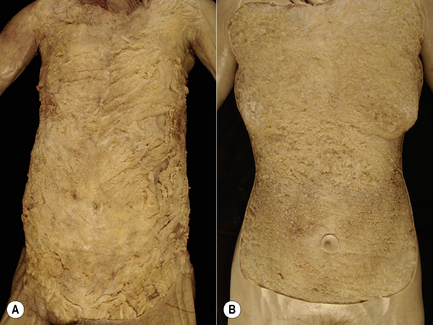
1.2 Somatic fascia Overview of the organization of somatic fascia in the body When we think about the somatic portion of the body, images of skeletal muscle, bones, and joints usually present to mind. However, none of these structures can suffer much direct contact without developing significant pathology. For protective reasons, all of the somatic structures are embedded in a matrix of soft connective tissue termed fascia – the bandage or packing substance of the body. Muscles develop in a matrix of connective tissue such that the adult organ is surrounded by an epimysium, bone arises in a matrix of embryonic fascia termed mesenchyme, which in the adult form becomes the periosteum, and joint capsules consolidate out of a thickening in mesenchyme (Gardner 1963) that ultimately forms a fascial covering over the dense layers of the capsule. In each case, the fascial sheet embracing the somatic structure protects it from direct abrasion by surrounding structures while also providing a conduit through which neurovascular bundles can easily penetrate. By surrounding the components of the somatic system, fascia creates complex and continuous planes or sheets of connective tissue that unite all portions of the body and present continuous planes along which anatomists tend to dissect (Huber 1930). The functions of fascia tend to dictate its structure. Fascia must be capable of significant distortion in multiple planes of direction and return rapidly to its native shape. This type of action is best met by constructing fascia out of irregular connective tissue where the fibrous component is interwoven; thus proper fascia is defined as connective tissue with an irregular distribution of fibrous elements as opposed to those tissues containing parallel arrays such as are seen in tendons, ligaments, aponeuroses and joint capsules (Clemente 1985; Standring 2008). The irregular weave of the fibrous component allows for movement and resistance in all directions but is master of none. Thus, tearing fascia apart can be difficult in all planes of dissection. Conversely, due to the highly regular arrangement of collagen fibers in a tendon, ligament, or aponeurosis, these structures can provide maximal resistance of stretch in one or a limited number of directions but can easily be shredded with finger tips when stressed in orthogonal planes. The density of the fibrous component of fascia will vary tremendously with is location and function. Thus, fascia underlying the skin must be very movable and therefore has a lower density of collagenous fibers; this is often given the ambiguous term superficial fascia (Singer 1935; Clemente 1985; Standring 2008). Alternatively, the fascia that invests muscle, ligament, tendon, or joint capsule is providing a stronger support role and is often termed investing fascia, the density of its collagen fibers being considerably higher; however, they are still irregular in weave (Singer 1935; Clemente 1985; Standring 2008). Several attempts at describing the fasciae of the body have been published (Gallaudet 1931; Singer 1935; Benjamin 2009). This chapter focuses on irregular connective tissue or “proper fascia” and will describe a system of four primary layers that cover the axial portion of the body. Modification of this fundamental plan will allow accommodation of the limbs. The four primary layers in the torso are arranged as a series of concentric tubes (Plate 1.2.1). Starting with the outermost layer of fascia, it is best termed the panniculus or panniculus adiposus: a term used by Singer (Singer 1935) in his treatise on fascia and strongly urged for general usage by Last (Last 1978) in his textbook of anatomy. Deep to the pannicular layer is the axial fascia of the torso. This layer gives rise to the investing fascia or epimysium of the axial muscles, peridentium and periligamentum of tendons and ligaments, and the periosteum of bone. The axial layer of fascia is continuous with the appendicular (investing) fascia in the extremity. As with the pannicular layer, the axial layer can be subdivided; however, again, in this chapter it will be treated as a primary layer. Internal to the axial fascia are two additional layers: the first surrounds the neural structures and can be termed meningeal fascia and the second surrounds all body cavities and is best termed visceral (splanchnic) fascia. In considering the limbs, the pannicular layer extends outward covering the entire surface of the limb. Under the pannicular layer, a fascial layer of similar composition to the axial fascia is present surrounding the muscles of the extremity, and can be termed appendicular fascia. It lies deep to the pannicular fascia and invests the appendicular muscles. Regional names often relate the fascia to a specific muscle, i.e., deltoid fascia, pectoral fascia, etc. Internal to the appendicular fascia is the intramuscular septum housing the neurovascular bundles; this septal layer is most likely to be derived from the axial fascia at the base of the limb. The outermost layer is the pannicular fascia (Singer 1935) and is often termed superficial fascia (Clemente 1985; Standring 2008). This layer can be subdivided into several sublayers as outlined in Chapter 1.3. The pannicular layer is derived from the somatic mesenchyme and surrounds the entire body, with the exception of its orifices such as the orbits, nasal passages, and the oral and aboral openings. It is composed of irregular connective tissue with marked regional variation in collagen fiber density as well as variation in adipose cell density (Fig. 1.2.1). While the outermost portion of this layer is typically invaded by much adipose tissue, the inner portion is more membranous in nature and generally very adherent to the outer portion, except over the abdomen where the two can be easily separated by blunt dissection. The thickness of the pannicular layer is highly variable in the human population. In the region of the head and neck, humans have several thin muscles embedded in the pannicular fascia; these are the platysma and associated facial muscles innervated by the facial nerve. Pannicular fascia covers both the axial and appendicular body.
Global organization of fascia in the body
Architecture of fascia – the four primary layers
Four primary layers of fascia
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Somatic fascia