Musculoskeletal
Gastrointestinal
Genitourinary
Systemic
Acetabular labral tear
Inflammatory bowel disease
Nephrolithiasis
Inflammatory arthropathies
Femoral head AVN
Appendicitis
Pelvic inflammatory disease
Lymphadenopathy
Adductor/flexor tendonitis
Diverticulitis
Epididimytis
Lymphoma
Stress fracture
Colorectal malignancy
Ovarian cyst
Sickle cell disease
Osteitis pubis
Gastrointestinal infection
Urethritis
Fibromyalgia
Femoroacetabular impingement
Cystitis
Lumbar radiculopathy
Ectopic pregnancy
Inguinal or femoral hernia
Endometriosis
Iliac apophyseal injury
Prostatitis
Symphyseal instability
Urinary tract infection
Hip osteoarthritis
Testicular/ovarian malignancy
Sports hernia
Testicular torsion
Musculoskeletal malignancy
Hydrocele/vericocele
Septic arthritis
Dysmenorrhea
History
As with any diagnosis, the history is often the most critical subset of clinical data available to the clinician evaluating athletic groin pain. Most patients with an ultimate diagnosis of sports hernia will describe an insidious onset of the exercise-related deep, dull, and diffuse pain about the lower abdomen or groin that is typically unilateral and that has been unresponsive to exhaustive rehabilitation efforts. Sports hernia almost always occurs in athletes participating in sports involving kicking, cutting, and explosive twisting and turning at speed [8]. As mentioned previously, it is therefore most commonly seen in ice hockey, soccer, Australian or American-rules football, tennis, and field hockey. The majority of cases (around 94 %) [1] are described as insidious, however in one series, Meyers et al. found that 71.3 % of patients could recall a specific event or injury which preceded their development of symptoms [17]. They often describe radiation pattern to the perineum, inner thigh, scrotum, or occasionally to the midline [1, 6]. Typically, these symptoms are completely relieved by rest and return with the resumption of rigorous sport often lasting 2–3 days following game day. In addition to frank athletic participation, symptoms are often reproduced by sit-ups, coughing or sneezing, and other valsalva producing maneuvers. The complaint of pain with increased intra-abdominal pressure is extremely important in diagnosing sports hernia, as an intra-articular hip problem will not produce this symptom. Kachingwe et al. describe five signs and symptoms, which when present together, make sports hernia the most probable diagnosis. They include: “(1) a subjective complaint of deep groin/lower abdominal pain, (2) pain that is exacerbated with sport-specific activities such as sprinting, kicking, cutting, and/or sit-ups and is relieved with rest, (3) palpable tenderness over the pubic ramus at the insertion of the rectus abdominis and or conjoined-tendon, (4) pain with resisted hip adduction at 0, 45, and/or 90 degrees of hip flexion, and (5) pain with resisted abdominal curl-up” [18].
In addition to these positive facets of the patient’s history, there are a number of pertinent negative findings that are helpful in narrowing the differential toward sports hernia. Patients do not tend to describe a history of fever, chills, or weight loss, which could point toward a more systemic diagnosis such as infection or malignancy. Persistent rest or night pain is unusual, which could again represent hip or systemic or neoplastic processes. Although stress fractures, such as those involving the femoral neck, can produce activity-related groin pain, they are typically closely linked to a discrete increase in physical activity, which is not classically associated with the presentation of sports hernia. Sports hernia is not typically associated with changes in bowel habits, as is the case with some gastrointestinal causes of lower abdominal and groin pain such as true hernia, inflammatory bowel disease, or diverticulitis. Similarly, although many reproductive disorders such as endometriosis, ovarian cyst formation, leiomyoma, and dysmenorrhea may cause similar groin pain, sports hernia symptoms do not change with the menstrual cycle as these diagnoses do. As such, a thorough gynecologic history as well as a physical exam is necessary in the evaluation of a female athlete when sports hernia is suspected. Sports hernia patients do not tend to report dysuria, which can be associated with other groin pain-producing diagnoses such as urethritis, epididymitis, or pelvic inflammatory disease [1, 4–6, 8–10].
The assembly of these pertinent positive and negative findings should considerably narrow a clinician’s differential diagnoses to a much smaller subset of musculoskeletal pathology. Most authors suggest that the diagnoses that are most difficult to distinguish from sports hernia from a history taking perspective are true hernia, hip adductor and flexor strains or tears, osteitis pubis, peri-articular, and intra-articular hip pathology such as labral, chondral, or osseous injury. Once a patient’s history has helped to narrow the differential to these musculoskeletal diagnoses, the physical exam and certain imaging modalities can help to reliably solidify a diagnosis of sports hernia.
Physical Exam
As described previously, a carefully taken history will have ruled out the more systemic and visceral disorders and narrowed the differential to a smaller subset of musculoskeletal diagnoses. These diagnoses include true hernia, hip adductor and flexor strains, osteitis pubis, peri-articular, and intra-articular hip pathology such as labral, chondral, or osseous injury and finally sports hernia. At this point, a clinician’s targeted physical exam, with these specific diagnoses in mind, should be able to eliminate the remaining mimickers and confidently diagnose sports hernia. One of the challenges of diagnosing sports hernia is that its pathoanatomy does not fit perfectly into one medical subspecialty, making it difficult for any one provider to adequately evaluate a patient with activity-related groin pain. The goal of this section is to provide the description of a set of physical exam maneuvers that cross over subspecialty division, allowing a single clinician to comprehensively assess the patient with suspicion of sports hernia.
True Hernia
The examination should be performed with the patient standing in front of and facing the physician. Initially, the physician will simply visually inspect the groin area with ideally oblique light looking specifically for any bulges. The physician should have the patient cough or valsalva and see if any bulging or abnormal motion occurs. Bulges above the inguinal crease indicate inguinal hernias (direct or indirect); those below the crease indicate the presence of a femoral hernia, the latter of which are a consideration mainly in females. The scrotum should be specifically palpated to assess for large indirect hernias. The examiner should then specifically palpate the regions just above and below the inguinal crease bilaterally, and have the patient cough or valsalva and note any bulge or impulse that occurs which will help to detect and localize any potential hernia. Finally, the physician should perform the traditional exam for inguinal hernia, placing a fingertip into the inguinal canal along the cord structures inverting the scrotum through the external inguinal ring. The presence of a bulge against the tip of the finger would indicate an indirect hernia, while a bulge or impulse with valsalva against the side of the finger through the transversalis fascia indicates the presence of a direct hernia [19]. The presence of a discrete hernia inherently removes sports hernia from the differential.
Adductor and Flexor Strains
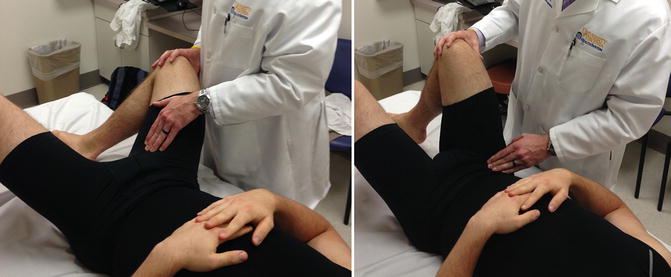
Careful palpation and resistance testing is the most reliable way to diagnose specific adductor and flexor pathology. The patient should be placed supine with knees bent and feet placed together. The patient should then allow their knees to fall apart so that the hips are in an abducted and externally rotated position. The adductors will be on stretch and can therefore be palpated to assess for tenderness. The patient should then be asked to adduct against resistance to increase the sensitivity of this exam. The patient should then flex the hip in neutral rotation to between 45° and 70°. The hip flexors will then be on stretch and can be directly palpated. The same procedure can be done against resistance increasing the sensitivity of the exam [20]. The presence of isolated adductor or flexor tendon pain with this exam indicates that a sports hernia is not present. It is important to note that it is common to have adductor/flexor pain or even strains in conjunction with sports hernia; however, a careful specific sports hernia exam must be performed regardless of the presence of adductor or flexor strains. It is important to note that the sensory nerves, which may be irritated and compressed in sports hernia, provide sensation to the inner thigh, scrotum and groin, and so it may produce pain that closely mimics an adductor strain. This pain is produced by palpation but less aggravated by resisted stretch as is the case with an adductor strain. Additionally, adductor strains should improve with a period of rest and should not worsen with valsalva-producing maneuvers (Fig. 7.1).