Thumb Hypoplasia
CASE PRESENTATION
A 9-month-old child comes in for evaluation of a “weak thumb” (Figure 10-1). The parents report that this was noted at birth but have not yet sought orthopaedic consultation due to other medical issues. While at times the child uses the thumb for spontaneous grasp and pinch, at other times the child will attempt to hold and manipulate small objects between the index and long fingers.
CLINICAL QUESTIONS
What are the characteristic clinical features of the hypoplastic thumb?
What medical conditions and syndromes are associated with thumb hypoplasia?
How is thumb hypoplasia classified?
What are the treatment principles?
What are the indications for surgical reconstruction?
What types of operations are performed for the hypoplastic thumb? What factors determine which types of operations to perform?
What is a pollex abductus?
What is a chondrodesis?
What are the expected outcomes and potential complications of surgical treatment?
THE FUNDAMENTALS
You don’t need thumbs…My best friend is my brother’s dog. He doesn’t have any thumbs and he’s doing fine.
—Pat Angerer, Iowa Hawkeyes offensive lineman
Etiology and Epidemiology
The upper limb develops during the fourth to seventh week of gestation (see Chapter 1). A number of signaling centers have been identified that contribute to upper limb morphogenesis, patterning, and differentiation. The apical ectodermal ridge (AER) is responsible for proximal-distal development, mediated by a number of fibroblast growth factors.1 The zone of polarizing activity (ZPA) has been implicated in anterior-posterior pattern formation, mediated in part by sonic hedgehog and homeobox (HOX) gene products. Finally, the WNT7a signaling center directs dorsalventral development. While the exact mechanisms are yet unknown, it is believed that abnormalities in the AER and/or ataxic insult on the ZPA may result in thumb hypoplasia, with or without radial longitudinal deficiency.2, 3 and 4
Thumb hypoplasia represents approximately 5% to 15% of all congenital hand differences.5,6 Males and females are equally affected, and the right thumb is more commonly involved than the left.7,8 In over half of cases, there is bilateral, though often asymmetric, involvement.
In up to 40% of cases, thumb hypoplasia may present in association with known syndromes (Table 10.1).7, 8 and 9 Awareness of syndromic associations is critical, as often the hand surgeon is the first medical care provider to evaluate the patient; in these situations, potentially life-altering diagnoses and lifesaving interventions can be made. The VACTERL syndrome denotes combined abnormalities of the vertebrae, anus, cardiovascular tree, trachea, renal system, and limb buds. (The classic “VACTERRL” syndrome involves Vertebral anomalies, Anal atresia, Cardiac defects, Tracheo-Esophageal fistula, Renal, and Radial Limb anomalies.)10, 11 and 12 Holt-Oram syndrome refers to thumb hypoplasia associated with congenital heart defects, typically atrial and ventricular septal defects. The genetic mutations for Holt-Oram syndrome have been identified as involving the TBX5 gene in over 70% of patients.13 Fanconi anemia also has an autosomal dominant inheritance pattern. In infancy, there are usually characteristic facial features (microphthalmos, strabismus, and hearing deficits).14 Pancytopenia often does not present until later in childhood. Fanconi anemia can be identified by a mitomycin C test, but it is now advocated that all infants with thumb hypoplasia and/or radial-sided defects be assessed early for Fanconi anemia with the diepoxybutane test, since a delay in diagnosis can have potentially life-threatening consequences.15 Thrombocytopenia with absent radius is also from autosomal recessive inheritance. While no causative genetic mutations have been identified, patients demonstrated deletions on the long arm of chromosome 116; both the c-mpl gene and the HOX genes have been implicated.17,18 The thrombocytopenia is present at birth. The platelet count usually improves with growth, and hand surgery should be delayed until it is safe.14, 15, 16, 17, 18 and 19
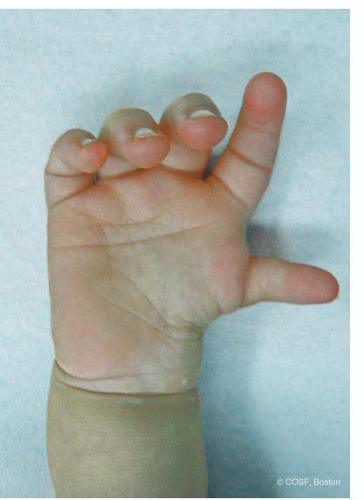 FIGURE 10-1 Clinical photograph of a Blauth type IIIA hypoplastic thumb. Note lack of IP joint skin crease and thenar muscle bulk. |
Table 10.1 Syndromes associated with thumb hypoplasia | |||||
|---|---|---|---|---|---|
|
Clinical Evaluation
Coaches have to watch for what they don’t want to see and listen to what they don’t want to hear.
—John Madden
Clinical evaluation begins with careful inspection and physical examination. To identify the underdeveloped thumb, one must understand what constitutes “normal.” In a previous study of 546 hands in 243 patients less than 18 years of age, it was determined that the tip of the adducted thumb reaches to 70% of the length of the index finger proximal phalanx, measured proximal to distal,20 and 32% of the length of the index finger from the meta-carpophalangeal (MCP) joint to its tip. The widths of the thumb and thumb nail were found to be 133% and 105% that of the adjacent index finger, respectively. Interestingly, these comparisons between normal thumb and index digits remain relatively constant among patients of different ages.
Thumb hypoplasia is characterized by five distinct clinical features. First, the thumb is smaller, shorter, and narrower. Second, there may be interphalangeal (IP) joint stiffness with relative paucity of the flexion and extension creases, due to underdevelopment of the extrinsic muscles. Third, the MCP joint is typically unstable, due to ligamentous insufficiency. Fourth, the thenar muscles are underdeveloped and weak, resulting in absent palmar abduction of the thumb and a concavity of the normally prominent thenar eminence. Finally, there is often a first web-space narrowing, likely due to the imbalance between the robust adductor pollicis and weak or absent thenars. As there is a high frequency of bilateral involvement, comparison to the apparently normal contralateral thumb may often be misleading.
In situations in which there are absent or rudimentary flexion and extension creases of the IP joint, a pollex abductus should be suspected.5 Defined as an abnormal connection between the flexor pollicis longus and extensor pollicis longus tendons, a pollex abductus may be seen in up to 35% of cases and will cause the thumb to rigidly abduct when the extrinsic flexors or extensors are activated. Pre- or intraoperative identification of a pollex abductus is critical, as failure to address this anatomic abnormality may result in suboptimal surgical outcomes.
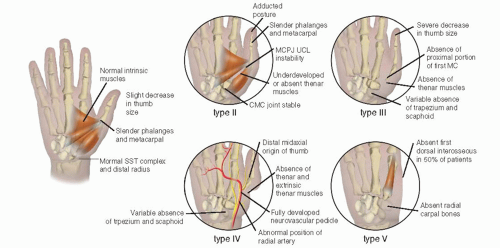
Classification systems of thumb hypoplasia assist in surgical decision making and reflect the evolution in the understanding of this condition. While Müller was among the first to categorize thumb hypoplasia, it is Blauth’s classification (and Buck-Gramcko’s modification thereof) that has withstood the test of time and is most commonly used today (Figure 10-2).21, 22 and 23 A type I thumb is smaller and shorter than normal but still has all the elements that constitute a normal-functioning thumb. Type II thumbs have underdeveloped skeletal elements, MCP instability, first web-space narrowing, and intrinsic (thenar) hypoplasia. Type III thumbs have additional extrinsic deficiencies. The type IV thumb refers to the so-called pouce flottant, or floating thumb; in these situations, the rudimentary thumb is connected to the radial aspect of the hand by a narrow skin bridge without any meaningful musculature or bony connection. Type V denotes the complete absence of a thumb. Type V thumbs are thought to be most common, while type III are second most common.7,8
Two important modifications of the Blauth classification are worthy of note, as they guide surgical planning. Lister subdivided type II thumbs according to
MCP joint stability; type IIA thumbs have uniaxial instability, whereas type IIB thumbs demonstrate global MCP joint instability.24 Furthermore, Manske and McCarroll subdivided type III thumbs into those with a stable carpometacarpal (CMC) joint (type IIIA) and those with unstable CMC joints (type IIIB).25 While the difference between type IIIA and IIIB thumbs is readily apparent in texts and schematic diagrams, the clinical distinction is often more challenging, particularly in the young child in whom there is incomplete ossification of the skeletal structures.
MCP joint stability; type IIA thumbs have uniaxial instability, whereas type IIB thumbs demonstrate global MCP joint instability.24 Furthermore, Manske and McCarroll subdivided type III thumbs into those with a stable carpometacarpal (CMC) joint (type IIIA) and those with unstable CMC joints (type IIIB).25 While the difference between type IIIA and IIIB thumbs is readily apparent in texts and schematic diagrams, the clinical distinction is often more challenging, particularly in the young child in whom there is incomplete ossification of the skeletal structures.
Plain radiographs may assist in the diagnosis and guide appropriate classification, typically demonstrating hypoplastic thumb phalanges or metacarpal, often with a tapered or absent metacarpal base. Initial radiographic evaluation should include the wrist and forearm, given the high association with radial longitudinal dysplasia and radial carpal involvement.26
Given the common syndromic associations, genetic consultation with appropriate cardiac, renal, and hematologic testing are critical in the evaluation of any child with thumb hypoplasia. This includes chromosomal challenge (or chromosomal fragility) testing to rule out Fanconi anemia.27 Furthermore, thorough evaluation of the spine and lower extremities should be done to identify associated VACTERRL or other conditions.
Surgical Indications
Given the importance of the thumb in all aspects of hand function, surgical reconstruction is recommended in all but type I thumb hypoplasia.28, 29 and 30 While the decision to proceed with surgery is easy for patients, families, and care providers alike, it is the type of operation to be performed that remains critical for success. In general, type II and IIIA thumbs are reconstructed, while type IIIB, IV, and V thumbs are treated with thumb ablation and index finger pollicization (see Chapter 11).
The principle of hypoplastic thumb reconstruction is simply to address each abnormal clinical element. The first web space should be deepened, the MCP joint stabilized, and opposition power restored. Little can generally be done to address size differences and thumb IP joint stiffness; for this reason, families should be counseled preoperatively that the thumb may remain smaller in appearance and stiff at the IP joint, even with successful surgical reconstruction.
First web-space deepening is typically achieved with two- or four-part Z-plasties. Alternatively, the Brand rotation flap can be utilized (Figure 10-3).31




Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree