Chapter 36 Pediatric hip orthoses
Developmental dysplasia of the hip
Studies of the natural history of hip dysplasia indicate that radiographic evidence of residual hip dysplasia is associated with the development of degenerative joint disease.5,13,28 Stulberg and Harris42,43 reported that 48% of 130 patients with degenerative joint disease of the hip had evidence of primary acetabular dysplasia. True subluxation is more strongly associated with degenerative joint disease, with the degree of subluxation correlating with the age at onset of symptoms.23,25 Symptoms of severe subluxation usually appear within the second decade of life.
The natural history of dislocated hips is dependent on whether the condition is unilateral or bilateral and on the presence or absence of a false acetabulum. In general, hips with a well-developed false acetabulum are more likely to be painful than are those without a false acetabulum. The pain is due to degenerative joint disease. Unilateral dislocations are more likely to be symptomatic than bilateral dislocations due in part to limb-length discrepancy, which leads to knee and back pathology. However, even bilateral dislocations are associated with back pain, probably because of hyperlordosis.49,51,52
Frejka pillow
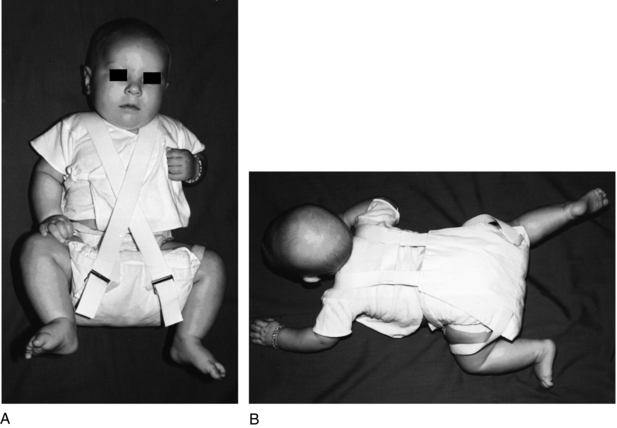
In 1941, Bedrich Frejka introduced a soft abduction pillow for treatment of DDH in infants (Fig. 36-1).34 He developed the device in response to the high rates of AVN associated with previous methods of treatment, which included Lorenz casting and various passive-abduction braces. The Frejka pillow was designed to maintain abduction; however, given the pillow’s soft nature, infants could easily overcome the abduction pressure. The pillow subsequently was modified to create a firmer construct. The most recent version consists of a 9- × 9- × ¾-inch foam pillow that is placed around the child’s buttocks, much like a diaper, and secured in place with a cloth harness and straps.
Even with this firmer construction, however, infants were not held in adequate abduction or flexion to allow the femoral head to be directed toward the triradiate cartilage. In addition to difficulties with attaining and maintaining reduction, the Frejka pillow developed a reputation for having high rates of AVN,16,17 although the literature does not support this association.4,45 Use of the Frejka pillow has essentially been abandoned in North America, although it is still used with reported good results in some areas of Europe.
Pavlik harness
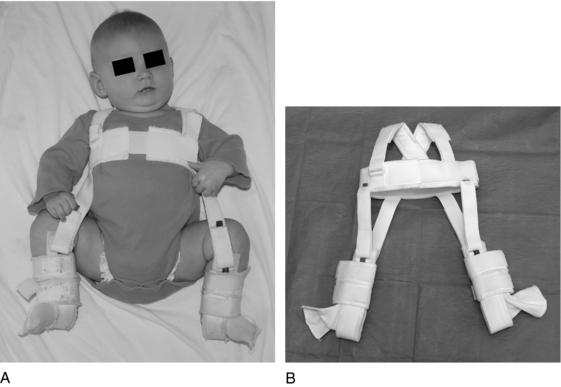
Arnold Pavlik joined Frejka in practice in 1932.34 The two men had a common interest in the treatment of hip dysplasia. Pavlik, noting the high rate of AVN with previous splints and the difficulty with maintaining hips in an acceptable position using the Frejka pillow, decided to design a new device (Fig. 36-2). His theory, as described in his classic article in 1957, was that with all previous devices, “the passive-mechanically reduced femoral head pushes against . . . obstacles in the acetabulum. Add to these circumstances the tension of the adductors and the passive-mechanically reduced femoral head cannot overcome these obstacles and damage to the head of the femur results.”37
Pavlik suggested that the hip requires active motion in order to develop normally. His harness is designed to prevent only extension of the hips. By placing the hips in the “rider position,” the device enables the adductors to relax with time and movement, allowing the head to spontaneously reduce. Once the head reduces, the harness maintains the reduction. Pavlik further argued that in cases where the acetabulum is filled with tissue, the constant motion of the hip (with associated redislocations and partial reductions) will create space for the head within the acetabulum. Furthermore, the motion prevents undue pressure on the head, thus preventing AVN.37
The Pavlik harness has two shoulder straps that cross in the back and are secured to a wide chest strap. Stirrups are suspended from the breast strap. When properly placed on the child, the chest strap is positioned at the nipple line, the anterior stirrup straps are located at the anterior axillary line, and the posterior straps overlie the scapulae. The anterior straps should maintain the hips in 90 to 110 degrees of flexion. Although it may seem that the posterior straps are designed to maintain wide abduction, this is distinctly counter to Pavlik’s theory and design. The straps should be tensioned to maintain 20 to 30 degrees of abduction only, with the remaining abduction arising from gradual relaxation of the adductors.
The harness is indicated for patients with dysplastic, subluxated, or dislocated hips. Pavlik recommended its use for infants younger than 12 months37; however, others have decreased the upper age limit to 8 months.12,33 Ultrasonography is used to determine the degree of dysplasia. Harcke’s method of dynamic sonographic evaluation and Graf’s static method are used to interpret the ultrasound scan and determine the need for treatment.
If the hip is dislocated upon initiation of the harness, the child should undergo weekly ultrasound evaluation until reduction is confirmed. If hip reduction cannot be documented within 3 weeks of beginning harness treatment, the harness should be abandoned because prolonged use of the harness without reduction can lead to significant complications. Most notably, persistent posterior dislocation maintained by the harness appears to erode the posterolateral acetabular wall,23 a condition sometimes referred to as Pavlik harness disease. If the hip is found to reduce, a protocol similar to that described above, with full-time harness wear followed by gradual weaning once the hip is radiographically normal, is used.
Many researchers have attempted to identify risk factors for failure of Pavlik harness treatment.11,12,25,48 The most commonly reported risk factors are bilaterality, absence of an Ortolani sign, age greater than 7 weeks at initiation of treatment, and less than 20% initial femoral head coverage as judged by ultrasound. Other risk factors are parental noncompliance and inappropriate use or application of the harness by the physician.
Complications associated with use of the Pavlik harness include Pavlik harness disease as well as skin irritation, femoral nerve palsy, inferior dislocation of the hip, and AVN of the femoral head.8,9,22,24,32,38,44,46,47,53 Femoral nerve palsy and inferior dislocation of the hip have been associated with excessive flexion of the hip, and both have responded favorably to lengthening the anterior straps, which decreases the flexion. AVN is the most serious complication; long-term results in these hips are less favorable and less predictable. Reported rates of AVN vary from 0% to 27%, with higher rates reported for treatment of dislocated hips than treatment of subluxated or dysplastic hips. Most surgeons believe that the incidence of osteonecrosis likely will approach zero if the Pavlik harness is appropriately applied and monitored.
Success rates with the Pavlik harness are reported to be 90% to 100% for treatment of hip subluxation or dysplasia and 80% to 95% for treatment of dislocated hips.8,9,12,32,37,38,44,47,53 These high rates of success, combined with the low rates of complication, make the Pavlik harness the gold standard for treatment of hip dysplasia and for the initial treatment of congenital hip dislocation.
Von Rosen orthosis
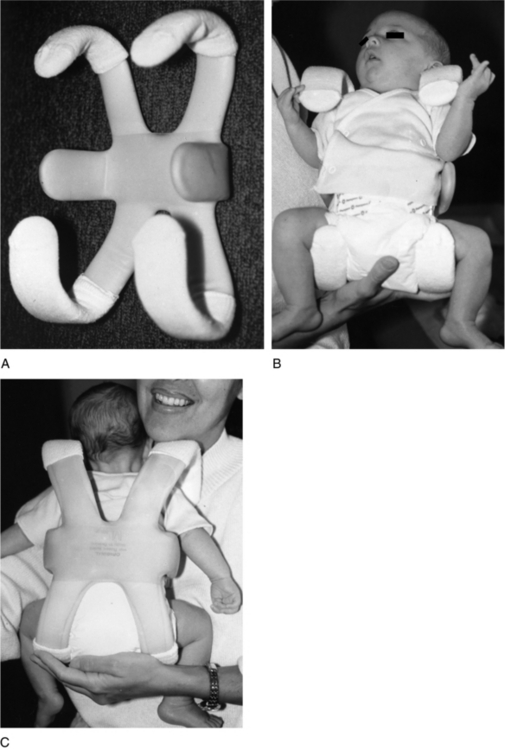
The Von Rosen orthosis is used in Scandinavian countries but is not frequently used in North America (Fig. 36-3). It is a passive restraining/positioning device. It is a malleable frame (originally metal but now plastic) with straps around the shoulders, waist, and thighs. The few available studies indicate very low rates of AVN but high rates of pressure ulcers with use of this device.16,20
Ilfeld orthosis
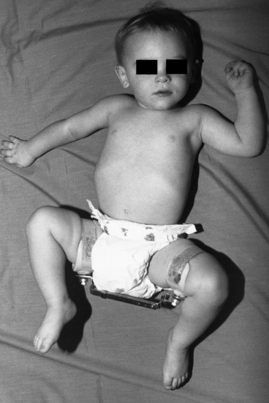
The Ilfeld orthosis is a passive positioning device that holds the hips in abduction but does not create significant hip flexion (Fig. 36-4). For this reason, it is more effective as a postoperative abduction device than for treatment of infantile hip dysplasia or dislocation. It consists of two thigh cuffs attached to an adjustable crossbar. This construct is attached to a waist strap to maintain positioning.
Plastazote hip abduction orthosis
Two different Plastazote hip abduction devices have been reported in the literature to successfully treat hip dysplasia and dislocation. Hedequist et al.15 reported the successful use of an abduction brace in 13 of 15 patients with dislocated hips who had not responded to Pavlik treatment (Fig. 36-5). None of the children developed AVN. The authors suggest a 3- to 4-week trial in an abduction orthosis for children whose hips fail to reduce in a Pavlik harness. Using a somewhat different design, Eberle7 reported his results on the use of an abduction orthosis in lieu of a Pavlik harness in 113 infants with 140 unstable hips (Fig. 36-6). Again, no instances of AVN occurred, and all but two hips had radiographic normalization without any further treatment. Both braces are made of a Plastazote foam that wraps around the legs and waist, maintaining the hips in approximately 70 to 90 degrees of flexion and wide abduction. Both allow free motion of the knees.
Legg-Calvé-Perthes disease
LCP disease is one of the most vexing problems faced by the pediatric orthopedist. The goal of treatment is to attain a congruous hip joint, ideally a Stulberg I or II. For this reason, the idea of containment, wherein the femoral head is maintained within the acetabulum and congruent remodeling is encouraged, is appealing. Multiple orthoses have been designed to hold the hip in abduction and to permit varying degrees of internal rotation and/or flexion, thus directing the head into the acetabulum. Although early reports on these devices were promising, subsequent reports were less favorable. Herring et al.18,19 published their findings from a multicenter study that included 451 hips affected with LCP disease. These authors found no difference in outcome among hips that received no treatment, those treated with range-of-motion exercises, and those treated with bracing. Thus, although bracing may have a role after surgical containment, the current literature does not support the use of bracing alone for containment.
Toronto orthosis
Bobechko2 introduced this ambulatory abduction orthosis in 1968 (Fig. 36-7). Two thigh cuffs are attached to a triangular frame, which in turn attaches to horizontal bars to which plates are attached. The hips are held in 45 degrees of abduction and are maintained in internal rotation by the fixed position of the shoes on the footplates. Hip and knee motion allow the child to ambulate with crutches.
< div class='tao-gold-member'>
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree