CHAPTER 16 1 Identify the characteristics of children who need orthotic intervention. 2 Explain the impact of upper extremity splinting on the development of childhood occupations. 3 Describe the major features and purposes of a resting hand splint, wrist splints, thumb splints, serpentine splints, and weight-bearing splints. 4 Describe the process for fabricating each of these splints, as well as individual variations. 5 Identify resources for the purchase of prefabricated pediatric splints. 6 Explain precautions for these splints and their variations. 7 Justify an effective and reasonable wearing schedule. 8 Explain how to provide instructions to care providers to maximize correct application and usage of the splints. 9 Judge when a splint is fitting properly and identify and correct errors in the fit of a splint. 10 Examine evidence for splinting children and recommend future areas of needed research. It may not be possible or desirable to accomplish all of the splinting goals with one splint. Attempting to do so may not meet any of the stated goals [Exner 2005]. Children with severe or complex hand problems may require a series of splints that addresses the most pressing needs first or that is serial in nature, with each new splint coming closer to the desired end product. Because the purpose of this chapter is to introduce basic concepts to beginning splinters, there are many types and variations of pediatric hand splints that will not be covered. A number of children may respond best to a splint designed to reduce spasticity (see Chapter 14). Children with traumatic injuries or burns can be approached in a manner similar to adults [Hogan and Uditsky 1998], which is described in previous chapters. Other children may benefit from the use of plaster or pneumatic splints for the elbow or hand (see Chapter 14). Some splints are part of interventions in advanced areas of practice, such as the neonatal intensive care unit. These complex or specialized splints are beyond the scope of this chapter. Readers are encouraged to read articles cited in the references at the end of this chapter for more information. Those who desire additional skills in these areas should explore continuing education courses or arrange for advanced study. • Abnormal muscle tone has been present since birth or infancy and may differ qualitatively from abnormal muscle tone acquired after disease or injury. • The child experiences the dynamic process of maturational and neurologic development, which has a continuous effect on the acquisition of functional hand skills. It is also important to realize that because of the plasticity and immaturity of the child’s systems inappropriate splints can result in harmful effects [Granhaug 2006]. • Muscles and tendons undergoing growth respond differently to stretch [Wilton 2003]. • Children experience continued growth of the upper extremities. As children grow, splints fit tighter and create pressure. During a growth spurt, the risk of deformity or skin breakdown may increase as a result of bone growth that exceeds growth or lengthening of muscles and soft tissues because of spasticity. Deformity may also occur secondary to a splint that has been outgrown and no longer fits properly. • Many children must rely on adults, such as parents or teachers, to apply and remove their splints. Therefore, the level of understanding and cooperation of these adults is a factor. • Children have a low tolerance for interference by adults and the imposition of a piece of equipment (splint) unfamiliar to them. Their cognitive level may be insufficient for them to understand abstract concepts such as prevention or to comprehend cause-and-effect relationships (if you wear this splint, then your hand will work better). They may resist holding still, become fearful and cry, or be able to cooperate only for brief periods of time because of a short attention span. Any or all of these factors may create greater challenges to the fabrication and application of the splint(s) for children. In addition, as the child asserts his or her autonomy, a power struggle may develop with adults and the child may resist donning or removal of the splint at home or school. • The placement and molding of a splint on a child is more difficult than on an adult because the child’s hand is much smaller in proportion to the therapist’s hand. The focus of this chapter is on splinting the child with a developmental disability or congenital anomaly. However, many of the principles and splints described also apply to adults with developmental disabilities. According to the Centers for Disease Control and Prevention (CDC), developmental disabilities are a diverse group of chronic conditions that result from a mental and/or physical impairment and interfere with major life activities [CDC 2006]. Many developmental disabilities, such as cerebral palsy, are accompanied by central nervous system dysfunction and abnormal muscle tone. According to Banker, “Arthrogryposis multiplex congenita is not a specific disorder but rather a symptom complex of congenital joint contractures associated with both neurogenic and myopathic disorders.…The main feature shared by these disorders appears to be the presence of severe weakness early in fetal development, which immobilizes joints, resulting in contractures” [Banker 1985, p. 30]. Programs that involve early passive stretching and serial splinting of contracted joints are recommended [Bayne 1986, Donohoe 2006, Palmer et al. 1985, Sala et al. 1996, Williams 1985]. Splints, such as a dynamic elbow flexion splint, have also been developed to compensate for lost muscle power [Kamil and Correia 1990]. Children with developmental disabilities or congenital anomalies often present with indwelling thumbs (thumbs held adducted into the palm). This may be the result of abnormal muscle tone, weakness, or abnormal anatomy of the hand. To effectively grasp and manipulate objects, it is crucial that the thumb be positioned in opposition. Splinting, along with active movement, is often required to effectively position the thumb in opposition for grasp and optimal hand function. Juvenile rheumatoid arthritis (JRA) is a systemic rheumatic disease that causes major disabilities in children younger than 16 years. Children with JRA may present with pain, fatigue, and reduced range of motion (ROM). These symptoms often result in difficulty performing school tasks and activities of daily living. In addition to medical management and interventions to promote participation, treatment for JRA may include splinting and passive and active ranging of the joints [Rogers 2005]. In summary, a number of pediatric diagnoses may indicate a need for splinting. However, rather than strictly on a specific diagnosis the final splinting decision is made on the basis of the limitations in specific movements, the type and severity of abnormal muscle tone, the extent of soft-tissue and bony involvement, the child’s functional level, the child’s environment, and the frame of reference guiding therapy. Before fabricating a splint, the therapist must complete a comprehensive assessment. According to the American Occupational Therapy Association (AOTA) Occupational Therapy Performance Framework, the therapist should consider performance in areas of occupation first and then evaluate performance skills, performance patterns, context, activity demands, and client factors [AOTA 2002]. This chapter discusses areas of assessment in the categories of areas of occupation, client factors, performance skills, and context. When considering a splint, it is essential that the therapist consider the child’s strengths and level of participation as well as musculoskeletal problems. Although the child may use an “abnormal pattern,” this pattern may afford the child his or her only opportunity for participation in valued occupations. It may be necessary for a temporary loss of function in the short term in order to gain increased function in the long term. However, careful thought should be given to splinting choices before deciding on an option that will take away a child’s ability to function in favor of “fixing” the problem. As Armstrong [2005, p. 481] stated, “Is an important action being taken away to gain something else? Which is more important?” The decision about whether to splint, and what type of splint should be made, should be client centered—and the assessments used to determine the effectiveness of the splint should also be client centered [McKee 2004]. According to McKee, “An occupation-based approach ensures that the central therapeutic aim for splinting remains that of enabling either current or future occupation rather than the mere provision of a splint” [McKee 2004, p. 307]. The quality and distribution of muscle tone should be assessed at rest and during functional activity. The therapist should also determine whether the amount of tone varies according to the child’s mood, physical health, amount of effort exerted, or state of alertness. Some children have greatly increased tone during active movement but minimally increased tone during rest or while asleep. If the child’s muscle tone is not significantly increased at night, there may be no need for a night splint [Exner 2005]. Children with decreased tone may need a splint to stabilize or support joints. Children who are severely hypotonic and lack active movement may need splints to offset the constant pull of gravity that could lead to contractures. The therapist should discriminate between types of joint end feel. When tightness at a joint is primarily the result of muscle and soft-tissue shortening, with full passive range still possible with effort, this effect is known as soft end feel. When the joint cannot be moved to the end of passive range, it is said to have a hard end feel. The latter, where full passive range cannot be obtained, is known as a contracture [Hogan and Uditsky 1998, Yamamoto 1993]. Active orthotic management or splinting during childhood may prevent many contractures and resulting deformities and thus improve the quality of life for children and their families. Early orthotic intervention is usually less costly to the medical and educational systems than attempts to treat a deformity after the fact. Prolonged stretching of soft tissue (such as that provided with a splint) appears to be of greater benefit in reducing contractures than repeated briefer stretch typical of passive ROM exercises [Hogan and Uditsky 1998, McClure et al. 1994]. Provision of some passive ROM is still necessary to keep the splinted joints mobile. Passive ranging is also important for joints that are not splinted. Understanding the possible physiologic mechanisms for the formation of a contracture can assist the therapist in splint design and establishment of wearing schedules. Hogan and Uditsky [1998], McClure et al. [1994], and Watanabe [2004] provided useful discussions of this topic. Briefly, when a joint is held in a fixed position (for example, wrist flexion) the result “is a decrease in the functional length of the periarticular connective tissues and associated muscles that have been held in this shortened position.…The muscle then accommodates to this shortened immobilized position through biological changes that take place such as a loss in the number of sarcomeres” [Hogan and Uditsky 1998, p. 71]. Preventing contractures, or minimizing their severity, is one of the most important functions of splinting for children with developmental disabilities or congenital anomalies. Even with ongoing intervention, prevention of all contractures in children who have severely increased tone can be difficult and may not be possible. However, even if an existing contracture cannot be improved splinting should be done to prevent the contracture from becoming worse. A moderate contracture is better than a severe contracture because the latter can result in problems with skin breakdown and can make care much more difficult. When working to decrease a contracture it is important to keep in mind that “soft tissue connective tissue responds better to low-load prolonged stress (LLPS) than high-load brief stress (HLBS)” [Granhaug 2006, p. 419]. Children with disabilities live, rest, play, and are productive in a variety of environments—including home, school, child care centers, and sometimes hospitals. The fabrication and monitoring of splints may occur in any of these environments. When selecting and designing a splint, persons who are responsible for donning the splint must be considered. Simplicity of design is desirable and may be a necessity in cases where the child interacts with multiple care providers in a variety of environments. Compliance with using the splint is likely to decline as the complexity with the donning and wearing schedule increases. In the hospital setting, care must be taken to obtain information from family members and the treating therapist (if applicable) about home and school settings that will influence splinting decisions. Careful planning must be made when splinting in the intensive care units of the hospital because splints must be fabricated with minimal handling of the infant or child and while navigating carefully around life-supporting tubes and monitors. Consideration must be given to incorporation of the use of the splints in the daily medical care provided by nursing staff. The therapist must also be familiar with the child’s medical condition and be able to recognize signs of stress that can be harmful to the child. Practice in the neonatal intensive care unit requires advanced competencies, and therapists considering practice in this environment should obtain training beyond entry level [Hunter 2005]. After an assessment is completed, the therapist can establish therapeutic goals and intervention strategies for the child. A splint may be a component of this treatment plan. According to Schoen and Anderson, orthotic devices (like adaptive equipment) are an important part of intervention because they reinforce neurodevelopmental treatment therapeutic goals: “If preventative measures such as adaptive equipment and orthotic devices are provided, then the child will receive consistent input to prevent or reduce the occurrence of deformities and limitations” [Schoen and Anderson 1999, p. 107]. Once a decision is made to provide a splint for a child, the splinting process is initiated. Thoughtful preparation is especially important when splinting children because of their short attention spans. In addition to having splinting and play materials close at hand, it is recommended that the therapist plan to have a second pair of adult hands to help with the fabrication process [Armstrong 2005]. This additional person might be a parent, teacher, paraprofessional, or another therapist. This is especially important if the child has increased tone, is not able to follow verbal instructions, or is likely to be uncooperative. The therapist must clearly explain the helper’s role so that efforts assist the process and not hinder it. This usually involves maintaining the child’s overall position, calming or entertaining the child, holding the arm just proximal to the joint being splinted, or stabilizing the material once in place and while it is cooling. When splinting with neoprene, the therapist should be alert to the possibility of skin irritation or rash. According to Stern et al. [1998, p. 573], “skin contact with neoprene poses two dermatological risks: allergic contact dermatitis (ACD) and miliaria rubra (i.e., prickly heat).” Although neoprene hypersensitivity is rare, the authors recommend that therapists screen patients for a history of dermatologic reactions; instruct clients to discontinue use and inform the therapist if a rash, itching, or skin eruptions occur; and report cases of adverse skin reactions to the manufacturer of the neoprene material. They also recommend that therapists limit their own exposure to neoprene and neoprene glue because of the exposure to thiourea compounds that are thought to contribute to allergic reactions. Thermoplastic materials range in conformability (and in stretch, thickness, and rigidity) and are described in Chapter 3. Generally, thermoplastic materials with a high plastic content have more conformability—whereas materials with a high rubber content have less stretch but are less likely to be indented with fingerprints during fabrication or stretch out of shape. When making a splint that counteracts the forces of spasticity, it is especially important to select a thermoplastic material that resists stretch (i.e., one with a high rubber content) because it is necessary for the therapist to apply considerable pressure to obtain the desired position of the wrist, thumb, and fingers [Armstrong 2005]. One way to reduce the stickiness is to add a tablespoon of liquid soap or shampoo to the hot water [Hogan and Uditsky 1998]. When splinting a neonate or young infant, the standard It may be helpful to plan on extending the splint material a little beyond that of the finished product in order to give the therapist leverage to help hold joints in position. The extra can be cut away when the essential part of the splint is finished and hardened [Granhaug 2006]. The therapist should heat the water to the temperature range recommended by the manufacturer. After cutting out the splint, it may be necessary to reheat the plastic to obtain the desired degree of pliability before the molding process. Before placing the plastic on a child’s extremity, the therapist should dry off the hot water and make sure the plastic is not too hot. Checking the thermoplastic material’s temperature can be done by placing it against the therapist’s face or anterior portion of the forearm. This is especially important when spot heating with a heat gun because this method tends to result in higher surface temperatures. To ensure a proper fit, the therapist should lay the padding on the child’s extremity before molding the plastic or place it on the thermoplastic material before molding the splint. When molding with padding, the stretch of the thermoplastic material and the contourability may be compromised. Therefore, the therapist should add padding only if absolutely necessary. In addition, padding becomes soiled and needs to be replaced. For more information on padding, see Chapter 3. Another way to create pressure relief around a bony prominence without using padding is to cover the prominence with a small amount of a firm therapy putty before forming the splint. The putty creates a built-in bubble and is removed from the splint after cooling [Hogan and Uditsky 1998]. Thin forms of padding may also be useful to create friction and reduce migration or shifting of splints, or for covering edges. Microfoam tape is useful for this purpose, especially on small splints. Straps can be secured at each end with hook Velcro, which is attached to the splint. This allows them to be easily replaced when they become soiled, which is important if the child drools on the splint or mouths it. However, loose straps easily become lost and many times are not placed on the splint at the correct angle or location. An alternative is to adhere the strap at one end with a rivet or strong contact adhesive. When soiled, straps must be removed by the therapist and a new strap reattached. See Chapter 3 for more detailed information about attaching straps. Increasing the likelihood that the child will not remove straps and the splint requires knowledge of child development and creativity. Children at certain ages (such as 2- and 3-year-olds) are in the developmental stage of asserting their autonomy and may resist the parent’s choice of clothing or food or splint application. In this case, using principles of behavior analysis (such as shaping or rewarding successive approximations, finding times during the day when the child is most likely to be compliant, and contingent use of praise and attention) may be helpful. Actively involving the child in the choice of colors and decorations may increase the child’s willingness to wear the splint. Strap Critter patterns are provided by Armstrong [2005], along with suggestions for using decorative ribbon, fabric paints, or shoelace charms. She also suggested describing the splint as something cool to wear and providing the child with language to use to explain to peers, such as this is my Batman or scuba diver’s glove. If positive methods to prevent splint removal have not worked, therapists can use their creativity to keep the little “Houdinis” in their splints, especially young children who do not understand cause and effect. Some kid-proof methods include using shoelaces, buttons, or socks/stockinette/puppets. Lacing can be done by punching holes along the lateral edges of the splint and lacing with wide decorative shoelaces. The therapist should place padding under the laces against the skin. To secure the laces, the therapist can use a “bow biter” (a plastic device available in children’s shoe departments) to hold the laces in place [Collins 1996]. Depending on the function of the splint, a sock puppet worn over the splint may be used as camouflage (Figure 16-1). Care must be taken not to provide any attachment the child could bite off and swallow.
Pediatric Splinting
Diagnostic Indications
Assessment
Areas of Occupation
Client Factors
Contractures
Context
Overview of the Splinting Process
Prepare the Environment
Selection of Splinting Materials
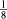 -inch material may be too thick and heavy. Rather, the therapist should use material that is 1/16-inch or 3/32-inch in thickness. The therapist’s experience and preferences also affect the choice of thermoplastic material. (See Chapter 3 for a review of splinting material.)
-inch material may be too thick and heavy. Rather, the therapist should use material that is 1/16-inch or 3/32-inch in thickness. The therapist’s experience and preferences also affect the choice of thermoplastic material. (See Chapter 3 for a review of splinting material.)
Patterns
Heating the Thermoplastic Material
Padding
Strapping
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Pediatric Splinting







