Fig. 1.1
Schematic anatomy of the pubic symphysis. (a) Partially rotated view (b) anterior view
Abdominal Wall
Numerous muscles responsible for stabilization of the pelvis have a common attachment point on the pubic symphysis, including the muscles of the abdominal wall. From superficial to deep the structures of the abdominal wall include: skin, fascia, external oblique muscle and fascia, internal oblique muscle and fascia, transversus abdominis muscle and fascia, and transversalis fascia. Deep to this is parietal peritoneum. The rectus abdominis is the principal vertical midline muscle of the abdominal wall, consisting of two strap-like muscle bellies. These bellies are divided by a strong fibrous band formed by the aponeuroses of other abdominal muscles, known as the rectus sheath. The difference between the manner in which the aponeuroses decussate and split the rectus in the superior and inferior aspects of the abdominal wall forms a potential area of vulnerability. In the cranial 3/4th of the wall, the internal oblique aponeurosis splits the rectus, leaving its posterior lamina and the transversus abdominis completely posterior. However, below the level of the semicircular or arcuate line in the caudal 1/4th of the abdomen, the internal oblique and transversus abdominis both pass anterior to the rectus, leaving only peritoneum as the posterior layer. This anatomic feature is hypothesized as a potential contributing factor in the development of hernias [4].
The rectus abdominis originates from the pubic symphysis crest and inserts on the xiphoid process and fifth to seventh costal cartilages. It is innervated by the lower costal and subcostal nerves, which arise from the ventral rami of the caudal six thoracic nerves. It receives the majority of its blood supply from the superior and inferior epigastric arteries, with smaller contributions from the posterior intercostal, subcostal, posterior lumbar, and deep circumflex iliac arteries. The rectus abdominis functions to flex the trunk, and compress and protect the abdominal viscera. The muscle tapers significantly from cranial to caudal with its proximal insertion approximately three times wider than its distal origin. The resulting concentration of force over a smaller area may predispose the distal origin of the muscle to injury [9].
The inguinal canal passes through the caudal extent of the abdominal wall, extending from the deep inguinal ring formed through the transversalis fascia to the superficial inguinal ring formed through external oblique aponeurosis (Fig. 1.2). The deep ring is located approximately midway between the anterior superior iliac spine and pubic tubercle, while the superficial ring is directly superolateral to the pubic tubercle. The spermatic cord in males and round ligament in females pass through it. The canal has both anterior and posterior walls, as well as a roof and floor. The anterior wall is formed by the aponeurosis of the external oblique muscle, while the transversalis fascia forms the posterior wall. In only 5 % of cases or less is the transversalis fascia joined by fibers from the internal oblique, forming the so-called conjoined tendon. The roof of the inguinal canal is composed of fibers of the internal oblique and transversus abdominis muscles and the inguinal ligament and lacunar ligament form the inferolateral boundary [9].
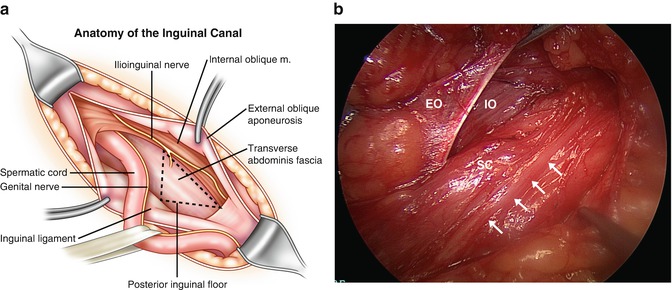

Fig. 1.2
(a) Schematic depiction of inguinal floor/canal anatomy; (b) operative photograph of normal inguinal anatomy—(left side)—EO external oblique aponeurosis, IO internal oblique, SC spermatic cord, arrows point to the ilioinguinal nerve
Two nerves of the abdominal wall, the ilioinguinal nerve and genital branch of the genitofemoral nerve, are often implicated in the pathologic process though to be responsible for chronic groin pain [10]. The ilioinguinal nerve is a branch of the lumbar plexus, originating from the L1 nerve root. It emerges from the lateral edge of the psoas muscle, piercing the transversus abdominis near the iliac crest and the internal oblique prior to entering the superficial inguinal ring. It does not enter the deep inguinal ring. Along its course, it provides branches to both the transversus abdominis and internal oblique before eventually providing sensation to the scrotum or labia majora and medial aspect of the thigh. The genitofemoral nerve emerges from the L1 and L2 nerve roots of the lumbar plexus before dividing into two branches. The femoral branch provides sensation to the skin of the anterior thigh in the area of the femoral triangle. The genital branch passes anterior to the psoas muscle and either perforates the transversalis fascia or passes directly into the deep inguinal ring. It travels within the spermatic cord to the scrotum, providing innervation to the cremaster and dartos muscles, as well as some fibers to the skin of the scrotum [9].
Adductor Muscle Group
The adductor muscles also have a common origin on the pubis. They not only provide adduction of the thigh but also function in concert with the hip flexors and external rotators to stabilize the pelvis through the swing phase of gait [8]. The muscles of the adductor group make up the medial compartment of the thigh (Fig. 1.3). They include the adductor longus, adductor magnus, adductor brevis, gracilis, and pectineus. The anatomic appearance and relationships on imaging are seen in Fig. 1.4.
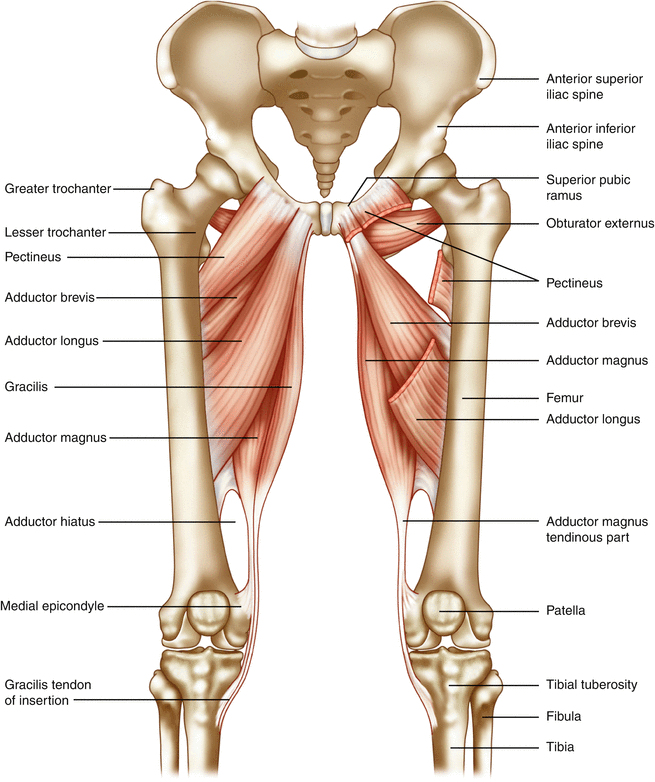
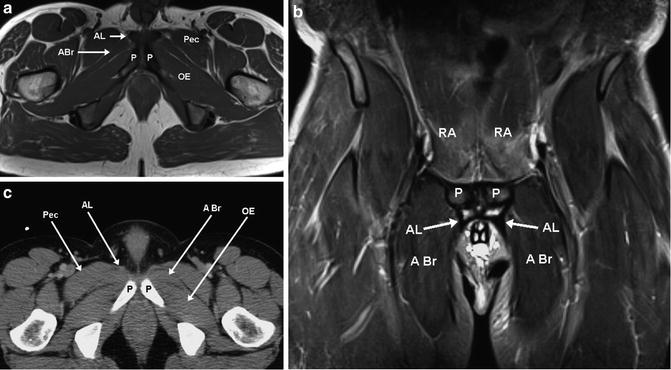

Fig. 1.3
Schematic anatomy of adductor muscle group

Fig. 1.4
Imaging of adductor group and relationships to pubis (a) axial MRI sequences; the adductor longus tendon is the dark triangular area just below the pubis; (b) coronal MRI. In this case, there is detachment of the adductor longus tendon from the pubis as evidenced by the area of bright signal just below the pubis; (c) CT cross-sectional appearance. AL adductor longus, ABr adductor brevis, Pec pectineus, P pubis, OE obturator externus, RA rectus abdominus
The adductor longus is the most anterior of the three adductor muscles, lying medial to the pectineus. Originating from the anterior margin of the pubis, it has a large triangle-shaped muscle belly that broadens significantly prior to its insertion on the linea aspera of the mid-femur [8]. The proximal musculotendinous junction is the most common site of injury, with a predominance of the tears involving the anterior aspect of the tendon. This has been attributed to both the more highly developed nature of the anterior compared to the posterior junction, where the muscle fibers attach direct to bone, as well as the relatively poor blood supply of the junction, which may decrease both the ability to resist force and repair injury [8]. The blood supply is predominately from a branch of the deep femoral artery known as the artery of the adductors. The muscle is innervated by an anterior branch of the obturator nerve via the L2–4 nerve roots [9].
Moving from anterior to posterior, the adductor brevis and adductor magnus are located posterior to the adductor longus. The adductor brevis originates from the anterior pubic body and inserts on the proximal linea aspera. Similar to the adductor longus, it receives its blood supply from the artery of the adductors and innervation from the anterior branch of the obturator nerve (L2–4 nerve roots). As its name implies, the triangular-shaped adductor magnus is the largest muscle of the group. It is composed of two distinct segments. The adductor segment arises from the inferior pubic ramus and inserts on the linea aspera distal to the adductor brevis. It acts to adduct the thigh, with its innervation provided by the posterior branch obturator nerve (L2–4 nerve roots). The muscle also contains a hamstring segment, which originates from the ischial tuberosity and attaches distally to the adductor tubercle of the femur. Functioning as a thigh extensor, it gains its innervation from the tibial division of the sciatic nerve (L4 nerve root). Given the muscle’s extensive size, the blood supply originates from multiple arteries. The majority of blood flow is provided by the deep femoral artery with smaller contributions from the medial circumflex and popliteal arteries [9].
The gracilis and pectineus muscles complete the adductor group. The most medial adductor muscle, the gracilis, is a strap-like muscle which attaches proximally to the pubic body and inferior ramus. It inserts distally on the pes anserine, acting to adduct the thigh and to flex and internally rotate the hip and flex the knee. In accordance with the other adductor muscles, it garners its blood supply from the artery of the adductors and innervation from the obturator nerve (L2–3 nerve roots) [9]. The pectineus muscle is located anterior to the adductor longus and is often classified as a muscle of the anterior, rather than medial compartment. It acts similar to the other adductor muscles, functioning to adduct the thigh and flex and internally rotate the hip, but through a different blood supply and innervation. The medial circumflex artery predominately supplies its blood supply, while the femoral nerve (L2–3 nerve roots) and accessory obturator nerve provides its innervation [8].
Etiology
Within the literature, there is a lack of agreement on the etiology of sports hernias. The incidence in professional athletes has been estimated between 0.5 and 6.2 % [10]. Published studies have identified sports that involve use of the proximal thigh and lower abdominal muscles for kicking, cutting, or pivoting as risk factors for development of the condition [4]. The most commonly implicated sports include soccer, ice hockey, rugby, or Australian rules football, American football, skiing, and running [11]. Men are much more commonly affected than women, and the condition is typically insidious in nature, with few athletes able to describe an acute event [4]. Symptoms are most commonly unilateral but can affect both sides [8].
Overuse, abdominal and adductor muscle strength mismatch, reduced hip range of motion, and congenital inguinal wall weakness have all been implicated in the development of chronic groin pain [10]. Imbalances in strength, coordination, endurance, or range of motion which lead to overload and eventual failure of muscle attachments and/or non-contractile tissues represent key factors in all proposed etiologies. The pubic symphysis can be viewed as a central point linking the posterior pelvis, abdominal wall, and lumbosacral spine with the hips and lower extremities. The concept of the “pubic joint” was first proposed by Meyers et al. [12] to help understand these complex relationships. In this model, the central pubis acts as a large complex rotational joint or central fulcrum for the powerful abdominal and thigh muscles. Imbalances in forces or motion would, therefore, place increased shear stress across the pubis and result in eventual excessive load and failure of the opposing muscles or aponeurotic attachments. Some authors have speculated that off-season training programs may accentuate the imbalance between strong adductor muscles and weak abdominals. This view is supported by studies which demonstrated that adductor strains were 20 times more likely in hockey training camps than during the regular season [10].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







