Chapter 123 Silybum marianum (Milk Thistle)
Silybum marianum (family: Compositae)
Common names: milk thistle, marian thistle, St. Mary’s thistle
 Chemical Composition
Chemical Composition
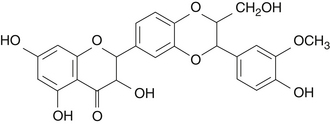
Silybum marianum contains silymarin, a mixture of flavanolignans, consisting chiefly of silybin, silydianin, and silychristine.1–3 The concentration of silymarin is highest in the fruit, but it is also found in the seeds and leaves. Other flavanolignans contained in Silybum include silandrin, silyhermin, silymonin, and neosilyhermin.1 Silybin is the silymarin component with the greatest degree of biological activity (Figure 123-1).
 History and Folk Use
History and Folk Use
Perhaps the most widespread folk use of this plant has been in assisting the nursing mother in the production of milk. It was also used in Germany for curing jaundice and biliary derangements. It is interesting to note that the discovery of the liver-protecting flavanolignans in S. marianum was the result not of systemic pharmacologic screening but rather of investigation of Silybum’s empiric effects in liver disorders.1
 Pharmacology
Pharmacology
Currently S. marianum extracts (usually standardized to contain 70% silymarin) are widely used in European pharmaceutical preparations for hepatic disorders. Silymarin is one of the most potent liver-protecting substances known.1–8
Hepatoprotection Effects
Free Radical Scavenging
Silybum’s ability to prevent liver destruction and enhance liver function is due largely to silymarin’s inhibition of the factors responsible for hepatic damage—free radicals and leukotrienes—coupled with its ability to stimulate liver protein synthesis. Silybum components prevent free radical damage by acting as antioxidants.1–4 Silymarin is many times more potent in antioxidant activity than vitamin E.
Effects on Hepatic Glutathione
Silymarin prevents the depletion of glutathione (GSH) induced by alcohol and other liver toxins. Even in normal people, silymarin has been shown to raise the basal GSH level in the liver by 35%.
Protection from Liver-Damaging Chemicals and Drugs
The protective effect of Silybum against liver damage has been demonstrated in a number of experimental and clinical studies. Experimental liver damage in animals can be produced by such diverse toxic chemicals as carbon tetrachloride, galactosamine, ethanol, and praseodymium nitrate. Silymarin has been shown to protect the liver from all of these toxins.1–47
Perhaps the most impressive of silymarin’s protective effects is against the severe poisoning by Amanita phalloides (the “death cap” or toadstool mushroom), an effect that has long been recognized in folk medicine.5–7 Ingestion of A. phalloides or its toxins causes severe poisoning and, in approximately 30% of victims, death.
Among the experimental models for measuring protection against liver damage, those based on amanitin or phalloidin toxicity are the most important because these two peptides from A. phalloides are the most powerful liver-damaging substances known. Silymarin has demonstrated impressive results in these experimental models. When silymarin was administered before amanita toxin poisoning, it was 100% effective in preventing toxicity.5,7 Even if given 10 minutes after the amanita toxin, it completely counteracted the toxic effects.
In two cases reported in the literature, silymarin prevented death and greatly reduced the amount of liver damage as long as 24 hours after ingestion of A. phalloides.6 This study reported on a husband and wife who ate toxic mushrooms and experienced gastrointestinal symptoms 18 hours later. Despite initial conventional treatment with gastric emptying, intravenous fluids, activated charcoal, and a duodenal tube, both patients’ laboratory parameters showed deteriorating liver and renal function. Mild hepatic encephalopathy developed in one of the patients. Treatment with intravenous silybinin at a dose of 20 mg/kg body weight, penicillin, and glucose for 3 days resulted in reversal of both the organ failures and encephalopathy.
Silymarin may also be of great value as an adjunct in patients receiving long-term drug therapy. A very interesting study found that silymarin, in an unusually high dose of 800 mg/day, given to psychiatric patients receiving phenothiazines or butyrophenones resulted in significant protection of the liver as measured by malondialdehyde serum liver enzyme levels.9 The silymarin did not interfere with the efficacy of the antidepressants.
Stimulation of Hepatic Protein Synthesis
Perhaps the most interesting effect of Silybum components on the liver is their ability to stimulate protein synthesis.4,10,11 This results in an increase in the production of new liver cells to replace the damaged old ones. Sonnenbichler and Zetl11 have suggested that “silybinin imitates in some way a physiological regulator in animal cells, so that the structure fits into a specific binding site on the polymerase and in such a way causes the observed effects on rRNA synthesis making the drug from Silybum marianum indeed interesting for liver therapy.” Interestingly, silybinin does not have a stimulatory effect on malignant hepatic tissue.10
Antiinflammatory Effects
Leukotrienes, key chemical mediators of inflammation produced by the transfer of oxygen to polyunsaturated fatty acids (a reaction catalyzed by the enzyme lipoxygenase), can also damage the liver. Silymarin has been shown to be a potent inhibitor of this enzyme, thereby inhibiting the formation of damaging leukotrienes.12
Silymarin has also been demonstrated to inhibit prostaglandin synthesis during inflammation.13 Free radical damage to membrane structures due to organic disease or intoxication results in increased release, through lipolysis, of fatty acids. This leads, among other things, to greater prostaglandin and leukotriene synthesis. Silymarin counteracts this deleterious process by suppressing the pathologic decomposition of membrane lipids and inhibiting prostaglandin formation.13 Leukotrienes and inflammatory prostaglandins are also involved in damage of the liver by toxins, so their neutralization by silybin is another mechanism for its protection of the liver.
Anticancer Effects
Silymarin has shown significant anticancer effects in both in vivo and in vitro cancer models—including skin, breast, lung, colon, bladder, prostate, and kidney carcinomas—as well as adjunctive actions when combined with standard cancer therapies.14–18 Some of the effects noted include that it:
• Prevents the expression of genes and enzymes pivotal in cancer development
• Modulates imbalance between cell survival and apoptosis through interference with the expression of cell cycle regulators and proteins involved in apoptosis
• Exerts significant antimetastatic effects
• Has a synergistic effect when combined with conventional chemotherapy agents, including growth inhibition, reversal of chemoresistance, apoptosis induction, and reduced chemotherapy side effects in a variety of models
These preliminary studies suggest a clinical application in cancer patients as an adjunct to established therapies so as to prevent or reduce chemotherapy as well as radiotherapy-induced toxicity.18 Considering the significant problem of serious nephrotoxicity from cisplatin and other chemotherapeutic agents, silybinin may be of great value as an adjunct in the treatment of cancer.
Other Pharmacologic Actions
Silymarin shows antiviral effects against hepatitis C virus cell culture infection, including inhibition of virus entry, RNA and protein expression, and infectious virus production.19
In animal studies silymarin has been shown to increase the proliferation of lymphocytes as well as levels of interferon-gamma, interleukin-4 (IL-4), and IL-10 cytokines in a dose-dependent manner.20 It has also shown a broad range of anticancer effects in various animal models and in vitro studies.21–23
Silymarin is a strong inhibitor of cyclic adenosine monophosphate(cAMP) phosphodiesterase, being 13 to 50 times more active than theophylline and 1 to 3 times more active than papaverine.24 Silymarin has also been shown to prevent the toxic effects of a variety of compounds, such as hemolysis induced by phenylhydrazine, damage from x-irradiation, and brain edema induced by triethyltinsulfate.25–27 Presumably these effects are related to silymarin’s significant membrane-stabilizing and antioxidant actions. Its action in increasing the osmotic resistance of red blood cells is also quite significant.28
Silymarin has also been shown to lower cholesterol levels in animal studies and may block cholesterol synthesis.29
In patients with hemochromatosis, silybin adminstration at meals was shown to reduce iron absorption.30
 Clinical Applications
Clinical Applications
Silymarin’s primary use is as an aid to the liver, although additional clinical applications are regularly being discovered. This substance can be used to support detoxification reactions or in the treatment of more severe liver disease. In numerous clinical studies, silymarin has been shown to have positive effects in treating several types of liver disease, including the following:31–48
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree