Fig. 9.1
Example of upper crossed syndrome (artist rendition)
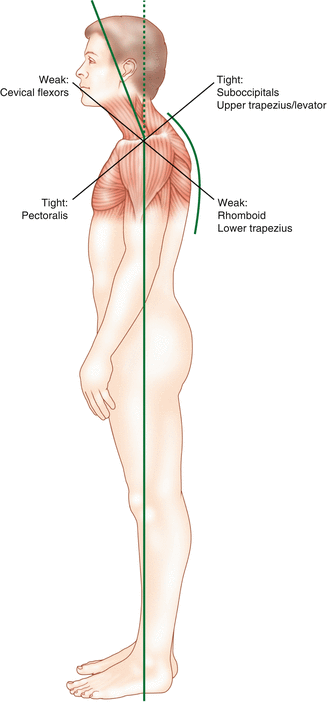
Fig. 9.2
Example of lower crossed syndrome (artist rendition)
Forward head position
Kyphotic shoulders
Tight pectoralis major
Tight upper trapezius
Tight levator scapula
Tight suboccipitals
Weak cervical flexors
Weak rhomboid
Weak lower trapezius
Dr. Janda described the lower crossed syndrome as muscular imbalances between the deep abdominal musculature and the gluteus medius and maximus. This syndrome is characterized by:
Anteriorly tilted pelvis
Weak gluteus medius and maximus
Weak abdominals
Tight iliopsoas
Tight rectus femoris
Tight erector spinae muscles
This imbalance results in postural deviations that include: anterior pelvic tilt, increased lumbar lordosis, lateral lumbar shift, lateral leg rotation, and knee hyperextension. There can also be subsequent joint dysfunction, particularly at the L4–L5 and L5–S1 segments, sacro-iliac joint, and hip joint [9]. Understanding and identifying these types of syndromes will help the practitioner understand what is occurring with the athlete’s static posture, so that dynamic abnormalities will be better understood (e.g., Why are the hamstrings tight? Why are the hip flexors short? Why does the center of gravity move anteriorly during a certain movement?) Some of the most common postural findings in sports hernia/athletic pubalgia cases are a combination of tight hamstrings, anterior pelvis tilt, excessive lordotic curvature, and shortened hip flexors. An observant therapist can detect all of these muscular imbalances in a person’s static posture [10].
Based on our clinical experience, we recommend that a dynamic full body screen be incorporated into the traditional assessment. The dynamic full body movement screening will help gain a qualitative value on how the patient moves and can be an important part of the assessment. There are varying schools of thought on movement screening. Though different, the screenings address complete body movements that can be scored into quantitative values to establish a baseline, monitor rehabilitation progression, or develop a global view of the underlying cause of the pathology. Any movement irregularity will be associated with some sort of muscular imbalance or motor control abnormality [5, 6]. This imbalance, or motor control issue, will show up on the screening and can be scored accordingly to the specifics of the test being administered. This screening offers a unique snapshot of how the body moves throughout the kinematic chain during specific movements. The purpose of the dynamic assessment will be to zero in on the causative factor of the pain and dysfunction. Once a full body screen has been obtained, the clinician can identify specific areas of compensation, evaluate locally, and address potential muscular weakness, flexibility, motor control, or joint mobility restriction appropriately. These screens may also be a predictive way of helping to prevent injury when applied as a pre-screen for athletic populations by identifying dysfunctional movement patterns and serve as a baseline prior to starting an exercise program [6, 11].
There are several commonly occurring movement dysfunctions observed in the sports hernia patient during a dynamic assessment. These include an elongated rectus abdominis, altered hip flexion patterns, an inability to disassociate the hips during movement, and delayed transverse abdominis timing and activation.
Elongated rectus abdominis: An anteriorly tilted pelvis, as observed in the lower crossed posture, will cause an elongation of the rectus abdominis musculature. This will place it in a biomechanically disadvantageous position in comparison to the adductors on the antagonistic side of the pelvis. Evaluation for a weak synergistic muscle will likely reveal deficient strength of the external oblique muscles [5]. Strengthening the external oblique will help correct the patient’s anterior pelvic tilt, while helping to decrease the strain on the common aponeurosis of the transverse abdominis, internal oblique, and underlying fibers of the rectus abdominis. Clinicians should instruct the patient to find a pelvic neutral position during corrective exercises.
Altered hip flexion patterns: Observation of hip flexion patterns typically reveals an externally rotated femur and almost “tailor” like hip flexion pattern, exaggerated in some patients more than others (Figs. 9.3 and 9.4). During functional movements such as running, the adductor musculature, which is starting out in a strained position, theoretically would become overworked while trying to maneuver into hip flexion and adduction from the abducted starting place.

Fig. 9.3
Normal hip flexion pattern

Fig. 9.4
Altered hip flexion pattern
Hip disassociation: The patient tends to be unable to achieve isolated hip flexion and extension without compensatory contralateral hip flexion. In our experience, establishing hip disassociation helps create the greatest strides in rehabilitation progression. This altered hip flexion pattern can be evaluated by having the patient lay supine off a corner of a wall. The patient lies with one hip flexed to 90°, gluteus musculature and hamstrings flush with the wall, while the other leg is extended out straight (0° of hip flexion) (Figs. 9.5 and 9.6). Most commonly, the sports hernia patient will demonstrate 10–20° of hip flexion with a component of external rotation on the hip at neutral (Figs. 9.7 and 9.8). In the suggested rehabilitation protocol, hip flexion and hip disassociation exercises are listed separately, although both types of exercises help to establish hip disassociation.

Fig. 9.5
Example of hip disassociation evaluation/exercise resting position—normal hip flexion mechanics (starting position)

Fig. 9.6
Example of hip disassociation evaluation/exercise resting position—normal hip flexion mechanics (ending position)

Fig. 9.7
Example of hip disassociation evaluation/exercise resting position—altered hip flexion mechanics (starting position)

Fig. 9.8
Example of hip disassociation evaluation/exercise resting position—altered hip flexion mechanics (ending position)
Delayed transverse abdominis timing and activation: The transverse abdominis has been shown to activate prior to other abdominal musculature to insure trunk stability prior to lower extremity movement. In patients with chronic groin pain, onset of this feed-forward mechanism is delayed [12]. Re-establishing the activation and timing of this muscle will be a component of the suggested rehabilitation progression.
After identifying any gross biomechanical deficits or dysfunctional movement patterns during the dynamic assessment, the athletic trainer may then look locally to determine the cause of the dysfunction. This examination will scrutinize the patient’s structural and dynamic findings associated with specific musculature and joints. Screening results may then lead to specific joint examinations including palpation of tissues, active and passive range of motion, manual muscle testing, and orthopedic special tests. The quantitative values can then be analyzed against other normative values in the literature and used as another tool for rehabilitative prescription.
Range of motion assessments during the initial evaluation will make the clinician aware of any flexibility issues that need to be addressed (Tables 9.1 and 9.2) [7, 13]. Evaluation may reveal passive range of motion that is not functional or being underutilized. Comparing passive range of motion values with active range of motion testing will reveal whether or not the patient has the ability to utilize their full motion. This indication of motor control should be tested in both weight bearing and non-weight bearing positions.
Table 9.1
Normal hip and knee range of motion
Joint | Flexion (°) | Extension (°) | Abduction | Adduction | Internal rotation (°) | External rotation (°) |
|---|---|---|---|---|---|---|
Hip | 125 | 10–30 | 45–50° | 10–30° | 35 | 45 |
Knee | 140 | 0 | n/a | n/a | 10 | 10 |
Table 9.2
Normal ankle range of motion
Dorsiflexion (°) | Plantarflexion (°) | Inversion (°) | Eversion (°) | |
|---|---|---|---|---|
Ankle | 20 | 50 | 5 | 5 |
The physical therapist Shirley Sahrmann coined the term “relative flexibility/stiffness” based on her clinical impression that most people don’t need to be passively stretched [5]. Stiffness refers to the tissue’s “resistance to passive elongation.” A majority of flexibility issues are due to a less stiff muscle and/or ligamentous complex relative to the stiffness of the muscle being stretched. The body will compensate through a pattern of least resistance to achieve its goal of functional movement. This sometimes results in the appearance of inflexibility when the problem is really a lack of stability, or stiffness, at another joint or muscle. When considering patient range of motion and flexibility, the clinician must discern if movement is accomplished at the expense of maintaining a neutral posture. This important differentiation insures that the muscle needs to be elongated before compromising its passive tension.
The etiology of sports hernia remains a subject of discussion (see Chap. 1). Some quantitative values and strength ratios that have been hypothesized as potential causes of sports hernia include: decreased adductor:abductor strength ratios [14], hip mobility/flexibility decrements [15], and the abdominal/adductor antagonistic equilibrium [16]. Addressing these deficits has been correlated with injury reduction. The clinician should consider these ratios during the evaluation, but they should not be the entire basis of the evaluation.
Rehabilitation
When designing a rehabilitation program for a patient that has been diagnosed with sports hernia/athletic pubalgia it is important for the clinician to design each program specifically from the findings of their assessment. For operative patients, preoperative assessment is highly recommended to provide a more accurate baseline. For the purpose of this chapter, we will describe how a therapist could proceed once a referral and diagnosis of sports hernia have been made for both non-operative and postoperative patients.
The success of conservative management of sports hernia/athletic pubalgia remains uncertain [17]. Most programs follow a process of a rest period, rehabilitation, functional activities, and a return to sport progression lasting approximately 6–8 weeks. Exercise progressions focus on core stabilization, hip range of motion, local and global strengthening, and then sport-specific activities. There have been two proposed algorithms to follow for conservative management. These rehabilitation programs can last up to 10 weeks or as little a 3–4 weeks. Success of each program is dependent on the mechanism of injury and the amount of advancement made through rehabilitation towards return to sport, with the goal of returning patients’ to their previous level of activity [4, 17]. Clinical experience and a review of the literature are the basis for the recommended strategy of this non-operative rehabilitative progression. The key determinant for success will be the amount of time allowed to facilitate the rehabilitation program and corrective exercise prescription. The following protocol would need to be catered to the specific deficits or dysfunction found in each patient.
Rest
The prescribed rest period varies according to the duration and severity of symptoms, but a range of 4–12 weeks has been found in the literature [2–4, 17–19]. This implies rest from all aggravating activities, including activities of daily living (ADLs) if the patient is that debilitated. Crutch use to reduce weight bearing should be considered in patients with pain during walking but is rarely indicated. Stationary bike may be allowed once the patient is pain free with ADLs. Modification of strength training activities should include eliminating all painful exercises, while limiting any Valsalva-type maneuvers to reduce strain on the core. Squats and lunges in particular should be avoided until the patient has reached more advanced levels of function through rehabilitation. At the physician’s discretion, anti-inflammatory medications may be prescribed during the initial resting phase of rehabilitation [1, 20–22]. Unfortunately, rest alone has been associated with only a temporary abatement in symptoms that tend to rapidly return upon resumption of activity.
Injections
There are mixed results in the literature regarding the efficacy of long acting steroid injections in the management of sports hernia. Injections are typically placed either in the pubic symphysis or near the pubic insertion of the adductor longus tendon. Schilders reported excellent pain relief following pubic cleft injections in patients with no evidence of adductor longus inflammation on magnetic resonance imaging (MRI). In patients with observable adductor inflammation, the majority had recurrence of pain at a mean of 5 weeks [23]. In contrast, Ashby [24] described successful pain relief following insertional injections in patients with identified adductor or rectus abdominis inflammation at the pubic attachment. Topol examined the effectiveness of monthly dextrose prolotherapy injections in the treatment of kicking-sport athletes with chronic groin pain. Subjects experienced pain relief following an average of 2.8 injections, with the location dependent on palpatory tenderness [25]. In each of these studies, the lack of a control group or comparison to the effects of time and rehabilitation are confounding factors. Providers should be cautious to avoid repeated injections into the symphysis pubis as this may result in osteolysis and weakening of ligamentous or capsule supports and secondary destabilization of this joint.
Modalities
The use of modalities in conjunction with active rehabilitation may help reduce patient pain and/or stiffness. A variety of forms of cryotherapy, thermotherapy, and electrical stimulation are recommended in the literature for management of sports hernia [1, 18, 20, 22, 26, 27]. Cryotherapy, including cold tub immersion, ice bags, or ice cup massage over the painful area, is frequently utilized as part of a course of treatment to reduce pain and inflammation. Heating modalities such as moist hot packs or therapeutic ultrasound over the proximal adductor tendon are often used in the post-acute stages to help reduce stiffness prior to stretching, soft tissue work, or therapeutic exercise. Various forms of electrotherapy are appropriate for pain control throughout the rehabilitation process, including transcutaneous electrical nerve stimulation, interferential current, or microcurrent.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







