Fig. 5.1
High-altitude retinopathy. This fundus photograph shows the retina of a high-altitude climber at 6870 m, who participated in the Muztagh Ata study in 2005. Shown are (A) peripapillary hemorrhages, (B, C) retinal hemorrhages at the temporal retinal vessels, (D) a white-centered hemorrhage (Roth spot) within the macular region, and (A) early signs of optic disk swelling (Schnetzler et al. 2006)
Signs of high-altitude retinopathy (HAR) include retinal hemorrhages (HARH), engorgement and tortuosity of retinal vessels, optic disk hyperemia and swelling, cotton wool spots, and even vitreous hemorrhage [15, 17, 21–23]. Both central retinal vein occlusion [24] and branch retinal vein occlusion with macular edema [19] inducing loss of visual acuity have been reported in association with altitude retinopathy. A subset of climbers show white-centered hemorrhages [17, 25], also known as Roth spots [26]. This specific type of bleeding observed at sea level occurs in patients with capillary fragility due to systemic infections, hypertension, diabetes [27], anemia, and leukemia [28]. High-altitude climbers with Roth spots often present with larger retinal hemorrhages compared to climbers without white-centered hemorrhages [16]. As mentioned earlier, retinal hemorrhages during high-altitude trekking are usually not symptomatic. However, depending on the location of the hemorrhage, there is a rare possibility that visual acuity will be markedly impaired, such as in foveal bleeding, especially if bilateral. If the latter occurs, aided descent would be necessary, as reabsorption of the blood may take days to weeks, depending on the severity of the hemorrhage.
Treatment
Similar to retinal hemorrhages occurring at sea level for different reasons, high-altitude retinal hemorrhages usually disappear within days or a few weeks without sequelae. Thus, the usual treatment protocol is to watch and wait for their resolution. Other HAR entities such as vein occlusions also require follow-up and may eventually need specific ophthalmic treatment.
Prevention
Adequate acclimatization will help to defer altitude illness. To date, no medication has been reported as successful in preventing retinal hemorrhages. Since HARH are of transient nature, there is no good evidence to discourage climbers who have experienced prior symptomatic retinal hemorrhages from going back to high altitude. If visual disturbances, which have occurred during a sojourn to high altitudes, do not resolve within a week, the climber should consult an ophthalmologist within maximally another week. Since there is no clear evidence that retinal hemorrhages are warning signs of impending severe acute mountain sickness or even high-altitude cerebral edema, continuation of the expedition can be ventured—under the premise that the climber is never alone during the further sojourn at high altitudes and only if visual disturbances due to retinal bleeding are minimal and do not impede the safety of the climb [29].
5.2.2.2 Optic Disk Swelling
Optic disk swelling (Fig. 5.2) has been reported to occur in up to 79 % of mountaineers at altitudes of 4560 m [20] and in up to at least 59 % of mountaineers at altitudes of 6800 m above sea level, increasing in incidence with ascent to higher altitudes and regressing quickly upon descent [30]. A correlation with low peripheral oxygen saturation and symptoms of acute mountain sickness has been reported in 27 climbers, concluding that optic disk swelling is most likely the result of hypoxia-induced brain volume increase [30]. This has been debated by Willman et al. [20], who did not find a correlation between optic disk swelling and symptoms of acute mountain sickness in 18 mountaineers. A possible explanation for this discrepancy is the different ascent profiles (rapid vs. slow) and the different heights reached in the two studies (4559 m and 6800 m).
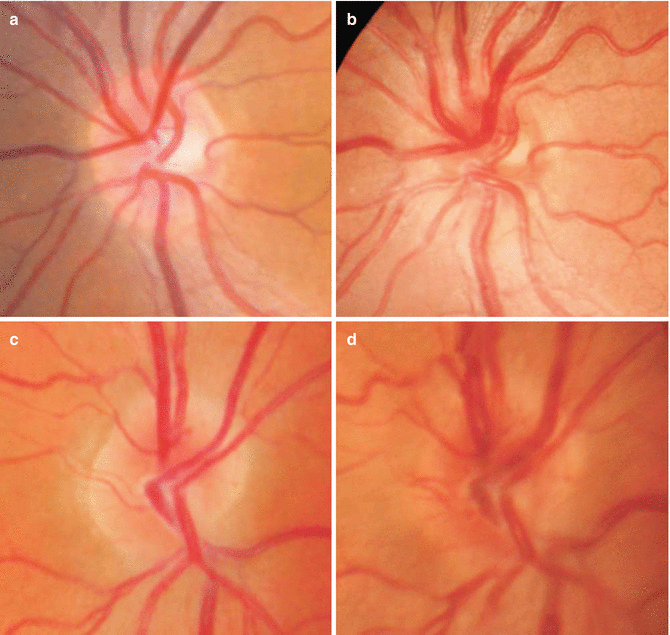

Fig. 5.2
Optic disk swelling. The left optic disk of climber 9 (group 1) appears normal at baseline examination (490 m), 1 month before the expedition (a), and swollen at camp 2 (6265 m) (b). Similar changes are seen in the right optic disk of climber 5 (group 2) at baseline examination, 1 month before the expedition (c), and at camp 3 (6865 m) (d)
Treatment
Since quick regression of optic disk swelling is seen upon descent and no lasting sequelae have been reported up till now, the mainstay of treatment is similar to further altitude illness entities where descending to lower altitudes is necessary. This option should be considered if symptoms and signs of AMS or HACE are detected.
Prevention
As for HAR, prudent selection of adequate climbing profiles with necessary acclimatization is certainly beneficial to the climber’s well-being during high-altitude sojourns.
5.3 Trekking-Related Ultraviolet Exposure
5.3.1 Acute Irradiation
5.3.1.1 Photokeratitis/Ultraviolet Keratitis
The cornea absorbs most ultraviolet radiation, which can cumulatively damage the corneal epithelium, the outermost layer of the cornea. Unprotected exposure to sun rays at high altitudes, often on highly reflective snow fields, most often leads to direct corneal epithelial injury, also known as “snow blindness.” The keratitis-effective irradiance seems to depend on altitude, characteristics of the ozone layer, and the reflectivity of the earth’s surface at time of exposure [31].
This ultraviolet keratitis is a self-limited inflammatory disorder of the cornea. Symptoms include excruciating pain, decreased visual acuity, foreign body sensation, burning, and tearing with a red eye. These symptoms commence about 6–12 h after extensive exposure to UV rays and will typically resolve within 72 h [32]. Clinically, a superficial punctate keratitis, usually bilateral, develops primarily. The more severe the case, the greater the damage sustained to cell adhesion, leading to epithelial defects which can progress to total abrasion of the corneal epithelium. Epiphora, conjunctival chemosis, and blepharospasm, impeding a thorough ophthalmic examination, usually also occur.
Treatment
To our knowledge, no prospective studies have reported on the treatment of photokeratitis. Common treatment modalities include topical anti-inflammatory drugs, cycloplegics, preservative-free lubricants, bandage contact lenses, and systemic analgesics. Long-term damage to the cornea is rare [31].
Prevention
The mainstay of handling snow blindness is prevention by wearing sunglasses which provide adequate protection, preferably with side shields, if at risk of exposure to UV rays.
5.3.2 Chronic Irradiation
Pinguecula, pterygia, cataract, age-related macular degeneration, and ocular surface squamous cell neoplasia/carcinoma are discussed in the paragraph on surfing.
Climatic droplet keratopathy, also known as spheroidal degeneration or Labrador keratopathy, has been strongly linked to actinic damage. The anterior cornea or conjunctiva is primarily affected. Slit-lamp examination shows a range from fine, subepithelial opacities without an effect on visual acuity, to axial corneal scarring and strongly decreased visual acuity [33].
5.4 Surfing
Surfboard riding, known as surfing, is an increasingly popular extreme water sport. Surfing is a complex activity as it relies on a surfer’s tactical, cognitive, psychological, technical, biomechanical, and physiological abilities [34].
Surfing originated centuries ago in the South Pacific where it was a central part of Polynesian and then Hawaiian culture. Joseph Banks is thought to have first described surfing in 1779 while on the HMS Endeavour during Captain James Cook’s third voyage (http://www.surfingforlife.com/history.html). Modern surfing as a sport, hobby, and recreation emerged in the early twentieth century. Since then, it has increased in popularity, with the number of surfers increasing each year [35], and it is currently practiced in many countries throughout the world. The International Surfing Association has estimated that there are around 23 million surfers worldwide (http://www.statisticbrain.com/surfing-statistics/).
A variety of surfboard designs exist; however, all surfboards have a pointed nose (tip), tail (back end), one to three fins, and an ankle leash. The board design used by each surfer will depend on their experience and wave conditions. “Shortboards” (around 1.83–2.13 m (6–7 feet) long) are typically preferred by experienced surfers as they are easy to maneuver, particularly in large waves, whereas “longboards” (2.44–3.04 m (8–10 feet) long) provide better stability and are therefore preferred by beginners and in smaller waves [36]. The surfboard is typically attached to the surfer’s ankle via an elasticized cord known as the “leash,” keeping the board with the surfer after a fall. The leash is typically 7–8 feet (2.1–2.4 m) long but can stretch to twice its length. The length of the leash is generally proportional to the length of the board. To prevent the surfer from slipping, the board is either rubbed with sticky wax or has nonskid pads [37].
Acute and chronic conditions have been associated with surfing in both adults [35] and children [38]. Acute trauma is most common, with lacerations, contusions, sprains, and fractures reported [35, 36], including injuries to the eye and orbit [39]. Environmental exposure, such as to ultraviolet light and salt water, is mainly responsible for chronic conditions [35]. Acutely painful ultraviolet keratitis can also affect the surfer.
5.5 Surfing-Related Ocular Trauma
Surfing-related ocular trauma can impact both the eye and the orbit. It is thought to occur infrequently but has the potential for significant morbidity. Of all eye trauma, sports-related injuries form a small proportion but have a significant morbidity [40]. The head and neck are common sites for surfing-related trauma, though fortunately major ocular or orbital trauma are infrequent [41, 42].
5.5.1 Epidemiology
There is limited data available on the worldwide epidemiology of surfing-related injuries [37]. Most studies conducted have included small numbers of patients and have been limited to a set geographical location [37]. In a cross-sectional survey of surfers at 8 Victorian beaches in Australia over 12 months, with 646 surfers enrolled (90 % male; median age, 27 years; median years surfing, 10), 145 surfers reported a significant acute injury in the 12 months prior to the survey in 2003 (0.26 injuries/surfer/year) [43]. A study of 346 surfers in Victoria published in 1983 reported an injury rate of 3.5 moderate and severe injuries per 1,000 surfing days. However, this data may overestimate the injury rate due to reporting bias as the studies were survey based [36]. For competitive surfing, a rate of 13 acute injuries per 1,000 h has been reported [42].
Overall, most studies have found being hit by a surfboard to be the most common cause of surfing-related injury [36, 37, 42–44]. For example, Taylor et al. reported striking a surfboard or another surfer (45 %), “wiping out” (36 %), and striking the seabed (18 %) as the most common causes of acute injuries [43]. In another survey study of the lacerations to the head, 15 % were to the eyebrow [36]. Three severe injuries were reported to have occurred in California in the winter months after the surfers “wiped out” when trying to ride a large wave or avoid an oncoming wave [45]. Head and leg injuries have been reported most commonly with surfing [36, 37], except in competitive surfers where knee sprains/strains occurred most frequently [42].
Data is also lacking on the epidemiology of ocular and orbital trauma due to surfing. In the literature, there have been more reports of surfing-related ocular injuries in males [46], but this is probably due to the fact that there are many more male than female surfers. Of all eye trauma, sports-related injuries form a small proportion but have a significant morbidity [40] and form a significant proportion of enucleations [47].
Eye injuries in surfing are mainly due to blunt trauma from direct high-energy collision with the tip of the surfboard [48], and the most common injuries include lacerations and soft-tissue injuries [36, 37]. When the energy is dissipated into the orbit, burst lacerations occur with disruption of ocular tissues, global rupture, and orbital fractures [41].
Over time, boards have become smaller and lighter with a sharp nose, tail, and skeg; leashes have been elasticized and surfing breaks have become more crowded [36]. It has been postulated that these factors may have resulted in an increase in head/face injuries, since shorter and lighter boards are more likely to be thrown around in the surf [39, 41], with the elasticized leash “snapping” the board back toward the surfer with considerable force and energy [37].
5.5.2 Mechanism and Clinical Features
Injury typically results from direct trauma by the surfer’s own surfboard [36, 37, 46]; impact with rocks or other surfers’ boards are less frequently responsible [36]. Injury most commonly results from impact with a sharp part of the surfboard such as the nose, fin, or tail [36, 45, 46] at high velocity following a fall [46]. The nose is most frequently involved as it is small enough to fit into the bony orbit [37, 46]. Trauma occurs when the energy from collision with the board is dissipated into the orbit; this disrupts ocular tissues and can produce global rupture and orbital fractures [41].
The introduction of leashes in surfing has been implicated in ocular injury [45]. The leash connects the surfer’s ankle to the base of the surfboard, preventing it from being lost following a fall. However, after a fall, the leash allows the surfboard—which can travel at great speed and have significant mass—to be snapped back at the surfer with great force and energy transmitted from the broken wave [37, 46]. The length of the leash can vary, and although a short leash has the advantage of keeping the surfboard close to the surfer, it may also place the surfer at greater risk [36]. In one series of surfing-related ocular injuries, all surfers were using short leashes [45]. In another, leashes were found to be responsible for 9 % of all injuries reported [36]. Notably, however, leashes can prevent injuries from loose boards and act as a floatation device in the case of severe injury [36].
Retained foreign bodies, although less common, have also been reported with surfing-related trauma and are thought to occur due to impact at high velocity [46]. This is similar to other sports with high-velocity impact, such as water skiing [46]. Notably, most modern surfboards are constructed with a light polyurethane foam core reinforced by a rigid fiberglass (silicon dioxide, various metals, and elements) and resin skin [37, 41]. These are covered by a fabric made by forcing molten glass through a sieve, which is then spun into threads and woven in sheets [41]. One study reported the case of an orbital foreign body due to retained fiberglass following a high-energy surfing trauma [41], while another reported a foreign body pseudotumor (“surfinoma”) in association with a retained piece of fiberglass from a surfboard [48].
5.5.3 Morbidity
Surfing-related eye injuries have a high ocular morbidity, with many resulting in permanent visual loss [45, 46]. In one study, retinal specialists in three states of the USA (California, Florida, and Hawaii) reported 11 injuries, with only two patients regaining their pre-injury vision. Five of these patients had a final vision of hand movements or worse [46]. The poor outcomes were due to a high rate of posterior segment trauma and globe rupture [46]. Given that young males entering their productive years are the most commonly affected, visual disability can have a significant psychosocial impact [46].
5.5.4 Management of Surfing-Related Ocular Trauma
Surfing-related ocular trauma should be managed according to principles of trauma management. This means that general trauma management should be provided prior to attending to the eye—control of bleeding, consideration of neck injury, immobilization of injured areas, and close monitoring for life-threatening emergencies, such as a cervical facture or splenic rupture [39]. Tetanus status should be determined and prophylaxis given as appropriate.
Ocular and orbital management will then depend on the severity of the injury and the particular ocular, orbital, and/or periorbital structures involved. Ocular and skin “aquatic” wounds should be irrigated with balanced salt solution and normal saline (0.9 % sodium chloride) [49], respectively, to reduce the risk of infection. If required, debridement is then performed to remove foreign bodies and/or devitalized tissue. As surfing-related trauma occurs in an aquatic environment, the water may be contaminated with bacteria and sediment. This should be followed by primary repair of a globe rupture or skin lacerations as soon as possible. However, if an injury is not debilitating, a surfer may continue to surf and delay their presentation for days [39], and secondary repair may be needed in some cases. Following globe rupture, retinal review is required due to the risk of vision-threatening posterior segment complications [46].
The literature reports cases of bacteria isolated from surfers wounds, including Staphylococcus albus, Staphylococcus aureus (coagulase-positive), Escherichia coli, and beta-hemolytic Streptococcus pyogenes (group A) [50]. The possibility of infection should therefore be considered, skin wounds should be cleaned, and broad spectrum antibiotic coverage given. If infection does occur, it may become chronic and be associated with soft tissue inflammation [51, 52]. Notably, some surf breaks may be located close to sewerage outlets. For ocular injury, close monitoring for endophthalmitis is essential.
Following an injury, the surfer should be strictly advised when they can return to surfing; surfers are notoriously keen to return to surfing and may do so before being advised [39].
5.6 Prevention of Surfing-Related Ocular Trauma
Prevention is a key part of the management of surfing-related ocular trauma, as injuries can have a high morbidity despite treatment once they have occurred [46]. Although board modifications and safety equipment can prevent injuries, they may alter the performance, look, and image of the board or surfer [37]; given that surfing is associated with a carefree attitude, the introduction of such preventative measures can be difficult [41]. In competitive surfing, mandatory use of modified boards and safety equipment may help their adoption on a wider scale [37]. Research to firmly establish the benefits of safety measures would also be beneficial [53].
5.6.1 Board Modifications
As the nose of the board, in particular, is responsible for most injuries, blunting or fitting a protective guard over this part can reduce injury [36, 37, 46], making the nose wider than the average human orbit—a width of 40 mm and a height of 35 mm [46]. In Australia, standards for nose shape now exist for surfboard manufacturers [54], as simple modifications to surfboard design have the potential to save sight.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







