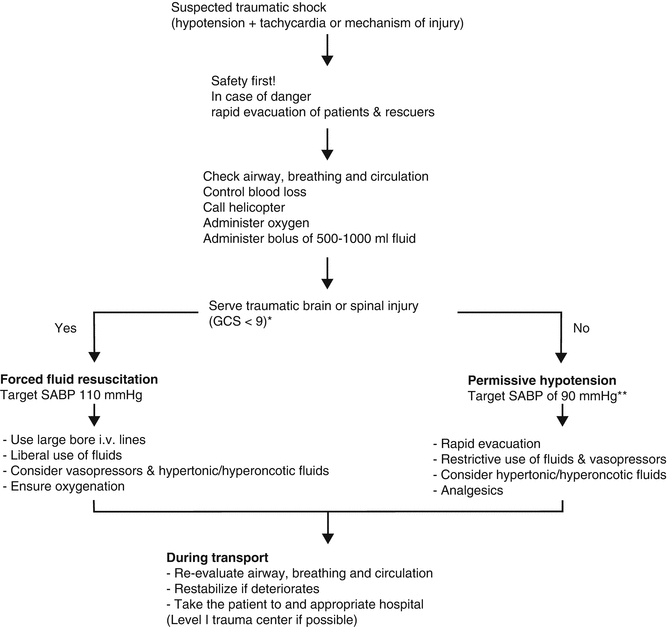

Fig. 8.7
Fluid management in traumatic shock. A protocol for the prehospital management of patients in traumatic shock with or without brain or spinal injury in mountainous terrain and remote areas. Impairment of consciousness does not necessarily indicate severe TBI in a shock patient; hypoxia, tension pneumothorax, cardiac dysfunction, and hypothermia should be excluded. If uncontrolled hemorrhage is suspected, lower values maintaining consciousness and/or palpable central pulses may be reasonable. GCS Glasgow Coma Scale, SABP systolic arterial blood pressure [23, 24]
All patients should be transported to an appropriate trauma center without delay if possible with helicopters [33]. Multiple trauma in combination with TBI in the mountains or remote areas shows poor outcome when compared to urban areas, and urban traumatic shock protocols may not apply in all situations.
8.5.1 Prehospital Treatment of Avalanche Victims
Approximately 150 people die on avalanches per year in Europe and North America [34]. In less developed countries, fatalities are presumed to be many times higher. If a person is caught by an avalanche, four factors are decisive for survival: grade of burial, duration of burial, presence of an air pocket and a free airway, and severity of trauma. The overall mortality is 23 % but in completely buried victims (head below snow) it is 52 % and only 4 % if the head is not covered. In completely buried victims, survival drops from 80 % after the first 20 min to 30 % at 35 min. Initial mortality is mainly caused by trauma, whereas the steep decline between 20 and 35 min is due to asphyxia. After this period, survival is decreasing slower depending on trauma and the possibility to breathe under the snow. Limiting factors in this period are hypoxia, hypercapnia, and hypothermia [35]. Decline of survival seems to be affected by snow density resulting in lower survival rate in Canada compared to Swiss findings representing the situation in the Alps [36] (Figs. 8.8 and 8.9).
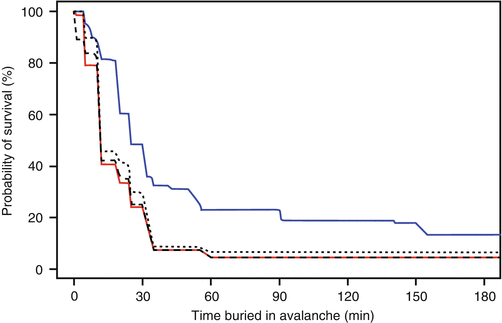

Fig. 8.8




Avalanche Survival Curve. Comparison of survival curves: Swiss survival curve (blue; n = 946) and Canadian survival curve (red; n = 301). The black dotted survival curve is based on the Canadian dataset without trauma fatalities (n = 255). The black dashed survival curve is calculated with the Canadian dataset where the extraction times for severe trauma fatalities was replaced with an estimated time of death of 1 minute after burial (n = 301) (From: Haegeli et al. [36])
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








